The Meyerson phenomenon in a teenager
Published Web Location
https://doi.org/10.5070/D37bm1s4wmMain Content
The Meyerson phenomenon in a teenager
Carmelo Schepis MD, Maddalena Siragusa MD
Dermatology Online Journal 14 (2): 28
Unit of Dermatology, Oasi Institute (IRCCS), Troina, Italy. cschepis@oasi.en.it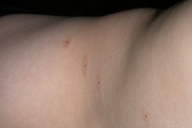 |
| Figure 1 |
|---|
| Figure 1. Multiple perinevic dermatitis over the trunk |
We evaluated a 12-year-old teenager because of the almost simultaneous occurrence, approximately 1 month earlier, of erythematous papulosquamous changes around small acquired nevi. On clinical examination we found at least seven nevi on the trunk (1.5-2.0 mm in diameter) surrounded by a ring of inflammation with irregular and not well defined margins (Fig. 1). We made a diagnosis of Meyerson phenomenon for which we did not require further exams and invited the parents to return after 6 months for a followup visit.
Meyerson (1971) firstly described two patients with a papulosquamous eruption surrounding some of the nevi on the trunk and limbs [1]. He reported the histology for both cases showing acanthosis, spongiosis, and parakeratosis associated with a lymphocytic perivascular infiltrate in the upper dermis. Meyerson hypothesized that these findings are an atypical form of pityriasis rosea. In subsequent reports, this eruption has been termed Meyerson phenomenon (MP)[2, 3], Meyerson nevus [4, 5], halo dermatitis, and halo eczema [6, 7].
Although Meyerson postulated this eruption to be the localization of pityriasis rosea around melanocytic nevi, that association is not clear. Even though pityriasis is common, MP is rare [8]. It more often involves a single nevus but may affect multiple nevi. Moreover, MP may occur around normal nevi, atypical nevi [2, 9], cutaneous tumors such as seborrheic keratoses [10], basal cell carcinoma, squamous cell carcinoma, dermatofibroma [11], keloid, stucco-keratosis, and insect bites [9].
The histological analysis shows parakeratosis, acanthosis and sometimes epidermal spongiosis. The upper dermis has a perivascular lymphocytic infiltrate, sometimes with eosinophils [2, 4, 9, 10]. Thus, the histological exam has little value for the diagnosis of this condition.
The pathogenesis of MP is still unclear, even if the upregulation of ICAM-1 seems to suggest a role for these cytokines [12]. The lack of the expression of interleukin-2 receptor by T lymphocytes in the infiltrate suggests that the process differs from that of allergic contact dermatitis [13].
Meyerson phenomenon is rarely encountered in adults and even more rarely in children; some authors hypothesize that a greater awareness of this phenomenon by specialists would result in more numerous reports [14].
Meyerson phenomenon does not require treatment; it tends to disappear with time. Local application of cortisone [2, 3] can be taken employed in those cases with a particularly intense inflamation and pruritus [9]. For the differential diagnosis, it is important to consider halo nevus [2], pityriaris rosea [1], and the roseola of syphilis.
In conclusion, MP is rare event with an unclear pathogenesis and a benign and non recurring course.
References
1. Meyerson LB. A Peculiar papulosquamous eruption involving pigmented nevi. Arch Dermatol 1971; 103: 510-512.2. Kus S, Ince U, Candan I, Gurunluoglus R. Meyerson phenomeneon associated with dysplastic compound nevi. JEADV 2006; 350-351.
3. Hofer T. Meyerson phenomenon within a nevus flammeus. Dermatology 2002; 205: 180-183.
4. Krischer J, Pechère M, Salomon D, Harms M, Chavaz P, Saurat JH. Interferon alfa 2b-induced Meyerson's nevi in a patient with dysplastic nevus syndrome. J Am Acad Dermatol 1999; 40: 105-106.
5. Crovato F, Nazzari G, Gambini C. Meyerson's naevi in pityriasis rosea. Br J Dermatol 1989; 120: 318-319.
6. Brenan J, Kossard S, Krivanck J. Halo eczema around melanocytic nevi. Int J Dermatol 1985; 24: 226-229.
7. Worret WI. Halo-ekzeme um Nävuszellnävi (Meyerson-Nävi). Hautarzt 1990;41: 262-264.
8. Stulberg DL, Wolfrey J. Pityriasis Rosea. Am Fam Phisician 2004; 69: 87-91.
9. Elenitsas R, Halpern AC. Eczematous halo reaction in atypical nevi. J Am Acad Dermatol 1996; 34: 357-361.
10. Tegner E, Björnberg A, Jonsson N. Haolo dermatitis around tumours. Acta Derm Venereol Suppl (Stockh) 1990; 70: 31-34.
11. Gallais V, Lacour JPH, Perrin C, Haliqua B, Ortonne JP. Haolo eczématiforme autor d'un histiocytofibrome : phénomène de Meyerson. Ann Dermatol Venereol 1993 ; 120 : 617-620.
12. Feal-Cortizas C, Vargas-Diez E, Buezo GF, Aragües M. Meyerson's nevus immunohistochemical finding in two cases. Australas J Dermatol 1997; 38(S2): 222.
13. Fernandez Herrera JM, Aragües Montanes M, Fraga Fernandez J, Diez CA. Halo eczema in melanocytic nevi. Acta Derm Venereol 1988; 68: 161-163.
14. Shifer O, TchetchiK R, Glazer O, Metzker A. Halo dermatitis in children. Pediatric Dermatol 1992; 9: 275-277.
© 2008 Dermatology Online Journal

