Follicular mucinosis associated with mycosis fungoides.
Published Web Location
https://doi.org/10.5070/D356j1882qMain Content
Follicular mucinosis associated with mycosis fungoides
Lesley Clark-Loeser MD, and Jo-Ann Latkowski MD
Dermatology Online Journal 10 (3): 22
From the Ronald O. Perelman Department of Dermatology, New York University
Abstract
A 62-year-old man with a 13-year history of mycosis fungoides presented with a 2-month history of alopecia of the scalp. The mycosis fungoides had remained untreated for the previous 3.5 years. A biopsy specimen from the scalp showed follicular mucinosis in association with mycosis fungoides.
Clinical synopsis
History.—A 62-year-old man had a 4-month history of a dermatosis involving the saclp, face, and trunk. In 1991, a diagnosis of mycosis fungoides, stage 1b was made. Treatment modalities employed from 1991 through August 2000, included topical nitrogen mustard, topical glucocorticoids, and ultraviolet B phototherapy. However, the patient was lost to follow-up until February 2004, at which time he presented to the New York Harbor View Healthcare Dermatology Clinic. He was concerned about a 2-month history of hair loss on his scalp. Additionally, the patient explained that he had not treated his previously diagnosed skin condition for 3.5 years. Biopsies were taken from the scalp and chest, and after review of the dermatopathologic findings, the patient was given intralesional triamcinolone injections to the patches of alopecia on his scalp, and he was started on acitretin 25 mg a day. However, over the subsequent 2 months, the alopecia progressed, and loss of his axillary hair was noted.
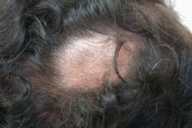
Physical examination.— There were several hairless patches with a cigarette-paper appearance and trace erythema at the leading edges without overlying scale. There was generalized facial erythema and a mild coarseness to the facial features. The chest, shoulders, abdomen, and back contained numerous flat erythematous plaques, coalescing in areas into medium-sized digitate plaques. Plaques along the clavicles had a notable cigarette paper surface appearance.
|
|
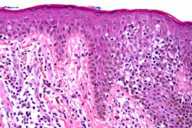
| Figure 1 | Figure 2 |
|---|
|
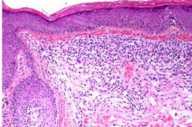
| Figure 3 |
|---|
Histopathology.—The dermis shows a moderately dense infiltrate of atypical lymphocytes, with a focal bandlike pattern that extends into the epidermis where there is minimal spongiosis. Lymphocytes have enlarged hyperchromatic nuclei with irregular contours. A scalp biopsy specimen shows in addition folliculotropism. An alcian blue stain shows early follicular mucinosis.
Immunohistochemical stains show positive staining of the atypical lymphocytes for T-cell markers (CD3, CD4, and CD8).There are rare CD20-positive B cells in the dermis only.
Diagnosis.—Follicular mucinosis associated with mycosis fungoides
Comment
First described in 1957, the term alopecia mucinosa referred to a characteristic disease process of follicular degeneration that lead to alopecia. To reflect the fact that the disease does not always present with or result in alopecia, the entity was renamed follicular mucinosa or follicular mucinosis in 1959. [1]
Follicular mucinosis may occur either as a primary benign disorder or as a secondary disorder associated with other benign or malignant diseases. There are two variants of primary follicular mucinosis. The more common is a spontaneously remitting process that presents in children and young adults. Less often, the primary variant occurs in older adults and is chronic and relapsing.
Benign conditions associated with secondary follicular mucinosis include spongiotic dermatitis, arthropod bites, alopecia areata, lupus erythematosus, sarcoidosis, hypertrophic lichen planus, lichen striatus, photo-induced eruptions, melanocytic nevi, familial reticuloendotheliosis, Goodpasture syndrome, and angiolymphoid hyperplasia. Secondary follicular mucinosis is most often observed in association with mycosis fungoides. Other associated malignant conditions include leukemia cutis, cutaneous B-cell lymphoma, acute myeloblastic leukemia, syringolymphoid hyperplasia, and Hodgkin's disease. [1,2,3] Mycosis fungoides with associated follicular mucinosis is felt to portend a more aggressive course. [3, 4]
A spectrum of clinical presentations exists. Typically follicular mucinosis occurs on the head and neck as indurated, plaques. Common presentations include plaques with prominent follicular openings and keratotic plugs and generalized or grouped follicular papules distributed on the trunk, proximal limbs, face, and scalp. Less commonly, the disease may resemble chronic eczema, alopecia areata, scarring alopecia, cystic lesions, or acneiform lesions. Histopathologic examination is essential in making this diagnosis. [1,3]
Histopathologic, features include mucin in the outer-root-sheath epithelia and sebaceous glands and an inflammatory infiltrate composed of lymphocytes, microphages, and eosinophils with folliculotropism of the lymphocytes. Some purport that the T-cell infiltrate stimulates the production of mucin by the keratinocytes and thus plays a role in the pathogenesis of follicular mucinosis.[1]
There is no specific treatment for follicular mucinosis. The primary variant tends to remit spontaneously. Nonetheless, a variety of therapeutic modalities have been employed with various degrees of success: topical, intralesional, and systemic glucocorticoids; PUVA photochemotherapy; x-irradiation; dapsone, antimalarials; indomethacin; minocycline; oral isotretinoin; interferon &alfa;-2b, and UVA1 phototherapy. Treatment for secondary follicular mucinosis requires treatment of the underlying or associated disease.
References
1. Bonta MD, et al. Rapidly progressing mycosis fungoides presenting as follicular mucinosis. J Am Acad Dermatol 2000; 43:635.2. Honig BJ, et al. Widespread eczematous dermatitis with erythematous facial plaques: alopecia mucinosa (follicular mucinosis [FM]) with possible mycosis fungoides (MF). Arch Dermatol 1991; 127:1397.
3. Anderson BE, et al. Alopecia mucinosa: report of a case and review. J Cutan Med Surg 2003; 7:124.
4. Apisarnthanarax N, et al. Mycosis fungoides with follicular mucinosis displaying aggressive tumor-stage transformation: successful treatment using radiation therapy plus oral bexarotene combination therapy. Am J Clin Dermatol 2003; 4:429.
© 2004 Dermatology Online Journal

