Mycobacterium marinum infection
Published Web Location
https://doi.org/10.5070/D33v9748jhMain Content
Mycobacterium marinum infection
Hien Tran MD PhD, Hideko Kamino MD, Ruth F Walters MD
Dermatology Online Journal 14 (10): 7
Department of Dermatology, New York UniversityAbstract
A 64-year-old man presented for evaluation of tender pustules that developed on his right hand and subsequently spread up his arms in a sporotrichoid manner. Owing to the prominent history of recent trauma followed by fish tank exposure, the patient was started on doxycycline for coverage of Mycobacterium marinum. Subsequent tissue culture grew M. marinum and confirmed the clinical diagnosis. M. marinum is an atypical mycobacteria that is ubiquitously found in aquatic environments. Owing to its optimal growth temperature of 25 to 35oC, infections in humans are mostly restricted to the skin. Furthermore, the organism can spread by lymphatic drainage leading to the clinical appearance of sporotrichoid lesions. The preferred treatment for M. marinum is doxycycline, which was started in our patient and has subsequently improved his clinical condition.
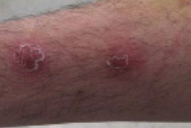 | 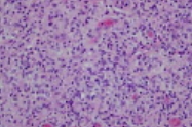 |
| Figure 1 | Figure 2 |
|---|
History
A 64-year-old man with a past medical history of Parkinson diease, depression, macular scars within the retina, and gastroesophageal reflux disease presented to the Veterans Administration New York harbor Healthcare System for evaluation of tender pustules that developed on his right hand and subsequently developed on his arms over the course of three weeks. The lesions were painful and tender. The patient lives in a monastery and denied any gardening work or recent exposure to thorny bushes. He described recent trauma to his right thumb with subsequent exposure to a fish tank that he frequently cleans. His medications included augmentin, clarithromycin, wellbutrin, clonazepam, paroxetine, mirapex, and trazodone. He had no known drug allergies.
Physical Examination
The right thumb had a punctum at the tip. There were four erythematous nodules with overlying scales in a linear array from the thumb to his forearm with overlying desquamation and erythema. On the right medial forearm and the inner upper arm were three dermal nodules without overlying skin changes. All nodules were tender to palpation. A purulent discharge was noted when a biopsy was performed.
Lab
Tissue culture grew Mycobacterium marinum after three weeks. Smear of exudate from a biopsy specimen showed no acid-fast bacilli.
Histopathology
In the reticular dermis and superficial subcutaneous tissue, there is a multinodular infiltrate of histiocytes and numerous neutrophils that are surrounded by lymphocytes and scattered plasma cells and eosinophils. Periodic acid-Schiff, Gomori methenamine silver, and acid-fast stains fail to show fungi and acid-fast bacilli.
Comment
Mycobacterium marinum is an atypical mycobacteria that is ubiquitously found in aquatic environments. It is prevalent worldwide in saltwater and freshwater in a wide geographic distribution. M. marinum is adapted to infecting ectotherms and therefore has an optimal growth temperature between 25°C to 35°C [1]. It can infect many different aquatic animals, which include fish, frogs, eels, and oysters, and also has been found in aquatic mammals such as dolphins and manatees.[2] Rarely, however, M. marinum can infect humans with an annual incidence in the US of 0.27 confirmed cases per 100,000 people [3]. Owing to its optimal growth temperature, M. marinum infection in humans is mostly restricted to the skin. However, in immunocompromised individuals, the organisms can disseminate and cause pulmonary and visceral infections [1].
M. marinum infection was originally known as swimming pool granuloma after a large outbreak occurred that was traced back to swimming pools. Subsequent to widespread use of chlorine, the majority of cases were found in fisherman and aquarium owners and led to the term fish tank granuloma [4]. The clinical history that often precedes such an infection involves recent trauma followed by exposure to water or handling of fish or shellfish. The infection clinically presents as papulo-nodular, verrucous, or ulcerated granulomatous inflammation, usually with minimal purulent discharge [2, 5]. Sporotrichoid lesions can be observed as the organism spreads by lymphatic drainage from the primary lesion and creates a chain of granulomatous, inflamed, pustular lesions. Rarely, M. marinum may cause deeper infections leading to tenosynovitis that can progress to septic arthritis and osteomyelitis [2, 6].
The presence of sporotrichoid lesions has a limited differential of disease entities. Among the possible disease entities that may cause sporotrichoid spread include deep fungal infections, sporotrichosis, cutaneous leishmaniasis, nocardiosis, pyogenic bacteria, cat scratch disease, other mycobacterial species, and tularemia [2, 4, 5]. Cultures from secretions and biopsies may often lead to the diagnosis. A tissue biopsy specimen may show acid-fast bacilli in some cases, but this is only true in a minority of cases. The organism normally serves as a complementary finding, and the biopsy specimen usually shows granulomatous inflammation [2].
In the case of our patient, history played a prominent role in determining the diagnosis. Owing to our high clinical suspicion of M. marinum infection, the patient was started on doxycycline at his initial visit. Tissue culture, a biopsy specimen, and a smear of the purulent matter that exuded from the biopsy site were sent for laboratory diagnosis. Although the smear and biopsy specimen were negative for acid-fast bacilli, the diagnosis was confirmed by a tissue culture that grew M. marinum.
Doxycycline is considered the preferred treatment for M. marinum, but a number of other antibiotic regimens exist [2, 5]. Clarithromycin with or without ethambutol also may be considered as an alternative treatment option [7]. For more invasive infections, the combination of rifampin with ethambutol has been advocated [8]. In some cases, surgical debridement and/or excision is required if deep structures are involved [9]. In general, therapy should be continued for at least two to three weeks after all lesions have resolved [10].
References
1. Stamm LM, Brown EJ. Mycobacterium marinum: the generalization and specialization of a pathogenic mycobacterium. Microbes Infect 2004; 6: 1418 PubMed2. Petrini B. Mycobacterium marinum: ubiquitous agent of waterborne granulomatous skin infections. Eur J Clin Microbiol Infect Dis 2006; 25: 609 PubMed
3. Sciacca-Kirby J, et al. Mycobacterium marinum infection of the skin. http//:emedicine.com/derm/topic281.htm. Cited 8 Feb 2006
4. Johnson RP, et al. Mycobacterium marinum infection: a case report and review of the literature. Cutis 2007; 79: 33 PubMed
5. Ramos-e-Silva M, Ribero de Castro MC. Mycobacterial infections In: Dermatology, edited by Bolognia, JL, et al. eds. Mosby; London 2003: 1159
6. Barton A, et al. Mycobacterium marinum infection causing septic arthritis and osteomyelitis. Br J Rheumatol 1997; 36: 1207 PubMed
7. American Thoracic Society. Diagnosis and treatment of disease caused by nontuberculous mycobacteria. Am J Respir Crit Care Med 1997; 156: 1 PubMed
8. Lewis FM, et al. Fish tank exposure and cutaneous infections due to Mycobacterium marinum: tuberculin skin testing, treatment, and prevention. Clin Infect Dis 2003; 37: 390 PubMed
9. Hess CL, et al. Mycobacterium marinum infections of the upper extremity. Plast Reconstr Surg 2005; 115: 55 PubMed
10. Donta ST, et al. Therapy of Mycobacterium marinum infections: use of tetracyclines vs. rifampicin. Arch Intern Med 1986; 146: 902 PubMed
© 2008 Dermatology Online Journal

