Annular epidermolytic ichthyosis
Published Web Location
https://doi.org/10.5070/D35wj9c3tvMain Content
Annular epidermolytic ichthyosis
Narayan S Naik MD
Dermatology Online Journal 9(4): 4
From the Ronald O. Perlman Department of Dermatology, New York University
Abstract
A 21-year-old woman presented to the Charles C. Harris Skin and Cancer Pavilion with a life-long history of palmoplantar keratoderma that was accompanied by episodic flares of polycyclic psoriasiform patches diffusely over the rest of her body. A biopsy specimen of a representative skin lesion showed epidermolytic hyperkeratosis. The particular phenotype that this patient exhibited has been reported in only seven families previously in the literature. Mutations in keratin 1 and 10 have been identified in these patients and are similar to those mutations in patients with classic epidermolytic hyperkeratosis.
Clinical summary
History.—A 21-year-old woman presented to the Charles C. Harris Skin and Cancer Pavilion in April 2001 with a history of palmoplantar keratoderma accompanied by episodic, slowly migratory, red patches with scale that involved the trunk and extremities and thickened, dirty-brown, corrugated plaques over the knees, elbows, and ankles. She was born premature but had no evidence of erythroderma or blisters at birth. The lesions began sometime during the first year of life. The patient denied problems with her hair, teeth, or nails. Previous treatments, which included topical tretinoin, oral isotretinoin, topical glucocorticoids, and keratolytics, have not resulted in sustained clinical improvement. Initially, she was thought to have an unusual variant of psoriasis and was treated with cyclosporine for a 3-month period without benefit. She was in otherwise good health and took no other medications except oral contraceptives. Her mother and numerous maternal relatives also had a history of palmoplantar keratoderma. Her father and sister were unaffected. A biopsy was obtained in July 2001 from a migratory erythematous patch. After the diagnosis was made, treatment with tazorotene cream was begun shortly thereafter and resulted in some clinical improvement.
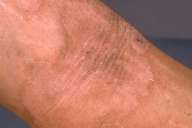
Physical examination.—Brown-black, hyperkeratotic, hyperlinear, ridged, verrucous plaques were present over the extensor surfaces of the knees, elbows, and ankles. Similar plaques affected the flexural areas of the axillae, antecubital fossae, and popliteal fossae. Yellow-brown, confluent, lichenified, and fissured hyperkeratotic plaques involved most of the palms and soles, with extension onto the dorsal aspects of the hands and feet. Polycyclic, psoriasiform, erythematous patches of variable size with annular scale involved large areas of the trunk and extremities. Examination of the hair, teeth, and nails did not show abnormalities. A KOH specimen taken from the leading edge of a scaly patch showed no fungal elements.
|
|
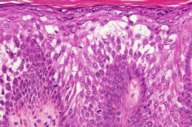
| Figure 1 | Figure 2 |
|---|
Laboratory data.—A complete blood count, liver function tests, chemistry panel, and lipid profile were normal.
Histopathology.—There is a hyperplastic epidermis with compact orthokeratosis and hypergranulosis with pronounced perinuclear vacuolization of the spinous keratinocytes with indistinct cell borders.
Diagnosis.—Annular epidermolytic ichthyosis (phenotypic variant of epidermolytic hyperkeratosis or bullous congenital icthyosiform erythroderma).
Comment
Bullous congenital ichthyosiform erythroderma is an autosomal dominant disorder classically presenting with widespread erythroderma and blisters at birth. With age, ichthyosis and ribbed hyperkeratosis may develop in association with a palmoplantar keratoderma. There is a great deal of clinical heterogeneity reported in this disorder. A wide variety of mutations in conserved regions of keratins 1 and 10 correlate with the variable phenotyes observed. All variants share a similar histologic and ultrastructural picture. Hyperkeratosis, vacuolization within the spinous and granular layers, and irregular, dense, keratohyalin granules are characteristic light microscopic features. Electron microscopy shows clumps of keratin filaments in the suprabasal layer.
The distinct phenotype seen in our patient has only been described in seven families thus far in the literature. Sahn et al. first reported this phenotype in 1992 and coined the term annular epidermolytic ichthyosis [1]. Since this initial report, Joh et al. identified a patient with similar clinical features that had a novel dinucleotide mutation within the 2B segment of the keratin 10 gene that was passed on to offspring [2]. This finding suggested that this phenotype probably represented a clinical variant of bullous congenital ichthyosiform erythroderma. Further evidence was provided by the discovery of another keratin 10 mutation in the helix termination region by Suga et al. in 1998 [3]. Keratin 1 mutations have been subsequently described in patients with similar clinical findings by Sybert et al., Yang et al., and Michael et al. [4, 5, 6]. However, the molecular mechanisms that caused the phenotype that results from these mutations is yet to be elucidated. It appears that most individuals experience a benign course with fairly localized disease.[1]
Treatment options in the small number of patients reported have included topical and oral retinoids, topical glucocorticoids, calcipotriene, and keratolytics.[1,6]
References
1. Sahn EE, et al. Annular epidermolytic ichthyosis: A unique phenotype. J Am Acad Dermatol 1992;27:348.2. Joh G-Y, et al. A novel dinucleotide mutation in keratin 10 in the annular epidermolytic ichthyois variant of bullous congenital ichthyosis erythroderma. J Invest Dermatol 1997;108:357.
3. Suga Y, et al. A novel helix termination mutation in keratin 10 in annular epidermolytic icthyosis, a variant of bullous congenital ichthyosiform erythroderma. J Invest Dermatol 1998;111:1220.
4. Sybert VP, et al. Cyclic ichthyosis with epidermolytic hyperkeratosis: A phenotype conferred by mutations in the 2B domain of keratin k1. Am J Hum Genet 1999;64:732.
5. Yang J-M, et al. An alanine to proline mutation in the 1A rod domain of the keratin 10 chain in epidermolytic hyperkeratosis. J Invest Dermatol 1997;109:692.
6. Michael EJ, et al. Epidermolytic hyperkeratosis with polycyclic psoriasiform plaques resulting from a mutation in the keratin 1 gene. Exp Dermatol 1999;8:501.
© 2003 Dermatology Online Journal

