Adenocarcinoma of the lung associated with pityriasis rubra pilaris
Published Web Location
https://doi.org/10.5070/D36vr5r017Main Content
Letter: Adenocarcinoma of the lung associated with pityriasis rubra pilaris
Cara B Garretson MD1, Mac L Machan MD2, Jennifer Krejci-Manwaring MD3, Daniel Aires MD2, Viseslav Tonkovic-Capin MD2
Dermatology Online Journal 17 (11): 14
1. Northwestern Memorial Physicians Group, Chicago, Illinois2. University of Kansas Medical Center Kansas City, Kansas
3. UT Health Science Center, San Antonio, Texas
Abstract
We describe a case of pityriasis rubra pilaris refractory to conventional treatment, found to be associated with an unrecognized primary adenocarcinoma of the lung. Complete resolution of the eruption followed surgical resection of the tumor.
Introduction
Presented is a case of pityriasis rubra pilaris associated with adenocarcinoma of the lung.
Case report
 |
| Figure 1 |
|---|
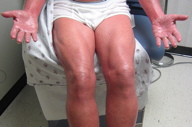
| Figure 1. Generalized erythroderma with waxy palmar keratoderma |
A 66-year-old man presented with a two-month history of pruritic, burning, scaly, erythematous, thin plaques beginning on his trunk and quickly progressing to erythroderma, with small foci of sparing. He also developed painful, confluent, waxy keratoderma of the palms and soles (Figure 1). He reported sweating, chills, shortness of breath on exertion, pedal edema, and a 20 pound weight loss since the onset of the rash. Medications included lisinopril/hydrochlorothiazide, levothyroxine, and aspirin. Family history included a sister with psoriasis. He had a 40-pack-year history of smoking.
 |  |
| Figure 2 | Figure 3 |
|---|---|
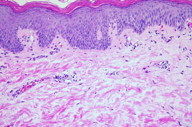
| Figure 2. Psoriasiform acanthosis and mild lymphocytic perivascular infiltrate Figure 3. Complete clearance of the skin and palms after lung tumor removal | |
Skin biopsy revealed psoriasiform acanthosis and a mild lymphocytic perviascular infiltrate consistent with pityriasis rubra pilaris (Figure 2). The erythroderma did not improve with topical or oral steroids, acitretin, emollients, or phototherapy. Over the next month, sweating, chills, and weight loss continued and he developed axillary and inguinal lymphadenopathy. A chest X-Ray and echocardiogram were normal. PPD was negative. A colonoscopy revealed a benign polyp. Complete blood count, basic metabolic panel, liver and thyroid function, and urinalysis were all within normal limits except for a sodium of 131 mMol/L (reference 137-147). Computed tomography showed a 1.6 cm nodule in the left upper lobe of the lung. Fine needle aspiration revealed adenocarcinoma. The patient underwent lobectomy and within several days his skin began to improve. His serum sodium also normalized, suggesting a possible Sydrome of Inappropriate Antidiuretic Hormone (SIADH), although this is generally described only with small cell carcinoma of the lung. One week post-operatively his skin was clear except for a few small areas of desquamation (Figure 3).
Comment
Although the cause of pityriasis rubra pilaris (PRP) is unknown, an autoimmune etiology has been proposed. Reported associations include autoimmune and rheumatologic diseases as well as infections [1, 2]. Human immunodeficiency virus (HIV) now has its own subgroup in the PRP classification [3]. Because of response to oral retinoids, another hypothesized etiology of PRP involves abnormal vitamin A metabolism or dysfunction of keratinization [1]. PRP has been linked with solid and hematologic malignancies including cutaneous squamous cell carcinoma, Merkel-cell carcinoma [4], leukemia [5], bronchogenic carcinoma, hepatocellular carcinoma and laryngeal carcinoma [6]. It can be difficult to determine if “paraneoplastic” PRP is coincidental or is truly associated with an underlying malignancy. Because our patient’s disease was recalcitrant and worsening despite therapy, a malignancy work-up was pursued. Of note, his chest x-ray was negative but the CT scan identified a small lung nodule. The patient’s rapid improvement following surgery supports the diagnosis of lung adenocarcinoma-associated paraneoplastic PRP. When suspicion is high and there are strong risk factors, an escalating search for internal malignancy may be beneficial.
ACKNOWLEDGEMENT: We are indebted to Garth Fraga MD.
References
1. Albert MR, Mackool BT. Pityriasis rubra pilaris. Int J Dermatol. 1999 Jan;38(1): p. 1-11. [PubMed]2. Chan H, Liu FT, Naguwa S. A review of pityriasis rubra pilaris and rheumatologic associations. Clin Dev Immunol. 2004 Mar;11(1): p. 57-60. [PubMed]
3. Miralles ES, Núñez M, De Las Heras ME, Pérez B, Moreno R, Ledo A. Pityriasis rubra pilaris and human immunodeficiency virus infection. Br J Dermatol. 1995 Dec;133(6): p. 990-3. [PubMed]
4. Huynh NT, Hunt MJ, Cachia AR, Veness MJ. Merkel cell carcinoma and multiple cutaneous squamous cell carcinomas in a patient with pityriasis rubra pilaris. Australas J Dermatol. 2002 Feb;43(1): p. 48-51. [PubMed]
5. Reinhardt LA, Rosen T. Pityriasis rubra pilaris as the initial manifestation of leukemia. Cutis. 1983 Jan;31(1): p. 100-2. [PubMed]
6. Batinac T, Kujundzić M, Peternel S, Cabrijan L, Troselj-Vukić B, Petranović D. Pityriasis rubra pilaris in association with laryngeal carcinoma. Clin Exp Dermatol. 2009 Dec;34(8): p. e917-9. [PubMed]
© 2011 Dermatology Online Journal

