Rowell syndrome (systemic lupus erythematosus + erythema multiforme)
Published Web Location
https://doi.org/10.5070/D35pf8k3r2Main Content
Rowell syndrome (systemic lupus erythematosus + erythema multiforme)
Arnold Lee MD, Priya Batra, MD PhD, Vika Furer MD, Wang Cheung MD, Nadia Wang MD, Andrew Franks Jr MD
Dermatology Online Journal 15 (8): 1
Department of Dermatology, New York UniversityAbstract
A 61-year-old woman with a history of chilblains and systemic lupus erythematosus (SLE) for 15 years presented with annular, erythematous, scaly papules and plaques on her face, neck, chest, abdomen, back, arms, and legs. A biopsy specimen showed a destructive interface dermatitis with extensive epithelial cell necrosis, which was consistent with lupus erythematosus with combined subacute cutaneous lupus and erythema multiforme-like features. These findings are most compatible with a diagnosis of Rowell syndrome. Rowell syndrome and its relation to lupus erythematosus and erythema multiforme are discussed.
History
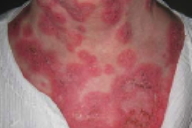 | 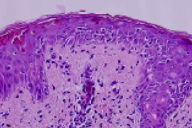 |
| Figure 1 | Figure 2 |
|---|---|
A 61-year-old woman with systemic lupus erythematosus (SLE) for 15 years and a positive history of chilblains initially presented with an arcuate, pruritic eruption that began on her back and became generalized about nine months ago after Pseudomonas and Klebsiella infections. A skin biopsy specimen was obtained from her suprapubic area. The initial eruption resolved with the use of prednisone and then flared intermittently when the medication was changed to dapsone, which was discontinued due to decreases in hemoglobin. Mycophenolate mofetil was then started and led to the resolution of her cutaneous eruption. However, she was unable to tolerate this medication, owing to abdominal pain and diarrhea. Azathioprine and etanercept were subsequently begun, but she reported appreciable worsening of the eruption. She presented to the emergency room with a one-month history of pruritic, annular, scaly lesions that started around her nipples and then spread to her trunk and extremities.
During her hospitalization, methylprednisolone and cyclosporine were begun and resulted in appreciable improvement. However, she developed medication-related hypertension. In view of her excellent response while on mycophenolate mofetil and her severe hypertension, cyclosporine was discontinued, methylprednisolone slowly tapered, and an enteric-coated form of mycophenolic acid was started.
Medical history included hypertension and hypothyroidism. Surgical history included hysterectomy, rotator cuff repair, rib fracture, right ankle fracture, and left foot fracture. Medications include hydroxychloroquine, methylprednisolone, levothyroxine, propranolol, doxepin, esomeprazole, loratadine, alprazolam, etanercept, and pramoxine lotion.
Physical examination
Well-defined, erythematous papules and plaques, mostly annular, some with scales, that coalesced into large, confluent, arcuate lesions were present on the face, neck, chest, abdomen, back, arms, and legs. No oral, genital, or ocular lesions were noted.
Laboratory data
A complete blood cell count with differential analysis was normal except for a white-cell count 3.4 x 109/L. An anti-nuclear antibody titer was >640 with a speckled pattern. Levels of SS-A and SS-B antibodies were elevated, 496eu/ml and 69eu/ml, respectively. C3 level was decreased at 82 mg/dL, and C4 was normal. Antibody to ds-DNA was negative. A comprehensive metabolic panel, rheumatoid factor, erythrocyte sedimentation rate, C-reactive protein, coagulation panel, thyroid stimulating hormone, urinalysis, and chest radiograph were normal.
Histopathology
There is superficial, perivascular, periadnexal, and interstitial infiltrate that is comprised of lymphocytes and a few plasma cells. Lymphocytes extend into a slightly atrophic epidermis, where there is basal vacuolar change, prominent necrotic keratinocytes, and overlying orthokeratosis with parakeratosis.
Diagnosis
Rowell syndrome (systemic lupus erythematosus + erythema multiforme).
Comment
Rowell syndrome (RS) is a rare entity, in which patients with lupus erythematosus (LE) develop lesions of erythema multiforme (EM). Scholtz first described the simultaneous appearance of LE with EM in 1922 [1]. In 1963, Rowell et al. reported four discoid LE (DLE) female patients with EM-like lesions that were associated with a speckled ANA pattern, positive rheumatoid factor, and antibodies to a saline extract of human tissues (anti-SjT) [2]. Because EM patients do not typically show accompanying immunologic characteristics or anti-SjT antibodies, this entity was classified as a distinct disease termed Rowell syndrome, with the following criteria: LE; EM-like lesions; and immunologic serum abnormalities: a speckled ANA pattern and positive rheumatoid factor (RF) [3, 4].
Since then, RS has been described in about 33 patients, most of whom were middle-aged women [2, 3, 5, 6, 7]. Although the initial reports of RS were described in patients with DLE, additional cases with SLE and subacute LE (SCLE) have been reported [3-8].
Several reviews have iterated that these RS case reports did not fulfill all of the original criteria [3, 6, 7]. For instance, a case report of RS by Maciejewski did not have the characteristic histopathologic findings of EM [7, 9]. Fiallo et al. described RS in an 18-year-old male SLE patient with a homogeneous ANA pattern [8]. Two RS cases had negative RF [3, 11]. A more detailed examination of the four patients Rowell et al. described showed erythrocyanosis of the legs and absence of mucosal involvement although it was later stated that recurrent episodes of EM in these patients involved the mucosae on rare occasions [2, 7]. A recent publication by Khandpur et al. detected EM of the lips, eyes, tongue, hard palate, and buccal and vulval mucosae in 47 percent of the cases reviewed. Also, anti-SjT antibody assays are no longer performed.
In view of these controversies, several publications addressed and redefined the criteria for diagnosing RS. In 1995, Lee et al. suggested the inclusion of chilblains as a diagnostic feature [10]. Zeitouni et al. proposed the following diagnostic criteria for RS in 2000: major criteria include SLE, DLE, or SCLE; EM-like lesions (with and/or without mucosal involvement); and an ANA with a speckled pattern. Minor criteria include chilblains, anti-Ro or anti-La antibody, and a positive RF [3]. All three major criteria and at least one minor criterion are required for the diagnosis of RS [3, 4]. A review of 18 case reports of RS between 1963 and 2000 showed that the speckled ANA pattern was the most consistent feature of RS and is described in about 88 percent of the cases, whereas RF is the least preserved feature and is present in only 41 percent [6]. Anti-Ro/La antibodies are detected in 53 percent of the cases [6]. Although chilblains had been described in all four of Rowell's original cases, this feature was found in only five of the 15 cases reported between 1982 and 2008 [6].
A more clinically relevant question and resulting controversy concern whether RS truly merits distinction as a unique clinical entity [7]. The speckled ANA pattern, which correlates with antibodies to various ribonucleoproteins, is not unique to RS; it is also positive in SLE, mixed connective-tissue disease, and scleroderma [6, 7]. Similarly, anti-Ro/La antibodies can be detected in SCLE (70%), Sjögren syndrome (80%), SLE (20-60%), rheumatoid arthritis, and scleroderma; they are strongly associated with photosensitivity and vasculitis in SLE [6, 7, 13]. These two antibodies contribute to the formation of the ANA speckled pattern [14]. Therefore, the concomitant appearance of this pattern with positive anti-Ro or anti-La antibody can be expected. Also, RF positivity can occur in DLE (17%), SLE (40%), scleroderma (40%), SCLE, and Sjögren syndrome [6]. Rowell and Beck documented that ANAs were more common in patients with LE and chilblains and these patients were also more likely to have RF [7, 12]. In view of the lack of specific features that distinguish RS from LE, Kuhn et al. suggested that Rowell syndrome is probably not a distinct entity and is now widely considered to be a variant of SCLE [15].
The therapeutic regimen, responses, and prognosis in RS are similar to those of SLE or DLE that occur alone [6]. Most of the reported cases showed good responses to mid-to-high doses of prednisone with azathioprine or antimalarials, such as chloroquine or hydroxychloroquine [4, 5, 6]. Zeitouni et al. described a case that was successfully treated with dapsone [3]. Because the occurrence of EM with LE did not alter the course, therapy, or prognosis of either disease and because this coexistence does not impart any unusual characteristics, Shteyngarts et al. made the argument that RS is not unique and that the serologic findings in these patients are probably coincidental [7].
References
1. Scholtz M. Lupus erythematosus acutus disseminatus haemorrhagicus. Arch Dermatol Syphilol 1922; 6: 4662. Rowell NR, et al. Lupus erythematosus and erythema multiforme-like lesions. Arch Dermatol 1963; 88: 176 [PubMed]
3. Zeitouni NC, et al. Redefining Rowell's syndrome. Br J Dermatol 2000; 142: 343 [PubMed]
4. Shadid NH, et al. Lupus erythematosus associated with erythema multiforme: Rowell's syndrome. Int J Dermatol 2007; 46: 30 [PubMed]
5. Duarte AF, et al. Rowell syndrome – case report and review of literature. Dermatol Online J 2008; 14 (3): 15 [PubMed]
6. Khandpur S, et al. Rowell's syndrome revisited: report of two cases from India. Int J Dermatol 2005; 44: 545 [PubMed]
7. Shteyngarts AR, et al. Lupus erythematosus associated with erythema multiforme: does Rowell's syndrome exist? J Am Acad Dermatol 1999; 40: 773 [PubMed]
8. Fiallo P, et al. Rowell's syndrome. Int J Dermatol 1995; 34: 635 [PubMed]
9. Maciejewski W. Annular erythema as an unusual manifestation of chronic disseminated lupus erythematosus. Arch Dermatol 1980; 116: 450 [PubMed]
10. Lee S, et al. Rowell's syndrome: a case report with subacute cutaneous lupus erythematosus and erythema multiforme. Can J Dermatol 1995; 7: 807
11. Parodi A, et al. Rowell's syndrome: report of a case. J Am Acad Dermatol 1989; 21: 374 [PubMed]
12. Rowell NR, Beck JS. The diagnostic value of an antinuclear antibody test in clinical dermatology. Arch Dermatol 1967; 96: 290 [PubMed]
13. Provost TT, et al. Significance of the anti-Ro (SS-A) antibody in evaluation of patients with cutaneous manifestations of connective tissue disease. J Am Acad Dermatol 1996; 35: 147 [PubMed]
14. Maddison PJ, Reichlin M. Quantitation of precipitating antibodies to certain soluble nuclear antigens in SLE. Arthritis Rheum 1977; 20: 819 [PubMed]
15. Kuhn A, et al. Clinical manifestations of cutaneous lupus erythematosus. J Dtsch Dermatol Ges. 2008; 6: 48 [PubMed]
© 2009 Dermatology Online Journal

