Linear and whorled nevoid hypermelanosis
Published Web Location
https://doi.org/10.5070/D34dg7t3t4Main Content
Linear and whorled nevoid hypermelanosis
Jale Yuksek MD1, Engin Sezer MD1, Ahmet Hakan Erbil MD 2, Ercan Arca MD 2, Halis Bülent Taştan MD 2, Zafer Kurumlu MD2, Murat Demiriz MD 3
Dermatology Online Journal 13 (3): 23
1. Department of Dermatology, Gaziosmanpasa University School of Medicine, Tokat, Turkey. jaleyuksek@mynet.com2. Department
of Dermatology, Gülhane Military Medical Academy, School of Medicine, Ankara, Turkey 3. Department of Pathology, Gülhane Military
Medical Academy, School of Medicine, Ankara, TurkeyAbstract
Linear and whorled nevoid hypermelanosis (LWNH) is a rare skin condition characterized by swirls and whorls of hyperpigmented macules in a reticulate pattern along Blaschko's lines; approximately 40 cases have been reported in the English language literature. We report a case of LWNH occurring in a 20-year-old man with widespread involvement over the trunk, face, upper limbs, and genitalia in association with scoliosis. A small hyperpigmented area on the abdomen was treated with a medium-depth chemical peel regimen using 70 percent glycolic acid and 35 percent trichloroacetic acid with no benefit. This is the first report of LWNH treated with medium-depth chemical peel.
Linear and whorled nevoid hypermelanosis (LWNH) is a reticulate pigmentary disorder characterized by hyperpigmented macules in a streaky configuration, evolving along Blaschko's lines [1, 2, 3]. Linear and whorled nevoid hypermelanosis was first described as a distinctive entity in 1988 by Kalter [1], and to date, approximately 40 patients have been reported in the literature. To the best of our knowledge, this is the first case from Turkey.
Extracutaneous findings including neurological, skeletal and ocular anomalies have been reported [4, 5, 6]. Herein we present a 20-year-old man with asymptomatic widespread, swirled hyperpigmented macules following the lines of Blaschko. The hyperpigmentation has been progressive since infancy and the patient also developed scoliosis during childhood.
Clinical synopsis
A 20-year-old man presented with asymptomatic, hyperpigmented patches that first appeared at age 6 months. The lesions spread gradually and stabilized within 2 years after birth. He was the product of a full-term vaginal delivery and his mother denied any medication during pregnancy. There was no history of antecedent blistering or inflammation. Psychomotor and mental developments were normal.
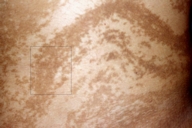
On physical examination, swirls and whorls of brown hyperpigmented macules on the trunk, neck, perioral area, genitalia, and upper limbs, along Blaschko's lines were observed. The macules consisted of reticulate and coalesced areas of hyperpigmentation, 1-3 mm in diameter. A Wood's lamp examination also accentuated the pigmented areas suggesting significant epidermal pigmentation.
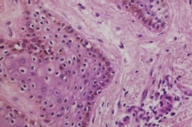
A skin biopsy specimen revealed diffuse hyperpigmentation of the basal layer and mild elongation of rete ridges (Fig. 1). Basal cell degeneration, pigmentary incontinence and melanophages in the upper dermis were not observed. Masson-Fontana staining was consistent with diffuse heavy melanin pigmentation in the basal layer of the epidermis. Routine laboratory investigations including complete blood count, biochemical and urinary analyses were within normal limits.
A diagnosis of LWNH was established based on clinical and histopathological findings. A small pigmented area on the abdomen was treated with a medium-depth chemical peel regimen using 70 percent glycolic acid and 35 percent trichloroacetic acid (TCA). After local anesthesia with lidocaine-prilocaine (EMLA) cream and degreasing with acetone, 70 percent glycolic acid gel was applied and left on the skin for 2 minutes. Then a 35 percent TCA solution was applied until an evident frosting appeared. After the procedure, topical emollients were used regularly until healing was achieved. No change in pigmentation was achieved after complete healing, which required 2 weeks (Fig. 2).
Discussion
Linear and whorled nevoid hypermelanosis is a rare entity characterized by reticulate hyperpigmented macules in a streaky configuration [1, 7]. Similar conditions were previously reported under names, such as zebra-like hyperpigmentation, zosteriform hyperpigmentation, reticulate hyperpigmentation of Iijima [8, 9].
Although LWNH is a sporadic disorder, one familial case has been reported by Akiyama [10]. Our patient was born from non-consanguineous parents and there was no family history of pigmentation disorders. Kalter described the onset as occurring within a few weeks of birth with the extent of pigmentation progressing during the first 2-3 years of life before stabilizing [1]. Clinical findings include reticulate hyperpigmented macules that coalesce to form streaks and whorled areas over the trunk, extremities, neck, and face following the lines of Blaschko [11, 12]. The pigmented streaks display a V-shaped pattern over the spine, an S-shaped or whorled pattern over the anterior and lateral aspects of the trunk, and a linear arrangement over the extremities and genitalia [2]. These patterns also were observed in this present case study. Palms, soles, mucous membranes, and hairs are spared. The histopathological features are diffuse moderate hyperpigmentation in the basal layer and occasional lentiginous elongation of rete ridges and a slight increase in the number of melanocytes [3, 10, 12]. Widespread melanosis with elongation of rete ridges and lack of dermal pigment deposits or melanophages are similarly identified in our patient.
Differential diagnoses include Bloch-Sulzberger incontinentia pigmenti, linear epidermal nevi, and linear atrophoderma of Moulin. Incontinentia pigmenti (IP) is an X-linked dominant condition primarily affecting women, with the exception of reports in the literature of 4 males presenting with coexistent Klinefelter's syndrome [13, 14]. In our patient, the clinical lack of a vesicular or verrucous stage as well as the histopathological lack of melanophages and pigmentary incontinence helped us to exclude the diagnosis of IP. Epidermal nevi may present as hyperpigmented streaks following Blaschko's lines during infancy, but become papillomatous and hyperkeratotic with time [1, 3]. A rare widespread form frequently reveals epidermolytic hyperkeratosis in histopathological sections [11]. Later in childhood, the onset of a unilateral distribution and the association of cutaneous atrophy differentiates linear atrophoderma of Moulin from LWNH [15]. Although the hypothesis is unproven, during embryogenesis, the development of somatic mosaicism may be the mechanism that results in LWNH.
The association of extracutaneous features including neurological, skeletal and ocular abnormalities have been reported [4]. Scoliosis, body and face asymmetry, pectus excavatus, supinated varus foot and skeletal deficits have been reported [5, 6, 16]. Various neurological and ocular problems including severe mental retardation with macrocephaly, seizures, bilateral giant cerebral aneurysms, nystagmus and anisocoria have also been reported [5, 17]. We observed scoliosis in our patient. Other neurological and ocular investigations including cranial MRI were all normal. In our opinion cases diagnosed as LWNH should be carefully investigated for possible associated abnormalities.
Little is known about the treatment strategies of LWNH. No satisfactory treatment modalities are currently available. A medium-depth chemical peel regimen using 70 percent glycolic acid and 35 percent TCA is often successfully used in various pigmentary conditions that show increased amounts of melanin in the basal layer (melasma and solar lentigines), but did not help our patient [18, 19]. An approach using new laser technologies would be a reasonable next step. To our knowledge a proven treatment approach for LWNH does not exist.
References
1. Kalter DC, Griffiths WA, Atherton DJ. Linear and whorled nevoid hypermelanosis. J Am Acad Dermatol 1988; 19: 1037-44. PubMed2. Alvarez J, Peteiro C, Toribio J. Linear and whorled nevoid hypermelanosis. Pediatr Dermatol 1993; 10: 156-8. PubMed
3. Kanwar AJ, Dhar S, Ghosh S et al. Linear and whorled nevoid hypermelanosis. Int J Dermatol 1993; 32: 385-6. PubMed
4. Nehal KS, Pebenito R, Orlow SJ. Analysis of 54 cases of hypopigmentation and hyperpigmentation along the lines of Blaschko. Arch Dermatol 1996; 132: 1167-70. PubMed
5. Schepis C, Siragusa M, Alberti A et al. Linear and whorled nevoid hypermelanosis in a boy with mental retardation and congenital defects. Int J Dermatol 1996; 35: 654-5. PubMed
6. Romano C, Pirrone P, Siragusa M et al. An additional case of linear and whorled nevoid hypermelanosis associated with birth defects and mental retardation. Pediatr Dermatol 1999; 16: 71-3. PubMed
7. Mendiratta V, Sharma RC, Arya L et al. Linear and whorled nevoid hypermelanosis. J Dermatol 2001; 28: 58-9. PubMed
8. Alimurung FM, Lapenas D, Willis I et al. Zebra-like hyperpigmentation in an infant with multipl congenital defects. Arch Dermatol 1979; 115: 878-81. PubMed
9. Schepis C, Alberti A, Siragusa M et al. Progressive cribriform and zosteriform hyperpigmentation: the late-onset feature of linear and whorled nevoid hypermelanosis associated with congenital neurological, skeletal and cutaneous anomalies. Dermatology 1999; 199: 72-3. PubMed
10. Akiyama M, Aranami A, Sasaki Y et al. Familial linear and whorled nevoid hypermelanosis. J Am Acad Dermatol 1994; 30: 831-3. PubMed
11. Harre J, Millikan LE. Linear and whorled pigmantation. Int J Dermatol 1994; 33: 529-37. PubMed
12. Kubota Y, Shimura Y, Shimada S et al. Linear and whorled nevoid hypermelanosis in a child with chromosomal mosaicism. Int J Dermatol 1992; 31: 345-7. PubMed
13. Lucky AW. Pigmentary abnormalities in genetic disorders. Dermatol Clin 1988; 6: 193-203. PubMed
14. Prendiville JS, Gorski JL, Stein CK et al. Incontinentia pigmenti in a male infant with Klinefelter syndrome. J Am Acad Dermatol 1989; 20: 937-40. PubMed
15. Wollenberg A, Baumann L, Plewig G. Linear atrophoderma of Moulin: a disease which follow Blaschko's lines. Br J Dermatol 1996; 135: 277-9. PubMed
16. Komine M, Hino M, Shiina M et al. Linear and whorled nevoid hypermelanosis: a case with systemic involvement and trisomy 18 mosaicism. Br J Dermatol 2002; 146: 500-2. PubMed
17. Megarbane A, Vabres P, Slaba S et al. Linear and whorled nevoid hypermelanosis with bilateral giant cerebral aneuysms. Am J Med Genet 2002; 112: 95-8. PubMed
18. Cook KK, Cook WR. Chemical peel of nonfacial skin using glycolic acid gel augmented with TCA and neutrolized based on visual staging. Dermatol Surg 2000; 26: 994-9. PubMed
19. Sezer E, Erbil H, Kurumlu Z, Tastan HB, Etikan I. A comparative study of focal medium-depth chemical peel versus cryosurgery for the treatment of solar lentigo. Eur J Dermatol 2007; 17: 26-9. PubMed
© 2007 Dermatology Online Journal