Pityriasis rotunda
Published Web Location
https://doi.org/10.5070/D37w41t9f8Main Content
Pityriasis rotunda
Erick A. Mafong
Dermatology Online Journal 8(2): 15
From New York University Department of DermatologyHistory
This 35 year old man complained of a problem on the skin of the torso for two years. The patient, who is from West Africa, noticed the appearance of several, dark, scaly, round spots on his torso for the past two years. The lesions were asymptomatic and have remained stable in terms of size and location. He denies any systemic systems. A review of systems, past medical history, and family history were not contributory. No seasonal variation in the condition was noted. Previously, treatment with emollients had been unsuccessful.
Physical Examination
Circular, scaly, hyperkeratotic patches, 2 to 5-cm in diameter were present on the torso. The lesions were darker than the surrounding skin.
Laboratory Data
A complete blood count and serum chemistry panel were normal. A purified protein derivative tuberculin test was negative. A potassium hydroxide preparation failed to show fungal elements
Histopathology:
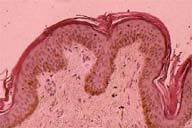 |
| Figure 1 |
|---|
There is slight psoriasiform hyperplasia with compact orthokeratosis and a diminished granular layer.
Comment
Pityriasis rotunda is a relatively rare condition that was first described as pityriasis circinata in 1913 in Japanese patients. Since then, its occurrence has been documented worldwide. It is characterized by asymptomatic, well-demarcated, circular, scaly patches, which are usually located on the torso and proximal portions of the extremities. In dark-skinned individuals, the number of lesions varies from one to 28 while in lighter-skinned patients, the lesions are more numerous. A proportion of patients with pityriasis rotunda has associated systemic illnesses that include malignant conditions, such as leukemia, lymphoma, carcinoma of the esophagus and stomach, and ademona of the prostate; malnutrition; tuberculosis; and hepatic and pulmonary disease.
The cause of primary rotunda is unknown. Generally, this condition is considered by many to be a form of acquired ichthyosis. A genetic predisposition and the presence of infection, malignant conditions, or malnutrition have been suggested. Familial cases have also been described in which an autosomal dominant inheritance appears to be present. Curiously, almost all light-skinned patients reported in the literature appear to be free of associated illnesses.
Treatment of pityriasis rotunda is difficult. Some patients respond to emollients. Others note a seasonal variation in their condition, with improvement during the summer and recurrence during the winter. Success with both topical and systemic retinoids has been reported. The lesions may also resolve spontaneously, particularly when the associated systemic condition is treated.
References
Toyama T. Uber eine bisher noch nicht beschriebene dermatose: pityriasis circinata. Arch Dermatol Syphiligr 116:243, 1913Weiss RM. Pigmented lesions in a patient with pulmonary tuberculosis. Arch Dermatol 127:1221, 1991
Grimalt R, et al. Pityriasis rotunda: report of a familial occurrence and review of the literature. J Am Acad Dermatol 31:866, 1994
Gibbs S. Pityriasis rotunda in Tanzania. Br J Dermatol 135:490, 1996 Pinto GM, et al. Pityriasis rotunda. Cutis 58:406, 1996
© 2002 Dermatology Online Journal

