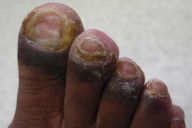
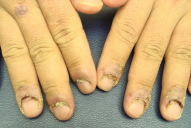
Nail disease in pemphigus vulgaris
Published Web Location
https://doi.org/10.5070/D34x05d6vhMain Content
Nail disease in pemphigus vulgaris
Brittany Dusek Serratos1, Rashid M Rashid MD PhD2
Dermatology Online Journal 15 (7): 2
1. University of Texas Medical School, Houston, Texas2. Department of Dermatology, MD Anderson Cancer Center, UT-Houston, Texas. Rrashid@mdanderson.org
Abstract
Patients affected by pemphigus vulgaris will occasionally present with associated and characteristic nail changes. This manuscript was prepared as a review of this unique presentation of pemphigus. Articles describing pemphigus vulgaris of the nail were compiled and reviewed and pertinent information was extracted to provide a concise analysis. The literature on this topic is still maturing. Publications to date suggest the incidence of nail and periungal involvement may correlate with the severity of mucocutaneous symptoms and the duration of the disease. The most common nail manifestations reported were acute or chronic paronychia and onychomadesis, and involvement of the fingernails. The nail changes may precede or develop concurrently with the mucocutaneous presentation. The diagnosis can be made by histologic identification and/or by the presence of IgG and C3 with direct immunoflourescence testing. Systemic treatment is required and highly effective; it includes a tailored combination of anti-inflammatory medications, immunosuppressive agents, and/or immunomodulatory treatments. This review aims to provide a better understanding of pemphigus vulgaris nail changes and guidance for clinical treatment. Unknown etiologies, predisposing factors, discrepancies evident in the literature, and limited research warrant further investigation of pemphigus vulgaris of the nail.
Introduction
Pemphigus vulgaris is a rare autoimmune disease that causes blistering lesions, primarily of the mucous membranes and skin. Occasionally, affected patients will present with associated, yet slightly variable, nail manifestations. Currently, there are very few substantial studies that thoroughly describe the nail involvement associated with pemphigus vulgaris, and even fewer studies supported by statistical evidence. This article reviews the available research and discusses a clinical approach to the etiology, diagnosis, and treatment of pemphigus vulgaris of the nail.
Etiology and predisposing factors
The mucocutaneous symptoms of pemphigus vulgaris are caused by the binding of IgG autoantibodies to desmosomal-associated glycoproteins, desmoglein 1, and/or desmoglein 3 [1, 2, 3, 4]. This autoimmune reaction leads to acantholysis, or disruption of cell-to-cell interactions, that manifests as painful blisters and erosive lesions.
Overall, there are 0.75 to 5 cases/million every year of pemphigus subtypes [5], with pemphigus vulgaris as the dominating presentation. Pemphigus vulgaris may develop at any age, but most commonly occurs during the fourth, fifth, and sixth decades [6, 7]. Case series studies conducted by Habibi and Schlesinger both found the average age of onset in their patient population to be approximately 46 years [8, 9].
Although the cause of nail involvement in patients with pemphigus vulgaris remains unknown, research consensus demonstrates a low reported incidence among the patient population [4, 10]. Bullae located in close proximity to the nail are believed to provoke nail involvement [8]. Recent research has suggested that nail involvement may correlate with an increased severity of the disease, as evidenced by lesions in other locations on the body [10]. Additionally, research has correlated the incidence of nail involvement with disease longevity, suggesting that patients with a longer duration of disease and accumulated inflammation are more likely to present with nail changes [8].
Presentation
The incidence of nail disease in pemphigus vulgaris patients is variable. The majority of patients (47%) present with nail manifestations initially in conjunction with mucosal and cutaneous lesions. Thirty-three percent of patients have pre-existing nail manifestations, and 20 percent of patients have nail manifestations as the only indication of disease [11]. When nail involvement presents initially, there will usually be a window of several weeks before presentation of the pemphigus vulgaris mucocutaneous symptoms [12]. Although many articles claim that nail manifestations in pemphigus are rare, the most recent pemphigus vulgaris prospective study conducted by Habibi et al. involving 79 patients with the disease found that 25 (34.2%) patients reported nail changes [8]. Twenty-four of these patients experienced nail changes during the course of the disease; one patient had an onycomycosis relapse due to a previous manifestation. Schlesinger et al. conducted a retrospective study involving 64 pemphigus vulgaris patients, and found a higher prevalence, with 47 percent of patients reporting nail manifestations [9].
There is also a large degree of variation in nail manifestations present among pemphigus vulgaris patients. The most common presentations reported in all studies are acute or chronic paronychia and onychomadesis [4, 10, 12]. Acute and chronic paronychia are the most frequent features, which presents in 51.9 percent of all cases of pemphigus vulgaris of the nail [12]. Acute paronychia is likely caused by infection, with S. aureus and C. albicans presenting as common infectious agents [12]. The prevalence of these agents was not provided in the literature. Chronic paronychia is likely caused by the acantholysis of the lateral nail fold. Onychomadesis is reported in 33 percent of cases [10], and can be attributed to autoimmune disease manifestations inhibiting normal nail plate growth and development; alternatively, by the formation of blisters beneath the nail causing detachment of the nail plate may produce this finding [13]. Habibi et al. speculates that prolonged inflammation of the nail matrix may cause nail changes such as onychomadesis and Beau's lines [8]. Other less frequently observed nail manifestations include subungual hemorrhage, discoloration of the nail plate, subungual hyperkeratosis, trachyonychia, nail pitting, onychomycosis, Beau's lines, onycholysis, and onychodystrophy [9, 10, 13, 14-18]. Nail manifestations frequently overlap among patients. Habibi et al. reported that 30 percent of patients with nail changes who had more than one type of manifestation [8]. Onychomycosis is reported in 25 percent of pemphigus vulgaris patients and this is found to have an increased incidence among patients undergoing immunosuppressive therapy [9]. By contrast, the incidence of onychomycosis in the general population is only 2.7 – 13 percent. Other symptoms reported include pain upon distal palpation of affected nails, excretion of an inflammatory serous exudates by the lateral nail folds upon light compression [13], black to red-blue discoloration of the proximal nailfolds, ulceration, erythema, and edema.
Fingernails are more commonly affected than toenails, and the thumbs and index fingers are the most frequent digits involved [10, 13]. Habibi et al. recorded a total of 101 involved nails in the patient population, 71 fingernails and 30 toenails [8]. Among the fingernails affected, there were 22 thumbs and 20 index fingers. The little finger was involved in only 4 cases, making it the least likely fingernail affected [8]. Additionally, Schlesinger et al. found that nail manifestations occurred only in the fingernails; among 30 patients affected by nail changes, 9 reported thumb involvement and 7 reported index finger involvement. The majority of patients in all studies have multiple affected nails [9].
Potential prognostic value
Nail involvement can present with exacerbation [12, 19] or reoccurrence [12, 20, 21] of pemphigus vulgaris. Moreover, nail involvement is augmented dually with duration of the symptoms [8] and increased severity of disease, as demonstrated by an increased number of periungual and mucocutaneous bullae. For example, Habibi et al. [8] found that among patients with nail changes, the mean duration of disease was 26.2 months. By comparison, the mean duration of disease was 10.6 months in patients without nail disease. (p<0.05) [8]. The same study found that out of 1580 total nails in the study, 71 had periungual bullae, with 31 percent leading to nail changes. Moreover, out of the 1509 nails that were not affected by periungual bullae, only 5.2 percent reported nail changes (p<0.005).
Diagnosis
The easiest and most painless method of diagnosing pemphigus vulgaris of the nail is to extract a biopsy specimen from perilesional skin and perform direct immunoflourescence testing. A positive result will reveal intercellular fluorescence with IgG immunoglobulins and C3 [22]. Specific direct immunoflourescence (DIF) testing of a nail bed, matrix, or nail fold biopsy is only indicated in cases of chronic paronychia or onychomadesis that precede mucocutaneous lesions, or in cases in which only a single nail is affected [16] and chronic immunosuppressive therapy is omitted [13]. If DIF is positive, the diagnosis can be confirmed by conducting subsequent indirect immunoflourescence testing using the patient's serum [22]. Additionally, a histological examination of biopsy specimens acquired from blistering lesions on the fingers will reveal acantholysis above the basal cell layer [23].
Differential Diagnosis
It is important to distinguish acute paronychia as a sign of pemphigus vulgaris exacerbation from other similar clinical presentations, such as bacterial or candidal paronychia, genetic paronychia, or trauma. Paronychia presenting with pemphigus vulgaris with have a characteristic pathologic feature: suprabasal acantholysis without spongiosis or exocytosis. In addition, ballooning degeneration, reticular degeneration, and multinucleated giant cells in the epidermis are absent, which may be present in the above-mentioned alternative diagnoses [12]. Bacterial and fungal cultures should be preformed.
Treatment
All studies maintain that the application of topical therapy in the treatment of nail manifestations is ineffective and that systemic treatment is mandatory to control symptoms. Additionally, appropriate immunosuppressive treatment can successfully control pemphigus vulgaris nail manifestations, with potentially minimal untoward effects [12]. A few regimens have been suggested, which must be tailored to each individual patient. For example, recent research has reported success in treatment of nail manifestations in pemphigus vulgaris patients with IVIG therapy, which resulted in complete nail recovery [10]. Other studies found the systemic use of corticosteroids with azathioprine, or corticosteroids with cyclophosphamide and mycophenolate mofetil to be highly effective in the treatment of nail manifestations with comparable success [11, 16, 23].
Prognosis
Prior to the advent of corticosteroids, the mortality rate of patients with pemphigus vulgaris was between 60 percent and 90 percent [24, 25, 26, 27]. The administration of corticosteroids and immunosuppressive drugs have effectively reduced the mortality rate to less than 10 percent [28]. Moreover, the available treatments for pemphigus vulgaris offer complete resolution of both nail and mucocutaneous manifestations [10]. Prognosis in regards to mortality and correlation with nail disease has not been reported.
Conclusion
The limited pool of research regarding the etiology, frequency, and presentation of pemphigus vulgaris of the nail necessitates further investigation. Although most studies in the literature claim that nail changes are a rare occurrence, recent research [8, 9, 29, 30] argues that a higher frequency may be observed. Furthermore, extrapolation from the reported literature continues to emphasize the neglected painful nature of pemphigus equally in periungal and mucocutaneous presentations [31]. Several studies have proposed that the future of pemphigus vulgaris nail research should involve exploring the antigenic properties of the nail unit as a separate entity [9, 13]. Hopefully future studies will provide a better understanding of this interesting ungual phenomenon.
References
1. Champion RH, Burton JL, Burns DA et al. Textbook of Dermatology. 6th ed. Oxford, Blackwell Science, 1998. p. 1849-1855.2. Eyre RW & Stanley JR. Identification of pemphigus vulgaris antigen extracted from normal human epidermis and comparison with pemphigus foliaceus antigen. J Clin Invest 1988; 81: 807-12. [PubMed]
3. Zillikens D, Schmidt E, Reimer S, Chimanovitch I, Hardt-Weinelt K, Rose C, Brocker EB, Kock M, Boehncke WH. Antibodies to desmogleins 1 and 3, but not to BP180, induce blisters in human skin grafted onto SCID mice. J Pathol 2001; 193 (1): 117-24. [PubMed]
4. Lieb J, Levitt J, Sapadin AN. Nail findings in pemphigus vulgaris. Int J Dermatol 2006; 45 (2): 172-4. [PubMed]
5. Amagai M. Pemphigus. In: Bolognia JL, Jorizzo JL, Rapini RP, editors. Dermatology. New York: Mosby; 2002. pp. 449-62.
6. Sampaio Sap & Rivitti EA. Dermatologia. Brasil. 2nd ed. Sao Paulo, Artes Medicas, 2000. p. 229-248.
7. Martins CR, Squiquera HL & Diaz LA. Pemphigus vularis and pemphigus foliaceus. Curr Probl Dermatol 1989; 1: 33-61. [PubMed]
8. Habibi M, Mortazavi H, Shadianloo S, Balighi K, Ghodsi SZ, Daneshpazhooh M, Valikhani M, Ghassabian A, Pooli AH, Chams-Davatchi C. Nail changes in pemphigus vulgaris. International Journal of Dermatol 2008, 47, 1141-1144. [PubMed]
9. Schlesinger N, Katz M, Ingber A. Nail involvement in pemphigus vulgaris. Br J Dermatol 2002; 146: 836-9. [PubMed]
10. Engineer L, Norton LA, & Ahmed AR. Nail involvement in pemphigus vulgaris. J Am Acad Dermatol 2000; 43: 529-35. [PubMed]
11. Cahali JB et al. Nail manifestations in pemphigus vulgaris. Rev. Hosp. Clin. Fac. Med. S. Paulo 57 (5): 229-234, 2002. [PubMed]
12. Lee HE, Wong WR, Lee MC, Hong HS. Acute paronychia heralding the exacerbation of pemphigus vulgaris. Int J Clin Pract 2004; 58: 1174-6. [PubMed]
13. Patsatsi A, Sotiriou E, Devliotou-Panagiotidou D, Sotiriadis D. Pemphigus vulgaris affecting 19 nails. Clinical and Experimental Dermatology, 34, 202-205. [PubMed]
14. Baumal A, Robinson MJ. Nail bed involvement in pemphigus vulgaris. Arch Dermatol 1973; 107: 751. [PubMed]
15. Berker DD, Dolziel K, Dawber RPR, et al. Pemphigus associated with nail dystrophy. Br J Dermatol 1993; 129: 461-464. [PubMed]
16. Kolivras A, Gheeraert P, Andre J. Nail destruction in pemphigus vulgaris. Dermatology 2003; 206: 351-352. [PubMed]
17. Reich A, Wisnicka B, Szepietowski JC. Hemorrhagic nails in pemphigus vulgaris. Acta Derm Venereol 2008; 88 (5): 542. [PubMed]
18. Rivera Diaz R, Alonso Llamazares J, Rodriguez Peralto JL, et al. Nail involvement in pemphigus vulgaris. Int J Dermatol 1996; 35: 581-82. [PubMed]
19. Akiyama C, Sou K, Furuya T et al. Paronychia: a sign heralding an exacerbation of pemphigus vulgaris. J Am Acad Dermatol 1993; 29: 494-496. [PubMed]
20. Kim BS, Song KY, Youn JI, et al. Paronychia – a manifestation of pemphigus vulgaris. Clin Exp Dermatol 1996; 21: 315-317. [PubMed]
21. Lauber J, Turk K. Beau's lines and pemphigus vulgaris. Int J Dermatol 1990; 29: 309. [PubMed]
22. Fulton RA, Campbell I, Caryland D, Simpson NB. Nail bed immunoflourescence in pemphigus vulgaris. Acta Derm Venereol (Stockh) 1983; 63: 170-2. [PubMed]
23. Mascarenhas R, Fernandes B, Reis JP et al. Pemphigus vulgaris with nail involvement presenting with vegetating and verrucous lesions. Dermatol Online J 2003; 9: 14. [PubMed]
24. Ahmed AR, Moy R. Death in pemphigus. J Am Acad Dermatol 1982; 7(2): 221-8. [PubMed]
25. Savin JA. International mortality from bullous diseases since 1950. Br J Dermatol 1976; 94(2): 179-89. [PubMed]
26. Savin JA. The events leading to the death of patients with pemphigus and pemphigoid. Br J Dermatol 1979; 101(5): 521-34. [PubMed]
27. Savin JA. Corticosteroids and death in pemphigus. J Am Acad Dermatol 1983; 9 (2): 275. [PubMed]
28. Chams-Davatchi C, Valikhani M, Daneshpazhooh M, Esmaili N, Balighi K, Hallaji Z, Barzegori M, Akhiani M, Ghodsi Z, Mortazavi H, Naraghi Z. Pemphigus: analysis of 1209 cases. Int J Dermatol 2005; 44 (6): 470-6. [PubMed]
29. Carducci M, Calcaterra R, Franco G, Mussi A, Bonifati C, Morrone A. Nail involvement in pemphigus vulgaris. Acta Derm Venereol 2008; 88 (1): 58-60. [PubMed]
30. Dhawan SS, Zaias N, Pena J. The nail fold in pemphigus vulgaris. Arch Dermatol 1990; 126: 1374-5. [PubMed]
31. Rashid RM, CAndido KD Pemphigus pain: a review on management. Clin J Pain. 2008 Oct;24(8):734-5. [PubMed]
32. Stone OJ, Mullins JF. Vegetative lesions in pemphigus. Dermatol Int 1966; 5: 137-40. [PubMed]
33. Parameswara YR, Naik RPC. Onychomadesis associated with pemphigus vulgaris. Arch Dermatol 1981; 117: 759-60. [PubMed]
© 2009 Dermatology Online Journal