Modified Bier block anesthetic technique is safe for office use for botulinum a toxin treatment of palmar and plantar hyperhidrosis
Published Web Location
https://doi.org/10.5070/D36g96v8fbMain Content
Modified Bier block anesthetic technique is safe for office use for botulinum a toxin treatment of palmar and plantar hyperhidrosis
Perry Solomon MD
Dermatology Online Journal 13 (3): 6
Bridges Medical Clinic, San Ramon, CABotulinum A toxin (BTX-A) to treat hyperhidrosis (HH) has been shown in many studies to be efficacious [1-12]. The FDA approved Botox™ in July 2004 to treat severe underarm HH. The 18-20 injections in this area are relatively pain free using several 0.3cc 31-gauge B-D short-needle insulin syringes to maintain the sharpness of the tip. However, more problematic is how to adequately anesthetize the hands and feet to treat HH in those areas. Although treating these areas is still an "off-label" use of Botox™, several techniques have been described to numb these regions to administer the 50 or so injections needed to inject the 100 units of Botox™ in each hand or foot. This amount can vary slightly depending upon the size of the patient.
Some practitioners utilize ice packs, spray with ethyl chloride, use some type of anesthetic cream such as EMLA, or use nothing at all, and when the patient feels the inevitable pain of the injections, stops and uses more of the same [1, 6, 12]. These methods have no place in a modern medical practice. Proper anesthesia for palmar and plantar injections is mandatory and, in my opinion, to not do so falls outside the standard of care that the patient should be given.
Jet injection of either BTX-A or anesthetic medication has been described [6, 8, 9, 13, 14, 15]. Several drawbacks limit these techniques. Jet injection of Botox™ has not been studied to see if the efficacy of the drug remains intact with the force of the injection through the skin. Using jet injection to place Lidocaine in the skin to then inject Botox™ into the skin weal appears to be a duplication of effort as well not having been clinically studies for efficacy. Along with the necessity of purchasing the injector (approximately $5,000) and the need to autoclave for 30 minutes the metal component and cold sterilizing of the plastic component adds further costs and time to what should be a simple procedure. The possibility of nerve injury, lack of efficacy, cost of equipment and cleaning, inability to properly inject the web spaces and digits and lack of clinical efficacy makes this method unreliable and not one that, at least at present, is a viable option.
There is a recent report published describing "vibration anesthesia to use when performing palmar and plantar injections [16]. The authors themselves write "the term anesthesia refers to the elimination of pain. . .and the term analgesia refers to the reduction of pain." They further state that "although the use of vibration anesthesia generally does not eliminate pain completely, it can serve to make the injections much more tolerable". This misnamed article does not really offer a viable technique to provide adequate and total anesthesia for the painful palmar or plantar injections.
One adequate anesthetic technique is to use a ulnar, median and radial nerve block for the hand and a posterior tibial and sural nerve block for the foot [8, 17, 18]. In experienced hands this type of block is an excellent way to provide anesthesia. Three major drawbacks exist however. One is that a successful block is very user dependent and there is a learning curve to performing it. Another is the potential for nerve injury that can happen from single attempts at these blocks as well as nerve injury from repeated injections [19, 20, 21, 22]. Lastly is the onset time and offset time. Since these procedures are done in an office setting, the 30 minutes or longer that the block needs to take effect and the hour or longer that it takes to wear off, can mean a 3-4 hour ordeal for the patient if both hands or both feet are injected, and can leave them unable to drive themselves home because of continued muscle weakness in those areas; this type of block gives a full motor as well as sensory block [23].
A more reliable, safer, easier and more rapid anesthetic block exists. The Bier block, as first described by Augustus Bier in 1908 [24], has been used as an excellent technique for Botox™ administration in a pain-free environment. However, all reports to date have utilized either the same methods that have been described for years, whose original application was for total arm anesthesia, or just using the same volume of anesthetic compound that has been used in the past and moving the cuff to the forearm [9, 23, 24, 25, 26, 27], and none have described using it for plantar injections. Over the past 5 years I have used a modified Bier block technique in over 150 patients to provide adequate and safe anesthesia in an office setting so that they have no pain during injections. Due to the much smaller volume of anesthetic injected, giving the patient a sensory block and not a major motor block, the patients can be ambulatory with full use of their hands and feet and drive themselves home within 10-15 minutes after the procedure is completed. The total time for anesthetizing both hands, injecting the Botox™ and recovery of function should not take longer than 1 hour. This modified Bier block technique was first presented in June 2003 [28].
Technique
A 22-gauge intravenous line is begun in a vein on the dorsum of the hand (foot) with a Hep-Loc cap placed on the end and secured to the skin with tape. No solution need be injected into this because of the timing of the introduction of the anesthetic. A single layer of gauze is placed on the patients wrist (ankle) with a 12" long tourniquet is wrapped snugly on top of this and connected to a pneumatic pressure machine.
 |
| Figure 1 |
|---|
An Eshmark bandage is then tightly wrapped from the patient's fingers (toes) to the cuff, with care not to dislodge the intravenous, and the pneumatic pressure is then turned on to 250-300 torr. The Eshmark is removed and a finger is placed on the radial artery (posterior tibial) to check for a pulse and the fingernail (toenail) beds tested for capillary refill to ensure proper occlusion of arterial blood flow to the hand (foot). When this is assured, lidocaine (0.5 %, preservative free) is injected into the intravenous line. The volumes used vary between 12 and 17cc (60-85 mg), depending on the size of the patient's hand (foot). The patient can experience some warmth in their hand (foot) during the injection that can be minimized by slow injection and the lidocaine. While the block is setting up the Botox™ is reconstituted. Using 2.5cc of preservative-free saline that is injected into the vial after the top is removed, the solution is drawn up into five separate 0.5cc 31 gauge B-D short needle insulin syringes. The top of the vial is removed so that the thin needle stays sharp to facilitate the injection.
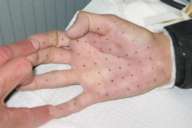 |
| Figure 2 |
|---|
A felt tip pen is used to mark the injection points in the hand. These are just reference points because, during the injections in the exsanguinated hand (foot) there are no bleeding marks to see where previous injections have taken place, it is easy to loose track and miss some areas. The injections should be made to the side of the pen marks so as not to "tattoo" the skin. The 50 or so injections are made at a 45-degree angle into the palm and fingers (sole and toes) in 2-unit aliquots. This should take about 5 minutes. When finished the tourniquet is released and the intravenous removed.
Discussion
This is the first published report of the modified Bier block technique for use in palmar and plantar injections. The criticisms of the classic Bier block technique used in the past no longer apply using this modification [23]. The primary concern had been that the sudden release of anesthetic systemically by a cuff failure or release of the tourniquet in a short amount of time after injection would cause systemic effects [29, 30]. These reports were made when bupivacaine was utilized for the anesthetic, which is no longer the standard of care. A review of 20 years history using the currently recommended anesthetic, preservative-free lidocaine 0.5 percent, showed that there was a complication rate of 1.6 percent using the standard volume used for full arm anesthesia of 50 cc of lidocaine 0.5 percent (250 mg), with dizziness, tinnitus and mild bradycardia being the majority and most severe of them [26]. If we extrapolate the maximum volume of lidocaine that is used in the modified technique, 17cc, (85 mg) the possible complication rate would be less then 0.7 percent, none of them serious. In the ulnar, radial and median nerve block, amounts of lidocaine up to 300 mg have been described. While not injected systemically in this type of block, the concentration is still 3.5 times what is being described in the modified approach.
 |
| Figure 3 |
|---|
There have been comments about bleeding from injection sites resulting in theoretical toxin washout with the hyperemia that comes after the tourniquet has been released [23]. With the small 31 gauge needle and the 45 degree injection, which seems to allow the tissue to compress the thin needle track, there is almost no bleeding from the tiny injection sites. All the Botox™ remains at the site of injection and does not leak out.
I do not use the iodine-starch test for the hands and feet. Unlike the underarms, where it serves to show injections points for hyperhidrotic areas, in all patients that I have treated, the whole palm and fingers (plantar foot and toes) have been involved in excessive sweating and testing these areas would serve no useful purpose in a clinical setting. Success is measured by patient satisfaction upon follow-up phone calls, not by an improved starch-iodine test performed a few weeks following the injections. It also serves no purpose at subsequent visits since the test would be invalid due to the fact that some areas will not have fully recovered from the Botox™ injections.
Regarding the pneumatic tourniquet, in no instance should a standard blood pressure cuff be used to occlude arterial blood flow because it is unreliable in holding a steady pressure and will result in an inadequate block. Although the pressure described can be higher than the 100 torr more than the patient's systolic pressure that is usually used, for the short time that the tourniquet is inflated it does not cause patient discomfort, nor have there been any reported instances of nerve damage for this short length of inflation and is a good standard pressure. There are several available types of automated occlusion machines costing $1,000-$2,000. If a physician plans to perform more then a dozen of this type of block per year, the cost will be easily recouped and the device will ensure a proper block.
The most difficult part of the procedure can occasionally be finding a vein for catheter placement. There are very rare occasions when the HH can cause patients to have vascular clamp down with venous access difficult. In these infrequent cases an ulnar, median and radial nerve block can be performed.
The fact that the modified Bier block technique is very safe, easy to learn and administer and allows full recovery within a very short time, makes it the anesthetic technique of choice in the office setting for providing a pain-free injection field for Botox™ injections in the hands and feet to treat hyperhidrosis.
References
1. Schnider P, Binder M, et al. Double-blind trial of botulinum A toxin for the treatment of focal hyperhidrosis of the palms. Br J Dermatol 1997;136:548-5522. Holmes S, Mann C, et al. Botulinum toxin in the treament of palmar hyperhidrosis. J Am Acad Dermatol 1998;39:1040-1041
3. Naumann M, Hofmann U, et al. Focal hyperhidrosis: effective treatment with intra cutaneous bolulinum toxin. Arch Dermatol 1998;134:301-304
4. Shelly WB, Talanin, et al. Botulinum toxin therepy for palmar hyperhidrosis. J Am Acad Dermatol 1998;38:227-229
5. Hockmann M, Schaller, et al. Optimizing botulinum toxin therapy for hyperhidrosis. Br J Dermatol 1998;138:553-554
6. Naumann M, Bergman I, et al. Botulinum toxin for focal hyperhidrosis: technical considerations and improvements in application. Br J Dermatol 1998;139:1123-1124
7. Naumann M, Flachenecker P, et al. Botulinum toxin for palmar hyperhidrosis. Lancet 1997;349: 252
8. Trinidade De Almeida A, Kadung B, et al. Improving Botulinum Toxin Therapy for Palmar Hyperhidrosis: Wrist Block and Technical Considerations. Dermatol Surg 2001; 27:34-36
9. Odderson IR. Axillary hyperhidrosis treatment with botulinum toxin A. Arch Phys Med Rehab 1998;79:350-352
10. Glogau RG. Botulinum A neurotoxin for axillary hyperhidrosis. No sweat Botox. Dermatol Surg 1998;24:817-818
11. Odderson IR. Hyperhidrosis treatment by botulinum A exotoxin. Dermatol Surg 1998;24:1237-1241
12. Saddia D, Voustianiouk A, et al. Botulinum toxin type A in primary palmar hyperhidrosis. Neurology 2001;57:2095-2099
13. Benohanian A. Surgical Pearl: Use of needle-free anesthesia in the treatment of palmar hyperhidrosis with botulinum A toxin. J Am Acad Dermatol 2005;52:1073-1074
14. Vadoud-Seyedi J, Simonart, T, et al. Treatment of Plantar Hyperhidrosis with Dermojet Injections of Botulinum Toxin Dermatology 2000;201:179
15. Benohanian, Antranik Palmar hyperhidrosis. Needle free anesthesia as an alternative to Bier's block and peripheral nerve blockade for botulinum toxin therepy. Dermatology Online Journal 12(6):26
15. Smith, K, Comite, S, et al. Vibration Anesthesia: A noninvasive method of reducing discomfort prior to dermatologic procedures. Dermatology Online Journal 2006;10(2):1
16. Moraru E, Auff E, et al. Hyperhidrosis of the palms and soles. Current Probl Dermatol 2002;30:156-169
17. Fugita M, Mann T, et al Surgical Pearl: Use of nerve blocks for botulinu toxin treatment of palmar-plantar hyperhidrosis J.Am Acad Dermatol 2001;45:587-589
18. Selender D. Peripheral nerve damage and regional anaesthesia. Br J Anaesth 1995;75:116-117
19. Selander D, Dhuner KG, et al. Peripheral nerve injury due to injection needles used for regional anesthesia. Acta Anaesth Scand 1977;21:182-188
20. Moore DC, Mulroy MF, et al. Peripheral nerve damage and regional anesthesia. Br J AnaesthI. 1994;73:435-436
21. Hernot S, Samii K. Different types of nerve injuries in locoregional anaesthesia. Ann Fr Anesth ReanimI 1997;16:927-934
22. Blaheta H-J, Vollert B, et al. Intravenous Regional Anesthesia (Bier's Block) for Botulinum Toxin Therapy of Palmar Hyperhidrosis is Safe and effective. Dermatol Surg 2002;28:666-672
23. Bier A. Uber einen neuen Weg Lokalanesthesie und den GliedmaBen ze erzuegen. Arch Klin Chir 1908;86:1007
24. Blaheta H-J, Deusch H, et al. Intravenous regional anesthesia (Bier's block) is superior to a peripheral nerve block for painless treatment of plantar hyperhidrosis with botulinum toxin. J Am Acad Dermatol 2003;48:302-304
25. Brown E, McGriff J, et al. Intravenous regional anaesthesia (Bier block): review of 20 years' experience. Can J Anaesth 1989;36:307-310
26. Vollert B, Blaheta H-J, et al. Intravenous regional anaesthesia for treatment of palmar hyperhidrosis with botulinum toxin type A. Br. J Dermatol 2001;133:632-633
27. Ponce-Olivera RM, Tirado-Sanchez A, et al. Palmar hyperhidrosis. Safety and efficacy of two anesthetic techniques for botulinum toxin therapy. Dermatology Online Journal 12(2): 9
28. Solomon, P. Hyperhidrosis Faculty Training and Curriculum Development Meeting. June 27-29, 2003; Chicago, Ill
29. Rosenberg PH, Kalso EA, et al. Acute bupivacaine toxicity as a result of venous leakage under the tournique cuff during a Bier block. Anesthesiology 1983;58:95-98
30. Heath ML. Bupivacaine toxicity and Bier blocks. Anesthsiology 1983;59:481
© 2007 Dermatology Online Journal

