Treatment of pityriasis amiantacea with infliximab
Published Web Location
https://doi.org/10.5070/D35905b6kvMain Content
Treatment of pityriasis amiantacea with infliximab
Ryan K Pham DO1, C Stanley Chan MD2, Sylvia Hsu MD2
Dermatology Online Journal 15 (12): 13
1. University of North Texas Health Science Center, Fort Worth, Texas2. Baylor College of Medicine, Houston, Texas. shsu@bcm.edu
Introduction
Pityriasis amiantacea (PA) presents as tenaciously adherent scales surrounding the base of scalp hairs that can result in hair loss [1]. Baron Jean-Louis Alibert of France first described the condition in 1832 as an asbestos-like tinea [2]. The exact cause of PA is unclear and may be due to a number of underlying conditions [3, 4, 5]. It is thought to represent a reaction pattern to inflammatory skin disease with the most common causes being psoriasis and seborrheic dermatitis [6].
It is important to determine the primary cause, because treatment strategies are guided by the etiology. Currently there are no guidelines or strong recommendations for the treatment of PA as there are a limited number of reports on PA. We present a case of a woman with chronic pityriasis amiantacea who had no improvement from topical treatments but displayed remarkable results after 3 infliximab (Remicade®) infusions.
Case Report
A 47-year-old Caucasian woman presented to her dermatologist in 2001 with thick adherent scale on her scalp hair. Her dermatologist diagnosed her with pityriasis amiantacea due to psoriasis and treated her for 18 months with tar shampoo without any improvement. She was then referred to our clinic. The patient presented to us with thick adherent scale over her frontal, parietal, and vertex scalp. She was otherwise healthy and did not take any medications. There were no other skin manifestations of psoriasis or seborrheic dermatitis. The patient was prescribed 10 percent salicylic acid in olive oil q h.s. and clobetasol solution q a.m. and was instructed to wash her hair daily with tar shampoo. The patient returned for follow-up monthly for 3 months without any improvement. She was then given the option of a systemic drug, but the patient wanted to continue using topical medications due to concerns about long-term safety issues with systemic medications. For the next 6 years the patient was treated with 20 percent salicylic acid in olive oil, clobetasol propionate foam, MG217® shampoo, Clobex® lotion and shampoo, and clobetasol solution without any improvement. Four months ago the patient returned to our clinic as her condition had worsened with serous drainage from the scales. The fluid from the affected sites was cultured and yielded only coagulase-negative Staphylococcus species. After failed treatments in the past and growing frustration, she consented to start infusion therapy with infliximab. Examination of her scalp before starting infliximab showed confluent thick adherent mat-like scale with clumping of hair in the frontal and vertex scalp (Fig. 1). After 3 infusions of infliximab 5 mg/kg at weeks 0, 2 and 6, the patient showed dramatic improvement; all of the adherent scale had resolved (Fig. 2).
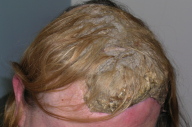 | 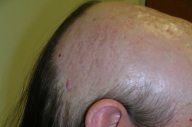 |
| Figure 1 | Figure 2 |
|---|
Discussion
Pityriasis amiantacea (PA) is a papulosquamous condition of the scalp that presents with asbestos-like thick scales attached to the hair shaft. Scales are arranged in an overlapping manner like flakes of asbestos, leading to its name amiantaceus [3]. The lesions can involve localized areas of the scalp or encompass it entirely. Long-standing inflammatory lesions of PA can lead to scalp fibrosis and result in permanent hair loss [7]. Pityriasis amiantacea seems to be more common in females and those of younger age, with a mean age of 23.8 in one of the largest studies of PA patients [6, 8].
The condition may be a reaction pattern to a number of inflammatory processes in the scalp. In one of the larger studies of patients with pityriasis amiantacea, scalp biopsies revealed pathologic diagnoses of psoriasis, seborrheic dermatitis, tinea capitis, atopic dermatitis, lichen planus, bacterial infection, and pityriasis rubra pilaris [6]. A recent report also describes PA as a manifestation of Darier disease [9]. Of these conditions, psoriasis and seborrheic dermatitis appear to be the most common causes for PA.
Staphylococcus aureus has been documented to be present in the majority of patients with PA [6, 10]. S. aureus isolation likely represents secondary bacterial infection or normal colonization. In one study, patients with Staphylococcal infection responded well with a combined regimen of systemic and topical antibiotics, topical corticosteroids, and coal tar [11]. Our patient grew only coagulase negative Staphylococcus, a common normal skin flora species.
In general, there is a paucity of studies regarding the treatment of PA. Effective and timely treatment of PA is critical to avoid scarring alopecia. The treatment should include keratolytic agents and topical corticosteroids [11]. Topical corticosteroids may reduce inflammation decreasing erythema and pruritus. They should be used intermittently, and their safety has not been documented beyond 4 weeks of use [11]. Keratolytic agents, like salicylic acid, help to remove thick, hyperkeratotic scales and improve penetration of other topical medications [12]. Shampoos containing ketoconazole, ciclopirox, and zinc pyrithione are also useful in treating thick scales.
PA can be difficult to effectively treat with topical medications as several weeks of use may be needed before benefits are seen, and the thick scale will often reaccumulate if not treated regularly. Topical treatments can also be messy and time-consuming, leading to high levels of non-compliance [13].
Systemic agents may be justified for select patients with severe pityriasis amiantacea that has failed to respond to topical treatments. Biologic agents, such as tumor necrosis factor-alpha (TNF-α) inhibitors, have been increasingly used for a variety of inflammatory dermatologic diseases [14]. Infliximab (Remicade®) was used in this case for PA due to psoriasis. This agent is a chimeric monoclonal antibody against TNF-α which leads to a decreased amount of interleukins (IL-1, IL-6) released from inflammatory cells, thus down-regulating inflammation downstream [15].
In cases of PA due to psoriasis, first-line treatment modalities involve keratolytics and topical corticosteroids. In cases of unrelenting disease, systemic therapies may be considered to prevent scarring alopecia and other associated morbidities. Our patient showed a tremendous response after 3 infusions of infliximab and is currently on an every 8-week infliximab 5 mg/kg maintenance regimen. To our knowledge, this is the first reported case of pityriasis amiantacea treated with a TNF-α inhibitor.
References
1. Plewing G, Jansen T. Seborrheic dermatitis. In Freedberg IM, Eisen AZ, Wolff K, et al., editors. Fitzpatrick's dermatology in general medicine, 6th edition. New York: McGraw-Hill; 2003. 1200-12012. Alibert JL. La porrigine amiantacea. Monographie des Dermatoses. Paris, France, 1832: 293-5.
3. Knight AG. Pityriasis amiantacea: a clinical and histopathological investigation. Clin Exp Dermatol 1977; 2: 137-142. [PubMed]
4. Hansted B, Lindoskov R. Pityriasis amiantacea and psoriasis: a follow-up study. Dermatologica. 1983; 166: 314-315. [PubMed]
5. Ring DS, Kaplan D. Pityriasis amiantacea: a report of 10 cases. Arch Dermatol 1993; 129: 913-914. [PubMed]
6. Abdel-Hamid IA, Salah AA, Moustafa YM, El-Labban AM. Pityriasis amiantacea: a clinical and etiopathologic study of 85 patients. Int J Dermatol 2003; 42: 260-4. [PubMed]
7. Langtry JAA, Ive FA. Pityriasis amiantacea, an unrecognized cause of scarring alopecia, described in four patients. Acta Derm Venereol. 1991; 71: 352-353. [PubMed]
8. Ring DS, Kaplan D. Pityriasis amiantacea: a report of 10 cases. Arch Dermatol 1993; 129: 913-914. [PubMed]
9. Hussain W, I. Coulson H, Salman WD. Pityriasis Amiantacea as the sole manifestation of Darier's disease. Clinical and Experimental Dermatology 2009; 34:552-558. [PubMed]
10. Shalev RM, Cohen AD, Medvedovsky E, Sashavinsky S, Tchetov T, Vardy DA. Pityriasis amiantacea associated with Staphylococcus aureus super-infection in bedouin patients. Microbial Ecology in Health and Disease 2004; 16-4: 218-221.
11. van der Vleuten CJ, van de Kerkhof PC. Management of scalp psoriasis: guidelines for corticosteroid use in combination treatment. Drugs 2001; 61(11):1593-8. [PubMed]
12. Matsunaga J, Maibach HI, Epstein E. Scalp and Hair, Palms and Soles. In Roenigk HH, Maibach HI. Psoriasis. 3rd edition. New York: Marcel Dekker Inc., 1998. 45-57.
13. Warren RB, Brown BC, Griffiths CE. Topical treatments for scalp psoriasis. Drugs 2008; 68(16):2293-302. [PubMed]
14. Alexis AF, Strober BE. Off-label dermatologic uses of anti-TNF alpha therapies. J Cutan Med Surg 2005; 9(6):296-302. [PubMed]
15. Gupta AK, Skinner AR. A review of the use of infliximab to manage cutaneous dermatoses. J Cutan Med Surg 2004; 8:77-89. [PubMed]
© 2009 Dermatology Online Journal

