Linear syringocystadenoma papilliferum: An uncommon event with a favorable prognosis
Published Web Location
https://doi.org/10.5070/D36tz6g6bbMain Content
Linear syringocystadenoma papilliferum: An uncommon event with a favorable prognosis
Antonio Martorell-Calatayud MD1, Virginia Sanz-Motilva MD2, Maria Angeles Garcia-Sales MA MD3, Calatayud-Blas A MD3
Dermatology Online Journal 17 (8): 5
1. Dermatology Department, Hospital General de Requena, Valencia, Spain. antmarto@hotmail.com2. Dermatology Department, Hospital 12 de Octubre, Madrid, Spain
3. Pathology Department, Hospital General de Requena, Valencia, Spain
Abstract
Syringocystadenoma papilliferum (SCAP) is an uncommon cutaneous adnexal tumor of uncertain histogenesis. Various authors have postulated that the tumor differentiates toward apocrine gland, eccrine gland, or the apo-eccrine gland. We present a patient with an unusual linear form.
Introduction
Syringocystadenoma papilliferum (SCAP) is an uncommon cutaneous adnexal tumor of uncertain histogenesis. Various authors have postulated that the tumor differentiates toward apocrine gland, eccrine gland, or the apo-eccrine gland [1].
The linear form is uncommon and generally involves the neck.
 |
| Figure 1 |
|---|
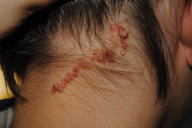
| Figure 1. Linear vesicle-like lesions on the neck |
Most cases of SCAP present as solitary lesions and occur in the head and neck region, often in association with a nevus sebaceus [1, 2]. The development of multiple SCAP lesions in the same patient is a rare event and a linear arrangement following Blaschko lines is exceptional. Thus, epidemiological, clinical, histopathological features and possible systemic associations in patients with linear SCAP are not well studied.
We report a case of linear SCAP presenting on the neck and review the past cases reported in the literature with the aim of better establishing the characteristics of this disease.
An otherwise healthy 15-year-old girl presented with a linear cluster of multiple, occasionally pruritic lesions on the left side of the neck. The papules had been present since early childhood and no significant change in size or general appearance was noted in the following years. Physical examination confirmed the presence of 20 discrete, erythematous vesicle-like papules in a linear array on the neck, each ranging from 2 to 6 mm in diameter (Figure 1).
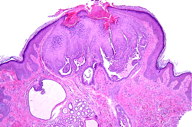
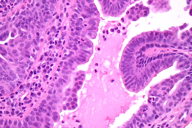
The cutaneous biopsy specimen showed areas of epidermal hyperkeratosis and parakeratosis associated with proliferations of structures composed of papillary projections lined by two rows of cells: an outer layer of cuboidal cells and an inner (luminal) layer of columnar cells with some evidence of decapitation secretion (Figure 2A). The stroma of the papillary projections regularly included plasma cells (Figure 2B). These features, consistent with SCAP lesions, were accompanied by histological structures compatible with hydrocystoma and apocrine cystadenoma.
Currently, the 3 recognized types of nevoid SCAP are plaque, solitary nodular, and linear types. The last form is very rare and only 13 cases of linear SCAP have been reported in the literature [3-13].
This linear variant is usually present at birth, and in a further 15 to 30 percent, it develops before puberty. At birth or early childhood, lesions consist of multiple linear papulo-vesicles with dome-shaped surfaces. These lesions, which may ulcerate, tend to increase in size at puberty and sometimes multiply in number, becoming more verrucous and papillomatous. Nearly all the cases of linear SCAP involved the neck, and in lesser frequency, chest, arm, and thigh [3-13]. None of them evolved from an existing nevus sebaceous.
Although linear SCAP presentations are variable, histopathological characteristics are distinctive. A unifying feature is the presence of duct-like invaginations and cyst-like cavities of various shapes and sizes extending from the epidermal surface into the body of the lesion. These extensions characteristically have keratinized epithelium near the surface of the lesion, transitioning to ducts lined by 2 epithelial cell layers, with an inner columnar layer resting on a basal low-cuboidal epithelial layer. The connective tissue stroma surrounding these duct-like structures contains a chronic inflammatory infiltrate with plasma lymphocyte predominance. An association of these lesions with dilated apocrine glands or cystadenoma-like structures seems frequent in linear SCAP [3-13].
Malignant transformation to basal cell carcinoma, squamous cell carcinoma, or sweat gland carcinoma has been described in plaque, solitary, and nodular types. However, none of linear cases evolved into a malignancy, probably because of their de novo origin [3-13].
Treatment options with acceptable aesthetic results include surgical excision and laser ablation (CO2) [12, 13].
In summary, SCAP can rarely present as multiple lesions in a linear array, unassociated with a nevus sebaceus or an epidermal nevus. It should therefore be included in the list of other adnexal tumors that can form linear arrangements, including nevus comedonicus, trichodiscoma, trichoepithelioma, basaloid follicular hamartoma, cylindroma, eccrine nevus, syringoma, eccrine poroma, eccrine spiradenoma, and basal cell carcinoma [9].
References
1. Abenoza P, Ackerman AB. Poromas. In: Abenoza P, Ackerman AB. Eds. Neoplasms with eccrine differenciation. Philadelphia: Lea and Febiger, 1990:113-185.2.Mammino JJ,Vidmar DA. Syringocystadenoma papilliferum. Int J Dermatol 1991;30:763-6. [PubMed]
3. Premalatha S, Rao NR,Yesudian P, Razack A, Zahra A. Segmental syringocystadenoma papilliferum in an unusual location. Int J Dermatol 1985;24:520-1. [PubMed]
4. de Bliek JP, Starink TM. Multiple linear syringocystadenoma papilliferum. J Eur Acad Dermatol Venereol 1999;12:74-6. [PubMed]
5. Goldberg NS, Esterly NB. Linear papules on the neck of a child: syringocystadenoma papilliferum. Arch Dermatol 1985;121:1198-201. [PubMed]
6. Krinitz K. Nevus syringocystadenosus papilliferus in linear arrangement. Hautarzt 1966;17:260-5. German. [PubMed]
7. Rostan SE, Waller JD. Syringocystadenoma papilliferum in an unusual location: report of a case. Arch Dermatol 1976;112: 835-6. [PubMed]
8. Epstein BA, Argenyi ZB, Goldstein G, Whitaker D. An unusual presentation of a congenital benign apocrine hamartoma. J Cutan Pathol 1990;17:53-8. [PubMed]
9. Patterson JW, Straka BF, Wick MR. Linear syringocystadenoma papilliferum of the thigh. J Am Acad Dermatol 2001;45:139-41. [PubMed]
10. Gonul M, Soylu S, Gul U et al. Linear syringocystadenoma papilliferum of the arm: a rare localization of an uncommon tumour. Acta Derm Venereol 2008;88:528-9. [PubMed]
11. Narang T, De D, Dogra S. Linear papules and nodules on the neck. Syringocystadenoma papilliferum. Arch Dermatol 2008;144:1509-14. [PubMed]
12. Yaghoobi R, Zadeh SH, Zadeh AH. Giant linear syringocystadenoma papilliferum of the scalp. Indian J Dermatol Venereol Leprol 2009;75:170-2
13. Pahwa P, Kaushal S, Gupta S, et al. Linear syringocystadenoma papilliferum: an unusual location. Pediatr dermatol 2011;28:61-2. [PubMed]
© 2011 Dermatology Online Journal