Annular lichen planus in association with Crohn disease
Published Web Location
https://doi.org/10.5070/D33qv3q0gbMain Content
Annular lichen planus in association with Crohn disease
Vasco Vieira Serrão MD1, Vasili Organ MD2, Luís Pereira MD2, Esmeralda Vale MD3, Suzete Correia MD3
Dermatology Online Journal 14 (9): 5
1. Dermatology Department, Hospital dos Capuchos, Lisbon, Portugal. vvsferreira@netcabo.pt2. Internal Medicine Department, Hospital de São José, Lisbon, Portugal
3. Dermatology Department, Centro de Dermatologia Médico-Cirúrgica de Lisboa, Lisbon, Portugal
Abstract
Background: Lichen planus is an idiopathic inflammatory disease of the skin and mucous membranes. Although the etiology is not established, it has been associated with autoimmune diseases, viral infections, drugs and dental restoration materials. However, the association with inflammatory bowel disease has been very rarely reported in the literature. Case Report: A 19-year-old female patient presented with annular lesions on her upper body and limbs, with a sharply defined border and non-atrophic skin in the center. The lesions were hyperpigmented and had been stable for over one year. The histopathology confirmed the diagnosis of annular lichen planus. She had weight loss, occasional diarrhea, and a severe anemia. The investigation of these symptoms led to the diagnosis of Crohn disease and a sickle cell trait. Therapy with systemic corticosteroids and mesalazine controlled the intestinal disease, with concomitant improvement of the skin lesions. Conclusions: As lichen planus can be associated with other immunological disorders, the association with inflammatory bowel disease should be considered in the evaluation of the patient.
Introduction
Lichen planus (LP) is an idiopathic inflammatory disease that can present with both skin and mucosal involvement [1]. It is considered an autoimmune disease mediated by CD8+ T cells, against basal keratinocytes that express modified epitopes [2, 3]. This can be the result of viral infection or vaccination, drugs, contact allergens and rarely underlying neoplasms [4, 5, 6, 7]. Annular LP is a rare variant affecting about 10 percent of patients and tends to have a chronic evolution [8]. Inflammatory bowel disease (IBD) can have many skin manifestations, but there are very few reports showing association with lichen planus [9, 10].
Case report
 |  |
| Figure 1 | Figure 2 |
|---|---|
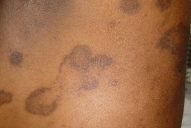
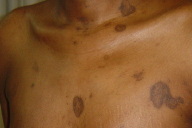
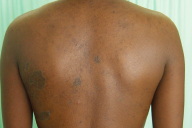
| Figure 1. Multiple annular asymptomatic lesions Figure 2. Annular lesions on the back, with sharply defined borders | |
A 19-year-old female patient, presented with multiple annular lesions for more than a year.
 |  |
| Figure 3 | Figure 4 |
|---|---|
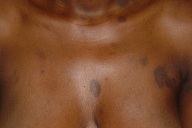
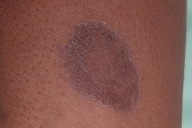
| Figure 3. Detail of a lesion on the back, showing the slightly elevated border Figure 4. Lesion on the arm, with non-scaling elevated border and central hyperpigmentation | |
The lesions presented with non-atrophic, hyperpigmented central areas and non-scaling, slightly elevated borders. Twenty-three annular lesions were present, ranging from 2 to 8cm in diameter. They appeared simultaneously, had initial centrifugal growth, and remained stable for one year despite the use of topical antifungal therapy and emollients. The patient denied the use of any systemic medication prior to the appearance of the skin lesions.
 |  |
| Figure 5 | Figure 6 |
|---|---|
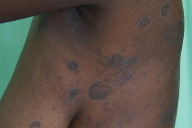
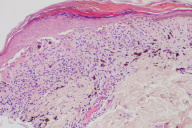
| Figure 5. Annular lichen planus, multiple lesions Figure 6. Annular lichen planus, showing characteristic histological changes on the elevated lesion border (H&E, x100) | |
The plaques were mostly on the trunk and upper limbs and although they were initially pruritic they were otherwise asymptomatic. No mucosal, genital, or nail changes were observed.
The histopathological examination of the lesion border revealed focal hyperkeratosis, epidermal hyperplasia, and wedge-shaped hypergranulosis. A band-like lichenoid lymphocytic inflammatory infiltrate was present with numerous melanophages. Cytoid bodies and subepidermal clefting (Max-Joseph spaces) could also be seen.
 |
| Figure 7 |
|---|
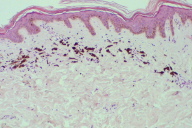
| Figure 7. Biopsy from the center of the lesion with post-inflammatory changes such as scarce inflammatory infiltrate and pigment incontinence (H&E, x100) |
The central area showed hyperkeratosis, epidermal flattening and numerous melanophages in the superficial dermis (pigment incontinence) with a scarce lymphohistiocytic infiltrate. An Orcein stain showed no changes in the elastic fibers. The findings were consistent with annular lichen planus.
The patient was of African descent and had prior laboratory evidence of chronic microcytic hypochromic anemia (hemoglobin: 8.6 g/dl, mean corpuscular volume: 55.8 fl). Self-limited episodes of abdominal pain and diarrhea had been present for the last six months, with mild to moderate intensity, without visible pus or blood. Due to the sudden worsening of the anemia (hemoglobin: 6.1 g/dl), the patient was admitted to the internal medicine department. Infections by the hepatitis B and C viruses, human immunodeficiency virus 1 and 2, Mycobacterium tuberculosis and intestinal parasites were excluded.
Sickle cell trait was diagnosed (hemoglobin S: 27.6%), but very low iron and ferritin levels and high sedimentation rate (74mm/h) were present, justifying further investigation.
 |
| Figure 8 |
|---|
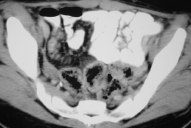
| Figure 8. Abdominal computer tomography: The mucosa of the colon and terminal ileum shows circumferential thickening |
The abdominal computer tomography revealed a uniform circumferential thickening from the ascending colon to the terminal ileum. The colonoscopy showed mucosal deformities and pseudo-polypoid images with vegetating and ulcerative areas. The biopsy taken was compatible with Crohn disease, and therapy was started with prednisolone (60mg/day) and mesalazine (1g 6/6h), with rapid response of both intestinal and cutaneous lesions.
After one month of therapy the elevated border disappeared, leaving only residual post-inflammatory hyperpigmented macules.
 |
| Figure 11 |
|---|
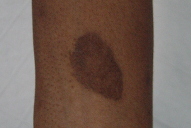
| Figure 11. Detail of the lesion on the arm after therapy: The elevated border disappeared, leaving a residual hyperpigmented lesion. |
The prednisolone dose was slowly tapered to 10mg/day and mesalazine was maintained; at 17 months, follow-up showed no recurrence of cutaneous or intestinal lesions.
Discussion
Annular lichen planus is an uncommon subtype of LP, usually presenting with small annular lesions, with elevated borders and central clearing [8]. Although initially thought to be more common in black patients, recent studies have not shown racial differences [11]. The male genitals and intertriginous areas are the more frequently affected locations and usually there are no lesions on the nails or mucosal sites [8, 11]. Annular lesions can occur associated with typical LP lesions, but most patients present with annular lesions only [11]. Annular atrophic LP might be considered another subtype, with central areas showing elastolysis secondary to previous inflammatory activity [12]; actinic LP presents with red-brown annular lesions mostly on sun-exposed skin [13]. In our patient the histopathology showed disease activity only in the elevated border and the central areas had a normal network of elastic fibers. The lesions were mostly on sun-protected sites.
LP has been associated with infections, autoimmune diseases, drugs, and contact allergies to metals, but the association with inflammatory bowel disease has very rarely been reported [4, 6, 10]. Crohn disease and LP have been described together in only two previous reports [9, 14]. In a review of 711 LP cases performed by an Italian group, only five patients (0.7%) had associated ulcerative colitis [10], and very few other reports on this association have been published [15-20]. The etiopathogenesis is not well understood, but the deposition of antigens or immune complexes of intestinal origin might trigger the cutaneous response [2, 3, 4]. This is one of the probable mechanisms responsible for other cutaneous associations of IBD, such as pyoderma gangrenosum, erythema nodosum, intestinal bypass syndrome, and cryoglobulinemia [21, 22]. The coincidence in the timing of appearance of both diseases and the response to therapy of both intestinal and skin lesions favors this association. Even so, the small number of cases could be interpreted as coincidental and systemic corticosteroids and sulphonamides can treat the skin lesions independently of their effect on the bowel disease [23]. Inflammatory bowel disease is frequently associated with skin disease and the fact they share an immunological pathogenesis makes this association probable. Further cases could help in confirming the association between both diseases.
References
1. Boyd AS, Neldner KH. Lichen planus. J Am Acad Dermatol. 1991 Oct;25(4):593-619. PubMed.2. Sugerman PB, Savage NW, Walsh LJ, Zhao ZZ, Zhou XJ, Khan A, Seymour GJ, Bigby M. The pathogenesis of oral lichen planus. Crit Rev Oral Biol Med. 2002;13(4):350-65. PubMed.
3. Sugerman PB, Satterwhite K, Bigby M. Autocytotoxic T-cell clones in lichen planus. Br J Dermatol. 2000 Mar;142(3):449-56. PubMed.
4. Lodi G, Scully C, Carrozzo M, Griffiths M, Sugerman PB, Thongprasom K. Current controversies in oral lichen planus: report of an international consensus meeting. Part 1. Viral infections and etiopathogenesis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005 Jul;100(1):40-51. PubMed.
5. Ellgehausen P, Elsner P, Burg G. Drug-induced lichen planus. Clin Dermatol. 1998 May-Jun;16(3):325-32. PubMed.
6. Calista D, Morri M. Lichen planus induced by hepatitis B vaccination: a new case and review of the literature. Int J Dermatol. 2004 Aug;43(8):562-4. PubMed.
7. Helm TN, Camisa C, Liu AY, Valenzuela R, Bergfeld WF. Lichen planus associated with neoplasia: a cell-mediated immune response to tumor antigens? J Am Acad Dermatol. 1994 Feb;30(2 Pt 1):219-24. PubMed.
8. Sakakibara K, Nakada T, Sueki H, Lijima M, Irisawa K. Annular lichen planus. J Cutan Med Surg. 2004 May-Jun;8(3):173-5. PubMed.
9. Keohane SG, Hayes PC, Hunter JA. Lichen planus and Crohn's disease. Acta Derm Venereol. 1997 Nov;77(6):488. PubMed.
10. Gruppo Italiano Studi Epidemiologici in Dermatologia. Epidemiological evidence of the association between lichen planus and two immune-related diseases. Alopecia areata and ulcerative colitis. Arch Dermatol. 1991 May;127(5):688-91. PubMed.
11. Reich HL, Nguyen JT, James WD. Annular lichen planus: a case series of 20 patients. J Am Acad Dermatol. 2004 Apr;50(4):595-9. PubMed.
12. Morales-Callaghan A Jr, Martinez G, Aragoneses H, Miranda-Romero A. Annular atrophic lichen planus. J Am Acad Dermatol. 2005 May;52(5):906-8. PubMed.
13. Salman SM, Kibbi AG, Zaynoun S. Actinic lichen planus. A clinicopathologic study of 16 patients. J Am Acad Dermatol. 1989 Feb;20(2 Pt 1):226-31. PubMed.
14. Kano Y, Shiohara T, Yagita A, Nagashima M. Erythema nodosum, lichen planus and lichen nitidus in Crohn's disease: report of a case and analysis of T cell receptor V gene expression in the cutaneous and intestinal lesions. Dermatology. 1995;190(1):59-63. PubMed.
15. Chemli S, Rym D, Jebali A, Hammami W. Association lichen planus and ulcerative colitis. A case report. Tunis Med. 2006 Jan;84(1):65-7. PubMed.
16. Giomi B, Pestelli E, Massi D, Caproni M, Fabbri P. Vulvar lichen planus associated with ulcerative colitis. A case report. J Reprod Med. 2003 Mar;48(3):209-12. PubMed.
17. Dhawan SS, Fields K. Lichen planus and ulcerative colitis-is there a relationship? Int J Dermatol. 1989 Oct;28(8):534. PubMed.
18. Cox NH, Finlay AY, Watkinson G. Atypical lichen planus associated with ulcerative colitis. Dermatologica. 1986;173(6):294-6. PubMed.
19. Cusano F, Errico G. Lichen planus and ulcerative colitis. Arch Dermatol. 1984 Aug;120(8):994-5. PubMed.
20. Wyatt EH. Lichen planus and ulcerative colitis. Br J Dermatol. 1975 Oct;93(4):465-8. PubMed.
21. Trost LB, McDonnell JK. Important cutaneous manifestations of inflammatory bowel disease. Postgrad Med J. 2005 Sep;81(959):580-5. PubMed.
22. Boh EE, al-Smadi RM. Cutaneous manifestations of gastrointestinal diseases. Dermatol Clin. 2002 Jul;20(3):533-46. PubMed.
23. Bauza A, Espana A, Gil P, Lloret P, Vazquez Doval FJ. Successful treatment of lichen planus with sulfasalazine in 20 patients. Int J Dermatol. 2005 Feb;44(2):158-62. PubMed.
© 2008 Dermatology Online Journal