Cutaneous mixed tumor with extensive chondroid metaplasia: a potential mimic of cutaneous chondroma
Published Web Location
https://doi.org/10.5070/D33zx859ddMain Content
Cutaneous mixed tumor with extensive chondroid metaplasia: a potential mimic of cutaneous chondroma
Jennifer Thompson BS, Stephen Squires MD, Mac Machan MD, Garth R Fraga MD, Daniel Aires MD
Dermatology Online Journal 18 (3): 9
University of Kansas Medical Center, Kansas City, KansasAbstract
True cutaneous chondromas are extremely rare. Previously they have reportedly been confused with soft tissue chondromas and cartilaginous developmental anomalies. Monophasic mixed tumor could potentially also be mistakenly diagnosed as a true cutaneous chondroma. We report a cutaneous mixed tumor with massive chondroid metaplasia that mimicked a true cutaneous chondroma. We also propose that cutaneous mixed tumor with chondroid metaplasia may better explain the presence of primary cartilaginous tumors in the skin and true cutaneous chondroma may not be a real entity.
History and physical examination
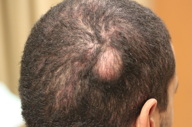
A 29-year-old male presented with a one-year history of an asymptomatic progressively enlarging mass on the right posterior scalp. He reported it began after he bumped his head at work. Exam revealed a 3.1 x 2.5 cm firm, subcutaneous nodule with no epidermal changes. The growth was excised. Clinical differential diagnoses included proliferating pilar cyst, pilomatricoma, and pilomatrical carcinoma.
 |  |
| Figure 1 | Figure 2 |
|---|---|
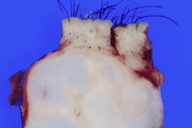
| Figure 1. Scalp mass Figure 2. A cross section through the excisional specimen demonstrates a subcutaneous tumor comprised of translucent grey nodules subdivided by fibrous bands | |
Histopathology
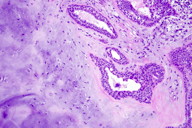
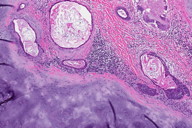
Gross examination showed a circumscribed, nonencapsulated subcutaneous nodule consisting of gelatinous grey-blue lobules separated by yellow-white fibrous bands. A representative section was submitted for histopathologic examination. It demonstrated abundant hyaline cartilage with mature chondrocytes. Rare epithelial glandular structures were identified, prompting submission of the remainder of the neoplasm for histopathologic examination. Additional sections demonstrated branching tubules lined by a double cell layer exhibiting apocrine decapitation secretion and follicular differentiation in the form of shadow cells, trichohyalin granules, and follicular germs. The tumor was diagnosed as a benign cutaneous mixed tumor with follicular and apocrine differentiation and marked chondroid metaplasia of the stroma.
 |  |
| Figure 3 | Figure 4 |
|---|---|
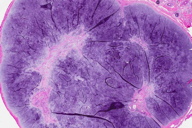
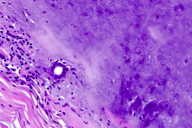
| Figure 3. Initial sections reveal a solid cartilaginous nodule (H&E, x6) Figure 4. A small tubule located at the edge of the tumor in the initial section (H&E, x400) | |
Discussion
Mixed tumors consist of commingled epithelial and mesenchymal components. Initially described in salivary glands by Billroth, they were first reported in the skin by Nasse [1, 2]. In 1961 Hirsch and Helwig suggested the term “chondroid syringoma” to distinguish mixed tumors of the skin from mixed tumors of other organs [3]. Headington subsequently recognized apocrine and eccrine subtypes [4]. Cutaneous mixed tumors (CMT) can form a chondroid stroma comprised of sulfated acid mucopolysaccharides with abundant hydroxyproline and proline similar to costal cartilage [3]. Chondroid metaplasia may be extensive, particularly in CMT of the scalp [3]. Hsueh and Santa Cruz presciently suggested that the rare chondroma of the skin might relate to overgrowth of the cartilaginous stroma in a CMT [5]. We describe a case with such extensive chondroid metaplasia that true cutaneous chondroma was initially suspected until additional tumor sampling revealed more obvious epithelial elements of CMT.
True cutaneous chondromas are exceedingly rare; only ten cases have been reported to date and some of the reported cases appear to overlap with other entities. True cutaneous chondroma is a diagnosis of exclusion. The differential diagnosis includes soft tissue chondromas and cartilage-forming cutaneous anomalies such as Meckel cartilage, accessory tragi, bronchogenic cysts and dermoid cysts [5-10]. Although extensive fibrous, osseous, and lipomatous metaplasia has been described in CMT, it is not usually included in the differential. We are unaware of any previously published photographic documentation of CMT with extensive chondroid metaplasia that might be mistaken for true cutaneous chondroma [12, 13, 14, 15]. Our case highlights the potential for misdiagnosis of CMT as true cutaneous chondroma.
Developmental anomalies and soft tissue chondromas account for most cartilage-forming skin tumors [5]. Developmental hamartomas can usually be excluded by congenital history and characteristic locations. Soft tissue chondromas are cartilage-forming tumors with a marked predilection for the hands and feet. Some authors have proposed synovial origin. They may exhibit cytologically atypical features such as pleomorphic nuclei, multinucleation, and macronucleoli, but behave as benign neoplasms. The atypical cytology of soft tissue chondroma led some authors in the past to promote the descriptive diagnosis “cartilaginous tumor” to highlight the lack of consensus on behavior. Soft tissue chondroma is currently accepted as benign, but the term “cartilaginous tumor” endures [16]. Hsueh and Santa Cruz provided a classification of cutaneous cartilaginous proliferations that is still applicable today. They suggested that chondroid syringoma might be largely cartilaginous and provoke difficulty in the differential with chondroma.
A CMT is a cutaneous neoplasm. Classification of such cutaneous neoplasms is based on differentiation, which tends to recapitulate the developmental potential of the cell of origin. The corium does not contain any structures that normally form cartilage. Hence, we question the existence of true cutaneous chondroma. In our opinion, chondroid metaplasia, as in our case of CMT, is a simpler explanation for those rare cutaneous cartilage-forming tumors that do not appear to be either developmental anomalies or soft tissue chondromas.
References
1. Billroth T. Beobachtungen uber geschwulste der speicheldrusen. Virchows Arch Pathol Anat. 1859;17:357-75.2. Nasse, D. Die geschewulste der speicheldrusen und verwandt tumoren des kopfes. Arch Klin Chir. 1892;44:233-302.
3. Hirsch P, Helwig EB. Chondroid syringoma. Mixed tumour of skin, salivary gland type. Arch Dermatol 1961;84:835-47. [PubMed]
4. Headington JT. Mixed tumors of skin: eccrine and apocrine types. Arch Dermatol. 1961;84:989-96. [PubMed]
5. Hsueh S, Santa Cruz DJ. Cartilaginous lesions of the skin and superficial soft tissue. J Cutan Pathol. 1982:9:405-16. [PubMed]
6. Holmes HS, Bovenmeyer DA. Cutaneous cartilaginous tumor. Arch Dermatol. 1976;112: 839-40. [PubMed]
7. Humphreys TR, Herzberg AJ, Elenitsas R, et al. Familial occurrence of multiple cutaneous chondromas. Am J Dermatopathol. 1994;16:56-9. [PubMed]
8. Shinojima Y, Hara H, Shimojima H, Terui T. Cutaneous chondroma with overlying pigmentation clinically mimicking dermatofibroma. Br J Dermatol. 2006;154:178-81. [PubMed]
9. Sarma DP, Chen M, Wang B. Chondroma cutis. Internet Journal of Dermatology. 2007; 6(1).
10. Kim HS, Choi KH, Kim HO, et al. A true chondroma cutis. J Eur Acad Dermatol Venereol. 2009;23(5):612-3. [PubMed]
11. Dahlin DC, Salvador AH. Cartilaginous tumor of soft tissues of the hands and feet. Mayo Clin Proc. 1974;49:721-25.
12. Kazakov D, Belousova I, Bisceglia M, et al. Apocrine mixed tumor of the skin (“mixed tumor of the folliculosebaceous-apocrine complex”). J Am Acad Dermatol. 2007;57(3):467-83. [PubMed]
13. Shimizu S, Han-Yaku H, Fukushima S, et al. Immunohistochemical study of mixed tumour of the skin with marked ossification. Dermatol. 1996;193:255-57. [PubMed]
14. Miracco C, De Santi MM, Lalinga AV, et al. Lipomatous mixed tumour of the skin : a histological, immunohistochemical, and ultrastructural study. Br J Dermatol. 2002;146:899-903. [PubMed]
15. Awasthi R, Harmse D, Courtney D, et al. Benign mixed tumour of the skin with extensive ossification and marrow formation : a case report. J Clin Pathol 2004;57:1329-30. [PubMed]
16. Ramirez-Barcena P, Rodriguez-Castellanos MA, Fajardo-Barajas D, Sandoval-Tress C. Cutaneous cartilaginous tumor. Dermatolo Surg. 2006;32:1513-15. [PubMed]
© 2012 Dermatology Online Journal