Reticulated lesion as an early diagnostic sign for giant cell arteritis
Published Web Location
https://doi.org/10.5070/D37bn752mdMain Content
Reticulated lesion as an early diagnostic sign for giant cell arteritis
Nicholas C Uffelmann, Jessica Kozel MD, Sofia B Chaudhry MD, Claudia I Vidal MD PhD
Dermatology Online Journal 18 (6): 6
Department of Dermatology, Saint Louis University, Saint Louis, MissouriAbstract
We report a case of giant cell arteritis (GCA) in an elderly woman. The patient presented to her dermatologist with a reticulated, purpuric patch on her frontal-temporal scalp and forehead that was associated with unilateral head pain. A punch biopsy of the lesion was suspicious for GCA, which was later confirmed by temporal artery biopsy. This case highlights a potential early cutaneous finding of GCA that may aid the clinician in the diagnosis before more severe complications occur.
Introduction
Giant cell arteritis (GCA), also known as temporal arteritis, is a systemic, granulomatous vasculitis that affects medium to large caliber vessels. The incidence of this disease is approximately 20/100,000 and primarily occurs in Caucasian females of Northern European descent over the age of 50 [1]. Common symptoms include localized headache, hyperesthesia, jaw claudication, fever, malaise, and vision disturbances. Scalp necrosis in the setting of GCA is a rare manifestation that is thought to be the result of progressive disease and delay in diagnosis [2]. We report a patient that was diagnosed with GCA after an initial presentation resembling retiform purpura, a pattern that we feel precedes the development of cutaneous necrosis.
Case report
 |
| Figure 1 |
|---|
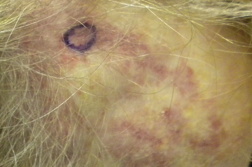
| Figure 1. Initial presentation of the unilateral, reticulated purpuric patch on the right frontal-temporal scalp and forehead. |
A 77-year-old Caucasian female presented to her dermatologist with a one-month history of unilateral head pain associated with a skin lesion. She had previously been treated with oral antibiotics for a presumed sinus infection with no relief. On physical exam, she had a tender, unilateral, reticulated purpuric patch on the right frontal-temporal scalp and forehead (Figure 1). Laboratory data taken a day prior showed she had a C-reactive protein (CRP) of 6.17 mg/L.
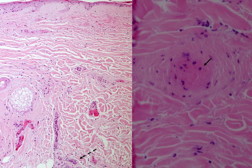
A punch biopsy of the purpuric area revealed necrosis of the eccrine and sebaceous glands with overlying hypoxic epidermal changes. The superficial dermis showed extravasated erythrocytes and small caliber vessels appeared congested. Rare fibrin thrombi were noted within small caliber vessels as well (Figure 2A-2B).
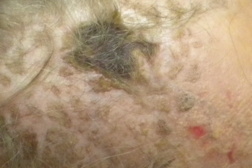
Given the anatomic location, history of pain, and patient demographics, a diagnosis of giant cell arteritis (GCA) was suspected. Laboratory data revealed an erythrocyte sedimentation rate (ESR) of 110 mm/hr. The patient was started on prednisone (60 mg/day) and referred for temporal artery biopsy, which confirmed the diagnosis of GCA. At her six-week follow up, the involved area of her scalp had progressed to necrosis with surrounding alopecia despite treatment with glucocorticoids (Figure 3). She denied experiencing any changes in vision. Throughout this time the patient was followed by serial ESRs, with her most recent level decreased to 13 mm/hr. She did not have a follow-up CRP. She is undergoing a slow taper off the prednisone and is currently taking 5 mg of prednisone orally.
Discussion
Retiform purpura consists of purpuric lesions in a serpentine or stellate pattern caused by a complete blockage of blood flow in the dermal and subcutaneous vasculature, often accompanied by extravasation of blood and cutaneous necrosis. The differential diagnosis of retiform purpura is broad. However, the two primary etiological categories are vasculitis (small and medium vessel disease) and microvascular occlusion syndromes related to thrombotic, embolic, or infectious diseases [3]. The cause of this reticulated patch in our patient was vasculitis, specifically giant cell arteritis. Therefore, it is important to recognize that cutaneous findings may aid clinicians in the diagnosis of giant cell arteritis. Prior reports have found that scalp necrosis can be associated with GCA, often indicating extensive vessel involvement [4]. The lack of clinical ulceration initially, as in our patient, may make the diagnosis more challenging. We feel the presentation of a mottled pattern that resembles retiform purpura on the scalp may be the preceding physical exam finding before necrosis ensues. This is supported by the time elapsed from the initial onset of symptoms to the diagnosis and onset of necrosis in this patient. Interestingly, scalp necrosis in the setting of GCA has been reported previously “on a background of lividoid change”; however, it was not clear from the prior report if the lividoid change described preceded the necrosis or if they occurred simultaneously [5].
Our patient presented with only a 1-month symptom history, compared to a reported average of 2.9 months from symptom onset to scalp necrosis [2]. Furthermore, the occurrence of necrosis after initiation of high dose glucocorticoid therapy has been reported [6].
The importance of early diagnosis and treatment of GCA is crucial to improving patient outcomes. If left untreated, GCA can be associated with severe complications, including tongue necrosis and permanent vision loss [7]. In fact, 30 percent of patients with GCA that progressed to scalp necrosis have reported vision loss [2]. Treatment with high dose corticosteroids (1-2 mg/kg/day) is recommended when the diagnosis of GCA suspected. Prompt initiation of therapy not only leads to improvement of cutaneous manifestations, but also has been shown to increase visual recovery [2, 7].
References
1. Salvarani C, Crowson CS, O’Fallon WM, Hunder GC, Gabriel SE. Reappraisal of the epidemiology of giant cell arteritis in Olmsted County, Minnesota, over a fifty year period. Arthritis Rheum. 2004; 51(2): 264-268. [PubMed]2. Tsianakas A, Ehrchen JM, Presser D, et al. Scalp necrosis in giant cell arteritis: case report and review of the relevance of this cutaneous sign of large-vessel vasculitis. J Am Acad Dermatol. 2009; 61(4): 701-706. [PubMed]
3. Wysong A, Venkatesan P. An approach to the patient with retiform purpura. Dermatol Ther. 2011; 24(2): 151-172. [PubMed]
4. Currey J. Scalp necrosis in giant cell arteritis and review of the literature. Br J Rheumatol. 1997; 36(7): 814-816. [PubMed]
5. Campbell FA, Clark C, Holmes S. Scalp necrosis in temporal arteritis. Clin Exp Dermatol. 2003; 28(5): 488-490. [PubMed]
6. Brick KE, Cook-Norris RH, Wetter DA, Warrington KA. Scalp necrosis in giant cell arteritis after initiation of therapeutic corticosteroids. J Am Acad Dermatol. 2010; 63(2): 343-344. [PubMed]
7. Kawasaki A, Purvin V. Giant Cell arteritis: an updated review. Acta Ophthalmol. 2009; 87(1): 13-22. [PubMed]
© 2012 Dermatology Online Journal