Bullous morphea
Published Web Location
https://doi.org/10.5070/D33r74n91zMain Content
Bullous morphea
Thomas C. Gallagher
Dermatology Online Journal 8(2): 11
From New York University Department of DermatologyHistory
This 81-year-old woman complained of a problem involving her lowerabdomen, lateral and anterior thighs, inguinal folds, intergluteal cleft, and popliteal fossae. Five years ago, the patient developed an indurated plaque on the left anterior thigh. The lesion slowly enlarged, and new plaques gradually appeared. She has noted progressive difficulty walking as the plaques have spread. Approximately six months ago, she first noted the vesicles and bullae in the abdominal and thigh plaques. Previous treatments have included medium and high potentcy topical glucocorticoids with miminal improvement. UVA phototherapy will be initiated.
Physical Examination
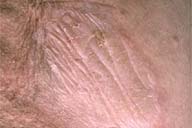 | 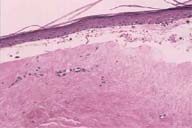 |
| Figure 1 | Figure 2 |
|---|
Multiple, hypopigmented, indurated plaques with scale were noted. There were several vesicles and bullae overlying the hypopigmented plaques of the abdomen and thigh.
Laboratory Data
An antinuclear antibody test was negative.
Histopathology
There is dermal sclerosis, a sparse perivascular infiltrate, papillary dermal edema, and a focal subepidermal blister. No adnexal structures are present. A direct immunofluorescence test shows no abnormal epidermal, basement-membrane zone, or vascular deposits of IgG, C3, IgM, IgA, or fibrin.
Comment
Bullous morphea is a rare disease, which occurs most commonly on the lower extremities and inferior abdomen. Fewer than 100 cases have been reported in the world literature.
While the etiology of bullous formation is not certain, lymphatic obstruction from the sclerodermatous process is considered the likeliest cause. Pautrier also suggested that vascular changes like arteritis and phlebosclerosis play a role in bullae formation. This hypothesis gains credence from the hemorrhagic nature of many morphea bullae. O'Leary found a correlation between local trauma and blister formation. Daoud, et al, found the eosinophil granule component major basic protein (MBP) in the base of morphea blisters. They concluded that major basic protein is responsible for blister formation in at least some cases of morphea.
Treatment of bullous morphea is unsatisfactory. A letter to Clin Exp Dermatol suggested that salazopyrin has some efficacy. Daoud, et al, found variable success with hydroxychloroquine. Broad-band low-dose UVA phototherapy and UVA1 phototherapy have efficacy in morphea. It is likely that bullous morphea would show a similar response as multiple authors have concluded that morphea and bullous morphea are distinct manifestations of the same disease.
References
Synkowski DR, et al. Bullous scleroderma. Arch Dermatol 117:135, 1981Su WP, Greene SL. Bullous morphea profunda. Am J Dermatopathol 8:144, 1986
Tosti A, et al. Hemorrhagic bullous lesions in morphea. Cutis 44:118, 1989
Daoud MS, et al. Bullous morphea: clinical, pathologic, and immunopathologic evaluation of 13 cases. J Am Acad Dermatol 30:937, 1994
Trattner A, et al. Bullous morphea: a distinct entity? Am J Dermatopathol 16:414, 1994
Micalizzi C, et al. Generalized bullous morphea. Efficacy of salazopyrin. Clin Exp Dermatol 21:246, 1996
Kerscher M, et al. Low dose UVA1 phototherapy for treatment of localized scleroderma. J Am Acad Dermatol 38:21, 1998
De Rie MA, Bos JD. Photochemotherapy for systemic and localized scleroderma. J Am Acad Dermatol 43:725, 2000
El-Mofty M. et al. Low-dose broad-band UVA in morphea using a new method for evaluation. Photodermatol Photoimmunol Photomed 16:43, 2000
© 2002 Dermatology Online Journal

