Proliferating trichilemmal cyst with focal calcification
Published Web Location
https://doi.org/10.5070/D35pk1k2pbMain Content
Proliferating trichilemmal cyst with focal calcification
Robert Anolik MD, Bahar Firoz MD, Ruth F Walters MD, Shane A Meehan MD, Hui C Tsou MD, Michael Whitlow MD PhD, Brent Wainwright
MD
Dermatology Online Journal 14 (10): 25
Department of Dermatology, New York UniversityAbstract
A 64-year-old man presented with a superficial, well-demarcated, skin-colored tumor on the left posterior scalp that measured 4 x 5 x 6 cm. The tumor was nearly hairless, rubbery, non-tender, and mobile over the underlying subcutaneous tissues. The lesion had grown slowly since arising approximately 30 years ago. Treatment options were declined in the past. However, with relatively more rapid growth over the past five years, the nodule began to cause intermittent pain and interfere with the patient's ability to lie on his back. The patient denied a history of similar lesions in himself or his family. A biopsy specimen showed a ruptured proliferating trichilemmal cyst with focal calcification. Complete excision is recommended for all benign proliferating variants owing to their potential for locally aggressive behavior and malignant transformation.
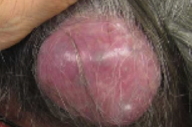 | 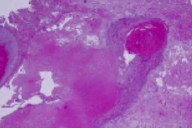 |
| Figure 1 | Figure 2 |
|---|
History
A 64-year-old man presented to the Veterans Affairs New York Harbor Healthcare System with a scalp nodule that had grown slowly since it arose approximately 30 years ago. Treatment options were declined in the past. Over the past five years, the rapid enlargement of the nodule was associated with intermittent pain that began to interfere with the patient's ability to lie on his back. The patient denied a history of similar lesions in himself or his family.
Medical history includes acne rosacea, diverticulosis, cataracts, retinal detachment, hyperlipidemia, and depression. Current medications include doxycycline, aspirin, and a multivitamin. He has no known drug allergies.
Physical Examination
A superficial, well-demarcated, skin-colored tumor that measured 4 x 5 x 6-cm over a normal skin base was located on the left posterior scalp medial to the mastoid process. The tumor was nearly hairless, rubbery, non-tender, and mobile over the underlying subcutaneous tissues.
Lab
None.
Histopathology
There are multiple, irregularly-shaped lobules and smaller aggregates of squamous epithelium that exhibit tricholemmal keratinization. The surrounding stroma is hyalinized with focal calcification. Granulation tissue is also noted.
Comment
The trichilemmal cyst, which is also known as a pilar cyst or wen, is clinically indistinguishable from the epidermoid cyst [1, 2]. Few clinical features may favor the diagnosis of a trichilemmal cyst although none are pathognomonic. About 90 percent of trichilemmal cysts are found on the scalp and an overlying punctum is normally absent [1, 2]. Trichilemmal cysts tend to be firmer and usually exit more easily through a surgical incision than do epidermoid cysts [1, 2]. Trichilemmal cysts present four to five times less commonly than the epidermoid type [1]. Some theorize that the trichilemmal cyst originates from budding of the external root sheath of hair follicles as a genetically determined aberration [3, 5]. This idea results from the cyst wall's resemblance to the sheath at the level of the follicular isthmus and from an autosomal dominant inheritance pattern that has been observed in some families [3, 5].
Histopathologic examination confirms the diagnosis of a presumed trichilemmal cyst. At the periphery is a fibrous capsule, which surrounds a rim of dark-staining basal cells [3]. More centrally, pale-staining, squamous keratinocytes increase in height until they transform abruptly into solid, eosinophilic-staining keratin [3]. For the most part, the epithelial lining does not form a granular-cell layer [3, 6]. Approximately 25 percent of lesions contain calcification regardless of age, and some may show ossification as well [3, 6].
Rare variants of the trichilemmal cyst should be recognized as a consequence of their prognostic implications. Proliferating trichilemmal cysts arise commonly in women over 60 years of age and can be atypically large, fungating, and ulcerated [3, 7, 8]. They commonly reach large sizes of 2 to 10 cm in diameter but may extend to 25 cm [6, 9]. Trauma and inflammation are among the theories for the transformation of a traditional to a proliferating cyst [10]. The histopathologic features of a proliferating trichilemmal cyst show relatively greater cellular atypia and squamous proliferation [11]. Rarely, malignant proliferating trichilemmal cysts have been described that can result in substantial morbidity and mortality [7]. About 30 well-described cases exist in the English literature [12]. Malignant variants tend to show rapid increase in size beyond 5 cm, development on sites other than the scalp, ulceration, and necrosis [13]. The histopathologic features of this variant include severe cellular atypia and invasion of surrounding tissue; they may demonstrate aneuploidy, loss of CD34 on immunostaining, and loss of wild-type p53 [14, 15, 16].
Trichilemmal cysts may be treated by simple excision if indicated for medical or cosmetic concerns [1, 7]. Complete excision is recommended for all benign proliferating variants owing to their potential for locally aggressive behavior and malignant transformation. Malignant proliferating variants require wide local excision with 1-cm margins or Mohs micrographic surgery [7]. Nodal dissection, radiotherapy, and chemotherapy also are considered in malignant cases [7].
References
1. Stone MS. Cysts. In: Bolognia JL, et al., eds. Dermatology. 2nd ed. London: Mosby, 2008: 16832. James WD, et al, eds. Epidermal nevi, neoplasms, and cysts. In: Andrew's Diseases of the Skin. 10th ed. Philadelphia: Saunders; 2006: 677
3. McKee P.H., et al, eds. Cutaneous cysts. In: Pathology of the Skin with Clinical Correlations. 3rd ed. China: Mosby, 2005: 1670
4. McKee P.H., et al, eds. Tumors of the hair follicle. In: Pathology of the Skin with Clinical Correlations. 3rd ed. China: Mosby, 2005: 1533
5. Leppard BJ, et al. Hereditary trichilemmal cysts: hereditary pilar cysts. Clin Exp Dermatol 1977; 2: 23 PubMed
6. Scott GA. Cutaneous cysts and related lesions. In: Barnhill RL, et al., eds. Textbook of Dermatopathology. 2nd ed. Philadelphia: McGraw-Hill; 2006: 562
7. Satyaprakash AK, et al. Proliferating trichilemmal tumors: a review of the literature. Derm Surg 2007; 33: 1102 PubMed
8. Janitz J, et al. Trichilemmal pilar tumors. Cancer 1980; 45: 1594 PubMed
9. Cysts and sinuses and pits. In: Weedon D, ed. Skin Pathology. 2nd ed. Edinburgh: Churchill Livingstone; 2002: 506
10. Brownstein MH, et al. Proliferating trichilemmal cyst: a simulant of squamous cell carcinoma. Cancer 1981; 48: 1207 PubMed
11. Sau P, et al. Proliferating epithelial cysts: clinicopathological analysis of 96 cases. J Cutan Pathol 1995; 22: 394 PubMed
12. López-Ríos F, et al. Proliferating trichilemmal cyst with focal invasion: report of a case and a review of the literature. Am J Dermatopathol 2000; 22: 183 PubMed
13. Warner TF. Proliferating pilar cyst with spindle cell component. J Cutan Pathol 1979; 6: 310 PubMed
14. Takata M, et al. A trichilemmal carcinoma arising from a proliferating trichilemmal cyst: the loss of the wild-type p53 is a critical event in malignant transformation. Hum Pathol 1998; 29: 193 PubMed
15. Herrero J, et al. Malignant proliferating trichilemmal tumours: an histopathological and immunohistochemical study of three cases with DNA ploidy and morphometric evaluation. Histopathology 1998; 33: 542 PubMed
16. Mehregan AH, et al. Malignant proliferating trichilemmal tumors--report of three cases. J Derm Surg Oncol 1987; 13: 1339 PubMed
© 2008 Dermatology Online Journal

