Factitial dermatitis: An unusual presentation in an old woman
Published Web Location
https://doi.org/10.5070/D348v806gpMain Content
Letter: Factitial dermatitis: An unusual presentation in an old woman
Paula Maio MD, Raquel Santos MD, Jorge Cardoso MD
Dermatology Online Journal 18 (4): 10
Dermatology and Venereology department, Hospital de Curry Cabral, Lisbon, PortugalAbstract
The importance of emotional factors in dermatological disorders has been recognized for several decades. However, very few reports have been published to date about the diagnosis and management of these disorders. A 78-year-old woman came to our department with 3 months evolution of a symmetrically distributed dermatosis involving only the face. It was characterized by multiple erosions, some of which had slightly geometrical shapes. We report an unusual case of late onset dermatitis artefacta with a rare successful outcome.
Case report
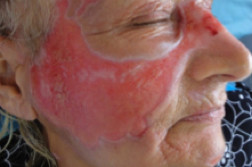 |
| Figure 1 |
|---|
| Figure 1. Clinical presentation of erosions. Geometrical shapes are noted at the inferior border of the lesion (arrow). |
A 78-year-old woman came to our department complaining of a dermatosis involving the periocular and malar regions of her face in a gross symmetrical distribution that was characterized mainly by erosions. The patient couldn’t be precise about the duration of the development of the dermatosis, telling a history of about a three month evolution.
She complained of severe relapsing itch but denied any other somatic symptoms such as pain, fever, mucosal lesions, weight loss, or psychological symptoms such as depression or anxiety.
The physical examination was unremarkable except for the symmetrically distributed skin lesions involving both the periocular and malar regions characterized mainly by erosions, which all seemed to be in the same stage of evolution. In some of them we could observe geometrical shapes (Figure 1). There were no vesicles or bullae, desquamation, or exudate.
A skin biopsy was taken from the border of one of these lesions and the histopathological examination revealed aspects that were suggestive of dermatitis artefacta.
The patient was discharged from the hospital under psychiatric care and she was started on the second-generation antipsychotic risperidone (4 mg/day) and the anxiolytic alprazolam (0.5 mg/day). This therapy together with local wound care allowed the slow regression of the facial lesions.
After the first month of therapy the patient reported that she had no itch or intent to scratch her face. On the third month of therapy we saw the complete healing of the facial lesions with some hypopigmented linear scars.
At one year of clinical follow up there were no further episodes and the patient is still under psychiatric care.
Discussion
Some patients with primary psychiatric disorders tend to seek dermatological attention first because they mistakenly believe that they have a purely skin disorder [1].
The group of factitial disorders refers to the creation (and sometimes the simulation) of physical or psychiatric symptoms. Among the disorders of this broad group dermatitis artefacta syndrome designates the creation of skin lesions unconsciously. The other factitial skin disorder is dermatitis paraartefacta syndrome in which patients act in a semiconscious way [2]. The disorder that refers to a consciously simulated process by which the patient creates skin lesions with the intent of obtaining a personal gain is designated malingering [3, 4].
The dermatitis artefacta represents a rare and difficult dermatological condition with respect to both diagnosis and treatment [4, 5, 6]. It is well known that it is more frequent in the female population with quoted female-to-male ratios ranging from 3:1 to 20:1. The highest incidence of this disorder occurs typically in late adolescence and in early adult life [5, 7].
The patients can use a variety of means besides scratching to cause the clinical visible skin changes and, in some cases, they can be easily mistaken for other dermatological conditions [5, 6]. Often, despite suspicion by the dermatologist, the patient’s denial of any symptoms of psychological distress makes the management and treatment of this particular factitial disorder very difficult.
Except in some mild and transient cases triggered by immediate stress, the prognosis for cure is usually very poor [6, 8, 9, 10].
We report this rare case of late onset dermatitis artefacta with a successful outcome after the correct psychiatric medication was initiated. More research studies are necessary to better document the causes, treatment outcome, and prognosis for this particular group of patients.
References
1. Koblenzer CS. Psychosomatic concepts in Dermatology. Arch Dermatol 1983;119:501-12. [PubMed]2. Humphreys F, Humphreys MS. Psychiatric morbidity and skin disease. What dermatologists think they see? Br J Dermatol. 1998;139:679-81. [PubMed]
3. Millard L. Dermatological practice and psychiatry. Br J Dermatol. 2000;143:920-1. [PubMed]
4. Fabisch W. Psychiatric aspects of dermatitis artefacta. Br J Dermatol. 1980;102:29-34. [PubMed]
5. Spraker MK. Cutaneous artefactual disease: An appeal for help. Pediatr Clin North Am. 1983;30:659-68. [PubMed]
6. Barańska-Rybak W, Cubała WJ, Kozicka D, Sokołowska-Wojdyło M, Nowicki R, Roszkiewicz J. Dermatitis artefacta - a long way from the first clinical symptoms to diagnosis. Psychiatr Danub. 2011 Mar;23(1):73-5. [PubMed]
7. Koblenzer CS. The current management of delusional parasitosis and dermatitis artefacta. Skin Therapy Lett. 2010 Oct;15(9):1-3. [PubMed]
8. Gattu S, Rashid RM, Khachemoune A. Self-induced skin lesions: a review of dermatitis artefacta. Cutis. 2009 Nov;84(5):247-51. [PubMed]
9. Leite RM, Nery NS. Dermatitis simulata: the mystery of the blue girl. Int J Dermatol. 2007 Dec;46(12):1317-9. [PubMed]
10. Jacobi A, Bender A, Hertl M, König A. Bullous cryothermic dermatitis artefacta induced by deodorant spray abuse. J Eur Acad Dermatol Venereol. 2011 Aug;25(8):978-82. [PubMed]
© 2012 Dermatology Online Journal

