Sarcoidosis involving the lacrimal, submandibular, and parotid glands with panda sign
Published Web Location
https://doi.org/10.5070/D380j4r407Main Content
Sarcoidosis involving the lacrimal, submandibular, and parotid glands with panda sign
Seray Külcü Çakmak1, Müzeyyen Gönül1, Ülker Gül2, Hülya Gündüz3, Özge Han4, Sezer Kulaçoğlu5
Dermatology Online Journal 15 (3): 8
1. Dermatologist, Ankara Numune Education and Research Hospital, 2nd Dermatology Clinic. seraycakmak@gmail.com2. Associate Professor, Ankara Numune Education and Research Hospital, 2nd Dermatology Clinic
3. Assistant, Ankara Numune Education and Research Hospital, 2nd Dermatology Clinic
4. Pathologist, Ankara Numune Education and Research Hospital, Pathology Clinic
5. Associate Professor, Ankara Numune Education and Research Hospital, Pathology Clinic
Abstract
Sarcoidosis is a granulomatous inflammation of unknown origin that varies in severity and distribution. We present a case of sarcoidosis with involvement of the skin, lacrimal, parotid, and submandibular glands. The patient had been previously misdiagnosed as having angioedema and allergic contact dermatitis; he had the rare finding of panda sign on gallium scintigraphy.
Sarcoidosis is a systemic granulomatous disease with an unknown etiology. It has been suggested that sarcoidosis develops in genetically predisposed individuals after exposure to certain enviromental and infectious agents, which trigger the inflammatory response and granuloma formation [1]. Although lung is the most common organ affected, it may involve any part of the body [2]. We present a case of sarcoidosis with involvement of skin, lacrimal, parotis and submandibular glands that was previously misdiagnosed as allergic contact dermatitis and angioedema.
Case Report
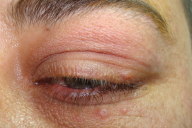
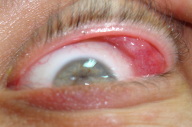
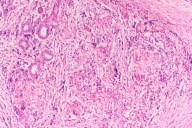
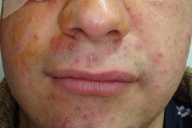
A 29-year-old man presented with a 1.5 month history of painless edema of bilateral upper eyelids. He had been diagnosed as having allergic contact dermatitis and angioedema previously and treated with antihistamines and topical steroids without any improvement. He did not have weight loss, fever, chills, or malaise. On physical examination 0.5-1 cm sized masses were palpated on the lateral side of his upper eyelids and 2-5 mm sized erythematous papules were observed around the eyes (Fig. 1). On eversion of the upper eyelids, the red, swollen palpebral lobe of the lacrimal gland was observed (Fig. 2). Routine laboratory examinations including complete blood count, routine biochemical analysis, and urinalysis were within normal limits; serum angiotensin converting enzyme level was 74 U/L (Normal: 8-52 U/L). The patient was examined in the eye clinic and orbital magnetic resonance imaging (MRI) was done according to their suggestion. Orbital MRI revealed diffuse, symmetrical hypertrophy of bilateral eyelids. A biopsy of the lacrimal glands revealed granulomas with epitheloid histiocytes in the center and a few lymphocytes on the periphery (Fig. 3). After the biopsy of lacrimal glands were performed, multiple erythematous 2-5 mm sized papules appeared on the face of the patient (Fig. 4).
 |  |
| Figure 3 | Figure 4 |
|---|---|
| Figure 3. Granulomas with epitheloid histiocytes in the center and few lymphocytes on the periphery (H&E x200) Figure 4. Multiple erythematous papules on the face of the patient | |
 |
| Figure 5 |
|---|
| Figure 5. The "panda sign" in radiogallium scintigraphy |
The histopathologic examination of the lesions revealed noncaseating epithelioid granulomas. No pathological finding was observed on electrocardiography, chest roentgenogram, chest computerized tomography and abdominal ultrasonography. Radiogallium scintigraphy revealed increased bilateral symmetrical lacrimal, parotid, and submandibular gland uptake. Radiogallium was not observed to be taken up by the lung (Fig. 5). The patient was diagnosed as having systemic sarcoidosis and 1 mg/kg/day prednisolone therapy was initiated. The lesions on the face and swelling of the eyelids regressed in 10 days and the corticosteroid was gradually tapered off.
Discussion
Sarcoidosis varies in severity and distribution from single-organ involvement and self-limiting disease to chronic multisystem inflammation and organ failure [2]. Sarcoidosis generally presents with bilateral hilar adenopathy, pulmonary infiltration, and skin or eye lesions. Ocular involvement is seen in approximately 25 percent of the sarcoidosis patients and the incidence varies with sex and race [3]. The most common ocular finding is anterior uveitis [1]. Other ocular manifestations include posterior uveitis, chorioretinitis, concuctival and eyelid granulomas. More rarely extraocular tissues may be affected, with the lacrimal gland most commonly affected [4]. Lacrimal gland enlargement most commonly presents as asymptomatic swelling of the lateral upper lid. Other presenting symptoms in patients with lacrimal gland involvement includes upper eyelid swelling, ptosis, and globe displacement [1, 4, 5].
Skin lesions of sarcoidosis may be specific and nonspecific. The characteristic histological picture of sarcoidosis is noncaseating epitheloid granulomas with minimal or absent associated lymphocytes or plasma cells [6]. Our patients had papular lesions that are included in the category of specific lesions demonstrating granulomatous inflammation on biopsy [5].
Gallium scintigraphy shows isotope concentration at sites of inflammation, including mediastinum, lungs, liver, spleen, salivary glands, lacrimal glands, and eye [1]. The image of symmetrical radiogallium uptake in the lacrimal and parotid glands is called the "panda sign;" the submandibular salivary glands may or may not be clearly delineated on the radiogallium images. The panda sign occurs in only a limited number of conditions; sarcoidosis, Sjögren syndrome and post-radiation changes of the head and neck are likely to account for over 90 percent of the recognized instances of panda sign [7]. Our patient had panda sign on gallium scintigraphy, which is positive in a small number of patients and is highly specific for sarcoidosis [8].
It is not always mandatory to treat sarcoidosis because the disease may remit spontaneously. Therapy is indicated for potentially dangerous disease including ocular involvement, neurosarcoidosis, cardiac sarcoidosis, and progressive disease that threatens organ function. Corticosteroids are the mainstray of treatment. The treatment of extrapulmonary sarcoidosis must be individualized. The basic approach should be to reduce the corticosteroid dose to the lowest effective dose. Some alternative agents like azathioprine, chloroquine, hydroxychloroquine, methotrexate, chlorambucil, pentoxifylline, cyclophosphamide, tetracycline derivatives, and infliximab may be used in refractory disease or as corticosteroid-sparing agents [5, 6]. Our patient was initially treated with 1 mg/kg/day prednisolone and then the prednisolone dose was tapered to 0.75 mg/kg/day after one month. The prednisolone dose was gradually tapered and discontinued at the end of 8 months. The patient has been followed up for 1 month after the cessation of therapy and there is no recurrence off prednisolone so far.
We present this case because of the rare finding of the panda sign on gallium scintigraphy and to remind physicians that the diagnosis of sarcoidosis should be considered in patients with swelling of the eyelids.
References
1. Bonfioli AA, Sarcoidosis, Semin Ophtalmol. 20(3)177-182, 2005. [PubMed]2. Jones N,. Sarcoidosis, Curr Opin Ophtalmol. 13(6)393-396, 2002. [PubMed]
3. Prabhakaran VC, Saeed P, Esmaeli B, Sullivan TJ, McNab A, Davis G, Valenzuela A, Leibovitch I, Kesler A, Sivak-Callcott J, Hoyama E, Selva D, Orbital and adnexal sarcoidosis, Arch Ophtalmol. 125(12)1657-1662, 2007. [PubMed]
4. Mavrikakis I, Rootman J, Diverse clinical manifestations of orbital sarcoid, Am J Ophtalmol. 144(5)769-75, 2007. [PubMed]
5. Judson MA, Sarcoidosis: Clinical presentation, diagnosis and approach to treatment, Am J Med Sci. 335(1)26-33, 2008. [PubMed]
6. Fernandez-Faith E, McDonnell J, Cutaneous sarcoidosis: differential diagnosis, Clin Dermatol. 25(3)276-87, 2007. [PubMed]
7. Sulavik SB, Spencer RP, Castriotta RJ, Panda sign-avid and symmetrical radiogallium accumulation in the lacrimal and parotid glands, Semin Nucl Med. 21(4)339-40, 1991. [PubMed]
8. Marchell RM, Thiers B, Judson MA, Sarcoidosis in Fitzpatrick's Dermatology in General Medicine, ed. Wolff K, Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, 7th ed. N. Y., Mc-Graw-Hill Companies; 2008.
© 2009 Dermatology Online Journal