Extramammary Paget disease
Published Web Location
https://doi.org/10.5070/D34kn8q2dfMain Content
Extramammary Paget disease
Robert Anolik MD, Christine Liang MD, Nadia Wang MD, Karla Rosenman MD, Miriam Pomeranz MD, Edwin Joe MD
Dermatology Online Journal 14 (10): 15
Department of Dermatology, New York UniversityAbstract
A 59-year-old man presented with a well-demarcated, tender ulcer at the base of the penile shaft that had been present for approximately five years. The ulcer had been responsive neither to topical antibacterials, antifungals, and glucocorticoids nor to oral acyclovir. A biopsy specimen showed an intra-epidermal neoplasm consistent with extramammary Paget disease (EMPD) based on light microscopy and immunohistochemistry. Patients with EMPD require extensive medical evaluation because of its association with adnexal carcinoma and visceral malignant conditions. Evaluation should include a full body skin and lymph node examination, colonscopy, cystoscopy, and sex-specific studies including pelvic and breast examinations, with imaging for women and prostate examination with prostate specific antigen levels for men. Close monitoring after treatment is important because of the recognized risk of recurrence and malignant conditions.
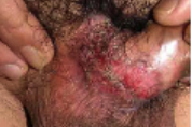 | 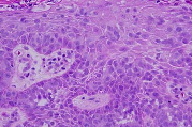 |
| Figure 1 | Figure 2 |
|---|
History
A 59-year-old man initially presented to the Urgent Care Clinic at Gouverneur Healthcare Services with the complaint of a penile ulcer. The ulcer began approximately five yeares ago. At times, it is painful and, at other times, nearly heals. The patient denies other similar lesions on himself or his wife. In the past, he was told that he might have a herpes simplex virus infection but was never treated for herpes simplex. Prior treatment included topical neomycin, triple antibiotic ointment, and Chinese herbal medicines. The patient was treated with acyclovir and with instructions to follow-up in the Dermatology Clinic.
In the Dermatology Clinic, the differential diagnosis and possibility of skin biopsy were discussed. Despite oral anti-herpetic treatment and topical antibacterial, antifungal, and anti-inflammatory agents, the patient appeared to improve at a slower than expected rate. After several weekly visits, the patient ultimately agreed to a skin biopsy.
Medical history includes gastroesophageal reflux. He takes no medicines, is without drug allergies, and, although he smokes cigarettes, denies alcohol intake or a history of intravenous drug abuse.
Physical Examination
A superficial, well-demarcated, crusted ulcer that measured 2 x 2 cm with a surrounding rim of erythema was noted at the base of the penile shaft. The ulcer was moderately tender. No penile discharge or testicular tenderness was noted. Inguinal lymphadenopathy was not present.
Lab
A complete blood count with differential analysis, basic metabolic panel, lipid profile, prostate specific antigen, and thyroid stimulating hormone were normal. The alanine amino transferase was elevated at 44 IU/L and alkaline phosphatase at 127 IU/L, herpes simplex virus type 1 antibody was positive, herpes simplex virus type 2 antibody was negative, human immunodeficiency virus antibody was non-reactive, syphilis IgG antibody was non-reactive, chlamydia and gonorrhea cultures were negative, herpes simplex virus culture were negative, bacterial culture grew coagulase negative S. aureus, occult fecal blood was negative, and urinalysis showed trace blood.
Histopathology
The mucosa is acanthotic and spongiotic with overlying parakeratosis, crust, and erosion. Within the mucosa, there are numerous atypical cells arranged as single units and as clusters with large vesicular nuclei, prominent basophilic nucleoli, and abundant pale staining cytoplasm. The atypical cells stain positively with periodic acid-Schiff, carcinoembryonic antigen, epithelial membrane antigen, and cytokeratin 7 and negatively for cytokeratin 20 and S100.
Comment
Extramammary Paget disease (EMPD) is a rare intra-epidermal adenocarcinoma. Despite sharing clinical and pathologic traits with mammary Paget disease (MPD), EMPD demonstrates important differences that include sites of involvement, pathogenesis, and relationship with associated malignant conditions.
The precise incidence of EMPD remains unknown although it arises far less frequently than does MPD [1]. EMPD of the vulva is the most common presentation and represents two percent or less of primary vulvar neoplasms [2]. EMPD arises in those aged 50 to 80 years and is more commonly found in women [3]. However, in the Asian population, men are more often afflicted [4]. Although no specific evidence of genetic predisposition has been found, rare familial occurrence has been reported [5].
Clinically, the eruption favors an apocrine gland distribution and most commonly arises on the vulva, penis and scrotum as well as on anal, perianal, axillary, and umbilical skin [6]. It also may occur on the buttock, thigh, eyelid, and external auditory canal [7]. When found on non-apocrine bearing sites, it is referred to as ectopic EMPD [1]. Multifocal and mucous membrane EMPD comprises a very small proportion of cases [8].
Extramammary Paget disease usually presents as a slowly-expanding, erythematous plaque, with sharp demarcation and an erythematous, scaly surface [1]. Pruritus is the most common presenting symptom [2]. The insidious onset, when combined with mimicry of intertrigo or tinea cruris, often delays the diagnosis five to ten years [9].
Histopathologic features include the characteristic Paget cells, which are large, round cells with abundant, pale cytoplasm and central or laterally compressed vesicular nuclei [1, 10]. These cells may be scattered singly or in the form of clusters, glandular structures, or solid nests and favor the lower portion of the epidermis [2]. A dense inflammatory infiltrate that can include plasma cells usually exists in the upper dermis [1]. Since other entities can demonstrate a pagetoid spread appearance, immunohistochemistry is employed to differentiate EMPD. Cytokeratin 7 has proven to be an important and sensitive marker for EMPD [2, 11].
The pathogenesis of EMPD remains uncertain. Many theorize that EMPD arises from at least two pathways, which are known as primary and secondary forms [8]. Primary EMPD originates from skin, in which the Paget cells represent erratic pluripotent cells of the epidermis or adnexae [8]. Secondary EMPD is associated with a distant adenocarcinoma, in which Paget cells are theorized to reflect the invasion of epidermotropic malignant cells [8]. Other theories suggest an oncogenic stimulus that simultaneously drives both intraepidermal and associated (adnexal or internal) adenocarcinomata [8]. In contrast, evidence supports one theory of the original of the Paget cell in MPD from cells of an epidermotropic breast carcinoma [8].
The prognosis for patients with EMPD and MPD is in part related to their relationship with an internal malignant condition. While MPD is nearly always associated with underlying mammary carcinoma, EMPD is reported to have an underlying adnexal adenocarcinoma in fewer that five percent of patients and a visceral malignant condition in 10 to 20 percent of patients [12, 13]. In primary EMPD, the prognosis is relatively favorable and worsens with vertical spread, particularly below one millimeter [8]. EMPD involvement of the external genitalia favors bladder, urethral, and prostate malignant conditions while perianal involvement favors colorectal neoplasms [2].
The association with underlying malignant conditions demands extensive evaluation on diagnosis of EMPD. Evaluation should include full body skin and lymph node examinations, colonscopy, cystoscopy, and sex-specific studies that include pelvic and breast examination with imaging for women and prostate examination with prostate specific antigen levels for men [8]. Oncologists, gynecologists, urologists, and gastroenterologists often are often involved in the patient's care.
Treatment of choice for local EMPD remains wide local excision or Mohs micrographic surgery [6, 13, 14]. Challenges stem from the spread of Paget cells beyond the visible limits of the lesion [3]. Margins of 1-cm have been shown to be effective when clear clinical margins are noted [15]. Some have proposed algorithms to indicate if and when lymph node dissection is appropriate in EMPD [4]. Alternative therapies include topical retinoids, 5-fluorouracil, and imiquimod [16]. For advanced EMPD that requires systemic treatment, no one chemotherapeutic regimen has yet been defined [9].
References
1. Shepherd V, et al. Extramammary Paget's disease. BJOG: An International Journal of Obstetrics & Gynaecology 2005; 112: 273 PubMed2. Smith KJ, et al. Cytokeratin 7 staining in mammary and extramammary Paget's disease. Mod Pathol 1997; 10: 1069 PubMed
3. Zollo JD, et al. The Roswell Park Cancer Institute experience with extramammary Paget's disease. Br J Dermatol 2000; 142: 59 PubMed
4. Chang YT, et al. Extramammary Paget's disease: a report of 22 cases in Chinese males. J Dermatol 1996; 23: 320 PubMed
5. Demitsu T, et al. Extramammary Paget's disease in two siblings. Br J Dermatol 1999; 141: 951 PubMed
6. O'Connor WJ, et al. Comparison of mohs micrographic surgery and wide excision for extramammary Paget's disease. Derm Surg 2003; 29: 723 PubMed
7. Heymann WR. Extramammary Paget's disease. Clin Dermatol 1993; 11: 83 PubMed
8. Kanitakis J. Mammary and extramammary Paget's disease. J Eur Acad Dermatol Venereol 2007; 21: 581 PubMed
9. Henning JS. Extramammary Paget's disease of the penis and scrotum. J Drugs Dermatol 2006; 5: 652 PubMed
10. Kirkham N. Tumors and cysts of the epidermis. In: Elder D, et al, eds. Lever's Histopathology of the Skin. 8th ed. New York: Lippincott Williams and Wilkins, 1997: 736
11. Park S, et al. Extramammary Paget's disease of the penis and scrotum: excision, reconstruction and evaluation of occult malignancy. J Urol 2001; 166: 2112 PubMed
12. Cooper, SM, et al. Anogenital (non-venereal) disease. In: Bolognia, JL, et al., eds. Dermatology. 2nd ed. London: Mosby, 2008: 1067
13. Tsutsumida A, et al. Indications for lymph node dissection in the treatment of extramammary Paget's disease. Derm Surg 2003; 29: 21 PubMed
14. Murata Y, et al. Extramammary Paget's disease of the genitalia with clinically clear margins can be adequately resected with 1cm margin. Eur J Dermatol 2005; 15: 168 PubMed
15. Ye JN, et al. Extramammary Paget's disease resistant to surgery and imiquimod monotherapy but responsive to imiquimod combination topical chemotherapy with 5- fluorouracil and retinoic acid: a case report. Cutis 2006; 77: 245 PubMed
16. Cohen PR, et al. Treatment of extramammary Paget disease with topical imiquimod cream: case report and literature review. South Med J 2006; 99: 396 PubMed
© 2008 Dermatology Online Journal

