Laugier-Hunziker syndrome: A case report and review of the literature
Published Web Location
https://doi.org/10.5070/D3475873ncMain Content
Laugier-Hunziker syndrome: A case report and review of the literature
Sophia Rangwala AB, Christy B Doherty MD, Rajani Katta MD
Dermatology Online Journal 16 (12): 9
Department of Dermatology, Baylor College of Medicine, Houston, Texas. rkatta@bcm.eduAbstract
Laugier-Hunziker syndrome (LHS) is a rare acquired disorder characterized by diffuse macular hyperpigmentation of the oral mucosa and, at times, longitudinal melanonychia. Although LHS is considered a benign disease with no systemic manifestations or malignant potential, it is important to rule out other mucocutaneous pigmentary disorders that do require medical management. Prompt clinical recognition also averts the need for excessive and invasive procedures and treatments. To date, only four cases have been reported in the United States. We present a 77-year-old man who had clinical features typical of LHS and we then provide a review of the literature on LHS and its mimickers.
Case report
 |  |
| Figure 1 | Figure 2 |
|---|---|
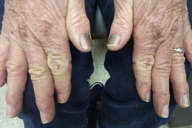
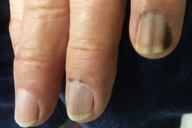
| Figures 1 and 2. Bilateral fingernails showing longitudinal melanonychia and hyperpigmented macules on the proximal nail folds | |
 |
| Figure 3 |
|---|
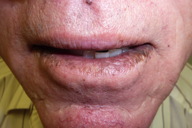
| Figure 3. Upper and lower lips demonstrating confluent brown hyperpigmented macules that extend into the mucosa of the oral commisure |
A 77-year-old non-smoking man with no significant past medical history was referred to our clinic for melanonychia striata on bilateral fingernails and toenails associated with hyperpigmented macules on the proximal nail folds and confluent brown hyperpigmented macules on both lips that extended into the mucosa of the oral commisure. The patient stated that the hyperpigmentation had developed gradually over the last four years and was asymptomatic. The patient denied past skin cancers, heavy metal exposure, or systemic symptoms, such as fatigue, recurring abdominal pain, or gastrointestinal bleeding. Family history was negative for gastrointestinal disease, skin cancer, and unusual oral or cutaneous pigmentation. The only active medication was oral terbinafine 250 mg daily given to him by his primary care physician for six weeks for suspected toenail onychomycosis, tinea pedis, and tinea corporis. Complete blood count, complete metabolic panel, and urinalysis were within normal limits. Upper gastrointestinal endoscopy and colonoscopy were unremarkable. The patient was diagnosed with Laugier-Hunziker syndrome (LHS) based on clinical findings and the lack of systemic involvement.
Discussion
Laugier-Hunziker syndrome was first described in 1970 by Laugier and Hunziker [1]; since then, only about 100 cases have been reported. Laugier-Hunziker syndrome predominates among middle-aged adults with mean onset at 50 years of age [2]. The pathogenesis is unknown and only one familial case has been described [3]. Laugier-Hunziker syndrome appears to be particularly prevalent in French and Italians, but has also been seen in Hispanics, Arabs, and Asians. To date, only four cases have been reported in the United States [4, 5, 6, 7].
The hyperpigmentation associated with LHS occurs spontaneously and gradually, and it is considered permanent [2]. On skin, LHS presents as grey to dark brown lenticular or linear smooth macules that are less than five millimeters in diameter. The lesions most commonly arise on the lips and oral mucosa, especially the lower lip, buccal region, and hard palate [2]. The genitals, fingers, gums, tongue, sclera, perianal region, and esophagus are affected less frequently [2, 8, 9, 10]. About half of patients have pigmented striata of their nails that vary in width and intensity and occur more commonly in the fingernails [11]. At times, the melanonychia is accompanied by pigmentation of the proximal nail fold, termed the pseudo-Hutchinson sign [6, 12]. No systemic effects or malignant predisposition has been recorded in LHS patients.
Past histological studies have demonstrated basal cell hypermelanosis, increased melanophages in the papillary dermis, pigment incontinence, and melanocytes that are normal in number and morphology [3], though one report does describe increased non-nested intraepidermal melanocytes [4]. Ultrastructural studies show increased melanosomes that vary in size and structure [2]. Dermoscopy is a useful noninvasive technique for diagnosis, but data in the literature is limited [13].
Laugier-Hunziker syndrome is a diagnosis of exclusion. If a patient has focal pigmentation, a thorough examination is warranted to rule out melanoma. The differential diagnosis for diffuse mucocutaneous and nail pigmentation includes Peutz-Jegher syndrome (PJS), Bandler syndrome, Cronkhite-Canada syndrome, lichen planus, Addison disease, smoking, drugs, heavy metal exposure, acquired immune deficiency syndrome (AIDS), and idiopathic melanoplakia and melanonychia (Table 1).
Peutz-Jegher syndrome is associated with small brown macules that are particularly concentrated on the lips and oral mucosa, but unlike LHS, the hyperpigmentation appears by early childhood and does not involve the nails. The cutaneous hyperpigmentation fades with puberty, whereas the oral pigmentation persists. Peutz-Jegher syndrome follows an autosomal dominant inheritance pattern secondary to a serine threonine kinase (STK) 11 enzyme defect, is associated with benign intestinal hamartomatous polyposis, and carries an increased risk of developing carcinomas, especially of the genitals, breast, and lung [14].
Bandler syndrome is a rare genodermatosis that presents with hyperpigmented macules in the hands, nails, and oral mucosa during infancy, as well as intestinal vascular malformations that can cause significant gastrointestinal bleeding [15]. Cronkhite-Canada syndrome presents in middle-aged adults and is characterized by mucocutaneous macular hyperpigmentation, alopecia, onychodystrophy, and intestinal hamartomatous polyposis [16]. Albright syndrome exhibits labial and genital pigmentation, but it is often unilateral and does not involve the nails. The disease is also accompanied by precocious puberty in females and fibrous dysplasia. Although neurofibromatosis may display pigmented macules of the lips, there are multiple other skin findings and no known nail changes [7].
Causes of primary adrenocortical insufficiency, such as Addison disease and adrenalectomy, are linked to hyperpigmentation of sun-exposed skin, scars, and mucosa caused by melanocytic hyperfunction stemming from elevated ACTH precursor levels. Like LHS, primary adrenal insufficiency may present as hyperpigmented macules distributed over the oral mucosa and nails, but it is also accompanied by systemic symptoms such as fatigue, weakness, weight loss, hypertension, and bowel changes [17].
Mucocutaneous pigmentation may also be secondary to extrinsic conditions. Smoking may cause mucosal pigmentation of the anterior gingiva but not the skin or nails [18]. Drug-induced oral pigmentation usually occurs after months to years of chronic use and tends to resolve once the drug is discontinued. The most common causative medications are tetracyclines, antimalarials, amiodarone, chemotherapeutics, oral contraceptives, phenothiazines, zidovudine (AZT), clofazimine, and ketoconazole [19]. Systemic exposure to heavy metals such as silver, gold, bismuth, and mercury may also be responsible for mucocutaneous discoloration. In AIDS patients, mucocutaneous and ungual pigmentation may be secondary to systemic drugs (AZT, clofazimine, ketoconazole), adrenal insufficiency, or other unclear causes [20].
Finally, idiopathic melanoplakia and melanonychia should be in the differential diagnosis. Idiopathic buccal melanosis is observed in 5 percent of Caucasians and 38 percent of individuals of African descent [21], but unlike LHS, has its onset during infancy or puberty. Idiopathic longitudinal melanonychia without associated oral macules is normal in 77 percent of blacks by 20 years of age and 90 percent by middle age [22].
Although LHS is a benign condition, patients may choose to have the associated pigmentation removed because of cosmetic disfigurement. A few case studies have demonstrated that cryosurgery, the Nd-YAG laser, and the Q-switched alexandrite laser may be safe and effective options for patients [23, 24, 25, 26]. Recurrence may occur after treatment, but this may be limited by sun avoidance [26].
Conclusion
Laugier-Hunziker syndrome should always be considered in the differential diagnosis of a middle-aged patient presenting with mucocutaneous and ungual hyperpigmentation but no systemic signs or symptoms. By recognizing LHS in the clinical setting, other pigmentary diseases can easily be excluded, and unwarranted tests and procedures can be prevented.
References
1. Laugier P, Hunziker N. Essential lenticular melanic pigmentation of the lip and cheek mucosa. Arch Belg Dermatol Syphiligr 1970;26:391-9. [PubMed]2. Veraldi S, Cavicchini S, Benelli C, Gasparini G. Laugier-Hunziker syndrome: a clinical, histopathologic, and ultrastructural study of four cases and review of the literature. J Am Acad Dermatol 1991;25:632-6. [PubMed]
3. Makhoul EN, Ayoub NM, Helou JF, Abadjian GA. Familial Laugier-Hunziker syndrome. J Am Acad Dermatol 2003;49:S143-5. [PubMed]
4. Moore RT, Chae KA, Rhodes AR. Laugier and Hunziker pigmentation: a lentiginous proliferation of melanocytes. J Am Acad Dermatol 2004;50:S70-4. [PubMed]
5. Mowad CM, Shrager J, Elenitsas R. Oral pigmentation representing Laugier-Hunziker syndrome. Cutis 1997;60:37-9. [PubMed]
6. Sterling GB, Libow LF, Grossman ME. Pigmented nail streaks may indicate Laugier-Hunziker syndrome. Cutis 1988;42:325-6. [PubMed]
7. Koch SE, LeBoit PE, Odom RB. Laugier-Hunziker syndrome. J Am Acad Dermatol 1987;16:431-4. [PubMed]
8. Lenane P, Sullivan DO, Keane CO, Loughlint SO. The Laugier-Hunziker syndrome. J Eur Acad Dermatol Venereol 2001;15:574-7. [PubMed]
9. Gerbig AW, Hunziker T. Idiopathic lenticular mucocutaneous pigmentation or Laugier-Hunziker syndrome with atypical features. Arch Dermatol 1996;132:844-5. [PubMed]
10. Yamamoto O, Yoshinaga K, Asahi M, Murata I. A Laugier-Hunziker syndrome associated with esophageal melanocytosis. Dermatology 1999;199:162-4. [PubMed]
11. Baran R. Longitudinal melanotic streaks as a clue to Laugier-Hunziker syndrome. Arch Dermatol 1979;115:1448-9. [PubMed]
12. Porneuf M, Dandurand M. Pseudo-melanoma revealing Laugier-Hunziker syndrome. Int J Dermatol 1997;36:138-41. [PubMed]
13. Tamiya H, Kamo R, Sowa J, Haruta Y, Tanaka M, Ishii M, Kobayashi H. Dermoscopic features of pigmentation in Laugier-Hunziker-Baran syndrome. Dermatol Surg 2010;36:152-4. [PubMed]
14. Beggs AD, Latchford AR, Vasen HF, Moslein G, Alonso A, Aretz S, Bertario L, Blanco I, Bülow S, Burn J, Capella G, Colas C, Friedl W, Møller P, Hes FJ, Järvinen H, Mecklin JP, Nagengast FM, Parc Y, Phillips RK, Hyer W, Ponz de Leon M, Renkonen-Sinisalo L, Sampson JR, Stormorken A, Tejpar S, Thomas HJ, Wijnen JT, Clark SK, Hodgson SV. Peutz-Jeghers syndrome: a systematic review and recommendations for management. Gut 2010;59:975-86. [PubMed]
15. Bandler M. Hemangiomas of the small intestine associated with mucocutaneous pigmentation. Gastroenterology 1960;38:641-5. [PubMed]
16. Cronkhite LW, Canada WJ. Generalized gastrointestinal polyposis; an unusual syndrome of polyposis, pigmentation, alopecia and onychotrophia. N Engl J Med 1955;252:1011-5. [PubMed]
17. Yesudian PD, Mendelsohn S, Rutter MK. Primary adrenocortical insufficiency masquerading as Laugier-Hunziker syndrome. Int J Dermatol 2008;47:596-8. [PubMed]
18. Siponen M, Salo T. Idiopathic lenticular mucocutaneous pigmentation (Laugier-Hunziker syndrome): a report of a case. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2003;96:288-92. [PubMed]
19. Dereure O. Drug-induced skin pigmentation. Epidemiology, diagnosis and treatment. Am J Clin Dermatol 2001;2:253-62. [PubMed]
20. Cohen LM, Callen JP. Oral and labial melanotic macules in a patient infected with human immunodeficiency virus. J Am Acad Dermatol 1992;26:653-4. [PubMed]
21. Fry L, Almeyda JR. The incidence of buccal pigmentation in caucasoids and negroids in Britain. Br J Dermatol 1968;80:244-7. [PubMed]
22. Baran R, Kechijian P. Longitudinal melanonychia (melanonychia striata): Diagnosis and management. Journal of the American Academy of Dermatology 1989;21:1165-75. [PubMed]
23. Ferreira MJ, Ferreira AM, Soares AP, Rodrigues JC. Laugier-Hunziker syndrome: case report and treatment with the Q-switched Nd-Yag laser. J Eur Acad Dermatol Venereol 1999;12:171-3. [PubMed]
24. Sheridan AT, Dawber RP. Laugier-Hunziker syndrome: treatment with cryosurgery. J Eur Acad Dermatol Venereol 1999;13:146-8. [PubMed]
25. Zuo YG, Ma DL, Jin HZ, Liu YH, Wang HW, Sun QN. Treatment of Laugier-Hunziker syndrome with the Q-switched alexandrite laser in 22 Chinese patients. Arch Dermatol Res 2010;302:125-30. [PubMed]
26. Papadavid E, Walker NP. Q-switched Alexandrite laser in the treatment of pigmented macules in Laugier-Hunziker syndrome. J Eur Acad Dermatol Venereol 2001;15:468-9. [PubMed]
© 2010 Dermatology Online Journal

