Cutaneous blastomycosis presenting as non-healing ulcer and responding to oral ketoconazole
Published Web Location
https://doi.org/10.5070/D32p56q0q9Main Content
Cutaneous blastomycosis presenting as non-healing ulcer and responding to oral ketoconazole
P Balasaraswathy DVD DNB1, and Theerthanath MD2
Dermatology Online Journal 9 (5): 19
From the Departments of Dermatology1 and Pathology2, KS Hegde, Medical Academy, Deralakatte, Mangalore, India. drbali@vsnl.com
Abstract
Primary cutaneous blastomycosis is a rare infection of the skin that usually follows trauma and presents as a papule or nodule that ulcerates. Although this infection often heals spontaneously, we present a case of a nonhealing ulcer following surgical drainage of cellulitis. Blastomycosis was diagnosed by histopathological examination and the infection responded well to oral ketoconazole therapy.
Introduction
Blastomycosis is an uncommon, chronic, granulomatous disease caused by the dimorphic fungus Blastomycetes dermatitidis [1, 2]. The spectrum of clinical manifestations of blastomycosis includes acute pulmonary disease, subacute and chronic pulmonary disease, and disseminated extrapulmonary disease. The skin is the most common site for dissemination, followed by bone, genitourinary tract, and central nervous system [2, 3]. Primary cutaneous blastomycosis is a rare illness [1], said to occur only after traumatic implantation of the fungus [2]. Blastomycosis is rare in India [4].
We report a case of cutaneous blastomycosis presenting as a nonhealing ulcer. This case is of interest because of its rarity, and response to oral ketoconazole therapy.
Case presentation
A 47-year-old male driver presented with a 2-month history of multiple ulcers, varying in size and involving the left lower extremity. The illness began with swelling of the left lower limb and redness around the left ankle, for which he underwent incision and drainage at a tertiary-care center. Following the procedure, a nonhealing ulcer developed at the site of the incision, and multiple new papules and nodules erupted along the left lower limb up to the mid-thigh. Many nodules ruptured, leaving multiple oval ulcers. The patient also complained of occasional transient swelling of the left inguinal region, and fever every evening. There was no history of any trauma preceding the illness. There was no history of cough, tuberculosis, diabetes, or exposure to venereal disease and HIV. He had received multiple unsuccessful courses of antibacterial drugs.
On examination, the patient was a moderately built, poorly nourished, middle-aged man with pallor. He had hyperpigmentation and edema of the left lower extremity with multiple soft nodules and ulcers of different sizes around the left ankle and leg. Some of the lesions were arranged in a linear pattern. The ulcers were well defined and oval. They exhibited undermined edges, healthy granulation tissue, and movable bases. The largest ulcer, 4.3 cm in diameter, was at the site of the incision at the lateral malleolus. The nodules were cystic and the leg edema was woody. There were 2-3 inguinal lymph nodes, about 1 cm in size, nontender and mobile. There were no varicose veins and the genitalia were normal. Systemic examination was normal.
|
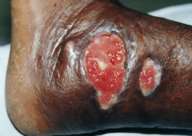
| Figure 1 |
|---|
| Ulcers over the left leg before treatment |
A differential diagnosis of cutaneous tuberculosis (scrofuloderma) and sporotrichosis was considered.
Laboratory investigations revealed a total leukocyte count of 9,300 cells/mm3 with 75 percent neutrophils, 22 percent lymphocytes and 3 percent eosinophils. ESR was elevated at 105 mm. A fasting blood glucose was 85 mg/dL and creatinine was 1 mg/dL. HBSAg, HCV, HIV and VDRL were nonreactive. Chest X-ray was normal, without evidence of parenchymal lesions or infiltrates. X-ray of the leg was also normal, without evidence of osteomyelitis. Mantoux test did not yield any induration. Culture of the pus yielded no bacterial pathogens. KOH mount from fluid of a fresh lesion revealed budding spores with broad base.
|
|
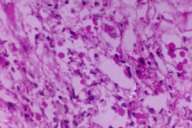
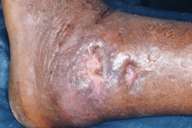
| Figure 2 | Figure 3 |
|---|---|
| Biopsy showing thick walled spores with broad based buds, suggestive of blastomycosis. (fig. 2) Healed ulcers after treatment (fig. 3) | |
A biopsy was performed from the ulcer edge. The epidermis showed ulceration with a moderate degree of epithelial hyperplasia and microabscesses extending into the dermis. The dermis showed focal areas of suppurative, granulomatous infiltrate with giant cells and the presence of many thick-walled spores measuring about 8-15 µ. Broad-based buds suggestive of blastomycosis were observed. Periodic Acid Schiff staining confirmed the presence of sporulating fungus.
The patient was treated with oral ketoconazole (200 mg twice daily). Within 3 weeks the ulcer healed. The patient was instructed to continue the treatment for an additional 6 months.
Discussion
Cutaneous blastomycosis can occur as the most common manifestation of disseminated extrapulmonary blastomycosis or the result of direct inoculation of the skin. The incidence of infection is highest in rural areas and in agricultural workers [5]. Adult males are most commonly affected, the majority being 30-50 years old [5]. Skin lesions in disseminated blastomycosis may be single or multiple, are often symmetrical, and are usually on the trunk rather than on the extremities [5]. In some cases, the primary pulmonary focus may resolve before the cutaneous manifestation appears [6]. Primary cutaneous blastomycosis is very rare, and unique skin involvement is very exceptional [1, 5]. Primary cutaneous blastomycosis follows traumatic implantation of the fungus [7], which may occur in a lab or morgue worker or paleontologist. In addition, animal bites or scratches and other kinds of trauma have been modes of infection [2]. After inoculation, an erythematous, indurated area with a chancre appears in 1-2 weeks and is associated with lymphangitis and lymphadenopathy. There is a strong tendency for spontaneous recovery [2, 5].
Clinically, cutaneous blastomycosis may be mistaken for keratoacanthoma, squamous cell carcinoma, tuberculosis, tertiary syphilis, leprosy, or bacterial pyoderma [4]. Criteria for the diagnosis of cutaneous blastomycosis include the presence of characteristic skin lesions (often with focal lymphadenopathy or lymphangitis), a history of inoculation with something likely to contain the organisms, no evidence of systemic involvement (before, during, or after presentation), and culture or direct smear demonstrating the organisms in the skin lesions or lymph nodes [2].
The diagnosis of blastomycosis may be confirmed through the identification of the yeasts of Blastomycetes dermatitidis in body fluids, tissues, or cultured material. Culture may be the first method of detecting the fungus in only 3.2 percent of patients [8], and even in the absence of culture the diagnosis may be made confidently by the histological method [9]. Fine-needle aspiration of the lesion has also been reported useful [4]. Histopathological examination may show epidermal hyperplasia, epidermal microabscesses and abscesses, epidermal necrosis, and dermal infiltration with inflammatory cells. The histopathological examination does not differentiate primary from secondary cutaneous blastomycosis [2].
Various antifungal drugs have been tried in the treatment of cutaneous blastomycosis, and oral triazoles, ketoconazole, fluconazole, and itraconazole, have been found useful [2, 10, 11]. Spontaneous remission has also been reported [2, 5]. Surgical excision, incision and drainage, radiation therapy, [2] and carbon dioxide laser vaporization [12] have been tried.
Our patient presented with a nonhealing ulcer following surgical drainage of a lower leg cellulitis. The unsuspected diagnosis of cutaneous blastomycosis was made on histological examination. He had no evidence of systemic involvement or immunosuppression. The ulcer healed after 3 weeks of oral ketoconazole administration. A diagnosis of cutaneous blastomycosis should be considered in cases of nonhealing ulcers and nodules. This disease may be underreported in this part of the world.
References
1. El Haouri M, Sedrati O, Erragragui Y, Ghfir M, Labraimi A, Zrara I, Baba N, El Alaoui N, Sekkat A. Cutaneous blastomycosis revealing a corticoadenoma. Ann Dermatol Venereol. 2001 Mar;128(3 Pt 1):253-6. PubMed2. Gray NA, Baddour LM. Cutaneous inoculation blastomycosis. Clin Infect Dis. 2002 May 15;34(10):E44-9. Epub 2002 Apr 17. PubMed
3. Bradsher RW. Clinical features of blastomycosis. Semin Respir Infect. 1997 Sep;12(3):229-34. PubMed
4. Desai AP, Pandit AA, Gupte PD. Cutaneous blastomycosis. Report of a case with diagnosis by fine needle aspiration cytology. Acta Cytol. 1997 Jul-Aug;41(4 Suppl):1317-9. PubMed
5. Hay RJ, Roberts SOB, Mackenzie DWR. Blastomycosis. In Rook, Wilkinson, Ebling Textbook of Dermatology. Champion RH, Burton JL, Ebling FLG (Editors). Fifth Edition. Blackwell Scientific Pub. Oxford. pp. 1195-97, 1992.
6. Mercurio MG, Elewski BE. Cutaneous blastomycosis. Cutis. 1992 Dec;50(6):422-4. PubMed
7. Body BA. Cutaneous manifestations of systemic mycoses. Dermatol Clin. 1996 Jan;14(1):125-35. PubMed
8. Lemos LB, Guo M, Baliga M.Blastomycosis: organ involvement and etiologic diagnosis. A review of 123 patients from Mississippi. Ann Diagn Pathol. 2000 Dec;4(6):391-406. PubMed
9. Rivasi F, Nanetti A, Cesinaro AM, Mazzoni A. Histopathological evidence of North American blastomycosis in Italy: report of two cases. APMIS. 2000 Apr;108(4):273-5. PubMed
10. Chodorowska G, Lecewicz-Torun B. Long-term observation of a case of cutaneous blastomycosis in Poland treated with fluconazole. Mycoses. 1996 Jul-Aug;39(7-8):283-7. PubMed
11. Kauffman CA. Newer developments in therapy for endemic mycoses. Clin Infect Dis. 1994 Aug;19 Suppl 1:S28-32. PubMed
12. Kantor GR, Roenigk RK, Bailin PL, Bergfeld WF, Bass J. Cutaneous blastomycosis. Report of a case presumably acquired by direct inoculation and treated with carbon dioxide laser vaporization. Cleve Clin J Med 1987;54(2):121-124. PubMed
© 2003 Dermatology Online Journal

