Results of a randomized, open-label, crossover study of the bioequivalence of subcutaneous versus intramuscular administration of alefacept
Published Web Location
https://doi.org/10.5070/D35b52c9r0Main Content
Results of a randomized, open-label, crossover study of the bioequivalence of subcutaneous versus intramuscular administration
of alefacept
Marianne T Sweetser MD PhD1, James Woodworth PhD1, Suzanne Swan MD2, Barry Ticho MD PhD1
Dermatology Online Journal 12 (3): 1
1. Biogen Idec, Inc., Cambridge, MA. marianne.sweetser@biogenidec.com2. DaVita Clinical Research, Hennepin County Medical Center, Minneapolis, MN
Abstract
Alefacept selectively reduces memory T cells and inhibits T-cell activation. Large randomized trials have shown that intramuscular (IM) delivery of alefacept is safe and effective in treating plaque psoriasis. Subcutaneous (SC) administration of alefacept may provide advantages for some patients including convenience, ease of use, and reduced pain on injection. We conducted a randomized, open-label, crossover study in 50 healthy volunteers to determine if alefacept 15 mg administered SC is bioequivalent to alefacept 15 mg administered IM. The pharmacokinetic parameters used to determine bioequivalence were area under the serum concentration-time curve to the last measurable value (AUClast; primary endpoint), peak serum concentration (Cmax), and AUC to infinity (AUC∞). For each of these parameters, the 90 percent confidence intervals for the least squares mean ratios of alefacept SC to alefacept IM were well within the conventional bioequivalence range of 80 percent to 125 percent. These data, together with the finding that the mean serum concentration-time curves for alefacept were nearly identical following both routes of administration, demonstrate the bioequivalence of alefacept SC and alefacept IM. No clinically important differences between the pharmacodynamic profiles (total lymphocyte and lymphocyte subset counts) of the two routes of administration were observed. Alefacept SC and alefacept IM were similarly well tolerated. Our results suggest that SC dosing may represent a viable delivery option for alefacept.
Introduction
Chronic plaque psoriasis is a dermatologic inflammatory disease characterized by infiltration of memory (CD45RO+) T cells into psoriatic lesions [1]. Alefacept, a fully human LFA-3/IgG1 fusion protein, selectively reduces memory T cells and inhibits T-cell activation. Alefacept has been proven safe and effective, with a prolonged duration of off-treatment response, in the treatment of chronic plaque psoriasis [2, 3, 4, 5]. For patients who initially achieved a ≥75 percent reduction in Psoriasis Area and Severity Index (PASI 75), a single course of alefacept maintained clinical improvement (≥50% reduction from baseline PASI [PASI 50]) for a median off-treatment duration of approximately 7 months, without the need for further therapy [3, 5].
The recommended alefacept treatment course is 15 mg once weekly for 12 weeks by intramuscular (IM) injection, administered by a health care professional. Because patient choice and convenience are important factors in determining patient satisfaction with a medication [6], administration of alefacept via subcutaneous (SC) injection may be a desirable alternative treatment option for some patients. Direct benefits of SC administration may include convenience, ease of use, and decreased pain upon injection [7].
This report presents the results of a randomized, open-label, crossover study designed to determine if alefacept 15 mg delivered SC is bioequivalent to alefacept 15 mg delivered IM. Secondary objectives were to compare the pharmacodynamic effect of alefacept SC and alefacept IM on peripheral blood lymphocyte and lymphocyte subset counts and to determine the tolerability of alefacept SC.
Materials and methods
The study was conducted in accordance with the ethical principles outlined in the Declaration of Helsinki, Good Clinical Practice (GCP) guidelines, and local regulations. Subjects gave written informed consent before participating in the study.
Subjects
Healthy subjects between 18 and 60 years of age inclusive and within 25 percent of their ideal body weight were eligible to enroll in the study. Key exclusion criteria included an abnormal CD4+ T-cell count; positive laboratory results for hepatitis C antibody, hepatitis B surface antigen, or human immunodeficiency virus at screening; history of serious local or systemic infection within 3 months of study drug administration; symptomatic viral or bacterial infection within 1 week of study drug administration; and fever within 48 hours of study drug administration. Treatment with the following was prohibited: any immunosuppressant agent within 1 year; any antibody, systemic steroid, or steroid inhaler within 6 months; and any investigational drug or approved therapy for investigational use within 3 months of study drug administration.
Study design
This was a randomized, open-label, 2-period crossover bioequivalence study conducted at a single site in Minneapolis, Minnesota, USA. All subjects received one dose of alefacept 15 mg SC and one dose of alefacept 15 mg IM. Subjects were randomized to 1 of 2 treatment sequences, stratified by gender: alefacept SC followed by alefacept IM or alefacept IM followed by alefacept SC. There was an 8-week washout period between the two doses.
Outcome measures
Blood samples for pharmacokinetic assessments were collected within 24 hours before each dose; at 1, 2, 4, 6, 9, 12, 24, 36, and 48 hours after each dose; and 3, 5, 6, 8, 15, 22, and 29 days after each dose. The primary pharmacokinetic parameter used to determine bioequivalence was the area under the serum concentration-time curve to the last measurable value (AUClast). Secondary pharmacokinetic parameters included peak serum concentration (Cmax) and AUC to infinity (AUC∞). All pharmacokinetic calculations were performed using noncompartmental methods. Calculations were performed using the computer program, WinNonlin® version 4.1 (Pharsight Corp., Mountain View, California, USA).
Pharmacodynamic assessments included total lymphocyte and lymphocyte subset (CD4+ and CD8+) counts at screening; within 24 hours before the initial dose; at 24 and 48 hours after each dose; 8 and 29 days after each dose; and for the second period, re-screening occurred 7 weeks and 3 days after the initial dose.
Tolerability was determined by adverse event (AE) monitoring, blood chemistry and hematology analyses, physical examinations, and vital signs.
Statistical analyses
The analysis of AUClast in prior IM bioequivalence studies demonstrated a standard deviation of 0.18 for the logged values. Assuming that a similar standard deviation was observed in this study, a sample size of 36 subjects (18 per sequence) would be sufficient to provide 95 percent power to obtain a 90 percent confidence interval (CI) for the geometric mean ratio that falls completely within the bioequivalence limits of 80 percent to 125 percent. Assuming an 18 percent dropout and missing information rate, a total sample size of 44 subjects was selected as the target enrollment to provide 36 evaluable subjects.
All subjects who received alefacept SC and alefacept IM were included in the bioequivalence analysis. The two one-sided hypotheses at the α = 0.05 level were tested by constructing the 90% CI for the geometric mean ratio of alefacept SC to alefacept IM for AUClast, Cmax, and AUC∞. The standard 80 percent to 125 percent bioequivalence criterion for log-transformed data was used. The data were transformed using natural logarithms. The log-transformed data were analyzed using an analysis of variance (ANOVA) model with factors for sequence, subjects within sequence, and route of administration. The CIs were constructed by the classical (shortest) CI approach, which is equivalent to Schuirmann's two one-sided tests procedure for bioequivalence [8].
All subjects who were randomized, received at least one dose of study drug, and had at least one assessment of a pharmacodynamic parameter were included in the pharmacodynamic analysis. All subjects who were randomized, received at least one dose of study drug, and had at least one postbaseline assessment of the safety parameter being analyzed were included in the safety analysis.
Results
Subjects
Fifty healthy subjects were enrolled in the study; 24 subjects were randomized to receive alefacept SC followed by alefacept IM and 26 subjects were randomized to receive alefacept IM followed by alefacept SC. A total of 42 subjects (84%) received both alefacept SC and alefacept IM and completed evaluations up to day 29 after each dose. Six subjects received only alefacept SC, and two subjects received only alefacept IM. Reasons for discontinuation in these eight subjects included voluntary withdrawal (n = 5), exposure of study drug to extreme temperatures (n = 2), and difficulties secondary to venipuncture (n = 1).
Demographics were balanced between the two treatment sequences (see Table 1). There were 29 male subjects (58%) and 21 female subjects (42%). The mean age of all subjects was 24.3 years, and mean weight was 73.9 kg. Forty-two subjects (84%) were white.
Pharmacokinetics
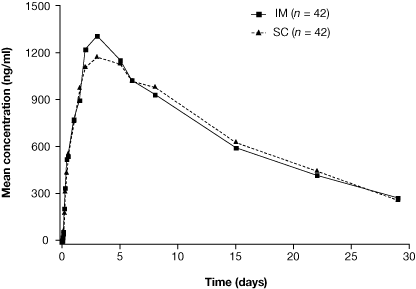 |
| Figure 1. Mean serum concentration (adjusted for baseline) of alefacept after intramuscular (IM) or subcutaneous (SC) administration over time. |
The mean serum concentration-time curves of alefacept were nearly identical following both SC and IM administration (Fig. 1). All pharmacokinetic parameters measured were similar after SC and IM dosing (see Table 2), although time to peak serum concentration (Tmax) was slightly delayed with SC. The 90 percent CIs for the least squares mean ratios of alefacept SC to alefacept IM for AUClast, Cmax, and AUC∞ were completely within the range of 80 percent to 125 percent (see Table 3). These data, together with the similar shape and trend of the mean serum concentration-time curves for both delivery routes, demonstrate that SC and IM administration of alefacept are bioequivalent. There did not appear to be a marked gender effect for any of the pharmacokinetic parameters (data not shown).
Pharmacodynamics
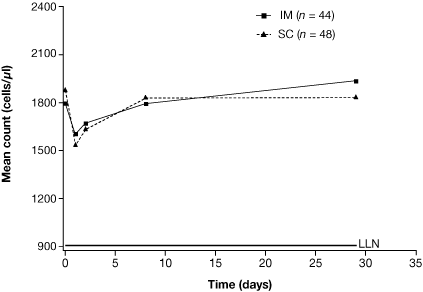 |
| Figure 2. Mean total lymphocyte count after intramuscular (IM) or subcutaneous (SC) administration of alefacept over time. LLN = lower limit of normal. |
A similar pattern of reversible reduction in mean total lymphocyte counts occurred following both SC and IM administration of alefacept, reaching a nadir at 24 hours after dosing and increasing to baseline values by day 8 (Fig. 2). Mean CD4+ and CD8+ T-cell counts followed a similar pattern of reduction and recovery for both delivery routes, consistent with the changes observed in total lymphocyte counts. At no time point measured did the mean total lymphocyte count, CD4+ T-cell count, or CD8+ T-cell count for either route of administration approach the lower limit of normal (910 cells/μl, 404 cells/μl, and 220 cells/μl, respectively).
Tolerability
Alefacept was similarly well tolerated when administered SC or IM. A total of 42 subjects (84%) reported one or more AEs (30 following alefacept SC; 33 following alefacept IM). The most common AEs were headache, upper respiratory tract infection, and pharyngolaryngeal pain (see Table 4). All AEs were mild or moderate in severity, with the exception of one serious unrelated event (herniated disk requiring surgery). Only one subject experienced an injection site reaction (mild pain) following dosing with alefacept SC. No injection site reactions were reported after dosing with alefacept IM. There were no withdrawals from the study or discontinuations of study drug because of AEs. No clinically important trends were observed in clinical laboratory evaluations, physical examinations, or vital signs.
Conclusions
Pharmacokinetic data in this study demonstrate that alefacept 15 mg delivered SC is bioequivalent to alefacept 15 mg delivered IM. This conclusion is supported by the AUClast, Cmax, and AUC∞ results. The 90 percent CIs for all three parameter ratios were well within the 80 percent to 125 percent limits. Moreover, the mean serum concentration-time curves of alefacept were comparable for both delivery methods. The transient pharmacodynamic effects of alefacept on total lymphocyte and lymphocyte subsets were similar for both routes of administration. Single therapeutic doses of alefacept were well tolerated in this study, with no apparent differences between SC and IM dosing.
Drug delivery via the SC route may offer benefits for patients, as the SC injection of alefacept may be less painful for some patients than IM administration. Switching from IM to SC injection is one approach recommended to reduce injection site pain [7]. For example, SC administered Haemophilus influenza type b vaccine was found to be less painful (p < 0.01) and to result in less tenderness at the injection site (p = 0.06) than IM injection in a large randomized study of 498 pediatric patients [9]. There were no observed differences between alefacept SC and alefacept IM in the incidence of injection site pain or other injection site reactions in this study. In addition to a potential reduction in injection site pain, SC administration may afford patients who wish to self-administer alefacept more convenience than IM administration.
In conclusion, SC and IM administration of alefacept 15 mg are bioequivalent, which may provide an additional delivery option for health care professionals and patients.
Acknowledgment: Writing and editorial assistance was provided by Thomson Scientific Connexions.
References
1. Prinz JC. The role of T cells in psoriasis. J Eur Acad Dermatol Venereol. 2003 May;17(3):257-70. PubMed2. Ellis CN, Krueger GG, for the Alefacept Clinical Study Group. Treatment of chronic plaque psoriasis by selective targeting of memory effector T lymphocytes. N Engl J Med. 2001 Jul 26;345(4):248-55. PubMed
3. Krueger GG, Papp KA, Stough DB, Loven KH, Gulliver WP, Ellis CN, for the Alefacept Clinical Study Group. A randomized, double-blind, placebo-controlled phase III study evaluating efficacy and tolerability of 2 courses of alefacept in patients with chronic plaque psoriasis. J Am Acad Dermatol. 2002 Dec;47(6):821-33. PubMed
4. Lebwohl M, Christophers E, Langley R, Ortonne JP, Roberts J, Griffiths CE, for the Alefacept Clinical Study Group. An international, randomized, double-blind, placebo-controlled phase 3 trial of intramuscular alefacept in patients with chronic plaque psoriasis. Arch Dermatol. 2003 Jun;139(6):719-27. PubMed
5. Gordon KB, Langley RG. Remittive effects of intramuscular alefacept in psoriasis. J Drugs Dermatol. 2003 Dec;2(6):624-8. PubMed
6. Shikiar R, Rentz AM. Satisfaction with medication: an overview of conceptual, methodologic, and regulatory issues. Value Health. 2004 Mar-Apr;7(2):204-15. PubMed
7. Brazeau GA, Cooper B, Svetic KA, Smith CL, Gupta P. Current perspectives on pain upon injection of drugs. J Pharm Sci. 1998 Jun;87(6):667-77. PubMed
8. Chow SC, Liu JP. On assessment of bioequivalence under a higher-order crossover design. J Biopharm Stat. 1992;2(2):239-56. PubMed
9. Leung AK, Chiu AS, Siu TO. Subcutaneous versus intramuscular administration of Haemophilus influenzae type b vaccine. J R Soc Health. 1989 Apr;109(2):71-3. PubMed
© 2006 Dermatology Online Journal

