Granuloma faciale of the scalp
Published Web Location
https://doi.org/10.5070/D35f93j33tMain Content
Granuloma faciale of the scalp
Inês Leite MD, Ana Moreira MD, Rita Guedes MD, Antónia Furtado MD, Eduarda Osório Ferreira MD, Armando Baptista MD
Dermatology Online Journal 17 (4): 6
Centro Hospitalar Vila Nova de GaiaAbstract
Granuloma faciale (GF) is an uncommon dermatosis with characteristic clinicopathological features. Extrafacial isolated GF is extremely rare. Pulsed dye laser (PDL) is a treatment option for GF to minimize the risk of scarring. We report a case of a 78-year-old male with an extensive GF of the scalp successfully treated with pulsed dye laser (PDL).
Introduction
Granuloma faciale (GF) is an uncommon benign dermatosis of unknown pathogenesis characterized by red, brown or violaceous papules, plaques or nodules that predominantly affects middle-aged men [1]. Lesions tend to follow a chronic course. We report a case of extensive GF of the scalp.
Case report
 |  |
| Figure 1a | Figure 1b |
|---|---|
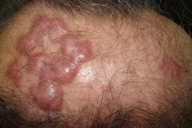
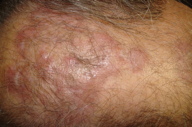
| Figure 1. Granuloma faciale of the scalp (1a) before and (1b) after treatment. | |
We describe the case of a 78-year-old asymptomatic male with a 3 month history of smooth erythematous to violaceus confluent tumors on the scalp covered by telangiectasias (Figure 1a). The patient did not report a history of similar lesions on the skin. Clinical diagnosis of cutaneous B-cell lymphoma, cutaneous metastases, GF, and sarcoidosis were considered.
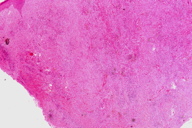 | 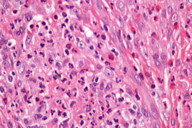 |
| Figure 2c | Figure 2d |
|---|
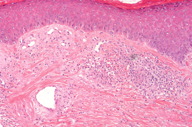
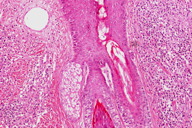
A cutaneous biopsy was performed and revealed an epidermis with no significant alterations that was separated from the underlying inflammatory infiltrate and telangiectatic vessels by a narrow and periadnexal Grenz zone (Figures 2a and 2b). There was a dense and diffuse infiltrate of lymphocytes, plasma cells, eosinophils and neutrophils involving the deep dermis (Figure 2c). Examination of the dermal infiltrate under a higher magnification revealed a polymorphous infiltrate consisting primarily of neutrophils, eosinophils, and plasma cells (Figure 2d). Dilated vessels were seen in the dermis with prominent endothelial cells and neutrophils in the vessel walls.
Routine and immunological serum analysis, urinalysis, angiotensin converting enzyme test, VDRL, and TPHA were normal. The chest x-ray was also normal. Polymerase chain reaction (PCR) for Mycobacterium tuberculosis on the cutaneous biopsy was negative.
Based on the clinical and histopathological findings, GF was diagnosed.
The patient was treated with intralesional corticosteroids (3 sessions) with some improvement followed by pulsed dye laser (PDL – 5 treatments). A wavelength emission of 585 nm and a pulse duration of 20 ms were used. Treatments were performed at 5.8 - 8.3 J/cm² with a cooling device. After these treatments there was a marked improvement (Figure 1b) and during a follow-up period of 6 months no recurrence was observed.
Discussion
Extrafacial GF has been reported but is rare and it usually coexists with facial lesions [1]. Extrafacial isolated involvement is extremely rare [2, 3, 4]. An extensive extrafacial granuloma faciale of the scalp has been reported [4].
Ortonne et al [1] studied 66 patients with GF (61 of these patients had only facial lesions) and suggested that it follows a chronic course with recurrent acute phases and that the most frequent histopathological features were the presence of a grenz zone, neutrophils, and telangiectasias. Vasculitis is not essential for histopathological diagnosis [1, 2].
GF is frequently resistant to therapy and there is no standard therapy for this dermatosis [5]. Topical tacrolimus [5], topical and intralesional corticosteroids [2], dapsone [2, 6], cryosurgery [7], surgical excision [6], pulsed dye laser (PDL) [8, 9] and other treatment modalities have been used with variable results. The patient’s extensive lesions required a treatment that minimizes the risk of scarring.
With this case we intend to emphasize that GF is often clinically misdiagnosed and that this dermatosis should be kept in mind in the differential diagnosis of plaques and tumors, namely on the face and scalp. There is no standard therapy for this disease and there is a high risk of scarring and relapse after its management. This case report also emphasizes the efficacy and safety of PDL in the treatment of this condition.
References
1. Ortonne N, Wechsler J, Bagot M, Grosshans E, Cribier B. Granuloma faciale: a clinicopathologic study of 66 patients. Dermatopathology. 2005 Dec;53(6):1002-1009. [PubMed]2. De D, Kanwar AJ, Radotra BD, Gupta S. Extrafacial granuloma faciale: report of a case. J Eur Acad Dermatol Venereol. 2007 Oct;21(9):1253-1302. [PubMed]
3. Castaño E, Segurado A, Iglesias L, López-Ríos F, Rodriguez-Peralto JJ. Granuloma faciale entirely in an extrafacial location. Br J Dermatol. 1997 Jun;136(6):978-979. [PubMed]
4. Kavanagh GM, McLaren KM, Hunter JA. Extensive extrafacial granuloma faciale of the scalp. Br J Dermatol. 1996 Mar;134(3):595-596. [PubMed]
5. Thiyanaratnam J, Doherty SD, Krishnan B, Hsu S. Granuloma faciale: case report and review. Dermatol Online Journal. 2009 Dec;15(15):3. [PubMed]
6. Requena C, Castejón P, Sanmartín O, Bortella-Estrada R, Nagore E, Serra-Guillén C, Sorní G, Guillén C. Rinophyma-like granuloma faciale. J Eur Acad Dermatol Venereol. 2006 Aug;20(7):868-902. [PubMed]
7. Panagiotopoulos A, Anyfantakis V, Rallis E, Chasapi V, Stavropoulos P, Boubouka C, Katsambas A. Assessment of the efficacy of cryosurgery in the treatment of granuloma faciale. Br J Dermatol. 2006 Apr;154(4): 357-360. [PubMed]
8. Ammirati CT, Hruza GJ. Treatment of granuloma faciale with the 585-nm Pulsed Dye Laser. Arch Dermatol. 1999 Aug;135(8):903--905. [PubMed]
9. Elston DM. Treatment of granuloma faciale with the pulsed dye laser. Cutis. 2000 Feb;65(2):97-81. [PubMed]
© 2011 Dermatology Online Journal