Sebaceous nevus syndrome: A case report of a child with nevus sebaceus, mental retardation, seizures, and mucosal and ocular abnormalities
Published Web Location
https://doi.org/10.5070/D36wj2q75bMain Content
Sebaceous nevus syndrome: A case report of a child with nevus sebaceus, mental retardation, seizures, and mucosal and ocular
abnormalities
Laura S Boger MD, Smita Awasthi MD, Daniel B Eisen MD
Dermatology Online Journal 18 (9): 5
Department of Dermatology, School of Medicine, University of California, Davis, Sacramento, CaliforniaAbstract
A 12-year-old girl presented with extensive epidermal nevi, new onset seizures, mental retardation, and oral and ocular abnormalities. We briefly review the case and epidermal nevus syndrome (ENS), which is characterized by epidermal nevi occurring in conjunction with neurologic, ocular, skeletal, and/or other system involvement.
History
A 12-year old girl presented to the dermatology clinic for evaluation and treatment of lesions on her scalp, face, and chest, which had been present since birth. The patient also reported new onset seizures, starting three weeks prior to presentation, intermittent difficulty breathing, blurry vision, and diplopia.
Physical examination
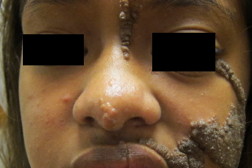
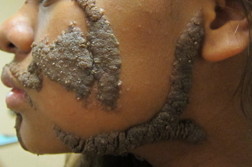
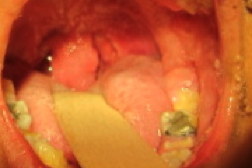
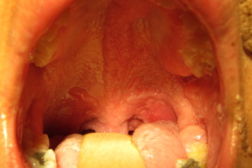
Hyperpigmented, verrucous linear plaques along the lines of Blaschko were distributed along an area extending from the midline chest to the scalp. Examination of the eyes was significant for enlargement of the left eye in comparison with the right and a pink verruciform plaque on the left sclera. Pink, papillomatous plaques were also present on the mucosal lip, hard and soft palates, and tongue. The patient’s uvula was enlarged and pendulous with papillomatous changes.
 |  |
| Figure 1a | Figure 1b |
|---|---|
| Figure 1. (1a and 1b) Hyperpigmented, linear, and arcuate verrucous plaques of the face. Figure 2. (2a and 2b) Uvular hypertrophy and pink plaques of the palate are shown. | |
 |  |
| Figure 2a | Figure 2b |
|---|
Histopathology
 |  |
| Figure 3 | Figure 4 |
|---|---|
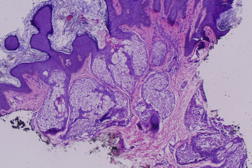
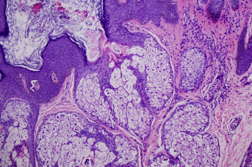
| Figures 3 and 4. Biopsy of the patient’s lesion showed papillated epidermal hyperplasia with enlarged sebaceous lobules. | |
The patient had a biopsy performed at an outside clinic. The slide was obtained for review and showed hyperkeratosis, acanthosis, and papillomatosis with large sebaceous lobules characteristic of a nevus sebaceus.
Discussion
Epidermal nevus syndromes (ENS) are composed of a diverse group of conditions with varying organ involvement, most commonly of the CNS, ocular, and skeletal systems, in association with epidermal nevi. These hamartomas of keratinocytes, apocrine, eccrine, sebaceous, or follicular elements, often follow the lines of Blascko, which are believed to correspond to the lines of embryonic development of the epidermis. The expression of these lines as epidermal nevi has been suspected to relate to genetic mosaicism [1, 2]. Several types of epidermal nevus syndrome are recognized, including linear nevus sebaceous syndrome (LNSS), nevus comedonicus syndrome, Proteus syndrome, Becker nevus syndrome, and CHILD syndrome [1, 2, 3].
LNSS, one of the most commons subtypes of ENS, originally consisted of the triad of a linear nevus, seizures, and mental retardation [4, 5]. However, subsequent reports demonstrated that not all affected individuals had epilepsy or mental retardation and that additional defects involving other neurologic, ocular, skeletal, cardiovascular, and urologic abnormalities may be present [4, 5]. Presently, LNSS generally refers to the association of nevus sebaceus (NS) with brain, eye, and skeletal abnormalities [1, 5].
A multidisciplinary approach to patients with LNSS is strongly advised. In addition to the dermatologist, the team should include a pediatrician, ophthalmologist, neurologist, and a geneticist. Ocular complications include coloboma, strabismus, lipodermoid of the conjunctiva, corneal opacities, and optic nerve defects [1, 5]. Routine brain imaging in children with LNSS is controversial, but electroencephalography, computed tomography, or MRI may be ordered to uncover abnormalities such as brain dysgenesis, cortical dysplasia, hemimegalencephaly, cerebral heterotopia, and low grade gliomas [1, 5]. A bone survey, as well as serum and urine calcium and phosphate, especially for a child with LNSS presenting with bone pain or bowed legs, is recommended to identify skeletal abnormalities such as kyphoscoliosis, limb deformities, and hypophosphatemic rickets [1, 5].
Treatment of NS can be difficult because of the extensive nature of some of the lesions and dermal location of the appendageal structures. Attempted therapies of epidermal nevi (with variable success) include physical modalities such as excision, cryotherapy, electrodessication, CO2 laser, and excision followed by phenol peel [2, 3]. Other treatments have included calcipotriol, tretinoin and 5-fluorouracil, keratolytics, intralesional steroids, and photodynamic therapy [2, 3].
References
1. Happle R. The group of epidermal nevus syndromes Part I. Well defined phenotypes. J Am Acad Dermatol. 2010 Jul;63(1):1-22; quiz 23-4. [PubMed]2. Brandling-Bennett HA, Morel KD. Epidermal nevi. Pediatr Clin North Am. 2010 Oct; 57(5):1177-98. [PubMed]
3. Sugarman JL. Epidermal Nevus Syndromes. Semin Cutan Med Surg. 2007 Dec;26(4):221-30. [PubMed]
4. van de Warrenburg BP, van Gulik S, Renier WO, Lammens M, Doelman JC. The linear naevus sebaceus syndrome. Clin Neurol Neurosurg. 1998 Jun;100(2):126-32. [PubMed]
5. Eisen DB, Michael DJ. Sebaceous lesions and their associated syndromes: Part II. J Am Acad Dermatol. 2009 Oct;61(4):563-78; quiz 579-80. [PubMed]
© 2012 Dermatology Online Journal

