Annular plaques: An unusual manifestation of graft-versus-host disease
Published Web Location
https://doi.org/10.5070/D31z0462hjMain Content
Annular plaques: An unusual manifestation of graft-versus-host disease
Laura J Alexander MD, Taraneh Paravar MD, Madeleine Duvic MD, Victor Prieto MD, Sharon R Hymes MD
Dermatology Online Journal 18 (6): 4
Department of Dermatology, University of Texas MD Anderson Cancer Center, Houston, TexasAbstract
Chronic cutaneous graft-versus-host disease (GVHD) classically presents with lichenoid papules or sclerotic plaques. This case highlights an unusual clinical manifestation of chronic GVHD and demonstrates that the skin morphology of chronic GVHD and cutaneous lymphoma may be similar. We report for the first time a case of annular scleroderma-like graft-versus-host disease in a patient following allogeneic stem cell transplant for CD30+ anaplastic large cell lymphoma. Treatment of these skin lesions with ultraviolet A1 (UVA1) phototherapy resulted in significant improvement.
Introduction
Chronic cutaneous graft-versus-host disease (GVHD) classically presents with lichenoid papules or sclerotic plaques. We report a unique case of annular scleroderma-like graft-versus-host disease in a patient following allogeneic stem cell transplant for CD30+ anaplastic large cell lymphoma. The morphology of his original lymphoma was also annular plaques. Two years after his allogeneic stem cell transplant, he developed annular hyperpigmented plaques on the shoulders, back, and trunk, which were biopsy-proven cutaneous T cell lymphoma; he was treated with donor lymphocyte infusions. He subsequently developed new annular lesions on the trunk and upper extremities and the biopsy specimen was consistent with scleroderma-like graft-versus-host disease, recalcitrant to topical corticosteroids. These plaques improved with ultraviolet A1 (UVA1) phototherapy. This case highlights an unusual manifestation of chronic cutaneous GVHD and demonstrates the diagnostic importance of a skin biopsy.
Case report
A 45-year-old man was diagnosed with Hodgkin lymphoma in 1991 for which he underwent chemotherapy with adriamycin, bleomycin, vinblastine, and dacarbazine (ABVD), as well as radiation. Subsequently, he developed non-Hodgkin lymphoma with a CD30+ phenotype and cutaneous involvement in 1997. Despite further chemotherapy with adriamycin, methylprednisolone, cytosine arabinoside, and cisplatinum (ASHAP) and an autologous peripheral blood stem cell transplant in early 1998, he had a cutaneous relapse in mid-1998 and was treated with psoralen plus ultraviolet A (PUVA) and interferon with some response. Because of further progression of his disease, he had a second stem cell transplant from a matched sibling in 1999. Lichen planus-like graft-versus-host disease developed subsequently, which was controlled with oral methylprednisolone and tacrolimus.
In 2001 he presented to the dermatology clinic with erythematous, annular plaques with central hyperpigmentation on his back. A biopsy showed an atypical perivascular dermal and subcutaneous lymphoid infiltrate, positive for monoclonal immunoglobulin heavy chain rearrangements, but without evidence of monoclonal T-cell receptor gamma chain gene rearrangements. The diagnosis was felt to be consistent with relapse of his cutaneous lymphoma. He was treated topically with clobetasol 0.05 percent cream and bexarotene 1 percent gel, and received a donor lymphocyte infusion.
 |  |
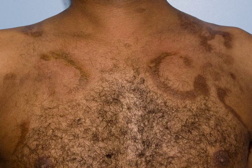
| Figure 1 | Figure 2 |
|---|---|
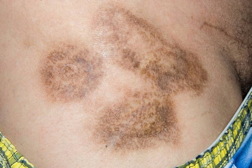
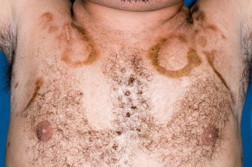
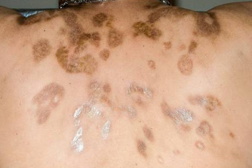
| Figure 1. Hyperpigmented indurated and sclerotic oval and annular plaques on upper the chest. Figure 2. Hyperpigmented indurated and sclerotic oval and annular plaques on the back. | |
Following this treatment, the patient developed red papules and plaques with dusky centers on his trunk, some with induration; the biopsies were consistent with chronic graft-versus-host disease. Photophoresis was started but discontinued after a few treatments related to the development of a seizure. Topical tacrolimus and intralesional triamcinolone were not helpful.
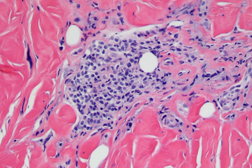 |
| Figure 5 |
|---|
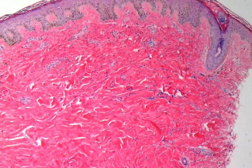
| Figure 5. Punch biopsy from upper back (H&E, x10) demonstrating perivascular and interstitial lymphoplasmacytic infiltrate. |
Over the next several years, his lesions progressed. The patient’s physical examination revealed multiple hyperpigmented, indurated and sclerotic oval and annular plaques on the upper chest, back, and flanks. There was no lymphadenopathy.
A punch biopsy of an upper back lesion was performed.
Microscopic findings
The biopsy specimen from the upper back showed mild acanthosis of the epidermis with flattened rete ridges. There were scattered dyskeratotic cells with mild vacuolar alteration of the basal layer. The dermis revealed thickened and sclerotic collagen. There was loss of periadnexal adipose tissue. Higher power view showed a perivascular and interstitial infiltrate of lymphocytes with some scattered plasma cells. There were no atypical lymphocytes. Therefore, immunohistochemical studies were not performed. However, several subsequent biopsies of coincident lesions showed a mixed CD4+ and CD8+ infiltrate with only rare CD30+ cells. PCR analysis showed no evidence of monoclonal T-cell receptor gamma chain gene rearrangements. The diagnosis was consistent with scleroderma-like graft-versus-host disease.
Clinical course
 |
| Figure 6 |
|---|
| Figure 6. Decreased thickness and induration of oval and annular plaques on upper back after UVA1 therapy. |
The patient was treated with clobetasol 0.05 percent ointment BID, which was ineffective. UVA1 was added, starting at low dose (30 J/cm²), three times per week. The dose was gradually increased as tolerated to 50 J/cm². There was a decrease in thickness and induration of his lesions. After 17 treatments (740 J), the patient discontinued all treatments.
Discussion
Hematopoietic stem cell transplantation (HSCT) using peripheral blood, cord blood, or bone marrow is used to treat a wide variety of genetic and immunologic disorders, as well as hematologic and solid organ malignancies [1]. A complication of HSCT, chronic graft-versus-host disease (cGVHD), often presents with cutaneous involvement and involves multiple organ systems.
Cutaneous cGVHD is most often divided into two categories: lichen planus-like and scleroderma-like. In scleroderma-like GVHD, lesions may be localized and morphea-like or develop deeper dermal or fascial involvement. On histology, the epidermis can be unremarkable, with rare vacuolar change, inflammation, or colloid body formation. The dermis is thickened and involvement may extend through the adipose to the fascia.
We highlight in this article a unique case of annular scleroderma-like cGVHD and its response to UVA1. A search in PUBMED with the search terms GVHD or graft-versus-host disease and annular, revealed no other reports of annular GVHD. Our patient is unique in that he had annular plaques both with his cutaneous lymphoma and cGVHD. It was difficult to clinically distinguish the two and ultimately, biopsy with immunostaining was helpful. Although both diagnoses presented with an annular morphology, his GVHD lesions were sclerotic and indurated, whereas his cutaneous lymphoma was not. In addition, the classic histologic features of scleroderma-like GVHD and lack of lymphocyte atypia excluded a diagnosis of lymphoma. Of note, the clinical changes of scleroderma-like GVHD would not be expected with the particular chemotherapeutic treatments he received.
Our case is also unique in that there have been few prior reports of cutaneous T cell lymphoma presenting as annular plaques. Rather, several reports present annular erythema as a manifestation of cutaneous T cell lymphoma [2, 3, 4].
There are currently a number of treatment options for scleroderma-like cGVHD. In our patient, UVA1 was helpful and topical corticosteroids were not. UVA1 has more recently been utilized as a treatment option [5]. The mechanism may include apoptosis of T cells leading to decreased inflammatory infiltrate and up-regulation of collagenase activity, thus decreasing the induration. Studies in atopic dermatitis indicate that UVA1 therapy is capable of down-regulating in situ expression of interferon-γ in lesional skin [6]. In addition, in vitro experiments showed that UVA1 is a potent inducer of the immunosuppressive cytokine interleukin-10 in human keratinocytes [6]. UVA1 therapy is usually well tolerated with few side effects. Erythema, tanning, polymorphic light eruptions, itching, and recrudescence of herpes simplex infection are the main acute adverse effects [6]. UVA1 is often used in combination with systemic immunosuppressive treatments, and thus patients are at increased risk of developing cutaneous malignancies. Furthermore, little is known about the long-term effects of low-, medium-, or high-dose UVA1 therapy [5].
A standard dosing regimen has not yet been established. It is not yet clear from studies whether high-, medium-, or low-dose UVA1 therapy is needed for successful collagenase induction. In this case, however, our patient saw improvement on medium dose therapy.
We report here for the first time a case of annular scleroderma-like GVHD in a patient following allogeneic stem cell transplant. We also demonstrate the morphologic similarity between his cutaneous lymphoma and cutaneous GVHD. Treatment with UVA1 and clobetasol demonstrated significant improvement in our patient.
References
1. Hymes SR, Turner ML, Champlin RE, Couriel DR. Cutaneous Manifestations of Chronic Graft-versus-Host Disease. Biology of Blood and Marrow Transplantation. 2006 Nov; 12: 1101-1113. [PubMed]2. Moura FN, Thomas L, Balme B, Dalle S. Mycosis fungoides mimicking an annular erythema. Clinical and Experimental Dermatology. 2009 Dec; 34(8): e581-e583. [PubMed]
3. Lim DS, Murphy GM, Egan CA. Mycosis fungoides presenting as annular erythema. British Journal of Dermatology. 2003 Mar; 148 (3): 591. [PubMed]
4. Ceyhan AM, Akkaya VB, Chen W, Bircan S. Erythema annulare centrifugum-like mycosis fungoides. Australasian Journal of Dermatology. 2011 Nov; 52 (4): e11-3. [PubMed]
5. Grundmann-Kollmann M, Behrens S, Gruss C, Gottlober P, Peter RU, Kerscher M. Chronic sclerodermic graft-versus-host disease refractory to immunosuppressive treatment responds to UVA1 phototherapy. Journal of the American Academy of Dermatology. 2000 Jan; 42 (1): 134-136. [PubMed]
6. Wetzig T, et al. Medium dose long wavelength ultraviolet A (UVA1) phototherapy for the treatment of acute and chronic graft-versus-host disease of the skin. Bone Marrow Transplant. 2005 Mar; 35(5): 515-519. [PubMed]
© 2012 Dermatology Online Journal