Secondary syphilis clinically mimicking pseudolymphoma of the face
Published Web Location
https://doi.org/10.5070/D36918r8tbMain Content
Secondary syphilis clinically mimicking pseudolymphoma of the face
Dr Arfan ul Bari MBBS MCPS FCPS1, and Dr Naeem Raza MBBS MCPS FCPS2
Dermatology Online Journal 12 (3): 20
1. Combined Military Hospital Muzaffarabad, Pakistan. albariul@gmail.com2. Combined Military Hospital Abbottabad, Pakistan
Abstract
Syphilis has been given titles such as the great imitator, the great mimic, and the great masquerader. It may lack pathognomonic signs and often presents similar to many other dermatological conditions. We present a case of a young woman who developed asymptomatic papulonodular lesions on the forehead; the lesions were clinically similar to pseudolymphoma but it was determined that she had secondary syphilis exhibiting prozone phenomenon. She also had alopecia of eyebrows. Both the alopecia as well as nodular lesions clinically resembling pseudolymphoma responded to and completely recovered with antisyphilitic treatment.
Syphilis remains a public health problem worldwide. The World Health Organization estimates that there are 12 million new cases of syphilis each year, with more than 90 percent occurring in developing nations [1]. Early (primary or secondary) syphilis is typically marked by ulcerative lesions that occur initially at the site of inoculation (primary), followed several months later by widespread cutaneous, mucosal, and even systemic manifestations (secondary) of the dissemination of the causal agent,Treponema pallidum. Even without treatment, both primary and secondary lesions resolve, and the infection enters a latent stage. During this stage, there are no clinical manifestations of disease, yet the infection may still be passed to children born to infected mothers; and it may progress, resulting in late manifestations (tertiary syphilis) [1, 2]. Secondary syphilis is often a subtle disease; the skin lesions may be easily overlooked and may mimic other dermatologic diseases. Skin rash is usually macular to maculopapular or papulosquamous which is symmetrically distributed and nonpruritic. Occasionally follicular and pustular lesions are seen but nodular and ulcerative lesions are very rare [1, 3]. Alopecia in different forms is also one of the presentations of the disease [2, 4]. The diagnosis of syphilis is based on clinical findings, demonstration of the causative agent under microscope, and serologic tests for syphilis [1, 3]. Very rarely, high antibody titer in undiluted specimens may result in false negative results of serological tests for syphilis; this is called the prozone phenomenon [5]. The organism is sensitive to penicillin, which remains the mainstay of therapy [1]. About one third of untreated patients with syphilis develop recognizable late complications. A higher mortality rate has been noted in populations with syphilis, and men are twice as likely to develop late complications [6]. Early recognition and treatment of syphilis is desirable.
Clinical synopsis
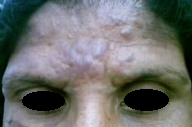
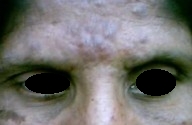
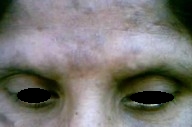
A 29-year-old woman (housewife from a countryside village) presented to PAF Hospital Sagodha with asymptomatic dusky erythematous papulonodular lesions on her forehead for 3 weeks. There was no history of fever, myalgia, arthralgia, or fatigue. She was a married house wife with four children. Her husband was serving in the army and visited home for about 1 week every 3-4 months. She denied extramarital relationships. On physical examination she had multiple, slightly violacious, nonpruritic, nontender papulonodular lesions on her forehead. These were centrally confluent to form a large nodular plaque. Two discrete isolated lesions were also located on right cheek. No similar lesions were found elsewhere on her body (Fig. 1). Diffuse alopecia of eyebrows was also noted (Figs. 2-4). Bilateral cervical lymph nodes were palpable and these were discrete, non tender, and mobile. Systemic examination was unremarkable.
 |
| Figure 5 |
|---|
| Figure 5. Followup 3 months after treatment (Completely recovered alopecia eye brows) |
Her blood complete picture, urine analysis and metabolic profile were within normal limits, and chest X-Rays also revealed no abnormality. Serum Venereal Disease Research Laboratory test (VDRL) was reported to be negative. Considering the asymptomatic nature of the lesions and negative VDRL, she was provisionally suspected as a case of pseudolymphomas; skin biopsy of an isolated peripheral lesion located along frontal hairline was performed. Histopathology of the lesion revealed dense perivascular plasma cell infiltrate in mid and deep dermis. In view of histopathology report VDRL was repeated with diluted serum and it was positive even at very high dilution [1:512]. Treponema pallidum haemagglutinationassay was also positive (1:64). Human immunodeficiency virus (HIV) screening was negative. Keeping in view the suggestive histopathology of the lesion and positive serological tests for syphilis (both treponemal and non treponemal tests) even at very high dilution, she was diagnosed as a case of secondary syphilis clinically mimicking pseudolymphoma and exhibiting prozone phenomenon in the laboratory. She was treated with two injections of Benzathine penicillin 2.4 million units intramuscularly at weekly interval. Her skin lesions started improving even after first dose (Fig. 2) and completely disappeared 4 weeks after treatment (Fig. 3, 4). Alopecia recovered in 3 months (Fig. 5) and VDRL was only positive in 1:4 dilutions (revealing a marked decline in antibody titre) Her husband was also contacted and treated simultaneously. He was counseled for contact tracing and methods of safe sex in future. Treatment of contacts was also emphasized.
Discussion
Secondary syphilis most commonly presents with a maculopapular or papulosquamous eruption that symmetrically involves the trunk and extremities. Sometimes only palms, soles, and mucous membranes are affected. Occasionally alopecia of scalp or eyebrows may be associated or be the only manifestation of the disease [2, 3, 4]. The papulonodular variant is rarely been described in the literature. Noduloulcerative lesions are also very uncommon and are only reported in association with concurrent HIV infection or lues maligna, a pustuloulcerative form of secondary syphilis that occurs in association with fever, headaches, and arthralgias [7, 8]. Our patient had many unusual features such as localization of the lesions to forehead and one cheek only, clinical resemblance of the lesions to those of pseudolymphoma, localization of alopecia to eyebrows, and exhibition of prozone phenomenon in the laboratory. It was only the histopathology report that raised the suspicion of syphilis and was later confirmed by serological tests done on diluted serum. Prozone phenomenon (also called hook effect) is more prevalent in HIV-positive individuals with syphilis than in luetic patients who are negative for HIV and similarly may be expected more frequently in syphilitic patients having multiple myeloma or other imunodefeciency states. This is likely to be due to B-cell dysregulation, leading to higher nontreponemal serologic titers [5, 9, 10]. In our case, it occurred in a previously healthy, non-HIV patient without any concurrent systemic manifestations.
Conclusion
Missed or neglected cases of syphilis progress to late syphilis, which has a significant rate of mortality and morbidity. Early diagnosis and treatment of syphilis will contributes to reducing the incidence of mortality as well as morbidity caused by syphilis. Secondary syphilis should be considered in the differential diagnosis of nodular lesions on face and alopecia of eyebrows. Syphilis should be added to the list of diagnoses belonging to the category of pseudolymphoma or lymphocytoma cutis.
References
1. Hook EW, Peeling RW. Syphilis Control - A Continuing Challenge. N Engl J Med 2004; 351: 122-4.2. Sanches MR. Syphilis: sexually transmitted diseases. In: Freedberg IM, Eizen AZ, Wolff K, Austen KF, Goldsmith LA, Katz SI, editors. FitzpatrickÕs Dermatology in general medicine. 6th ed. New York: Mc Graw Hill; 2003. vol II. p. 2163-88.
3. Chapel TA. The signs and symptoms of secondary syphilis. Sex Transm Dis1980;7:161-4
4. Cuozzo DW, Benson PM, Sperling LC, Skelton HG. Essential syphilitic alopecia revisited. J Am Acad Dermatol 1995; 32: 840-3.
5. el-Zaatari MM, Martens MG, Anderson GD. Incidence of the prozone phenomenon in syphilis serology. Obstet Gynecol 1994; 84: 609-12.
6. Clark, E. G., and N. Danbolt. The Oslo Study of the natural course of untreated syphilis. An epidemiologic investigation based on a re-study of the Boeck-Bruusgaard material. Med Clin North Am 1964; 48: 613-23.
7. McComb ME, Telang GH, Vonderheid EC. Secondary syphilis presenting as pseudolymphoma of the skin. J Am Acad Dermatol 2003; 49: S174-6.
8. Hodak E, David M, Rothem A, Bialowance M, Sandbank M. Nodular secondary syphilis mimicking cutaneous lymphoreticular process. J Am Acad Dermatol 1987; 17: 914-7.
9. Jurado RL, Campbell J, Martin PD. Prozone phenomenon in secondary syphilis. Has its time arrived? Arch Intern Med. 1993; 153: 2496-8.
10. Young H. Guidelines for serological testing for syphilis. Sex Transm Infect 2000; 76: 403-5.
© 2006 Dermatology Online Journal