Nodular amyloidosis in a patient with liver cirrhosis
Published Web Location
https://doi.org/10.5070/D33qn2q2wsMain Content
Nodular amyloidosis in a patient with liver cirrhosis
Makiko Ueno, Toshiyuki Yamamoto, Maaya Yamanaka, Tsuyoshi Matsunaga
Dermatology Online Journal 17 (7): 10
Department of Dermatology, Tsuchiura Kyodo General Hospital, Ibaraki, JapanAbstract
A 43-year-old Japanese man with alcoholic liver cirrhosis developed a nodule on the face 1 year prior to presentation. Histopathological examination showed amyloid deposition in the entire dermis, with numerous plasma cells. Nodular primary localized cutaneous amyloidosis is a rare form of amyloidosis, which needs long-term follow-up because of the possibility of the development of systemic amyloidosis. Also, this type of cutaneous amyloidosis may have other complications.
Introduction
Primary localized cutaneous amyloidosis (PLCA) is defined by deposition of amyloid in previously normal skin with no evidence of deposits in internal organs. Amyloidosis is classified into more common macular, papular, and the rare nodular form. We report herein a case of nodular amyloidosis on the face in a patient with alcoholic liver cirrhosis.
Case report
 |  |
| Figure 1 | Figure 2 |
|---|---|
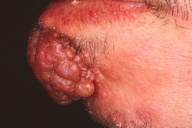
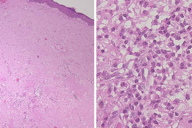
| Figure 1. Clinical appearance Figure 2. (A) Histologic view. (B) Plasma cell infiltration within the amorphous materials | |
A 43-year-old man visited our department, complaining of a nodule, which had gradually enlarged in size over12 months. He was suffering from liver cirrhosis related to alcohol. A physical examination showed a reddish, dome-shaped, multi-nodular lesion on the chin (Figure 1). Its surface was irregular. Biopsy specimen revealed amorphous materials in the entire dermis with prominent plasma cell infiltration (Figures 2A and 2B). The amorphous material positively stained with Congo-red and AL (κ). Also, the homogenous materials produced a characteristic apple-green birefringence under polarized light. The results of laboratory testing showed a decreased number of platelets, abnormal liver functions, and elevated serum levels of IgG (3310 mg/dl) and IgA (1090 mg/dl). Urinary Bence-Jones protein was negative and serum protein electrophoresis revealed no M-protein. Chest X-ray, electrocardiogram, and echocardiography were within normal ranges. There was no clinical evidence of systemic amyloidosis, such as organomegaly or macroglossia. The nodule was surgically removed and covered by a full-thickness skin graft. Thereafter, no recurrence was seen.
Discussion
Nodular amyloidosis presents with a single or multiple nodules on the face, trunk, and extremities and there is a predisposition for males [1, 2]. The nodules sometimes develop following chronic stimuli or minor trauma [3]. In the nodular type, amyloid is originated from AL protein produced by local plasma cells; modified β2-microglobulin is also shown to be a component of amyloid fibrils [4]. Apart from macular and lichen amyloidosis, amyloid materials are situated in the entire dermis. Plasma cell infiltration is prominent within or in peripheral areas of the amyloid materials, which is the important feature to differentiate it from nodular colloid degeneration [5]. In primary systemic amyloidosis, periorbital small, waxy nodules are seen. Although patients with nodular amyloidosis may develop systemic amyloidosis after long-term follow-up, recent papers indicate that the ratio is lower than previously reported [1, 2].
Several complications have been shown to be associated with cases of nodular amyloidosis. In a series of 16 cases of nodular amyloidosis, 2 patients had Sjögren syndrome, 2 had diabetes mellitus, and 3 had liver disease [2]. In particular, association with Sjögren syndrome is remarkable [6]. Nodular amyloidosis may be the result of a benign clonal proliferation of plasma cells in the skin owing to the lymphoproliferative characteristics of Sjögren syndrome. The present case did not have Sjögren syndrome, but had liver cirrhosis. Chronic inflammation may induce the homing of plasma cells into the skin, which may lead to the development of nodular amyloidosis.
References
1. Woollons A, Black MM. Nodular localized primary cutaneous amyloidosis: a long-term follow-up study. Br J Dermatol 2001; 145: 105-109. [PubMed]2. Moon AO, Calamia KT, Walsh JS. Nodular amyloidosis: review and long-term follow-up of 16 cases. Arch Dermatol 2003; 139: 1157-1159. [PubMed]
3. Kalajian AH, Waldman M, Knable AL. Nodular primary localized cutaneous amyloidosis after trauma: a case report and discussion of the rate of progression to systemic amyloidosis. J Am Acad Dermatol 2007; 57: S26-29. [PubMed]
4. Fujimoto N, Yajima M, Ohnishi Y, Tajima S, Ishibashi A, Hata Y, Enomoto U, Konohana I, Wachi H, Seyama Y. Advanced glycation end product-modified beta2-microglobulin is a component of amyloid fibrils of primary localized cutaneous nodular amyloidosis. J Invest Dermatol 2002; 118: 479-484. [PubMed]
5. Lai KW, Lambert E, Coleman S, Scott G, Mercurio MG. Nodular amyloidosis: differentiation from colloid milium by electron microscopy. Am J Dermatopathol 2009; 31: 472-474. [PubMed]
6. Meijer JM, Schonland SO, Palladini G, Merlini G, Hegenbart U, Ciocca O, Perfetti V, Leijsma MK, Bootsma H, Hazenberg BP. Sjögren’s syndrome and localized nodular cutaneous amyloidosis: coincidence or a distinct clinical entity? Arthritis Rheum 2008; 58: 1992-1999. [PubMed]
© 2011 Dermatology Online Journal

