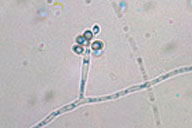
Zoonotic sporotrichosis transmitted by cats in Rio de Janeiro, Brazil. A case report.
Published Web Location
https://doi.org/10.5070/D33cr2c5dbMain Content
Zoonotic sporothricosis transmitted by cats in Rio de Janeiro, Brazil. A case report
Manoel P. Oliveira-Neto, Marise Mattos, Marcia Lazera, Rosani S. Reis, and Janice M. Chicarino-Coelho
Dermatology Online Journal 8(2): 5
From the Evandro Chagas Hospital, Oswaldo Cruz Foundation, Rio de Janeiro, Brazil.Abstract
Sporotricosis is a ubiquitous mycosis characterized by nodular lesions of the cutaneous or subcutaneous tissues and adjacent lymphatics that usually suppurate and ulcerate. Secondary spread to the articular surface and bone or dissemination to the central nervous system, genitourinary tract or lungs is also possible. All forms of sporothricosis are caused by a single species, Sporothrix schenkii. In the great majority of cases the fungus gains entrance into the body through trauma to the skin with some kind of plant materials such as thorns or splinters. Zoonotic transmission is also possible and several animals are implicated. This kind of transmission is most frequently a professional hazard of people dealing with animals but in some parts of the world, including Rio de Janeiro city and metropolitan region, an increase in transmission by pet cats has been noted. In these cases the infection may be observed in the family environment, an important epidemiological consideration to clinicians.
Case report
A 34 year old Brazilian housewife from the Rio de Janeiro metropolitan area, complained of an asymptomatic cutaneous ulcer on the left forearm and palpable subcutaneous nodules. Her illness had begun as a small pimple about two months prior to presentation. She had recently been nursing her cat that had been experiencing cutaneous ulcers for about six months but denies any kind of injury such as a scratch or bite. A veterinarian diagnosed the cat ulcers as consequent to an eczematous reaction.
 |
| Figure 3 |
|---|
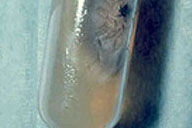
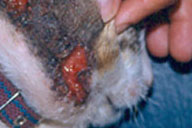
| Figure 3. Two large ulcers on the cat. Note that patient handled the animal with bare hands. |
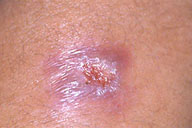
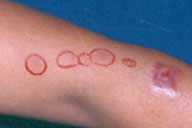
On physical examination she presented with an ulcer that measured 10 mm in diameter with an indurated base and raised, erythematous borders on her left forearm. Subcutaneous nodules, more palpable than visible, extended in a linear and ascending distribution on the left arm in the direction of the axilla.
Examination of the cat disclosed several small ulcers scattered over the animal's body and two large ulcers in the right retroauricular region and cheek.
 |
| Figure 4 |
|---|
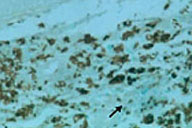
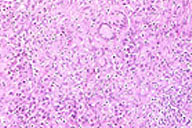
| Figure 4. Histopathology of the border of patient's ulcer showed a granulomatous infiltrate with numerous Langhans' cells and histiocytes (H&E, original magnification 100x) |
The patient's laboratory tests were normal or negative and included: VDRL, complete blood cell count, blood chemistry, urinalysis, chest X-Ray and parasitological examination of fecal samples. Biopsy specimens of the patient and cat ulcers were obtained for histological preparations and culture.
Histology (H&E stain) of the patient's ulcer showed a granulomatous infiltrate with many histiocytes and Langhans giant cells. Stains for fungi, cocci and mycobacteria were negative.
The cat's ulcer showed (H&E stain) a nonspecific inflammatory infiltrate composed of lymphocytes, histiocytes and plasma cells with many round elements in an intra as well as extra-cellular disposition. The round elements observed in H&E were stained with methenamine silver and a pathological diagnosis of fungous infection was made.
Fragments of biopsy specimens from both patient and cat were submitted for mycological cultures and yielded pure cultures of Sporothrix schenkii.
Discussion
The clinical diagnosis, confirmed by histology and cultures, was sporotrichosis, a cosmopolitan, subcutaneous mycosis. Sporothrix schenkii is a dimorphic fungus widely dispersed in nature and found mainly in dead or senescent plant matter, soil and several animals including equines, cats, dogs, pigs and birds. [1] Zoonotic transmission is rare, but exposure to the numerous fungal organisms present in skin lesions of cats enhance the infective capability of such lesions and may produce disease by simple contact without any penetrating injury.[2,3] The first report of human sporotrichosis transmitted by cats was published in 1982 [4] but cases involving accidents with cats had already been reported much earlier in the Brazilian literature [5]. Since 1982 several other cases of this type of transmission have been reported. [6,7,8,9] In recent years an increase of cat-transmitted sporothricosis has been reported in some regions such as Malaysia [7] and Rio de Janeiro. [10] The clinical picture of human sporotrichosis transmitted by cats does not differ from the classical type of transmission induced by wood splinters and other organic materials except for the fact that lymphangitic forms are more frequent. The therapy is the same. Potassium iodide and itraconazole are both effective. [11] In the case here reported the patient's disease resolved spontaneously. Zoonotic transmission is more frequent as an occupational hazard for veterinarians and veterinary assistant personnel, including students, but clinicians should be aware of transmission from household pet cats to family members.
References
1. Schell WA. Agents of chromoblastomycosis and sporotrichosis. In: Topley and Wilson's Microbiology and Microbial infections. Ajello LJ & Hay RJ Eds. 9rd ed. Vol 4. Medical Mycology. London: Arnold, 1998 pp 315-336.2. Dunstan RW, Reimann KA, Langham RF. Feline sporotrichosis. J Am Vet Med Assoc 1986;189(8):880-3. PubMed
3. Reed KD, Moore FM, Geiger GE, Stemper ME. Zoonotic transmission of sporotrichosis: case report and review. Clin Infect Dis 1993;16(3):384-7. PubMed
4. Read SI, Sperling LC. Feline sporotrichosis. Transmission to man. Arch Dermatol 1982;118(6):429-31. PubMed
5. Almeida F, Sampaio SAP, Lacaz CS, Fernandes JC. Dados estatisticos sobre a esporotricose. Analise de 344 casos. An bras Dermatol 1955;30:9-12
6. Dunstan RW, Langham RF, Reimann KA, Wakenell PS. Feline sporotrichosis: a report of five cases with transmission to humans. J Am Acad Dermatol 1986;15(1):37-45. PubMed
7. Zamri-Saad M, Salmiyah TS, Jasni S, Cheng BY, Basri K. Feline sporotrichosis: an increasingly important zoonotic disease in Malaysia. Vet Rec 1990;127(19):480. PubMed
8. Marques SA, Franco SRVS, Camargo RPM, Dias LDF, Haddad Junior V, Fabris VE. Esporotricose do gato doméstico (Felix catus): transmissão humana. Rev Inst Med trop S Paulo. 1993; 35:327-330
9. Smilack JD. Zoonotic transmission of sporotrichosis [letter; comment]. Clinical Infectious Diseases 1993;17(6):1075. PubMed
10. Barros MB, Schubach TM, Gutierrez Galhardo MC, Schubach Ad, Monteiro PC, Reis RS, Zancope-Oliveira RM, Lazera Md, Cuzzi-Maya T, Blanco TC, Marzochi KB, Wanke B, Valle AC. Sporotrichosis: an emergent zoonosis in Rio de Janeiro. Mem Inst Oswaldo Cruz 2001;96(6):777-9. PubMed
11. 11. Restrepo A, Robledo J, Gomez I, Tabares AM, Gutierrez R. Itraconazole therapy in lymphangitic and cutaneous sporotrichosis. Arch Dermatol 1986;122(4):413-7. PubMed
© 2002 Dermatology Online Journal