Multiple facial cylindromas: A case report
Published Web Location
https://doi.org/10.5070/D385w0032dMain Content
Multiple facial cylindromas: A case report
Amiya Kumar Nath MD, Carounanidy Udayashankar MD
Dermatology Online Journal 18 (2): 8
Indira Gandhi Medical College and Research Institute, Puducherry Pondicherry, Pondicherry, IndiaAbstract
Cylindroma is a benign skin appendageal tumor arising from pluripotent stem cells in the folliculo-sebaceous-apocrine unit. Multiple cylindromas are usually seen as a component of Brooke-Spiegler syndrome (BSS) or as the only skin lesions of familial cylindromatosis (FC). The usual site of occurrence of such tumors is the scalp. We report a case of multiple cylindromas involving the face without any other feature of BSS and no family history supporting the possibility of FC. Multiple cylindromas of 7 years duration, confirmed by histopathological examination of multiple biopsies, were seen on the face of a 70-year-old woman. There was no history of similar lesions in any of her family members. Examination of the scalp revealed no lesions. Surgical excision of the larger lesions was performed to improve the facial appearance of the patient. This case is being reported for the unusual occurrence of multiple cylindromas only on the face without any features of BSS or FC.
Introduction
Brooke-Spiegler syndrome (BSS, OMIM# 605041), familial cylindromatosis (FC, OMIM# 132700), and multiple familial trichoepithelioma (MFT, OMIM# 601606) were originally described as distinct entities with each having a unique OMIM number [1, 2, 3]. Patients with BSS are predisposed to multiple skin appendage tumors such as cylindroma, trichoepithelioma, and spiradenoma. FC is characterized by cylindromas and MFT by trichoepitheliomas as the only tumor type [1, 4, 5, 6]. However, because these disorders show overlapping phenotypic features, and because different manifestations of each have been described within a single family, many consider these disorders to represent a phenotypic spectrum of a single disease entity. This contention is further strengthened by the fact that mutation in a single CYLD gene is responsible for all three syndromes [1, 5]. Multiple cylindromas without the other components of BSS appear to be exceedingly rare, if they occur at all [7]. However, components of BSS may be present in clinically separate lesions or in different histopathology foci, which may be missed if the lesion representing the admixture is not biopsied. However, in some close cases the distinction between BSS and FC would seem best clinically because a histopathological admixture may be missed and CYLD identification also may not help. We noted a case of multiple cylindromas occurring unusually only on the face without any other clinical or histopathological components of BSS in a elderly women. The onset of her tumors at 63 years of age is well beyond the age of occurrence of skin lesions of BSS or FC. Because a careful family tree charting did not reveal any other family member with similar skin lesions, we describe this condition as multiple non-familial facial cylindromatosis.
Case report
 |
| Figure 1 |
|---|
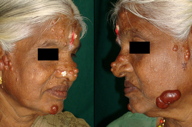
| Figure 1. Multiple cylindromas on the face Figure 1a. Right side Figure 1b. Left side, with a tendency to grouping in the preauricular regions |
A 70-year-old woman presented with multiple asymptomatic swellings over the face for the past 7 years with a progressive increase in size and number over the years. Some lesions grew significantly in the last 6 months producing visible facial disfigurement; for this reason she sought our consultation. There was no history of similar lesions in any of her family members.
On examination, multiple, rounded, smooth surfaced, firm, non-tender, freely mobile skin colored to reddish papules and nodules of varying sizes (3 mm to 4 cm) were seen on the face (forehead, nose and chin, pre-auricular region, and along the jaw-line). There was tendency to develop a grouping of lesions in the preauricular regions (Figure 1). Examination of scalp revealed no lesions. Examination of other areas of the skin, mucosa, nails, and hair showed no abnormalities.
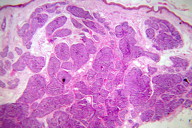
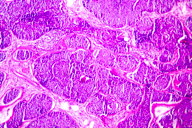
Excisional biopsy of a nodule revealed a non-encapsulated tumor composed of closely set tumor lobules forming mosaic-like masses giving a jigsaw-puzzle appearance. The tumor lobules were separated from each other by thin bands of hyaline material (Figure 2). On higher magnification two types of cells were seen – larger cells with a moderate amount of cytoplasm and a vesicular nucleus in the center of the tumor lobule and small cells with little cytoplasm and compact nuclei in the periphery. The small cells were seen surrounding duct-like spaces and masses of hyaline material within a few tumor lobules (Figure 3). A diagnosis of cylindroma was made based on the typical histopathological findings.
Surgical excision of the larger lesions was performed to improve the facial appearance of the patient and all those lesions revealed cylindroma on histopathology.
Discussion
Cylindroma is a benign cutaneous appendageal tumor that most often affects the scalp, with a strong predilection for middle-aged and elderly females [8]. It occurs more often as a solitary lesion [9]. Lesions on the face and neck away from the scalp margin are unusual; in less than 10 percent of cases these may occur on the trunk and limbs [2]. The rate of growth is slow and the tumors seem to stop growing after reaching a certain size. The tumors are generally asymptomatic, but an occasional patient may have pain [2]. Cases with multiple lesions tend to be dominantly inherited [9] and clinically present as multiple, smooth, firm, pink to red, somewhat pedunculated nodules of various sizes [2]. In such cases, new tumors continue to develop over the years. Scalp lesions may be present in large numbers and cover the entire scalp like a turban (turban tumor, considered to be the most florid and disfiguring feature of BSS, is fortunately seldom observed) [9]. A rare variant with multiple lesions in linear array has been reported [9].
The origin of cylindromas appears to be from pluripotent stem cells in the folliculo-sebaceous-apocrine unit [1, 8, 9]. Mutation in CYLD gene (a tumor suppression gene) on chromosome 16q12–q13 is responsible for tumorogenesis in the affected patients through constitutive NF-κB activation (e.g. owing to the inability of mutated CYLD to downregulate this activation) [8]. Loss of heterozygosity at the CYLD locus has been found in both inherited and sporadic tumors [1]. It has been reported to follow radiotherapy epilation of the scalp [2].
Histopathologically, cylindromas are poorly circumscribed dermal tumors composed of numerous islands of epithelial cells, separated often only by their hyaline sheath and a narrow band of collagen, giving a jigsaw-puzzle appearance [7, 9]. They exhibit multiple molecular defects in their basement membrane zone, including the lack of mature hemidesmosomes, defective processing of laminin 5, and abnormalities in collagen IV alpha 1- and alpha 5-chain expression [8]. Two types of basaloid cells constitute the islands: relatively undifferentiated cells with small, dark-staining nuclei present predominantly at the periphery of the islands, often in a palisade arrangement. More differentiated cells with large, light-staining nuclei present in the center of the islands [9]. In addition, tubular lumina are often present. The lumina are lined by cells that usually have the appearance of ductal cells [9].
Local aggressive behavior and malignant transformation are uncommon and usually associated with long-standing turban tumors of the scalp [7, 10]. However, metastasis of malignant tumors is very rare [7].
Sporadic, solitary cylindromas are not inherited; they appear in adulthood and occur either on the scalp or the face [9]. BSS is autosomal dominant in inheritance with a high penetarnce of 60 percent to 100 percent [3]. In BSS and FC, lesions usually develop in early adult life (2nd or 3rd decades of life [3]), but may occur even in childhood or adolescence [7]. In BSS, the different types of tumor mostly adhere to specific predilection sites on the body [4]. Trichoepitheliomas are commonly encountered on the central face in the perinasal area, whereas spiradenomas usually develop on the upper trunk. Cylindromas mostly manifest on the head and neck as multiple lesions [4]. Phenotypic and histopathological variations may occur between the different members of the affected family, with elder members tending to have more numerous and larger lesions [3]. Spiradenomas usually manifest as solitary, reddish-to-pink nodules on the trunk, whereas both cylindroma and trichoepithelioma present in groups of partly coalescing and confluent tumors [4]. We ruled out BSS/FC in our case by the absence of family history, late onset of the lesions, and the absence of trichoepitheliomas or spiradenomas clinically and in multiple histopathological sections.
There is no curative therapy yet available for multiple cylindromas. Currently, surgical excision or laser ablation is the treatment of choice in multiple cylindromas [3, 4]. Total scalp and forehead excision with coverage by skin grafts has been described in patients with turban tumors [4]. Recently, a therapeutic attempt has been made to treat single cylindroma in BSS with topically applied salicylic acid at varying concentrations. Salicylic acid acts by interfering with the NF-κB signaling pathway [4].
References
1. Bowen S, Gill M, Lee DA, Fisher G, Geronemus RG, Vazquez ME, Celebi JT. Mutations in the CYLD gene in Brooke-Spiegler syndrome, familial cylindromatosis, and multiple familial trichoepithelioma: lack of genotype-phenotype correlation. J Invest Dermatol 2005;124:919-20. [PubMed]2. Calonje E. Tumours of the Skin Appendages. In: Burns T, Breathnach S, Cox N, Griffiths C, eds. Rook’s Textbook of Dermatology, 8th edn., Singapore: Wiley-Blackwell 2010: 53.28-53.29.
3. Layegh P, Sharifi-Sistani N, Abadian M, Moghiman T. Brooke-Spiegler syndrome. Indian J Dermatol Venereol Leprol 2008;74:632-4. [PubMed]
4. Parren LJ, Bauer B, Hamm H, Frank J. Brooke-Spiegler syndrome complicated by unilateral hearing loss. Int J Dermatol 2008;47 Suppl 1:56-9. [PubMed]
5. Accessed from http://www.omim.org/entry/605041 on 12.10.2011.
6. Accessed from http://www.omim.org/entry/132700 on 12.10.2011.
7. Weedon D. Tumors of cutaneous appendages. Weedon’s Skin Pathology, 3rd Edn., China: Churchill Livingstone Elsevier 2010: 785-786.
8. Massoumi R, Podda M, Fässler R, Paus R. Cylindroma as tumor of hair follicle origin. J Invest Dermatol 2006;126:1182-4. [PubMed]
9. Klein W, Chan E, Seykora JT. Tumors of the epidermal appendages. In: Elder DE, Elenitsas R, Johnson BL, Murphy GF, eds. Lever’s Histopathology of the Skin, 9th edn., Philadelphia: Lippincott Williams & Wilkins 2005: 897-898.
10. Nair PS. A clinicopathologic study of skin appendageal tumors. Indian J Dermatol Venereol Leprol 2008;74:550. [PubMed]
© 2012 Dermatology Online Journal