Cutaneous piloleiomyomata
Published Web Location
https://doi.org/10.5070/D359n73024Main Content
Cutaneous piloleiomyomata
Gideon Smith MD PhD, Noushin Heidary MD, Rishi Patel MD, Karla Rosenman MD, Shane A Meehan MD, Hideko Kamino MD, Miguel Sanchez
MD
Dermatology Online Journal 15 (8): 10
Department of Dermatology, New York UniversityAbstract
A 49-year-old man presented with an eight-month history of intermittently painful, subcutaneous nodules that were increasing in size, number, and pain intensity. A biopsy specimen showed smooth muscle proliferation, which also stained positive for actin, and was consistent with piloleiomyoma. The patient was placed initially on gabapentin and then nifedipine with very limited success in pain control. The lesions continued to proliferate, and the patient was referred to surgery for excision.
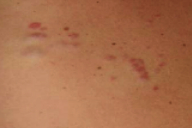 | 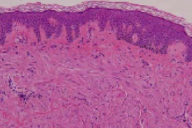 |
| Figure 1 | Figure 2 |
|---|---|
History
A 49-year-old man presented to the Dermatology Clinic at Bellevue Hospital Center with an eight-month history of intermittently, intensely painful subcutaneous nodules. The lesions began as one or two barely palpable papules on the left upper back and enlarged and increased in number on the left upper back and developed as fifteen smaller, firm, exophytic papules along the skin tension lines on the right lower back. The patient reported progressive sharp, pinching or stabbing pain that initially lasted several seconds but subsequently persisted from ten minutes to four hours. The frequency of painful episodes increased from every few days to four or five times daily. The intensity of the pain is triggered by both pressure and cold. During his initial clinic visit, the patient reported that the level of pain was preventing him from sleeping, sitting, or participating in normal every day activities, and he assessed that this condition was having an appreciable negative effect on the quality of life. In the first month of treatment, the patient developed a new lesion on the right shoulder and reported an increase in the frequency of pain episodes. The patient was placed initially on gabapentin and then nifedipine with limited success in pain control. The lesions continued to proliferate, and the patient was referred to surgery for excision.
Physical Examination
On the upper back were six, pink-to-flesh-colored-to- red, firm, subcutaneous, oval nodules, which ranged in size from 8 mm to 1.3 cm in length by 4 mm to 6 mm in width. On the mid area of the back were ten to 15 similar, although slightly smaller, nodules that followed the lines of skin tension. A single, 4 mm, firm, flesh-colored nodule was noted on the lateral aspect of the right shoulder.
Laboratory data
None.
Histopathology
There is a circumscribed, non-encapsulated proliferation of smooth muscle bundles in an interlacing configuration in the papillary and upper reticular dermis.
Comment
Cutaneous leiomyoma is a benign, smooth-muscle neoplasm that was first reported in 1854 by Rudolf Virchow [1]. In the skin, leiomyomas can occur in any of three separate locations where smooth muscles occur: arrector pili muscles (piloleiomyomas), blood-vessel walls (angioleiomyomas), and genital/areolar skin. Regardless of location, the lesions are similar in appearance as well-demarcated, oval, red-brown, intradermal nodules that are fixed to the superficial skin and that range from 2 mm to 2 cm. Genital leiomyomas are usually solitary and asymptomatic. In contrast, piloleiomyomas, which are the most common type, are usually multiple, occur in groups in linear or dermatomal arrangements, and are frequently painful. The pain is described as burning, pinching, or stabbing and can be elicited by a variety of stimuli, which include cold, trauma, touch, and pressure. The pain also or may be spontaneous [2]. The origin of the pain is poorly understood but may be due to either an increased density of nerve fibers or, as is more commonly believed, contraction of the smooth muscle [2]. Extensor surfaces are most commonly involved, but the trunk, face, and neck also can be affected. It is common, however, for more than one body location to be affected [3]. Age of onset is in the second to fourth decades with no gender-bias. Angioleiomyomas are painful in 50 percent of cases, with similar triggers; they are most common in middle aged women and are located on the lower leg.
In 75 percent of patients with multiple leiomyomas, a mutation in the fumarate hydratase gene located on chromosome 1q42.3-43 has been described [4]. Although most cases are isolated, some cases of familial clusters, which include identical twins [5], have been documented, which suggests a subset with a pattern of autosomal dominant inheritance but incomplete penetrance. This genetically inherited variant has been reported to have an association with type II papillary renal carcinomas and renal collecting duct cancers.
The disease is usually regarded as benign although development of leiomyosarcoma as well as other forms of leiomyoma have been reported. Although mortality may be low, morbidity from the disease can be high. Lesions can be painful to the level of disability. The lesions do not spontaneously regress but typically enlarge and increase in number, with an associated progression in the level of pain and impingement of the activities of daily living.
Treatment options are limited. Excision is curative, but recurrence is common, especially in patients who initially present with multiple lesions [2]. Recurrence has been reported from six weeks to 15 years after surgery. Electrocoagulation, cryotherapy, and radiation therapy also have been utilized in treatment but have been shown to have little clinical benefit. A single report of carbon-dioxide laser ablation was recently published [6]. This approach had previously been used successfully with uterine leiomyomas where recurrence rates are much lower. In the skin the use of the carbon-dioxide laser provided a three-month resolution after treatment in a single 73-year-old patient. Oral nitroglycerin, nifedipine, and phenoxybenzamine [7, 8] have been tried in an attempt to promote smooth muscle relaxation; however, success has been limited. A subset of patients are unable to tolerate these medications or have a medical contraindications to their use.
Symptomatic treatment has been attempted with pain blocking medications, such as gabapentin, due to the neuropathic nature of the pain. This approach has met with variable, but always incomplete, pain resolution.
References
1. Kohler S. Muscle, adiopose and cartilage neoplasms. In: Bolognia JL, et al. Dermatology, London, Mosby Elsevier, 2nd edition, 2008, 23912. Holst VA, et al. Cutaneous smooth muscle neoplasms: clinical features: histologic findings, and treatment options, J Am Acad Dermatol 2002; 46, 477. [PubMed]
3. Raj S, et al. Cutaneous pilar leiomyoma: clinicopathologic analysis of 53 lesions in 45 patients. Am J Dermatopathol 1997; 19:2 [PubMed]
4. The Multiple Leiomyoma Consortium. Germline mutations in FH predispose to dominantly inherited uterine fibroids, skin leiomyomata and papillary renal cell cancer. Nat Genet 2002; 30:406 [PubMed]
5. Rudner EJ, et al. Multiple cutaneous leiomyoma in identical twins. Arch Dermatol 1964: 90: 81 [PubMed]
6. Christenson LJ, et al. Treatment of multiple cutaneous leiomyomas with CO2 laser ablation. Derm Surg 2000; 26: 319 [PubMed]
7. Thompson JA. Therapy for painful cutaneous leiomyomas. J Am Acad Dermatol 1985; 13:865 [PubMed]
8. Abraham Z, et al. Muscle relaxing agent in cutaneous leiomyoma, Dermatologica 1983; 166: 255 [PubMed]
© 2009 Dermatology Online Journal

