Radiation-induced angiosarcoma
Published Web Location
https://doi.org/10.5070/D36s33w48rMain Content
Radiation-induced angiosarcoma
C Lane Anzalone1 BS, Philip R Cohen2,3,4 MD, Abdul H Diwan6 MD, Victor G Prieto4,5 MD
Dermatology Online Journal 19 (1): 2
1. Medical School, University of Texas at Houston School of Medicine, Houston, Texas2. Department of Dermatology, University of Texas at Houston School of Medicine, Houston, Texas
3. University of Houston Health Center, University of Houston, Houston, Texas
4. Department of Dermatology, University of Texas MD Anderson Cancer Center, Houston, Texas
5. Department of Pathology, University of Texas MD Anderson Cancer Center, Houston, Texas
6. Department of Pathology, Baylor College of Medicine, Houston, Texas
Abstract
BACKGROUND: Radiation-induced angiosarcomas are uncommon adverse sequelae related to treatment of tumors. Early diagnosis and treatment are key to successful management. PURPOSE: The purpose of this case study is to describe the clinical characteristics of radiation-induced angiosarcomas. MATERIALS AND METHODS: We retrospectively reviewed the medical literature using PubMed, searching the terms angiosarcoma, breast, post, radiation, and treatment. Patient reports and previous reviews of the subject were critically assessed and the salient features are presented. RESULTS: Approximately one hundred patients have been diagnosed with radiation-induced angiosarcomas. The condition presents within the radiation field, approximately six years after initial treatment. We describe the dramatic efficacious response of our patient’s angiosarcoma to adjuvant chemotherapy both preoperatively (gemcitabine and docetaxel) and postoperatively (gemcitabine and docetaxel followed by ifosfamide and adriamycin). CONCLUSION: We recommend that new skin lesions within or adjacent to radiation ports should be considered for biopsy. Also, for lesions that are larger, ill-defined, or both, several sites should be sampled to ensure an accurate diagnosis and to prevent the possibility of a false negative interpretation.
Introduction
Angiosarcomas are rare, malignant, aggressive tumors of the vascular endothelium [1]. The breast is a common site of the body to develop angiosarcoma [1]. Angiosarcomas of the breast can be categorized into primary and secondary forms [2]. Primary angiosarcomas of the breast occur sporadically in young women without previous history of mammary carcinoma or associated factors; they usually present as palpable masses [2]. Secondary forms of angiosarcomas include the vascular tumor presenting in sites of congenital or acquired lymphedema [3]. Stewart-Treves syndrome is defined as an acquired lymphedema-associated angiosarcoma, typically developing following radical mastectomy with axillary lymph node dissection; patients may or may not have received radiation to the ipsilateral chest [4]. Another secondary form of angiosarcoma is a radiation-induced angiosarcoma of the breast, which may occur in patients with mammary carcinoma following breast conservation therapy with therapeutic radiation exposure [1].
Case report
A 52-year-old woman presented in January 2009 with an erythematous, indurated dermal plaque on her left medial breast. Four years earlier, in September 2003, she had been diagnosed with ductal carcinoma in situ of the left breast. Initially, she underwent a lumpectomy followed by a left segmental mastectomy and re-excision. Postoperatively, she received radiation therapy to the left breast, which was completed in November 2003. She had received 50 Gray in 25 fractions and an additional 10 Gray in 5 fractions, for a total dosage to the area of 60 Gray.
Hormonal treatment with tamoxifen for 6 months was stopped because of adverse side effects. Following completion of these treatments, she noticed a small pink macule on the lower medial aspect of her left breast. A lesional skin biopsy was interpreted to be benign.
 |  |
| Figure 2c | Figure 2d |
|---|
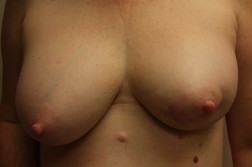
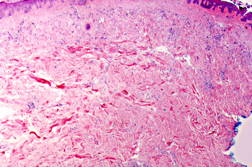
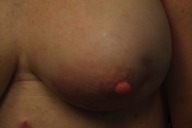
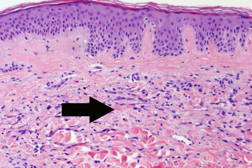
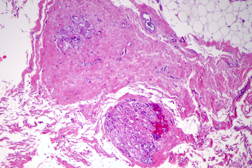
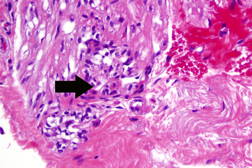
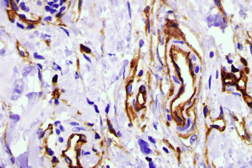
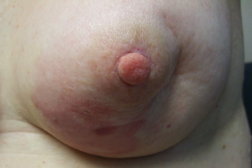
The area remained the same until December 2008 when she noted that it began to become larger and thicker. MRI showed skin thickening enhancement in the medial aspect of her left breast confined to the dermis. Examination of her chest in January 2009 showed an asymptomatic erythematous plaque measuring 4 x 2 cm with underlying induration (Figure 1). A lesional skin biopsy revealed a slight hyperchromasia of the endothelial cells lining the irregularly shaped vessel; a CD31 immunohistochemical study of the lesional skin biopsy showed an increased number of small vessels in the dermis (Figure 2). There was no response to treatment with topical corticosteroid cream (betamethasone dipropionate 0.05% ointment) twice daily for 3 weeks.
 |
| Figure 3c |
|---|
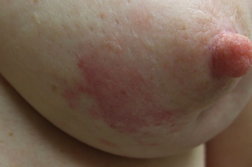
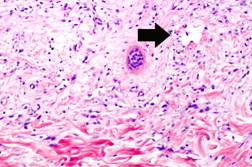
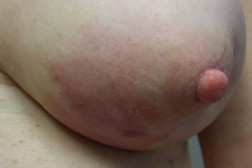
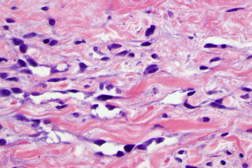
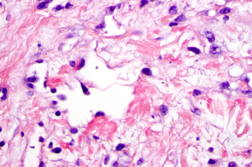
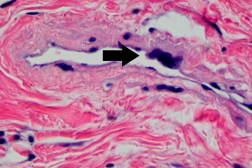
Approximately four months after her initial visit, the area became further thickened and increased in size. The induration and erythema continued to progress in all directions on the left breast to 6 cm in height and width ranging from 8 cm superiorly to 5.5 cm inferiorly (Figure 3). Three additional skin biopsies of the left breast lesion all showed similar pathologic changes. There was irregular proliferation of small vascular structures with hyperchromatic endothelial cells and irregular shape (Figure 4). Correlation of the clinical features and microscopic findings were consistent with the diagnosis of angiosarcoma.
 |
| Figure 5c |
|---|
The patient was initially treated with gemcitabine and docetaxel during the next four months. There was dramatic improvement in the skin changes of the left breast. After completion of six cycles of chemotherapy, she underwent a left total mastectomy in November 2009. Only rare foci of atypical vascularity were able to be detected (Figure 5); subsequently, she received an additional six cycles of gemcitabine and docetaxel followed by three cycles of ifosfamide and adriamycin from December 2009 to April 2010. There are no signs of recurrence after 30 months of follow-up.
Discussion
Over the past few decades, breast-conserving therapies, which include lumpectomy/segmentectomy, axillary staging, and radiation therapy, have largely supplanted radical mastectomy as the preferential treatment of breast cancer [5]. This evolution of breast cancer treatment has caused an increase, although still a rare side effect, in the numbers of cutaneous radiation-induced angiosarcomas and a decrease in the surgically-induced Stewart-Treves angiosarcoma [5]. The change in management of in situ and early breast cancer has altered the average onset of the post-treatment angiosarcoma; radiation-induced angiosarcomas typically present 72 months after treatment (with a recorded onset range from 11 to 291 months) while the lymphedema-associated Stewart-Treves variant of angiosarcoma (in patients with or without radiotherapy to the ipsilateral chest) displays a 10-15 year latency (Table 1) [3, 6, 7].
Radiation-induced angiosarcoma may occur in the remaining irradiated breast tissue following breast-conservation therapy [3]. Clinically, cutaneous angiosarcoma occurs in the superficial soft tissues [3]. The presentation may vary in appearance as red plaques or painless black, blue, red or violaceous nodules of variable size or as a bluish-black, bruise-like discoloration, overlying a painless area of induration [5]. Mammography of angiosarcoma may show nonspecific results. Therefore, accurate diagnosis of angiosarcoma based on this modality can be a challenge [3]. Skin thickening and bruising may be attributed to skin changes after radiation [8].
Indeed, the presentation of radiation-induced angiosarcoma after breast cancer is often suggestive of recurrent breast carcinoma [8]. Alternatively, the clinical manifestation of angiosarcoma in the radiation port may be interpreted as a benign hemorrhage or infection [8]. Atypical vascular lesions may also present in the field of radiation; whereas they typically follow a benign course, rarely they may progress to angiosarcoma [9]. Recently a case of composite atypical vascular lesion and Langerhans cell histiocytosis (a group of idiopathic disorders of unknown pathogenesis) was reported to develop after radiation therapy for breast carcinoma [9].
Effective treatment relies on early diagnosis. Punch biopsy and fine needle aspiration are the sampling techniques of choice. The heterogeneity of the tumor can cause false negative biopsies. Therefore, multiple biopsies should be taken to prevent artifact effect from samples taken from the wrong area or deep to the cutaneous lesions [10]. The edge of the angiosarcoma has low-grade changes that may prove indistinguishable from post-irradiation transformation [11].
Simple mastectomy with wide surgical margins is the most common treatment of choice [5]. Recurrence rates are high at 46.5 percent, typically occurring 9 months after treatment [3]. A more aggressive excision may yield a longer disease-free survival rate [3, 12].
Angiosarcoma has been associated with a high rate of recurrence following excision. Therefore, additional treatment options have been administered both before and after surgical excision. A combination of adriamycin, cisplatin, ifosfamide, and paclitaxel has produced success in the treatment of three patients: a 62-year-old male, a 24-year-old male, and a 69-year-old female [13]. Docetaxel and thalidomide may also be considered as therapeutic options in the treatment of cutaneous angiosarcoma [14, 15]. Our patient illustrates the successful treatment with preoperative gemcitabine and docetaxel, surgical excision, and postoperative chemotherapy with gemcitabine and docetaxel, followed by ifosfamide and adriamycin.
Conclusion
Radiation-induced angiosarcomas are rare adverse sequelae to treatment of tumors. Careful long-term observation of the radiation field is important, as the angiosarcoma can present, on average, six years after therapy. Early diagnosis and prompt treatment are important due to the aggressive nature of the angiosarcoma. Our patient illustrates the dramatic efficacious response to adjuvant chemotherapy both preoperatively (gemcitabine and docetaxel) and postoperatively (gemcitabine and docetaxel followed by ifosfamide and adriamycin) chemotherapy. We recommend consideration for biopsy of new skin lesions within or adjacent to radiation ports. Also, several biopsy sites should be sampled to ensure accurate diagnosis and to prevent the possibility of false negatives.
References
1. Glazebrook KN, Magut MJ, Reynolds C: Angiosarcoma of the breast. AJR Am J Roentgenol 2008;190:533-538. [PubMed]2. Wang XY, Jakowski J, Tawfik OW, Thomas PA, Fan F: Angiosarcoma of the breast: a clinicopathologic analysis of cases from the last 10 years. Ann Diagn Pathol 2009;13:147-150. [PubMed]
3. Esler-Brauer L, Jaggernauth W, Zeitouni NC: Angiosarcoma developing after conservative treatment for breast carcinoma: case report with review of the current literature. Dermatol Surg 2007;33:749-755. [PubMed]
4. Stewart FW, Treves N: Lymphangiosarcoma in postmastectomy lymphedema; a report of six cases in elephantiasis chirurgica. Cancer 1948;1:64-81. [PubMed]
5. Bolin D, Lukas G: Low-grade dermal angiosarcoma of the breast following radiotherapy. Am Surg 1996;62:668-672. [PubMed]
6. di Meo N, Drabeni M, Gatti A, Trevisan G: Letter: A Stewart-Treves syndrome of the lower limb. Dermatol Online J 2012;18(6):14. [PubMed]
7. Abbott R, Palmieri C: Angiosarcoma of the breast following surgery and radiotherapy for breast cancer. Nat Clin Pract Oncol 2008;5:727-736. [PubMed]
8. West J, Liao SY, Cho D: Angiosarcoma after Breast Conservation: Diagnostic Pitfalls. Clin Breast Cancer 2008;8:94-96. [PubMed]
9. Pan Z, Bland KI, Wei S. Composite cutaneous atypical vascular lesion and Langerhans cell histiocytosis after radiation for breast carcinoma: can radiation induce Langerhans cell histiocytosis? Dermatol Online J. 2011 Dec 15;17(12):6. [PubMed]
10. Deutsch M, Werner R: Angiosarcoma of the breast with delay in diagnosis. Clin Adv Hematol Oncol 2004;2:320. [PubMed]
11. Rosen PP, Sarcoma. Rosen’s Breast Pathology. In Rosen PP (ed): Philadelphia: Lippincott, Williams & Wilkings, 2001; 813-861.
12. Maddox JC, Evans HL: Angiosarcoma of the head and neck. Cancer 1981;48:1907-1921. [PubMed]
13. Asmane I, Litique V, Heymann S, Marcellin L, Métivier AC, Duclos B, Bergerat JP, Kurtz JE: Adriamycin, cisplatin, ifosfamide and paclitaxel combination as front-line chemotherapy for locally advanced and metastatic angiosarcoma. Analysis of three case reports and review of the literature. Anticancer Res 2008;28:3041-3045. [PubMed]
14. Nagano T, Yamada Y, Ikeda T, Kanki H, Kamo T, Nishigori C: Docetaxel: a therapeutic option in the treatment of cutaneous angiosarcoma: report of 9 patients. Cancer 2007;110:648-651. [PubMed]
15. Raina V, Sengar M, Shukla NK, Deo SS, Mohanty BK, Sharma D, Ray R, Das P, Rath GK: Complete response from thalidomide in angiosarcoma after treatment of breast cancer. J Clin Oncol 2007;25:900-901. [PubMed]
© 2013 Dermatology Online Journal