Familial benign chronic pemphigus (Hailey-Hailey disease)
Published Web Location
https://doi.org/10.5070/D35x694103Main Content
Familial benign chronic pemphigus (Hailey-Hailey disease)
Melanie Warycha MD, Rishi Patel MD, Shane Meehan MD, Joseph F Merola MD
Dermatology Online Journal 15 (8): 15
Department of Dermatology, New York UniversityAbstract
A 57-year-old woman presented with a 27-year history of vesicles and crusted erosions of the intertriginous folds. Prior treatments had included topical glucocorticoids, mupirocin, and minocycline, all of which provided minimal relief. A skin biopsy specimen was consistent with Hailey-Hailey disease. Hailey-Hailey disease is the result of mutations in the ATP2C1 gene and is characterized by recurrent vesicles and erosions in intertriginous areas. Whereas topical and/or systemic antibiotic/antifungal agents in combination with topical glucocorticoids is the mainstay of treatment, case reports have documented dramatic improvement with oral retinoids, calcitriol, and tacrolimus.
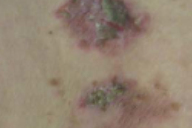 | 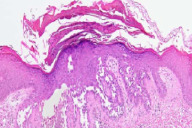 |
| Figure 1 | Figure 2 |
|---|
History
A 57-year-old woman presented to the Charles C. Harris Skin and Cancer Unit in January, 2009, with a 27-year history of vesicles and crusted erosions of the intertriginous folds. These lesions began to erupt on her back at the age of 30 years, with eventual spread to the hips, flanks, inframammary areas, axillae, and inguinal areas. The lesions were associated with a stinging and burning sensation but, on occasion, were noted to be pruritic. She reported that the eruption would flare around the time of her menstrual periods. The patient denied any other modifying factors, which included seasonal variation, heat, friction, or sweating. Her sister and daughter both had similar lesions although her presentation was the most severe. The patient had consulted several dermatologists prior to her visit and had one previous biopsy. Prior treatments had included topical glucocorticoids, mupirocin, and minocycline, all of which provided minimal relief. Four months prior to presentation to our clinic, she experienced a flare in the right inguinal fold, with soreness of the perianal and vulvar areas. Oral prednisone was initiated, and she experienced an improvement in the recurrence and quantity of erosions. However, this medication was discontinued because she could not tolerate side effects of fatigue and stomach upset. On presentation to our clinic, she received intralesional triamcinolone injections to the right inframammary lesion and right medial thigh, at a dose of 10 mg/ml and total injection quantity of 1.5 ml. In addition, she was started on doxycycline 100 mg twice daily and lidex ointment. On a follow-up visit, calcipotricine cream was added, which the patient believes has decreased the quantity of erosions she develops. She denies new vesicle formation. Past medical history includes hypothyroidism and hypercholesterolemia. Medications include levothyroxine, atorvastin, and orlistat. Review of systems was negative.
Physical Examination
On the inframammary and inguinal regions and on the left hip, were erythematous plaques with overlying crusts and maceration. The remainder of the examination, with included the oropharynx, was negative.
Laboratory data
None.
Histopathology
There is epidermal hyperplasia with suprabasal acantholysis that involves the spinous layer giving a 'dilapidated brick wall' appearance.
Comment
Familial benign chronic pemphigus (Hailey-Hailey disease) is an autosomal dominant disease that is characterized by recurrent, fragile, vesicles and erosions in intertriginous areas (i.e., axillary folds, groin, submammary region, and neck folds). Skin lesions most commonly present between the second to fourth decades of life and can be pruritic, painful, and malodorous; recurrent lesions may lead to restricted mobility [1]. Healing occurs without scars. Longitudinal white bands in the fingernails, which are not associated with nail fragility, may facilitate diagnosis in patients with limited or atypical disease presentations. Hailey-Hailey disease has a chronic, relapsing-remitting course and can be exacerbated by friction, heat, sweating, constrictive clothing, physical trauma, infection, and stress [2]. In addition, approximately 17 percent of female patients experience premenstrual worsening of their disease, which suggests that sex hormones may play a role [3]. Histopathologic examination shows widespread suprabasal acantholysis with loss of intercellular bridges, which results in a dilapidated brick-wall appearance. Necrotic keratinocytes are uncommon, and direct immunofluorescence tests are negative [2].
Recent studies have demonstrated that Hailey-Hailey disease is the result of mutations in the ATP2C1 gene, which encodes Ca2+/Mn2+- ATPase protein 1 (hSPCA1), that is localized to the Golgi apparatus [4]. Keratinocytes with an ATP2C1 mutation, thus, have deficient Ca2+ signaling, with dysregulated sorting and glycosylation of desmosomal proteins, which gives rise to epidermal defects in skin lesions. A total of 98 ATP2C1 mutations have been reported worldwide in patients with Hailey-Hailey disease. Linkage analysis has localized the gene locus to chromosome 3q21-q24 [5]. Two clinical segmental variants have been identified. Segmental type 1 occurs in patients with a heterozygous postzygotic mutation. Segmental type 2 is a result of somatic loss of the wild-type allele that leads to segmental homozygosity. In this clinical variant, acantholysis also is seen within adnexal structures [2].
Patients with Hailey-Hailey disease should avoid potential aggravating factors, such as friction and sweating. Furthermore, treatment with topical and/or systemic antibiotic/antifungal agents should be initiated if colonization is suspected. Topical antimicrobials are often used in combination with topical glucocorticoids [1]. Alternative topical treatments with reported success include topical calcitriol [6] and tacrolimus ointment [7]. Case reports have documented improvement with oral retinoids [8], and one report noted a lasting response of 50 percent clinical improvement above baseline with Alefacept, with a decrease in the severity of disease flares five months after therapy [9]. In some patients, disease can be recalcitrant to medical treatments, and more invasive approaches may be required. Wide surgical excision of intertriginous folds, although still a therapeutic option, is associated with appreciable morbidity and complications, which include scar contractures and restricted mobility, graft failure, and thromboembolic events; thus this surgery has fallen out of favor [10]. Carbon dioxide laser ablation is a less invasive approach although problems with hypertrophic scars have been reported [11]. Radiotherapy has also had success in local disease control although it does not seem to influence the natural course of the disease [12].
References
1. Burge SM. Hailey-Hailey disease: the clinical features, response to treatment and prognosis. Br J Dermatol 1992;126:275 [PubMed]2. Hohl D, Mauro T. Darier Disease and Hailey-Hailey Disease. In: Bologna J, et al, eds. Dermatology, 2nd edition. 2008: 798
3. Szigeti R, et al. Premenstrual exacerbation in calcium ATPase disorders of the skin. J Eur Acad Dermatol Venereol 2007;21:412 [PubMed]
4. Hu Z, et al. Mutations in ATP2C1, encoding a calcium pump, cause Hailey-Hailey disease. Nat Genet 2000;24:61 [PubMed]
5. Zhang ZZ, et al. Three novel ATP2C1 mutations in Chinese patients with Hailey-Hailey disease. Br J Dermatol 2008;158:831 [PubMed]
6. Bianchi L, et al. Treatment of Hailey-Hailey disease with topical calcitriol. J Amer Acad Dermatol 2004;51:475 [PubMed]
7. Rabeni EJ, Cunningham NM. Effective treatment of Hailey-Hailey disease with topical tacrolimus. J Am Acad Dermatol 2002;47:797 [PubMed]
8. Berger EM, et al. Case reports: successful treatment of Hailey-Hailey disease with acitretin. Drugs Dermatol 2007;6:734 [PubMed]
9. Hurd DS, et al. A case report of Hailey-Hailey disease treated with alefacept (Amevive). Br J Dermatol 2008;158:399 [PubMed]
10. Hamm H, et al. Hailey-Hailey disease: eradication by dermabrasion. Arch Dermatol 1989;21:1506
11. Kartamaa M, Reitamo S. Familial benign chronic pemphigus (Hailey-Hailey disease): treatment with carbon dioxide laser vaporization. Arch Dermatol 1992;128:646 [PubMed]
12. Narbutt J, et al. Effective treatment of recalcitrant Hailey-Hailey disease with electron beam radiotherapy. J Eur Acad Dermatol Venereal 2007;21:567 [PubMed]
© 2009 Dermatology Online Journal

