Hidradenitis should not be renamed acne inversa
Published Web Location
https://doi.org/10.5070/D35g21t4mqMain Content
Hidradenitis should not be renamed acne inversa
Noah Scheinfeld
Dermatology Online Journal 12 (7): 6
Department of Dermatology St Lukes Roosevelt Hospital Center
There has been a trend in recent years to rename hidradenitis suppurativa (HS) with the proposed term acne inversa, which is more histologically correct. In an article that appeared in the International Journal of Dermatology about 2 years ago, Sellheyer and Krahl [1] stated the following:
When the histopathology, clinical presentation and some of the therapeutic aspects of "hidradenitis suppurativa" are those of acne (modified under the special circumstances of anatomical regions rich in apocrine glands), why not call it as such and abandon the misnomer? It is acne inversa because, in contrast to acne vulgaris, the disease involves ectopic (intertriginous) localizations and not the regions classically affected by acne vulgaris. In conclusion, the term "hidradenitis suppurativa" should be abandoned. "Hidradenitis suppurativa" is acne inversa!
Nevertheless, although the observations concerning histology are helpful, a reconsideration of acne's relationship to other conditions along with recent genetic data suggests that despite some common features, HS and acne vulgaris (AV) are distinct.
It is clear that HS is a misnomer because it does not involve the apocrine sweat gland. However, the term HS is describing a distinct condition and this would be the basis for leaving the names of the diseases as they are.
|
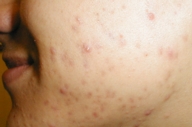
| Figure 1 |
|---|
| Mild facial acne |
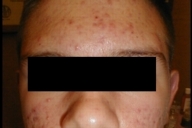
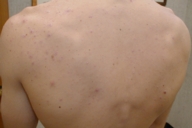
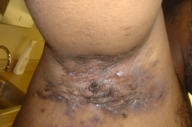
Clinically, acne and HS present in different locations. Mild acne (Fig. 1) and nodulocystic Acne (Figs. 2 and 3) involve the face, chest and back; HS involves the intertriginous areas of the body (Fig. 4). Although location alone cannot be used to distinguish conditions, the skin in different locations has different qualities (thickness, sweat gland density) that result in very different cutaneous disease manifestations.
|
|
| Figure 2 | Figure 3 |
|---|---|
| Nodulocystic acne of the face and back | |
It is true that all the diseases of the follicular occlusion tetrad have primary follicular involvement in common. However, acne vulgaris is distinct in many ways from HS (Table 1). Hidradenitis has many systemic associations that AV does not. The strongest piece of data that acne vulgaris and HS are distinct is a recent report of Gao [2] that identifies the basis of HS in a Chinese kindred as a genetic mutation at chromosome 1p21.1-1q25.3; no such genetic link for AV has yet been defined. Interestingly, the proband of this kindred, whose pictures were contained in the article, had nodules of hidradenitis around his ears and on his neck but his cheek appeared almost acne free.
|
| Figure 4 |
|---|
| Hidradenitis suppurativa of the axilla |
In conclusion, histology alone does not define dermatology. Acne has a constellation of causes and presentations that HS does not share (see Table 2). Hidradenitis suppurativa has more in common with acne fulminans than it does with acne vulgaris, but HS has different associations and may have a distinct genetic basis that neither AV nor AF share. More information must be obtained about the genetic basis of all of these disease states before proposing changes in nomenclature that could cause significant confusion with the redefinition of a large niche in the schema of dermatology. Because HS has many unique aspects, its current name, although a misnomer, should remain unchanged.
References
1. Sellheyer K, Krahl D. "Hidradenitis suppurativa" is acne inversa! An appeal to (finally) abandon a misnomer. Int J Dermatol. 2005;44:535-40.2. Gao M, Wang PG, Cui Y, Yang S, Zhang YH, Lin D, Zhang KY, Liang YH, Sun LD, Yan KL, Xiao FL, Huang W, Zhang XJ. Inversa acne (hidradenitis suppurativa): a case report and identification of the locus at chromosome 1p21.1-1q25.3. J Invest Dermatol. 2006;126:1302-6.
3. Bhalla R, Sequeira W. Arthritis associated with hidradenitis suppurativa. Ann Rheum Dis. 1994;53:64-6.
4. Jansen I, Altmeyer P, Piewig G. Acne inversa (alias hidradenitis suppurativa). J Eur Acad Dermatol Venereol. 2001 ;15: 532-40.
5. Shah N. Hidradenitis suppurativa: a treatment challenge. Am Fam Physician. 2005; 72: 1547-52.
6. Barth JH, Layton AM, Cunliffe WJ. Endocrine factors in pre- and postmenopausal women with hidradenitis suppurativa. Br J Dermatol. 1996; 134: 1057-9.
7. Kunynetz RA. A review of systemic retinoid therapy for acne and related conditions. Skin Therapy Lett. 2004; 9: 1-4.
8. Iqbal M, Kolodney MS. Acne fulminans with synovitis-acne-pustulosis-hyperostosis-osteitis (SAPHO) syndrome treated with infliximab. J Am Acad Dermatol. 2005; 52(5 Suppl 1): S118-20.
9. Bergfeld WF. The pathophysiology of acne vulgaris in children and adolescents, Part 1. Cutis. 2004;74:92-7.
10. Burkhart CN, Gottwald L. Assessment of etiologic agents in acne pathogenesis. Skinmed. 2003; 2: 222-8.
© 2006 Dermatology Online Journal

