Plate-like cutaneous osteoma on the scalp
Published Web Location
https://doi.org/10.5070/D36dg4434jMain Content
Plate-like cutaneous osteoma on the scalp
Thaer Douri, AZ Shawaf
Dermatology Online Journal 12 (4): 17
Ministry of Health, Syria-Hama. s-dori@scs-net.orgAbstract
Platelike osteoma cutis is a rare lesion that is most often congenital. We report a 25-year-old woman who developed a linear plate of subcutaneous bone in a normal area of scalp.
Platelike osteoma cutis is a rare lesion that is most often congenital [1]. Primary ossification of cutaneous and subcutaneous tissues rarely may occur without any underlying tissue abnormality or preexisting calcification [2]. We report a case of primary ossification recognized as plate-like cutaneous osteoma.
Clinical synopsis
A 25-year-old woman had a hard linear plate-like lesion of the scalp (Fig. 1). The lesion started 5 years before and there was no history of a previous problem in that area (i.e., no trauma, morphea, or nevus). All routine blood tests, including calcium and phosphorus, were normal.
Physical examination revealed a hard linear plate-like subcutaneous mass under a normal epidermis. The lesion was surgically removed.
The histopathology examination showed intradermal and subepidermal bone tissue composed of calcified bone trabeculae disposed in plate-like or sheet array, and including haversian canals, osteoclasts, and osteoblasts (Fig. 2).
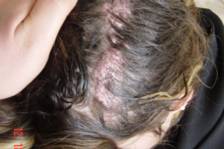 | 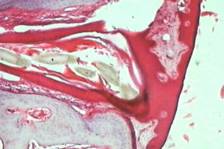 |
| Figure 1 | Figure 2 |
|---|
Discussion
Osteoma cutis is a rare, benign skin disorder characterized by the formation of bone in skin. There are two major classes of osteoma cutis, primary and secondary. Secondary osteoma cutis can be a sequel of multiple disorders including nevi, scleroderma, pilomatricoma (Malherbe calcifying epithelioma), dermatomyositis, basal cell carcinoma, scars, inflammation, trauma, calcification of appendageal and fibrous proliferations, and venous stasis. Most commonly it is seen in patients with a long history of acne and scarring. In patients treated with oral tetracycline or minocycline, the osteomas may develop pigmentation and appear bluish [4].
Primary ossification of cutaneous and subcutaneous tissues rarely occurs, and is without any underlying tissue abnormality or preexisting calcification [2].
Primary ossification of the skin occurs in four major clinical settings in the absence of preexisting skin lesions. The first is characterized by generalized neonatal nodules extending into the subcutaneous tissue (without evidence of Albright hereditary osteodystrophy). The second group includes patients with a single plate-like osteoma of the scalp or extremities appearing in the neonatal period without evidence of antecedent trauma or infection. The third group involves a small osteoma, presenting later in life, anywhere on the body; transepidermal elimination of chalky bone may occur [3]. The fourth type was reported by Worret and Burgdorf who described plate-like osteoma cutis in a 4-month-old infant who had a slowly enlarging bony plate within the dermis on the lateral thigh and knee. In addition, they described 12 other patients who had similar findings. Based on these cases, they coined the term plate-like osteoma cutis and proposed the diagnostic criteria as follows [2]:
- lesion present at birth or within the first year of life
- no evidence of abnormal calcium or phosphorus metabolism
- no history of infection, trauma, or other predisposing events
- the presence of at least one bony plate with or without other cutaneous osteomas.
Further reports of plate-like osteoma cutis are in the literature. An 18-year-old woman had a progressive enlarging plate of subcutaneous bone in the scalp since birth [5]. A 7-year-old girl was reported with a plate-like cutaneous ossification of the forehead resulting in aesthetic deformities. She had other dermal ossifications in the inguinal and preauricular region, as well as the left hand and a small focus in the extraocular muscles of the left orbit [6].
Our patient may be categorized as plate-like osteoma of the scalp, also not originating in the neonatal period. The lesion began at about age 20 and was without a history of antecedent trauma. Not all cases of osteoma cutis can be clearly categorized [3].
The pathogenesis of primary osteoma cutis remains unclear. Burgdorf and Nasemann theorized two possible processes; one theory assumes a disordered embryologic process, whereby primitive mesenchymal cells differentiate normally into osteoblasts but migrate to the wrong location. However, this remains speculative. The second theory, which appears more plausible, interprets the presence of bone as a result of osteoblastic metaplasia of mesenchymal cells, such as fibroblasts [4].
Treatment of osteoma cutis primarily involves surgical excision. Excellent cosmetic results have occurred in cases of acne-induced osteoma cutis after full-face dermabrasion and punch excisions of individual osteomas [3]. Our patient was treated with surgical excision.
References
1. Monroe AB, Burgdorf WH, Sheward S. Platelike cutaneous osteoma. J Am Acad Dermatol. 1987 Feb;16(2 Pt 2):481-4. PubMed2. Worret WI, Burgdorf W. [Congenital, plaque-like osteoma of the skin in an infant]. Hautarzt. 1978 Nov;29(11):590-6. PubMed
3. Touart DM, Sau P. Cutaneous deposition diseases. Part II. J Am Acad Dermatol. 1998 Oct;39(4 Pt 1):527-44; quiz 545-6. PubMed
4. Altman JF, Nehal KS, Busam KJ, Halpern AC. Treatment of primary miliary osteoma cutis with incision, curettage, and primary closure. J Am Acad Dermatol. 2001 Jan;44(1):96-9. PubMed
5.Sanmartin O, Alegre V, Martinez-Aparicio A, Botella-Estrada R, Aliaga A. Congenital platelike osteoma cutis: case report and review of the literature. Pediatr Dermatol. 1993 Jun;10(2):182-6. PubMed
6. Tresserra L, Tresserra F, Grases PJ, Badosa J, Tresserra M. Congenital plate-like osteoma cutis of the forehead: an atypical presentation form. J Craniomaxillofac Surg. 1998 Apr;26(2):102-6. PubMed
© 2006 Dermatology Online Journal

