Aquagenic wrinkling of the palms: A case report and literature review
Published Web Location
https://doi.org/10.5070/D35d57w5zzMain Content
Aquagenic wrinkling of the palms: A case report and literature review
Zain Syed MD1, Molly Wanner MD2, Omar A Ibrahimi MD PhD3
Dermatology Online Journal 16 (7): 7
1. University of Virginia, Charlottesville, Virginia2. Department of Dermatology, Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts
3. Harvard Combined Program in Dermatology, Massachusetts General Hospital, Boston, Massachusetts. omar.ibrahimi@gmail.com
Abstract
Aquagenic wrinkling of the palms (AWP) is a condition that results in pain and edema of the hands after exposure to water. We describe a 32-year-old woman who presented with a several-year history of AWP. She was unable to tolerate a 20 percent aluminum chloride solution because of irritation, but a gel formulation of 15 percent aluminum chloride controlled her symptoms without side effects.
Case report
A 32-year-old woman with fibromyalgia and rheumatoid arthritis presented to our outpatient clinic for evaluation of a palmar eruption. She noted a several-year history of adverse reactions to water that involved only the palms and not the soles. The reaction initially started with swelling and tenderness, but after a few minutes, she would develop “blisters” and “holes” in her skin. When she washed dishes with warm water, the patient reported that the lesions became more noticeable and symptomatic. The abnormalities and pain resolved within thirty to ninety minutes after drying her hands. She denied any concomitant hyperhidrosis. She had no family history of similar problems and she denied any personal or family history of cystic fibrosis. Her medications included acetaminophen/hydrocodone, levongesterol, modafinil, and topiramate.
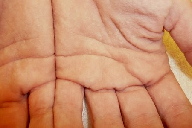 | 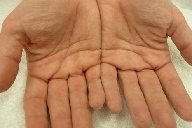 |
| Figure 1a | Figure 1b |
|---|---|
| Figures 1a and 1b. Appearance of “pebbly” palms following immersion in water for 5 minutes. | |
Her palms were unremarkable on physical exam. Following immersion of hands in water for five minutes, she developed skin-colored, pebble-like papules with prominent eccrine ostia (Figures 1a and 1b), consistent with a positive “hand in bucket sign.”
The patient was given 20 percent aluminum chloride solution that helped prevent development of her palmar lesions. However, she had to discontinue its use secondary to skin irritation and pain. Upon switching to 15 percent aluminum chloride in a gel vehicle, she noted better control of symptoms without any irritation.
Discussion
Of historical interest, patients with a strikingly similar condition, hereditary papulotranslucent acrokeratoderma, were first reported by Onwukwe et al. in 1973 [1]. The report described “persistent, asymptomatic, yellowish-white, translucent papules and plaques that appear on the hands and feet,” and the changes were “associated with fine-textured scalp hair and an atopic diathesis.” The onset of lesions in the reported kindred was noted to occur around puberty and transmission was suggested to be autosomal dominant. The keratoderma was noted to be exacerbated by water immersion initially, but later ceased to be sensitive to water immersion. Histologic analysis of the papules showed orthohypergranulosis, acanthosis, and a relatively normal dermis [1].
Subsequently, several reports appeared in the literature describing a morphologically similar, yet distinct condition known by several names, including: aquagenic wrinkling of the palms (AWP), acquired aquagenic palmoplantar keratoderma [2], transient reactive papulotranslucent acrokeratoderma [3] or aquagenic syringeal acrokeratoderma [4]. These patients, mostly female, were noted to rapidly develop white to translucent papules on their palms following immersion in water (“hand in bucket sign”) [5]. This condition was also found to be associated with pain and edema. Symptoms were noted to resolve with drying of the skin. Moreover, plantar involvement was not commonly observed. An autosomal recessive mode of inheritance was proposed [3]. Histological studies showed dilated eccrine ostia and a hyperkeratotic stratum corneum [3, 4].
The majority of reported cases of AWP have associated cystic fibrosis (CF). Cystic fibrosis is caused by mutations in the CFTR gene. In 2005, Katz and colleagues reported 2 such patients who exhibited homozygosity for the ΔF508 CFTR mutation, suggesting that this particular mutation may be a predisposing factor for AWP [6]. It has been proposed that AWP is caused by an increase in the water-binding capacity of keratins mediated by high salt concentrations in the epidermis as seen in CF patients. An alternative proposed pathogenic mechanism in CF patients is the abnormal regulation of cell-membrane water channels, such as aquaporin 3, by CFTR. Other pathogenic theories for AWP include defective stratum corneum barrier function, occlusion of the eccrine duct ostia, or weakness of the eccrine duct wall [6].
Drug-induced cases of aquagenic wrinkling of the palms have been reported in single case reports associated with aspirin [7] and rofecoxib [8]. The proposed mechanisms for both these cases involve an increase in the sodium retention of epidermal cells. In both cases, the proposed mechanism is COX-2 inhibition in epidermal cells, which may cause increased sodium reabsorption in a mechanism similar to the effect of COX-2 inhibitors on kidney cells [7].
Most treatment regimens for AWP focus on decreasing the hyperkeratosis associated with the condition, or with providing a water barrier to prevent exposure. Treatments involving the application of 12 percent ammonium lactate creams or petroleum jelly or the use of gloves have not been shown to be effective [4, 9]. Using 20 percent aluminum chloride solution has been reported to result in a rapid improvement of symptoms in a series of three patients [2]. Our patient was unable to tolerate the solution because of its irritating properties. However, the use of 15 percent aluminum chloride in a gel vehicle managed to control our patient’s symptoms without the overly drying and irritating effects of the alcohol solution. The use of aluminum chloride in a more tolerable gel vehicle may be of benefit in other patients with AWP who are unable to tolerate the solution form.
References
1. Onwukwe MF, Mihm MC, Toda K. Hereditary papulotranslucent acrokeratoderma: a new variant of familial punctate keratoderma? Arch Dermatol. 1973;108:108-110. [PubMed]2. Yan AC, Aasi SZ, Alms WJ, James WD, Heymann WR, Paller AS, Honig PJ. Aquagenic palmoplantar keratoderma. J Am Acad Dermatol. 2001;44:696-9. [PubMed]
3. English JC 3rd, McCollough ML. Transient reactive papulotranslucent acrokeratoderma. J Am Acad Dermatol. 1996;34:686-7. [PubMed]
4. MacCormack MA, Wiss K, Malhotra R. Aquagenic syringeal acrokeratoderma: report of two teenage cases. J Am Acad Dermatol. 2001;45:124-6. [PubMed]
5. Rizzo C, Bragg J, Soldano AC, Cohen D, Soter NA. Hereditary papulotranslucent acrokeratoderma. Dermatol Online J. 2008;15:14:3. [PubMed]
6. Katz KA, Yan AC, Turner ML. Aquagenic wrinkling of the palms in patients with cystic fibrosis homozygous for the delta F508 CFTR mutation. Arch Dermatol. 2005;141:621-4. [PubMed]
7. Khuu PT, Duncan KO, Kwan A, Hoyme HE, Bruckner AL. Unilateral aquagenic wrinkling of the palms associated with aspirin intake. Arch Dermatol. 2006;142:1661-2. [PubMed]
8. Carder KR, Weston WL. Rofecoxib-induced instant aquagenic wrinkling of the palms. Pediatr Dermatol. 2002;19:353-5. [PubMed]
9. Itin PH, Lautenschlager S. Aquagenic syringeal acrokeratoderma (transient reactive papulotranslucent acrokeratoderma). Dermatology 2002;204:8-11. [PubMed]
© 2010 Dermatology Online Journal

