Rubinstein-Taybi syndrome (broad thumb-hallux syndrome)
Published Web Location
https://doi.org/10.5070/D37xm3p7nfMain Content
Rubinstein-Taybi syndrome (broad thumb-hallux syndrome)
Sherry H Hsiung MD
Dermatology Online Journal 10 (3): 2
From the Ronald O. Perelman Department of Dermatology, New York University
Abstract
Rubinstein-Taybi syndrome is a rare genodermatosis with characteristic features that include downward sloping palphebral fissures, broad thumbs and halluces, and mental retardation. Dermatologic manifestations include capillary malformations, keloid formation, and pilomatricomas. Systemic features may involve the cardiac, audiologic, ophthalmologic, endocrine, neurologic, and respiratory systems. The syndrome is sporadic in nature and has been linked to microdeletion at 16p13.3 encoding CREB-binding protein gene (CREBBP).
Clinical synopsis
History.—A three-year-old girl was referred to the Charles C. Harris Skin and Cancer Pavilion for evaluation of an arthropod assault. During the clinical evaluation, her mother stated that the patient had a syndrome consisting of mental retardation, broad thumbs and great toes, and facial abnormalities. The patient's medical history includes a patent ductus arteriosus that has yet to be corrected. She had surgical removal of adenoids and myringomotomy of the Eustachian tubes. She was also treated with ranitidine for presumptive gastroesophageal reflux.
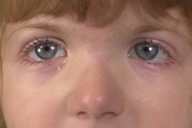
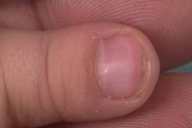
Physical Examination.—The facies showed downward lateral sloping of the palpebral fissures. Broad thumbs and great toes were noted. She did not have any capillary malformations or keloids. There were no heart murmurs.
|
|
| Figure 1 | Figure 2 |
|---|
Diagnosis.—Rubinstein-Taybi syndrome (broad thumb-hallux syndrome).
Comment
Rubinstein-Taybi syndrome (RTS) was initially reported by Michail et al. in 1957 as the broad thumb-hallux syndrome and then was described by Rubinstein and Taybi in 1963 [1] in children with broad thumbs and toes with facial abnormalities and short stature. Since that time, there have been over 250 cases documented in the literature. It has been estimated that 1 per 300-500 institutionalized persons with mental retardation over age 5 have the syndrome. Male and female individuals are affected at equal rates [2].
Typical facial features include downward slanting palpebral fissures toward the ears, hypertelorism, long eyelashes, high-arched eyebrows, prominent nose, and malpositioned ears with dysplastic helices. In addition, characteristic skeletal findings are broad, short, terminal phalanges of the thumbs and halluces, and postnatal growth retardation with head circumference below the fiftieth percentile. Dermatologic features include capillary malformations in approximately 50 percent of patients and higher incidence of keloid formation [3] and pilomatricomas [4].
There may be systemic involvement of multiple organ systems. Of children with RTS, 24-38 percent have cardiac abnormalities, which include atrial and ventricular septal defects, patent ductus arteriosus, coarctation of the aorta, pulmonic stenosis, and bicuspid aortic valve abnormalities [5]. Feeding difficulties and gastroesophageal reflux disease require aggressive treatment in young children to prevent nutritional- and growth deficits. Cryptorchidism affects 78-100 percent of male infants [6]. There is an increased incidence of benign and malignant tumors as well as leukemia and lymphoma [3, 7]. Other organ systems that may be involved include audiologic, ophthalmic, endocrine, neurologic, and respiratory systems [6].
Rubinstein-Taybi syndrome is associated with a mutation in the CREB-binding protein gene (CREBBP) located on chromosome 16p13.3. CREBBP has been identified as a nuclear protein that participates as a coactivator in cyclic AMP-regulated gene expression. The precise relation between microdeletion in the CREBBP and the phenotype of Rubinstein-Taybi has yet to be elucidated.
References
1. Rubinstein JH, Taybi H. Broad thumbs and toes and facial abnormalities. Am J Dis Child 1963;105: 588.2. Spitz JL. Genodermatoses: a full-color clinical guide to genetic skin disorders. Lippincott, New York: New York, Williams & Wilkins 1996, pp.308-9.
3. Siraganian P, et al. Keloids and neoplasms in the Rubinstein-Taybi syndrome. Med Pediatr Oncol 1989; 17: 485.
4. Masuno M, et al. Pilomatrixomas in Rubinstein-Taybi syndrome. Am J Med Genet 1998; 77: 81.
5. Stevens C, Bhakta M. Cardiac abnormalities in the Rubinstein-Taybi syndrome. Am J Med Genet 1995; 59: 346.
6. Wiley S, et al. Rubinstein-Taybi syndrome medical guidelines. Am J Med Genet 2003; 119A: 101.
7. Miller R, Rubinstein JH. Tumors in Rubinstein-Taybi syndrome. Am J Med Genet 1995; 56: 112.
8. Petrij F, et al. Diagnostic analysis of the Rubinstein-Taybi syndrome: five cosmids should be used for microdeletion detection and low number of protein truncating mutations. J Med Genet 2000; 37:168.
© 2004 Dermatology Online Journal

