Cyclophosphamide pulses with oral prednisolone in the treatment of pemphigus: A pilot study
Published Web Location
https://doi.org/10.5070/D36ns4v35jMain Content
Cyclophosphamide pulses with oral prednisolone in the treatment of pemphigus: A pilot study
Radhakrishna Bhat1, Vinod K Sharma1, M Ramam1, Ashok Kumar2
Dermatology Online Journal 11 (3): 4
1. Department of Dermatology and Venereology, All India Institute of Medical Sciences, New Delhi, India. aiimsvks@yahoo.com
2. Department of Clinical Immunology, All India Institute of Medical Sciences, New Delhi, India
Abstract
An open labeled clinical trial aimed at assessing the efficacy and safety of pulse intravenous cyclophosphamide with daily oral prednisolone in the treatment of pemphigus was carried out. Twenty-six patients (12 men, 14 women; mean age, 48.4 years), comprising 25 cases with pemphigus vulgaris and 1 with pemphigus vegetans (<10% body surface area involvement) who did not achieve adequate control on corticosteroids with or without other adjuvants were included. After baseline evaluation, monthly intravenous boluses of cyclophosphamide (15mg/kg) along with daily oral prednisolone (starting dose 1mg/kg/day, tapered according to clinical response) were administered. Patients were assessed monthly for clinical activity and side-effects. All patients experienced significant clinical improvement within 1 month of starting treatment. Healing of skin and mucosal lesions occurred respectively at mean durations of 2.1 and 3.6 months. Three weeks to 8 months later, 9 patients had recurrences of activity on tapering/withdrawal of prednisolone, mainly in the oral mucosa. Side effects of treatment included amenorrhea (3 patients), microscopic hematuria (3) which cleared with co-administration of mesna, vomiting (1), weight gain (10), gastritis (1), and cataract (2). It is concluded that treatment with monthly intravenous cyclophosphamide boluses along with daily oral prednisolone clears lesions of pemphigus with < 10 percent body surface involvement, and this may be an alternative regimen for pemphigus. Monitoring for adverse effects is essential.
Introduction
Pemphigus is a potentially fatal disease, associated with a mortality rate as high as 90-100 percent when untreated [1]. The prognosis dramatically improved with the introduction of systemic corticosteroids in its therapy. Prednisone in doses varying from 40 to 400 mg has been used in the treatment of pemphigus, the higher doses being required for 5-10 weeks for disease control [2]. Various adjuvants have been used to reduce the side effects associated with steroid monotherapy. These include immunosuppressive agents (e.g., azathioprine, cyclophosphamide, cyclosporine, mycophenolate mofetil), anti-inflammatory agents (e.g., gold, antimalarials, dapsone, niacinamide), as well as immunomodulatory therapies (e.g., plasmapheresis, extracorporeal photopheresis, intravenous immunoglobulins). The use of such steroid-sparing adjuvants has brought the mortality in pemphigus down to less than 10 percent.[3]
High-dose intravenous methylprednisolone (250-1000 mg a day for 4-5 consecutive days) [4, 5], or dexamethasone (100 mg a day for 3 consecutive days) with cyclophosphamide (500 mg on 1 day) [6] pulses (DCPs) have been found to be effective in achieving long-term remission, the latter regimen being widely used in centers in India. Pulse intravenous cyclophosphamide without a concomitant corticosteroid pulse has also been used in recalcitrant cases of pemphigus with encouraging results [7, 8]. Pulse cyclophosphamide has fewer side effects than traditional cyclophosphamide administration with regard to urinary bladder malignancies and gonadal toxicity [9, 10]. We conducted a pilot study of cyclophosphamide pulses (15 mg/kg) along with prednisolone (1 mg/kg) in the treatment of pemphigus.
Methods
This pilot study was an open-labeled prospective clinical trial conducted during the period 2000-2002. It included 26 patients of pemphigus who presented to the dermatology outpatient department at a tertiary care hospital in New Delhi, India. The study was approved by the institute ethics committee.
Patients
Patients with mild to moderate pemphigus (< 10 % of body surface involvement), whose lesions did not heal completely and those who continued to develop new lesions while on adequate doses of daily corticosteroids with or without adjuvants (azathioprine, dapsone, or methotrexate) were included. Children, unmarried individuals, those who had not completed their families, pregnant or lactating women, patients older than 65 years, and those with hepatic disease were excluded. Written informed consent of the patients was taken before their inclusion. Patients in the reproductive age group who consented to being included were counseled on the need for adequate contraception during this therapy.
Pre-treatment evaluation
The clinical diagnosis was confirmed in all the patients by Tzanck smear examination, histology, and direct immunofluorescence showing epidermal intercellular IgG with or without IgM. The approximate percentage of body surface involved was determined by considering each area equivalent to that of the patient's palm as 1 percent. Baseline investigations in all patients included complete blood counts, fasting blood glucose, serum electrolytes, renal and hepatic function tests, urine examination (albumin, sugar, and microscopic examination), chest x-ray, and electrocardiogram.
Treatment regimen
Patients included in the study were treated as inpatients or in day care with a monthly intravenous dose of 15 mg/kg of cyclophosphamide in 200 ml of 5 percent dextrose or dextrose-normal saline over 1 hour, followed by hydration with 500 ml of 5 percent dextrose or normal saline given intravenously over 5-6 hours after the pulse. In addition, patients were advised to increase their daily water intake to ≥3 liters/day for 3 days, starting on the day before the cyclophosphamide pulse was administered. They were also advised to void frequently.
Oral ondansetron (8 mg) was used as an antiemetic, with 3 doses at 12 hour intervals, the first dose being administered 1 hour before the pulse.
In addition to monthly pulses of cyclophosphamide, the patients received daily oral prednisolone (started at 1 mg/kg, with the dose being tapered after control of disease activity). They were also prescribed oral ranitidine (150 mg twice daily), and oral calcium and potassium supplements. One patient was administered an intralesional triamcinolone injection (1ml of 10 mg/ml) for persistent skin lesions.
Secondary infections of skin lesions were treated with appropriate antibiotics before the study regimen was started. Patients with oral candidiasis were treated with oral fluconazole (50-100 mg daily for 2-4 weeks).
Followup
Assessment of clinical response
Patients were assessed monthly for clinical activity in terms of new blisters, extent of body surface/mucous membrane involvement, and the Nikolsky sign. Clinical photographs were taken.
Patients were considered to have improved clinically if skin or mucosal erosions showed healing, and to have achieved clinical inactivity when all skin and mucous membrane lesions had completely healed and there were no new lesions. A recurrence of activity was indicated by the appearance of any fresh oral or cutaneous lesion of pemphigus, with confirmation by Tzanck smear examination. Recurrences were treated by restarting and increasing the daily dose of prednisolone by 10-20 mg/day, while the cyclophosphamide pulses were continued.
Monitoring for adverse effects
Adverse effects as reported by the patient were recorded. Urinary complaints including hematuria were specifically sought. Laboratory monitoring consisted of complete blood counts fortnightly, urine examination (routine and microscopic) monthly, as well as renal function tests (urea, creatinine) and liver function tests (bilirubin, AST, ALT, alkaline phosphatase) at 0, 1, 3, and 6 months. Monitoring for adverse effects of steroids was also carried out (fasting blood sugar at 0, 1, 3, and 6 months, and chest X-rays at 0 and 6 months). Weight and blood pressure were recorded at every visit.
Patients who developed cyclophosphamide-induced microscopic hematuria (defined as RBCs found in urine at microscopy on at least 2 separate occasions) were treated with intravenous mesna (equivalent in mg to 60 % of the cyclophosphamide pulse dose, administered in 3 divided doses over 8 hours).
Statistical analysis
Descriptive statistics were used. Mean durations to clearance of lesions and recurrences were calculated.
Results
Twenty-six patients were treated with the study regimen. Two additional patients satisfied the study criteria, but did not give consent for inclusion. Fourteen of the patients included were female, and the age of the patients ranged from 25 to 65 years (mean±SD, 48.4±10.4 years).
Twenty-five patients had pemphigus vulgaris, and 1 had pemphigus vegetans, the duration of illness was 2 months to 12 years (median, 18 months). Twenty-two (84.6 %) had cutaneous erosions or blisters along with mucosal erosions; skin involvement alone and mucosal involvement alone were seen in 2 patients each. Lesions occurred most often on the trunk (22 patients), followed in order of frequency by the head and neck areas (17), lower limbs (14), upper limbs (12), genitalia (2), and periungual skin (2). Seven patients had secondary infection of their skin lesions at presentation.
Mucosal involvement was severe in 6, moderate in 11, and mild in 7 patients. Oral erosions occurred in all 24 patients with mucosal involvement. Nine patients had oral candidiasis. Other mucosal surfaces also were involved, with 4 patients having nasal involvement, and 2 each having conjunctival and genital erosions. In addition, 10 patients complained of odynophagia, indicating probable oropharyngeal involvement.
Patients received 7-19 cyclophosphamide pulses (Mean±SD, 11.5 ± 3.8 pulses), each being 500-1200 mg (770.8 ± 135.8 mg). The pulse dose was reduced in 1 patient from 1200 mg to 1000 mg as microscopic hematuria developed at 1200mg.The initial daily dose of prednisolone was 35-80 mg (52.5 ± 9.8 mg). The cumulative doses of cyclophosphamide were 4500-17550 mg (9175.6±3794.0 mg), and those of prednisolone 3450-15000 mg (7148.1±2501.2 mg).
A. Response
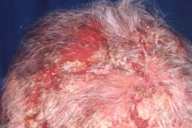
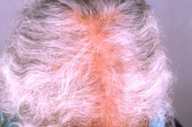
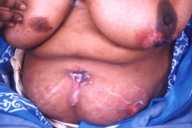
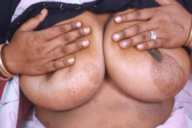
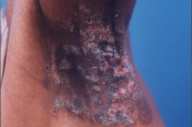
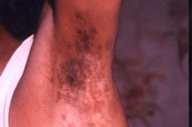
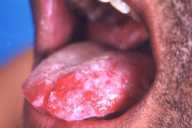
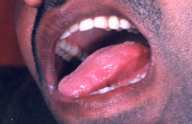
All patients had improved significantly at the end of 1 month with onset of healing of skin and mucosal lesions, and patients with oral involvement reported being able to increase their oral intake. Complete healing of lesions occurred at a mean duration of 2.1 months (0.5-10 months) in the skin (Figs. 1-3) and at 3.6 months (1-6.5 months) in the mucous membranes (Fig. 4).
|
|
| Figure 1A | Figure 1B |
|---|---|
| Fig 1. Scalp lesions (A) Before treatment and (B) Clearance with treatment. | |
|
|
| Figure 2A | Figure 2B |
|---|---|
| Fig 2. Erosions on the trunk (A) Before treatment and (B) Clearance with treatment. | |
|
|
| Figure 3A | Figure 3B |
|---|---|
| Fig 3. Vegetating axillary lesions (A) Before treatment and (B) Clearance with treatment. | |
|
|
| Figure 4A | Figure 4B |
|---|---|
| Fig 4. Oral erosions (A) Before treatment and (B) Clearance with treatment. | |
Nine (34.6 %) patients had recurrences 3 weeks to 8 months later. Of these 6 had oral recurrences. Five of these 9 recurrences occurred with withdrawal of corticosteroid (after a mean period of 2.3 months), three after tapering of prednisolone to 10 mg/day, and one with missed cyclophosphamide pulses. Recurrences were managed as described above, and cleared in eight out of the nine patients at a mean of 2 months (range 1-4.5 months) from their onset, and had not cleared in one patient at the time of analysis. Three of these eight patients developed a second recurrence at 1-2.5 months after clearance of the first, which were again managed as above.
After 3, 6, 9, and 12 months of treatment, 13/26 (50 %), 21/26 (80.8 %), 9/16 (56.3 %), and 9/11 (81.9 %) of patients respectively were free of all lesions. It was also seen that the dose of daily prednisolone could be tapered from a mean of 52.5 mg at the start of the regime, to a mean of 10.5 mg in the eleven patients who completed 12 months of treatment. All six patients followed up at 15 months and both patients followed up at 18 months also had no clinical activity. The proportions of patients with clearance and in whom daily prednisolone could be discontinued were determined at various points of the follow-up (Table 1). The dose of daily prednisolone could be tapered off in all the patients, and completely discontinued in eight (30.8 %) patients. These eight patients were off daily prednisolone for a mean of 5.6 months at the time of this report. A cross-sectional analysis of the clinical and treatment status of patients, done at the point of writing this report, is summarized in Table 2.
| Months | 0 | 3 | 6 | 9 | 12 |
|---|---|---|---|---|---|
| Total inactive (a + b) | 0 | 13 | 21 | 9 | 9 |
| a. Off prednisolone | 0 | 0 | 4 | 4 | 4 |
| b. On prednisolone | 0 | 13 | 17 | 5 | 5 |
| Active, on prednisolone | 26 | 13 | 5 | 7 | 2 |
| Prednisolone dose(mg.)(mean±SD) | 52.5±9.8 | 21.5±12.8 | 13.5±9.3 | 9.7±9.0 | 10.5±8.3 |
| Total no. of patients | 26 | 26 | 26 | 16 | 11 |
| Status at last visit | No. of patients | Percentage |
|---|---|---|
| Complete clinical inactivity | 23 | 88.4 |
| On cyclophosphamide pulses only | 8 | 30.8 |
| On cyclophosphamide pulses with prednisolone (5-20 mg/day) |
15 | 57.6 |
| Clinical activity present | 3 | 11.6 |
| Total | 26 | 100 |
Adverse effects
Amenorrhea developed in three (21.4 %) of the fourteen female patients, aged 25-35 years, occurring after 3-6 pulses. Three (11.5 %) patients had microhematuria after 3-7 pulses, and one of these patients also complained of passing brown colored urine. Urine culture was found to be sterile in all these patients, and their corresponding platelet counts were normal. Microhematuria subsided in all three patients, with 1-2 co-administrations of mesna. Relative lymphopenia, defined as a differential lymphocyte count of <12.5 percent, was seen in five patients. None of the patients in this series developed absolute leucopenia or other cytopenias. Pulse administration caused nausea in three patients, and vomiting in one patient despite adequate administration of oral ondansetron. These symptoms were controlled by the addition of oral metoclopramide, and the cyclophosphamide pulses were continued. Corticosteroid side effects seen included weight gain (10 patients), cushingoid features (6), and acneiform eruption (6). Furuncles occurred in five patients. One patient developed gastritis; it was confirmed on endoscopy and subsided on treatment with lansoprazole. Two patients who complained of visual blurring beginning while on treatment were found to have cataracts; they were advised cataract extraction with intraocular lens implantation. None developed diabetes or hypertension. Renal and hepatic function tests as well as chest x-rays showed no abnormalities in any patient during followup. None of the patients required discontinuation of cyclophosphamide pulses due to adverse effects.
Discussion
Pulse intravenous cyclophosphamide therapy is established in the treatment of various autoimmune diseases such as autoimmune thrombocytopenic purpura, systemic lupus erythematosus, and lupus nephritis; this treatment is associated with improved outcome compared to other therapies including daily oral cyclophosphamide [9, 10]. Studies suggest that, for these conditions, pulse cyclophosphamide is more effective than oral or intravenous pulse corticosteroid therapy and has fewer side effects than daily oral cyclophosphamide, especially with regard to urinary bladder malignancies and gonadal toxicity [9, 11].
Cyclophosphamide pulse therapy has been used previously in a few patients with pemphigus. Fleischli et al.[8] found that disease control was achieved in 2-5 months of starting cyclophosphamide pulses, with good to excellent response in six out of nine patients. In another report, remission was achieved at 7 and 10 months respectively in two patients [7]. In comparison, Ratnam et al.[12] achieved initial control of pemphigus with daily steroids in low-dose (45-60 mg/day) and high-dose (120-150 mg/day) regimens, at a mean of 24 days and 19.6 days respectively in these two groups. In a study by Pasricha and co-workers [13], 308 (72 %) out of 422 pemphigus patients treated with DCPs went into remission within 1 year of starting treatment, 205 (48.5%) achieving remission within 6 months, and another 103 (23.5 %) at 7-12 months.
In the above study, of the total of 401 patients who achieved remission with DCPs, 98 (24.4 %) required additional dexamethasone pulses, 75 (18.7 %) daily steroids, and 108 (26.9 %) required both [13]. These data imply that a certain dose of corticosteroid between pulses is essential in order to completely heal lesions in the first year of treatment in pemphigus. Our patients received no pulse corticosteroid, and this might account for the recurrences seen when the daily steroid was tapered or withdrawn. Low doses of daily steroid for longer durations after clearance of lesions may therefore be required in some patients.
Although all our patients achieved clearance of lesions, recurrences occurred in a significant proportion. Similarly, Fleischli et al.[8] described flares of activity in three patients after an excellent response had been achieved with cyclophosphamide pulses, as did Pandya et al. [7] in two patients they treated. Seventeen percent of patients treated with DCP [13] and 3 (50 %) of six responders to methylprednisolone pulses[4] were reported to develop relapses or disease flares. Patients on daily steroids alone also developed flares or relapses in 33-77 percent [1, 12, 14]. Treatment may thus lead to healing and prevent further disease progression, but milder recurrences seem inevitable in a proportion of patients treated with any of the currently available modalities.
Untreated pemphigus carried a high mortality rate, but this was brought down with the advent of steroid therapy [1]. Death occurred in 21.7-31.8 percent of patients on daily steroids [1, 14], in 4.5 percent of patients on DCPs[13], and in two (22.2 %) out of nine patients in the previous series treated with pulse cyclophosphamide [8]. No deaths were encountered in the current series; this may be partly because patients with extensive pemphigus were not included because the efficacy of this regimen was yet to be assessed.
Cyclophosphamide pulses probably facilitate tapering of the daily steroid dose, although only a controlled study can give definitive evidence of this. In Fleischli's group, one (11.1 %) patient was able to stop daily steroid, and five (55.5 %) patients had their steroid dose tapered [8]; both patients described by Pandya et al.[7] had had their daily steroid withdrawn. In both reports, patients were receiving high doses of daily corticosteroid without adequate response before the introduction of cyclophosphamide pulses. In our patients too, the mean daily dose of prednisolone could be reduced from 52.5 mg at the beginning of treatment to 21.5 mg within 3 months (Table 1) while maintaining response. It is not otherwise possible to maintain disease inactivity on such tapered doses of daily steroid alone, and high-dose steroid pulses are usually required. For instance, in Pasricha's study conducted at the same center, 205, 103, and 54 patients respectively required 1-6, 7-12, and 13-24 monthly dexamethasone pulses with or without cyclophosphamide pulses (500 mg/month, a lower dosing than in this study) and daily prednisolone to achieve remissions [13]. In addition, side effects of steroid therapy were mild in most cases in our study, and we believe that the cyclophosphamide pulses contributed to this by allowing early reduction of the daily steroid dose, and its discontinuation in eight patients.
Side effects attributable to cyclophosphamide were seen in six (23.1 %) patients. Though all patients had clinical clearance, only five developed relative lymphopenia. The reason for this is not clear, given the role of B lymphocytes in the causation of the lesions of pemphigus. There was no correlation between the occurrence of skin infections and fall in lymphocyte counts. None of our patients experienced severe infective complications.
Urologic toxicity is a major consideration with cyclophosphamide use, hemorrhagic cystitis and late bladder malignancies being the foremost [15, 16]. The pulsed regimen has been associated with lower levels of bladder toxicity as compared to daily cyclophosphamide therapy [17]. This may result from reduced cumulative doses[18] and the ability to ensure better hydration with the pulses. The possibility of late bladder toxicity cannot as yet be ruled out in the present study. Three (11.5 %) of our patients developed microhematuria. Because cystoscopies were not performed, hemorrhagic cystitis cannot be ruled out in them. Co-administration of mesna is therefore recommended in all cases receiving cyclophosphamide pulses when cost is not a limiting factor.
Amenorrhea was seen in three (21.4 %) of the fourteen female patients included. These patients had completed their families and were not very concerned about this symptom, but this regimen cannot be recommended for female patients in the reproductive age group. Amenorrhea due to cyclophosphamide therapy may be irreversible [19, 20], and is associated with large cumulative doses and prolonged lengths of treatment [21]. However, a lower incidence of gonadal toxicity in males and females has been reported with pulse cyclophosphamide regimens as compared to daily dosing [20, 22]. In this context, it may also be noted that the cumulative dose of cyclophosphamide (500-1000mg/month) is significantly lower than that with the DCP regimen (2000mg/month) because the latter also involves administration of daily oral cyclophosphamide (50mg) in addition to the pulse doses.
Pulse regimens used for pemphigus involve intravenous administration of methylprednisolone for up to 5 days [5], or dexamethasone for 3 consecutive days with cyclophosphamide on day 1 (DCP) [6,13]. A major advantage with the study regimen is that the pulse is administered only on 1 day every month, and patients can be treated in day-care. This significantly reduces the number of workdays lost to patients because of therapy, thereby enhancing compliance with treatment.
Conclusion
In conclusion, cyclophosphamide pulse therapy along with daily prednisolone appears effective in clearing clinical disease in pemphigus, and the pulses may have a steroid-sparing effect. Monitoring for adverse effects is essential. This regimen may serve as an alternative in patients who respond inadequately to other modalities. However, controlled studies are essential to assess its role in the management of pemphigus as well as its safety in the long term.
Acknowledgement:Dr. Manoj K Singh, Department of Pathology, All India Institute of Medical Sciences, for providing confirmation of the diagnosis of pemphigus, by histopathology and direct immunofluorescence.
References
1. Seidenbaum M, David M, Sandbank M. The course and prognosis of pemphigus: A review of 115 patients. Int J Dermatol. 1988 Oct;27(8):580-4.PubMed2. Lever WF, Schaumburg-Lever G. Treatment of pemphigus vulgaris: Results obtained in 84 patients between 1961 and 1982. Arch Dermatol. 1984 Jan;120(1):44-7. PubMed
3. Bystryn JC, Steinman NM. The adjuvant therapy of pemphigus: An update. Arch Dermatol 1996; 132(2): 203-212. Arch Dermatol. 1996 Feb;132(2):203-12. PubMed
4. Werth VP. Treatment of pemphigus vulgaris with brief, high-dose intravenous glucocorticoids. Arch Dermatol. 1996 Dec;132(12):1435-9. PubMed
5. Chryssomallis F, Dimitriades A, Chaidemenos GC, Panagoitides D, Karakatsanis G. Steroid-pulse therapy in pemphigus vulgaris: long term follow-up. Int J Dermatol. 1995 Jun;34(6):438-42. PubMed
6. Pasricha JS, Khaitan BK, Raman RS, Chandra M. Dexamethasone-cyclophosphamide pulse therapy for pemphigus. Int J Dermatol. 1995 Dec;34(12):875-82. PubMed
7. Pandya AG, Sontheimer RD. Treatment of pemphigus vulgaris with pulse intravenous cyclophosphamide. Arch Dermatol. 1992 Dec;128(12):1626-30. PubMed
8. Fleischli ME, Valek RH, Pandya AG. Pulse intravenous cyclophosphamide therapy in pemphigus. Arch Dermatol. 1999 Jan;135(1):57-61. PubMed
9. Werth VP. Pulse intravenous cyclophosphamide for treatment of autoimmune blistering diseases: Is there an advantage over the oral route? Arch Dermatol. 1997 Feb;133(2):229-30. PubMed
10. Flanc R, Rober M, Strippoli G, Chadban S, Kerr P, Atkins R. Treatment of lupus nephritis. Cochrane Database Syst Rev. 2004;(1):CD002922. PubMed
11. Haubitz M, Ehlerding C, Kamino K, Koch KM, Brunkhorst R. Reduced gonadal toxicity after I.V. cyclophosphamide administration in patients with nonmalignant diseases. Clin Nephrol. 1998 Jan;49(1):19-23. PubMed
12. Ratnam KV, Phay KL, Tan CK. Pemphigus therapy with oral prednisolone regimens: A 5 year study. Int J Dermatol. 1990 Jun;29(5):363-7. PubMed
13. Pasricha JS. Pulse therapy in pemphigus and other diseases. 2nd Ed, New Delhi: Pulse Therapy and Pemphigus Foundation, 2000.
14. Rosenberg FR, Saunders S, Nelson CT. Pemphigus: A 20 year review of 107 patients treated with corticosteroids. Arch Dermatol. 1976 Jul;112(7):962-70. PubMed
15. Ho VC, Zloty D. Immunosuppressive agents in dermatology. Dermatol Clin. 1993 Jan;11(1):73-85. PubMed
16. Fraiser LH, Kanekal S, Kehrer JP. Cyclophosphamide toxicity: Characterizing and avoiding the problem. Drugs. 1991 Nov;42(5):781-95. PubMed
17. Martin F, Lauwerys B, Lefebvre C, Devogelaer JP, Houssiau FA. Side effects of intravenous cyclophosphamide pulse therapy. Lupus. 1997;6(3):254-7. PubMed
18. Koldingsnes W, Grant JT, Omdal R, Husby G. Wegener's granulomatosis: Long-term follow-up of patients treated with pulse cyclophosphamide. Br J Rheumatol. 1998 Jun;37(6):659-64. PubMed
19. Ahmed AR, Hombal SM. Cyclophosphamide (Cytoxan): A review on relevant pharmacology and clinical uses. J Am Acad Dermatol. 1984 Dec;11(6):1115-26. PubMed
20. McCune WJ, Fox D. Intravenous cyclophosphamide therapy of severe SLE. Rheum Dis Clin North Am. 1989 Aug;15(3):455-77. PubMed
21. Dutz JP, Ho VC. Immunosuppressive agents in dermatology: An update. Dermatol Clin. 1998 Apr;16(2):235-51. PubMed
22. Richmond R, McMillan TW, Luqmani RA. Optimisation of cyclophosphamide therapy in systemic vasculitis. Clin Pharmacokinet. 1998 Jan;34(1):79-90. PubMed
© 2005 Dermatology Online Journal

