Lassueur-Graham-Little-Piccardi syndrome
Published Web Location
https://doi.org/10.5070/D36dx536t6Main Content
Lassueur-Graham-Little-Piccardi syndrome
Monika Srivastava MD, Radha Mikkilineni MD, Jody Konstadt MD
Dermatology Online Journal 13 (1): 12
New York University Department of DermatologyAbstract
A 52-year-old man presented for evaluation of patchy alopecia of the scalp, axilla, and groin and of follicular spiny papules. Histopathologic examination showed a dense, follicular, lymphocytic infiltrate and interfollicular interface changes. Lassueur-Graham-Little-Piccardi syndrome is characterized by the triad of scarring, patchy alopecia of the scalp, non-cicatricial alopecia of the axillae and pubis, and a keratotic, follicular eruption. There may be an etiologic relationship with lichen planus. Treatment is difficult, although isolated reports have demonstrated success with cyclosporin and thalidomide.
Clinical synopsis
A 52-year-old man presented to his dermatologist with a pruritic eruption that involved the trunk and extremities. He noted patchy hair loss of the scalp and patches of hair loss in the left axilla and the pubis. The patient denied constitutional symptoms. Review of symptoms was negative for photosensitivity, oral ulcers, and cardiopulmonary complaints. He was not taking any medications. Past treatment with prednisone had reduced hair loss of scalp and also improved the eruption on his trunk and extremities.
 |  |
| Figure 1 | Figure 2 |
|---|
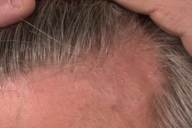
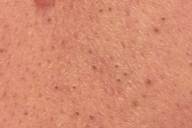
On the mid and lower areas of the back and on the arms, follicular, 1-mm, spiny papules were present. In the scalp there were patches of scarring alopecia without erythema. In the left axilla and in the suprapubic area there were patches of nonscarring alopecia.
 |
| Figure 3 |
|---|
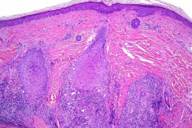
Histopathology reveals a dense peri-follicular lymphocytic infiltrate. Lymphocytes extend into the basal layer, and there is focal vacuolar alteration of the follicular basement membrane
Comment
Lassueur-Graham-Little-Piccardi syndrome is characterized by a triad of features that include scarring alopecia of the scalp, non-cicatricial alopecia of the axillae and pubis, and a lichenoid follicular eruption. It was initially described by Piccardi in 1913. In 1915, Graham-Little published a similar case observed by Lassueur [1]. Since then several case reports of this syndrome have been published.
Clinically, the scarring alopecia often precedes the follicular eruption by months to years [2]. The follicular eruption has been characterized as several related or similar entities that include keratosis pilaris, lichen spinulosis, follicular lichen planus, and lichen planopilaris [3, 4]. Pruritus often can be severe although it is not always constant. Lassueur-Graham-Little-Piccardi syndrome has usually been described in middle-aged women [5]. The differential diagnosis includes folliculitis spinulosa decalvans, discoid lupus erythematosus, follicular mucinosis, sarcoidosis, and keratosis pilaris atrophicans [6].
The etiology of Lassueur-Graham-Little-Piccardi syndrome remains controversial. It has been associated with classic lichen planus [7]. There has been a case report linking the syndrome to hepatitis-B vaccination [8]. There have been cases of familial Lassueur-Graham-Little-Piccardi syndrome. A mother and daughter afflicted with this syndrome were reported. Both patients demonstrated HLA-DR1 [6]. This HLA type is also seen in familial cases of lichen planus and provides further evidence that Lassueur-Graham-Little-Piccardi is etiologically related to lichen planus. A case of Lassueur-Graham-Little-Piccardi syndrome in a patient with complete androgen insensitivity syndrome was reported [9]. It is unclear if there is any causal relationship between these two conditions.
Treatment of the Lassueur-Graham-Little-Piccardi syndrome is difficult with respect to both the scarring alopecia and the follicular, keratotic eruption. Topical, intralesional, and systemic glucocorticoids, retinoids, and PUVA photochemotherapy have not been consistently successful. There has been a case report of treatment with cyclosporin (4 mg/kg/day) with improvement in erythema, hyperkeratotic papules, and induction of partial hair growth in the patient [5]. There also has been anecdotal success with thalidomide [10].
References
1. Ghislain PD, et al. Lassueur-Graham Little-Piccardi syndrome: a 20-year follow-up. Dermatology 2003;206:3912. Dawber RPR, et al. Disorders of hair: cicatricial alopecia. In: Champion RH, et al., eds. Rook-Wilkinson-Ebling Textbook of Dermatology, sixth edition. Oxford: Blackwell Science, 1998: 2935
3. Pages F, et al. Syndrome de Lassueur-Graham Little. Ann Dermatol Syphiligr 1961;88:272
4. de Graciansky P, Pons A. Syndrome de Graham Little-Lassueur. Bull Soc Fr Dermatol Syphiligr 1969;76:849
5. Kubba R, Rook A. Graham Little syndrome: follicular keratosis with cicatricial alopecia. Br J Dermatol 1975;93(suppl 11):53
6. Viglizzo G, et al. Familial Lassueur -Graham-Little-Piccardi syndrome. Dermatology 2004;208:142
7. Crickx B, et al. Syndrome de Lassueur-Graham Little: 2 observations. Ann Dermatol Venereol 1990;117: 7
8. Bardazzi F, et al. Graham Little-Piccardi-Lassueur syndrome following HBV vaccination. Acta Derm Venereol 1999;79:93
9. Vega Gutierrez J, et al. Graham Little-Piccardi-Lassueur syndrome associated with androgen insensitivity syndrome (testicular feminization). J Eur Acad Dermatol Venereol 2004;18:463
10. George SJ, Hsu S. Lichen planopilaris treated with thalidomide. J Am Acad Dermatol 2001;45:965
© 2007 Dermatology Online Journal

