Disseminated cutaneous rhinosporidiosis
Published Web Location
https://doi.org/10.5070/D37fn1t1nqMain Content
Disseminated cutaneous rhinosporidiosis
Rashmi Kumari MBBS, Chandrashekar Laxmisha MD, Devinder M Thappa MD DHA MNAMS
Dermatology Online Journal 11 (1): 19
Department of Dermatology and STD, JIPMER, Pondicherry - 605 006, India. dmthappa@vsnl.net
Abstract
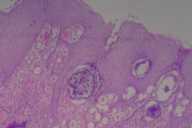
Rhinosporidiosis is a chronic granulomatous disorder caused by Rhinosporidium seeberi. It frequently involves the nasopharynx and occasionally affects the skin. We herewith report a 55-year-old man who has disseminated cutaneous rhinosporidiosis. He presents with multiple reddish lesions over the nose of 10 year's duration. In the past year, he develops skin lesions over the right arm and over back. Histopathological examination of the skin biopsy specimen from the representative cutaneous lesions shows hyperplastic epithelium with numerous globular cysts of varying shape, representing sporangia in different stages of development. His serology for HIV infection by ELISA is negative. On the basis of these clinical and histopathological findings, a diagnosis of nasal rhinosporidiosis with cutaneous dissemination is made.
Introduction
Rhinosporidiosis is a chronic granulomatous disorder caused by Rhinosporidium seeberi. The organism has never been isolated in vitro, and its taxonomic position is unclear. The disease is endemic in India and Sri Lanka but has also been reported from the United States, South America, and Iran [1, 2, 3]. It is more common in adult men and is possibly transmitted to humans by direct contact with spores through dust, through infected clothing or fingers, and through swimming in stagnant waters [2]. Rhinosporidiosis frequently involves the nasopharynx (70 %) presenting as a painless, friable, polypoidal growth, which may hang anterior to the nares or posteriorly into the pharynx. The lesions are pink or purple-red and studded with minute white dots, which are sporangia containing the spores [1, 3]. Nasal obstruction and bleeding are the most common symptoms. The conjunctiva and lacrimal sac are involved in 15 percent of cases. Occasionally, rhinosporidiosis affects the lips, palate, uvula, maxillary antrum, epiglottis, larynx, trachea, bronchus, ear, scalp, vulva, vagina, penis, rectum, and the skin. We herewith report a 55-year-old man with disseminated cutaneous rhinosporidiosis.
Clinical synopsis
A 55-year-old man presents with a 10-year history of multiple reddish lesions on the nose. Over the past year he has developed skin lesions on the right arm and the back. He indicates that he was healthy 10 years prior when he develops a reddish, friable lesion in the right nostril. The lesion is associated with anosmia, nasal block, hemorrhage, and crusting. He develops a similar lesion over the left nostril 2 years later. He describes swimming in ponds in his village. An otolaryngologist excises the lesion; he is started on dapsone (100 mg per day). He stops the treatment after a few months. The lesions recur after a few years in the same areas. On examination a solitary, pedunculated reddish growth (4 × 3 cm) with hemorrhagic crusting is seen on the left ala nasi. On anterior rhinoscopy reddish friable polyps studded with tiny white dots are seen. Examination of the nose and palate is normal. A similar pedunculated growth (2 × 1 cm) is seen on the lumbar area of back. A 1-cm verrucous plaque is seen on the flexor aspect of right forearm.
|

|
| Figure 1 | Figure 2 |
|---|---|
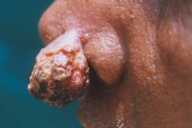
| Pedunculated lesion on the tip of nose (Fig. 1). | |
| Hyperpigmented verrucous pedunculated lesion on the back (Fig. 2). | |

|
| Figure 3 |
|---|
| Discoid verrucous plaque over the forearm |
Histopathological examination of the skin biopsy specimen from the representative cutaneous lesions shows hyperplastic epithelium with numerous globular cysts of varying shape, representing sporangia in different stages of development. His serology for HIV infection by ELISA is negative. A final diagnosis of nasal rhinosporidiosis with cutaneous dissemination is made.
All the cutaneous lesions are excised and he is then referred to an otolaryngologist for further management. He is restarted on dapsone (100 mg po per day).
Discussion
Rhinosporidiosis is usually limited to the surface epithelium of nasal mucosa, but, rarely, wide dissemination with visceral involvement can occur [4]. The nasal lesions start as an often-pruritic papule that grows into an erythematous polypoidal mass that may cause obstruction of the nose and nasopharynx. Small cysts and pseudocysts develop and may discharge a combination of pus, mucus, and organisms, creating tiny white dots on the lesion's surface and giving lesions a characteristic strawberry-like appearance [5].
Cutaneous lesions in rhinosporidiosis are not very common and usually start as friable papillomas that become pedunculated [4]. Cutaneous rhinosporidiosis may also present as warty papules and nodules with whitish spots, crusting, and bleeding on the surface. Three types of skin lesions can occur: (1) satellite lesions, in which skin adjacent to the nasal rhinosporidiosis is involved secondarily; (2) generalized cutaneous type with or without nasal involvement, occurring through hematogenous dissemination of the organism; (3) primary cutaneous type associated with direct inoculation of organisms on to the skin. Careful inspection of the surface of warty lesions and the presence of typical nasopharyngeal lesions usually help in the diagnosis of cutaneous rhinosporidiosis. The various differential diagnoses include warts, verrucous tuberculosis and granuloma pyogenicum [4]. Our patient has a satellite lesion adjacent to the nose, and the rest of the cutaneous lesions may represent autoinoculation.
The diagnosis can easily be clinched by performing a Giemsa-stained imprint smear [2]. Fine-needle aspiration cytology from the lesion may be an additional diagnostic tool [1]. Histopathology reveals enormous number of mycotic elements in the subepithelial connective tissue. These elements consist of sharply defined globular thick-walled cysts (sporangia), up to 0.5 mm in diameter, which contain numerous rounded endospores, 6-7 µ in diameter. Immature and collapsed sporangia are also present. Occasionally microabscesses may form. This disease must be differentiated from coccidiodomycosis whose different clinical presentation and smaller sporangia size (less than 60 µ in diameter) allow for an easy distinction [5].
Surgical removal and electrodesiccation are the treatments of choice [4]. Dapsone may arrest the maturation of sporangia and accelerate degenerative changes in them. The effete organisms are then removed by an accelerated granulomatous response.
References
1. Ramanan C, Ghorpade A. Giant cutaneous rhinosporidiosis. Int J Dermatol 1996 Jun;35:441-2. PubMed2. Kamal MM, Luley AS, Mundhada SG, Bohhate SK. Rhinosporidiosis. Diagnosis by scrape cytology. Acta Cytol 1995 Sep-Oct;39(5):931-5. PubMed
3. Thappa DM, Venkatesan S, Sirka CS, Jaisankar TJ, Gopalkrishnan, Ratnakar C. Disseminated cutaneous rhinosporidiosis. J Dermatol 1998 Aug;25(8):527-32. PubMed
4. Vijaikumar M, Thappa DM, Karthikeyan K, Jayanthi S. Verrucous lesion of the palm. Postgrad Med J 2002 May;78(919):302,305-6. PubMed
5. Longley BJ. Fungal diseases. In: Elder D, Elenitsas R, Jaworsky C, Johnson B. Lever's Histopathology of the skin. 8th edn. Philadelphia: Lippincott Williams and Wilkins1997: 517-552.
© 2005 Dermatology Online Journal