Epidermodysplasia verruciformis associated with HPV 10
Main Content
Epidermodysplasia verruciformis associated with HPV 10
Amir Zahir1 MD, Lauren Craig2 BA, Peter Rady3 MD PHD, Stephen Tyring3 MD PHD MBA, Alison Ehrlich1 MD MHS
Dermatology Online Journal 19 (4): 2
1. Department of Dermatology, Medical Faculty Associates, George Washington University, Washington, DC2. George Washington University School of Medicine and Health Sciences, Washington, DC
3. Department of Dermatology, University of Texas Medical School at Houston, Houston, Texas
Abstract
Epidermodysplasia verruciformis (EV) is a rare, inherited dermatologic condition demonstrating an increased susceptibility to specific HPV genotypes, resulting in both benign and malignant skin lesions. Epidermodysplasia verruciformis lesions are frequently described as pityriasis versicolor-like scaly macules, flat wart-like papules, or verrucous and seborrhic keratosis-like papules and plaques. Acquired EV has been described in patients with HIV and in those who are on immunosuppressive therapy. We discuss a patient with congenital EV who presents with skin lesions associated with HPV 10, a less frequently cited causative subtype, and histological findings that are not classic for EV.
Introduction
Epidermodysplasia verruciformis (EV) is an inherited disease characterized by an increased susceptibility to certain HPV subtypes, often manifesting as verruca plana-type lesions with mild to moderate hyperkeratosis, acanthosis, and enlarged vacuolated keratinocytes with perinuclear halos and blue-gray cytoplasmic pallor [1]. The term “acquired EV” describes a syndrome nearly identical to congenital EV that afflicts immunocompomised patients [2]. HPV types that are typically associated with EV include 5, 8, 9, 12, 14, 15, 17, 19 to 25, 36, 38, 47, and 50 [3]. HPV 5 and 8 have been described frequently, based on their potential to cause malignant lesions [4]. In this report, we discuss a presentation of EV and the detection of a less frequently cited causative HPV subtype, HPV 10, that produced histologic findings that are not classic for EV.
Case report
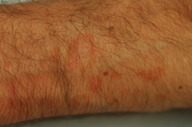 |
| Figure 1 |
|---|
A 42-year-old male presented to our clinic with a thirty-year history of reddish-brown papules on the extensor surfaces of his arms and anterior legs. He was treated with liquid nitrogen nine years prior and the treatment resulted in central clearing of his lesions. The physical examination revealed erythematous papules and macules on the extensor surfaces of his forearms (Figure 1). No clinical sign of cutaneous carcinoma was present. He has no personal history of skin cancer or immunosuppression. The patient was adopted and does not know if he has a family history of recalcitrant warts or skin cancer. A 4 mm punch biopsy of a papule on his left arm was performed. Microscopic examination revealed epidermal acanthosis, hyperkeratosis, vacuolation of superficial keratinocytes in the granular layer, and mild perivascular infiltrate in the superficial dermis (Figures 2 and 3). These findings are consistent with verruca plana. In situ hybridization was performed to detect multiple HPV subtypes. The tissues were analyzed for HPV types 2, 5, 6, 8, 11, 16, 18, 30, 31, 33, 35, 42, 43, 44, 45, 51, 52, 68, and 70. The results were all negative. HPV typing by nested PCR for the detection of epidermodysplasia verruciformis associated HPV types using an EV-HPV primer system was negative [5].
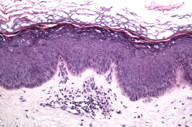 | 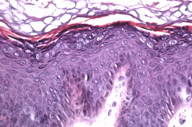 |
| Figure 2 | Figure 3 |
|---|
Single PCR using the GP5+/6+ HPV primer system revealed a putative HPV fragment. The sequencing of the isolated PCR products and the computer-assisted analysis (NCBI-BLAST) of the PCR products identified HPV type 10 DNA [6].
Discussion
Epidermodysplasia verruciformis (EV) is a rare, inherited dermatologic condition in which patients have an increased susceptibility to specific HPV genotypes, resulting in both benign and malignant lesions. Although it has an autosomal recessive transmission in most cases, x-linked recessive and autosomal dominant forms also exist [7]. The disease was first described by Lewandowski and Lutz in 1922 and is characterized by both impaired immunity and viral oncogenesis [4]. The term “acquired EV” has been used to describe a condition with clinical features similar to EV that occurs in immunocompromised patients, specifically those with HIV or those on immunosuppressive therapy [2].
Epidermodysplasia verruciformis usually begins in childhood but may also occur later in life [8]. It presents as erythematous to flesh colored scaly macules or as flat, wart-like papules located on the dorsum of the hands, extremities, face, and neck. These lesions range in pigmentation and often amalgamate to form patches and plaques. Verrucous and seborrheic keratosis-like lesions frequently appear on the forehead, neck, and trunk [4, 8, 9].
There are multiple HPV types associated with EV. The benign form of the disease may present with only flat warts associated with HPV 3 and 10. These two subtypes are non-oncogenic and infect normal hosts [10]. Other HPV types that are more commonly associated with EV include 5, 8, 9, 12, 14, 15, 17, 19 to 25, 36, 38, 47, and 50 [3]. Epidermodysplasia verruciformis caused by these subtypes usually present with pityriasis versicolor, verrucous, and seborrheic keratosis-like lesions [8, 9]. Malignant transformation has been associated more specifically with HPV-5, HPV-8, and HPV-14d [4]. Approximately 30-50 percent of patients with EV develop squamous cell carcinoma usually during the fourth decade of life, most commonly on sun-exposed surfaces [1, 11].
Epidermodysplasia verruciformis has been linked to the EV1 and EV2 loci on chromosomes 17 and 2, respectively. Mutations have been identified in both the EVER1 and EVER2 genes, which are located on the EV1 locus [3]. These genes code for zinc containing transmembrane proteins hypothesized to be integral to the immune response against HPV. Mutations in these proteins are thought to lead to the increased susceptibility to HPV infection and the increased propensity for malignant change observed in EV patients. However, these EVER mutations are not found in all patients with EV [9]. Patients with acquired EV are susceptible to the same strains of HPV infecting those with congenital EV. In contrast to congenital EV, the lesions of acquired EV are less likely to progress into skin cancer. Epidermodysplasia verruciformis - HPV types have been isolated from squamous cell carcinomas in immunocompromised patients, but a direct progression to the development of malignancy in acquired EV lesions has not been firmly established. This is likely related to a lack of long term follow up and small patient population [2].
The classic histological finding of epidermodysplasia verruciformis is a verruca plana-type lesion with mild to moderate hyperkeratosis, acanthosis, and enlarged vacuolated keratinocytes with perinuclear halos and blue-gray cytoplasmic pallor [1].
The classic histologic features of EV are not seen in all patients who have this condition. In a study by Nuovo et al in which skin biopsies from patients with lesions similar to those seen in EV were examined histologically and for the presence of HPV DNA by standard and PCR in situ hybridization, it was determined that as the viral DNA copy number increased, infected tissues exhibited cells with prominent blue-gray pallor and perinuclear halos in areas of acanthosis. They also speculated that cells containing an irregular granular layer and rare perinuclear halos could be the earliest recognizable histological changes induced by the virus. They concluded that there is a wide spectrum of histological changes that can be seen in patients with EV and it was uncommon for patients with EV to have the classic histologic features [1].
In situ hybridization for the detection of HPV types 2, 5, 6, 8, 11, 16, 18, 30, 31, 33, 35, 42, 43, 44, 45, 51, 52, 68, and 70 was negative in our patient. This test has a sensitivity of 89.5 (77.4–95.7) [12]. The HPV DNA in our sample could have contained copy numbers less than 10 viral genomes per cell, which is the threshold for detection of in situ hybridization [13]. PCR in situ hybridization can be used to amplify HPV types associated with EV not detected by standard in situ hybridization [1]. HPV typing by nested PCR for the detection of EV associated HPV types using an EV-HPV primer system was negative [5]. Single PCR using the GP5+/6+-HPV primer system was positive for HPV 10 [6].
Our patient does not have the classic histological features of EV (1). He also does not have a history of HIV or immunosuppressant therapy, ruling out the possibility of acquired EV. Instead, he has a form of congenital EV induced by HPV-3 and HPV-10, which consists of multiple plane wart-type lesions that do not have a tendency for malignant transformation [10]. Although plane warts induced by HPV-3 and HPV-10 can occur in patients without EV, they are usually described as erythematous flat topped papules that do not usually grow to confluence. Instead, as seen in our patient, the plane wart-type lesions associated with EV are more abundant, tend to amalgamate, and are generally flatter compared to typical flat warts. The possibility of this patient having EV with high malignant potential was excluded based on the negative HPV subtypes of 5, 8, and 14d. As seen in the study by Nuovo et al and in the above case, EV can present as a spectrum of lesions and the absence of characteristic pathology should not sway a clinician from making the diagnosis and applying treatment [1, 9].
Treatment of EV remains challenging. Patients should be routinely monitored for the development of cutaneous cancers because of its malignant potential [4]. Surgery is the primary option for localized malignancies. For more widespread lesions, alternative treatments have yielded inconsistent results (See Table 1). Sun avoidance and photoprotection are also recommended [14]. Systemic retinoids, including acitretin, etretinate, and isotretinoin, have been used with variable success. Although they have been effective in decreasing the number of EV lesions, recurrence is common upon discontinuation of treatment [7, 15-19]. Interferons given alone or in combination with systemic retinoids have also been effective in treating EV associated warts and squamous cell carcinomas [7, 18, 20]. Maintenance therapy may be needed to prevent relapse [4]. Imiquimod has been used to effectively treat squamous cell carcinomas in patients with EV [21]. It has also been combined with systemic interferons to treat Bowen disease and EV associated lesions [22]. Cimetidine, a histamine 2 antagonist, has shown variable results [23, 24]. Topical 5-aminolevulinic acid photodynamic therapy has been effective in treating EV lesions, but multiple treatments may be needed to prevent relapse [25].
References
1. Nuovo G, Ishag M. The Histologic Spectrum of Epidermodysplasia Verruciformis. The American Journal of Surgical Pathology 2000; 24(10): 1400-1406. [PubMed]2. Rogers HD, Macgregor JL, Nord KM, et al. Acquired epidermodysplasia verruciformis. J Am Acad Dermatol 2009; 60(2): 315-320. [PubMed]
3. Gewirtzman A, Bartlett B, Tyring S. Epidermodysplasia verruciformis and human papilloma virus. Curr Opin Infect Dis 2008; 21: 141-146. [PubMed]
4. Patel T, Morrison K, Rady P, Tyring S. Epidermodysplasia verruciformis and susceptibility to HPV. Disease Markers 2010; 29: 199-206. [PubMed]
5. Berkhout RJ, Tieben LM, Smits HL, Bavinck JN, Vermeer BJ, ter Schegget J. Nested PCR approach for detection and typing of epidermodysplasia verruciformis-associated human papillomavirus types in cutaneous cancers from renal transplant recipients. J Clin Microbiol 1995; 33(3): 690-695. [PubMed]
6. de Roda Husman AM, Walboomers JM, van den Brule AJ, Meijer CJ, Snijders PJ. The use of general primers GP5 and GP6 elongated at their 3' ends with adjacent highly conserved sequences improves human papillomavirus detection by PCR. J Gen Virol 1995; 76: 1057- 1062. [PubMed]
7. Gubinelli E, Posteraro P, Cocuroccia B, Girolomoni G. Epidermodysplasia verruciformis with multiple mucosal carcinomas treated with pegylated interferon alfa and acitretin. Journal of Dermatological Treatment 2003; 14: 184-188. [PubMed]
8. de Oliveira WR, et al. Clinical aspects of epidermodysplasia verruciformis. J Eur Acad Dermatol Venereol 2003; 17(4): 394-398. [PubMed]
9. Sri J, Dubina M, Kao G, Rady P, Tyrking S, Gaspari A. Generalized Verrucosis: A Review of the associated diseases, evaluation, and treatments. J Am Acad Dermatol 2012; 66(2): 292- 311. [PubMed]
10. de Sá NB, Guerini MB, Barbato MT, Di Giunta G, Nunes DH. Epidermodysplasia verruciformis: clinical presentation with varied forms of lesions. An Bras Dermatol 2011; 86(4 suppl 1): 57-60. [PubMed]
11. Majewski S, Jablonska S. Do epidermodysplasia verruciformis human papillomaviruses contribute to malignant and benign epidermal proliferations? Arch Dermatol 2002; 138(5): 649-654. [PubMed]
12. Kelesidis T, Aish L, Steller MA, et al. Human papillomavirus (HPV) detection using in situ hybridization in histologic samples: correlations with cytologic changes and polymerase chain reaction HPV detection. Am J Clin Pathol 2011; 136(1): 119-127. [PubMed]
13. Nuovo G. PCR In Situ Hybridization: Protocols and Applications, 3rd ed. New York, NY: Lippincott-Raven Press, 1997.
14. Lane JE, Bowman PH, Cohen DJ. Epidermodysplasia verruciformis. South Med J 2003; 96: 613-615. [PubMed]
15. Iraji F, Faghihi G. Epidermodysplasia verruciformis: association with isolated IgM deficiency and response to treatment with acitretin. Clin Exp Dermatol 2000; 25(1): 41-43. [PubMed]
16. Lutzner M, Blanchet-Bardon C, Orth G. Clinical observations, virologic studies, and treatment trials in patients with epidermodysplasia verruciformis, a disease induced by specific human papillomaviruses. J Invest Dermatology 1984: 83(1) (suppl 1): 18-25. [PubMed]
17. Al Rubaie S, Breuer J, Inshasi J, Al Saady S, Fathi I. Epidermodysplasia verruciformis with neurological manifestations. Int J Dermatol 1998; 37(10): 766-771. [PubMed]
18. Rallis E, Papatheodorou G, Bimpakis E, Butanska D, Menounos P, Papadakis P. Systemic low-dose isotretinoin maintains remission status in epidermodysplasia verruciformis. J Eur Acad Dermatol Venereol 2008; 22(4): 523-525. [PubMed]
19. Anadolu R, Oskay T, Erdem C, Boyvat A, Terzi E, Gurgey E. Treatment of epidermodysplasia verruciformis with a combination of acitretin and interferon-2a. J Amer Acad Dermatol 2001; 45(2): 296-9. [PubMed]
20. Craven N, Griffiths C. Retinoids in the management of non-melanoma skin cancer and melanoma. Cancer Surv 1996; 26: 267-288. [PubMed]
21. Berthelot C, Dickerson M, Rady P, et al. Treatment of a patient with epidermodysplasia verruciformis carrying a novel EVER2 mutation with imiquimod. J Am Acad Dermatol 2007; 56(5): 882-886. [PubMed]
22. Baskan E, Tunali S, Adim S, Turan A, Toker S. A case of epidermodysplasia verruciformis associated with squamous cell carcinoma and Bowen’s disease: a therapeutic challenge. J Dermatolog Treat 2006; 17 (suppl 1): 179-183. [PubMed]
23. Micali G, Nasca M, Dall’Oglio F, Musumeci M. Cimetidine therapy for epidermodysplasia verruciformis. J Am Acad Dermatol 2003; 48(suppl 2): 9-10. [PubMed]
24. de Oliveira W, Neto C, Rivitti E. The lack of a clinical effect of cimetidine in the treatment of epidermodysplasia verruciformis. J Am Acad Dermatol 2004; 50(6): 14-15. [PubMed]
25. Karrer S, Szeimies R, Abels C, Wlotzke U, Stolz W, Landthaler M. Epidermodysplasia verruciformis treated using topical 5-aminolaevulinic acid photodynamic therapy. Br J Dermatol 1999; 140: 935-938. [PubMed]
© 2013 Dermatology Online Journal


