Contact urticaria to raw potato
Published Web Location
https://doi.org/10.5070/D340v7642pMain Content
Contact urticaria to raw potato
Z Martínez de Lagrán, FJ Ortiz de Frutos, M González de Arribas, F Vanaclocha-Sebastián
Dermatology Online Journal 15 (5): 14
Department of Dermatology, Hospital 12 de Octubre, Madrid, Spain. zurine.martinezdelagranalvarezdearcaya@osakidetza.netAbstract
Although potatoes represent a large part of diets worldwide, adverse reactions to them are considered uncommon and usually result from ingestion, mainly in children. In contrast, immediate reactions to contact with raw potato has been reported more frequently in adults, usually in the form of an oral contact dermatitis or contact urticaria, but also may manifest as asthma, rhinoconjunctivitis, wheezing or even anaphylaxis. We report a case of non-occupational allergic contact urticaria caused by raw potato, which we then documented by prick testing.
Adverse reactions to food can occur through ingestion, inhalation, and mucous membrane or skin contact [1]. This latter route has been described in occupational and non-occupational settings and may manifest as irritant contact dermatitis (the most common one), allergic contact dermatitis, or contact urticaria (CU) [1]. Adverse reactions from contact with potatoes are uncommon. We report a case of non-occupational allergic CU caused by raw potato, rarely described in the literature, and document this with prick testing [2, 3, 4, 5, 6].
A 41-year-old woman presented to our department because of pruritic lesions that developed upon areas subjected to friction in both hands (more intense in the right one). These had appeared when she began to work storing books in a factory. We initially considered the lesions to be irritant contact dermatitis.
The patient also, complained about pruritus and described papulo-vesicular eruptions on the hands immediately after skin contact with raw potatoes, which resolved 20-30 minutes after ceasing contact. There were no late reactions nor worsening of the pre-existing eczema. The lesions were restricted to the contact areas with potatoes. No systemic symptoms were recorded. Ingestion and contact with cooked or processed potatoes induced no reaction. The patient described no problems with latex gloves, other topical products, or other foods.
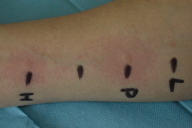 |
| Figure 1 |
|---|
| Figure 1. Positive results to raw potato (P) and positive control (histamine, H) in prick by prick. The test with latex (L) and physiologic saline are negative. |
Patch testing to the European standard, standard additional series, and pieces of raw potato was negative. A prick-test using a commercial latex antigen was also negative. Finally, a prick-by-prick test with raw potato, showed a positive result after 20 minutes, supporting the diagnosis of CU (Fig. 1).
The term contact urticaria (CU) was introduced by A.A. Fisher in 1973 and refers to whealing, erythema, and pruritus appearing within minutes after cutaneous or mucosal contact with the causative agent and clearing completely within a maximum of 24 hours [7]. It is usually limited to the contact areas, but it may present at distant sites or as generalized urticaria. Internal organs can be involved and the reaction can even culminate in anaphylactic shock. The degree of severity has been classified under the term, contact urticaria syndrome, in which 4 states have been described: 1 (localized urticaria, itching or burning), 2 (generalized urticaria), 3 (rhinoconjuntivitis, asthma or gastrointestinal symptoms) and 4 (anaphylaxis). Pre-existing dermatosis, such as irritant contact dermatitis facilitate the development of CU, probably through increasing penetration of offending substances [7].
Three types of CU have been described: non-immunologic CU, immunologic CU and CU of uncertain mechanisms. In the immunologic/allergic one, a type I hypersensitivity reaction mediated by allergen-specific IgE is implicated [7].
The paradigm for IgE-related CU is natural rubber latex allergy. Foods, mainly raw fruits and vegetables, are the next commonest cause [7]. There are a few cases of CU owing to raw potato reported in the literature [2, 3, 4, 5, 6].
Serologic assays for measurement of specific IgE titres (e.g. RAST) and in vivo skin prick tests performed with the suspected substance using commercial reagents or the natural product can help to confirm the diagnosis of allergic CU. The "prick-by-prick" or double puncture technique, consists of piercing the natural food with the lancet immediately before puncturing the patient's skin, usually on the volar aspect of the forearm, with the same lancet [8]. Histamine is used as a positive control and physiologic saline as a negative one. The results are evaluated at 15-20 minutes and graded according to the diameter of the wheal. A reaction is considered to be positive when the diameter is at least 3 mm more than the negative control. This test is very useful when testing a product for which commercial allergens are not available; it avoids the possible alteration of the processed allergens, especially if they are labile.
The term "protein contact dermatitis" (PCP) was introduced in 1976 to describe a particular form of contact dermatitis to food proteins [9]. Clinically, it is a chronic and recurrent eczema, usually affecting the hands and forearms. Exacerbations may be in the form of pruritus, urticaria, or vesicular lesions noted rapidly after contact with the causal agent. In contrast to contact urticaria, the pre-existing eczema often worsens after the resolution of the exacerbations. Patients with PCP usually show a positive prick test. However, although the clinical picture and biopsy findings are consistent with eczema, patch testing is generally negative. The underlying mechanism of PCP is perhaps a combination of immediate (type I) and delayed (type IV) hypersensitivity reactions, together with an irritant component. Differentiating this from CU is sometimes difficult. In fact, some authors consider that repeated episodes of CU can result in the development of a PCP. In our case, the fact that the urticarial reactions resolve completely without residual signs or worsening of the previous hand dermatitis supports the diagnosis of CU.
Until now, four potato allergens have been identified. The glycoprotein "patatin" (Sol-t-1) is the most important one [10] and shows a significant homology with a latex allergen, leading to the possibility of cross-reaction [11].
The existence of heat-labile potato proteins (unstable in the presence of digestive enzymes and gastric acid) that lose their allergenic properties when cooked or eaten, explains why some subjects show symptoms only after contact with raw potatoes and not with processed potatoes or after oral intake [12].
Allergic CU to potato is a well known but uncommon entity. We report a typical case confirmed by a positive result in the prick-by-prick test.
References
1. Bahna SL. Adverse food reactions by skin contact. Allergy 2004;59:66-70. [PubMed]2. Larkò O, Lindstedt G, Lundberg PA, Mobacken H. Biochemical and clinical studies in a case of contact urticaria to potato. Contact Dermatitis. 1983;9(2):108-14. [PubMed]
3. Carmichael AJ, Foulds IS, Tan CY. Allergic contact dermatitis from potato flesh. Contact Dermatitis 1989;20:64Ð65. [PubMed]
4. Jeannet-Peter N, Piletta-Zanin PA, Hauser C. Facial dermatitis, contact urticaria, rhinoconjuntivitis, and asthma induced by potato. Am J Contact Dermat.1999;10(1):40-2. [PubMed]
5. Gómez-Torrijos E, Galindo PA, Borja J et al. Allergic contact urticaria from raw potato. J Investig Allergol Clin Immunol 2001;11(2):129. [PubMed]
6. Delgado J, Castillo R, Quiralte J et al. Contact urticaria in a child from raw potato. Contact Dermatitis 1996;35(3):179-80. [PubMed]
7. Wakelin SH. Contact urticaria. Clin Exp Dermatol 2001;26(2):132-6. [PubMed]
8. Lachapelle JM, Maibach HI, Ring J, Darsow U, Rustemeyer T. Patch testing and prick testing. 2nd Ed. Springer Berlin Heidelberg. 2009.
9. Hjorth N, Roed-Petersen J. Occupational protein contact dermatitis in food handlers. Contact Dermatitis 1976; 2: 28Ð 42. [PubMed]
10. Seppälä U, Majamaa H, Turjanmaa K, et al. Identification of four novel potato (Solanum tuberosum) allergens belonging to the family of soybean trypsin inhibitors. Allergy 2001;56(7):619-26. [PubMed]
11. Schmidt MH, Raulf-Heimsoth M, Posch A. Evaluation of patatin as a major cross reactive allergen in latex-induced potato allergy. Ann Allergy Asthma Immunol 2002;89(6):613-8. [PubMed]
12. De Swert LF, Cadot P, Ceuppens JL. Diagnosis and natural course of allergy to cooked potatoes in children. Allergy 2007;62(7):750-7. [PubMed]
© 2009 Dermatology Online Journal

