Recurrence of periumbilical Paget disease after fresh Mohs treated with slow Mohs with CK-7
Published Web Location
https://doi.org/10.5070/D31vj001qzMain Content
Letter: Recurrence of periumbilical Paget disease after fresh Mohs treated with slow Mohs with CK-7
I Salgüero Fernández1, L Rios Buceta1, Carmen Moreno Garcia del Real2, Rosario Carrillo Gijón2
Dermatology Online Journal 17 (7): 13
1. Department of Dermatology, Hospital Ramón y Cajal, Madrid, Spain. irenebsf@hotmail.com2. Department of Pathology, Hospital Ramón y Cajal, Madrid, Spain
Abstract
Extrammamary Paget disease (EMPD) is an uncommon neoplasm that often involves the skin of the genital or perianal regions. There are no clearly established guidelines for treatment, but surgical excision with wide margins (3-5 cm) or Mohs micrographic surgery (MMS) are the techniques of choice when there is no association with an underlying neoplasm. We present a case of EMPD in an unusual location (periumbilical skin). This was treated with fresh MMS, but reappeared, necessitating a second MMS (slow).
Case report
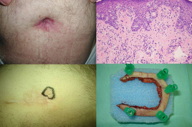 |
| Figure 1 |
|---|
A 59-year-old male presented with a two-month history of a persistent pruritic plaque on the periumbilical skin (Figure 1). During these months he was diagnosed with chronic eczema and treated with topical corticosteroids and an oral antihistamine, but there was only minor improvement of pruritus. He had no personal history of atopic dermatitis, psoriasis, or potentially causative drug intake.
Dermatological examination revealed an erythematous and indurated plaque with sharp demarcation without any palpable, underlying tumor. The plaque was 20 mm in diameter with an oozing surface. No enlarged lymph nodes were detected.
The results of radiological investigations, including chest X-ray and computed tomography scans of the chest, abdomen, and pelvis were normal. Tumor markers CEA, CA-125, and CA 15-3 were also within the normal range.
 |
| Figure 2 |
|---|
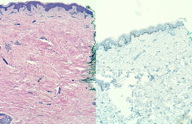
| Figure 2. Scattered Paget cells on the basal layer and CK-7 (H&E) |
A biopsy performed on the abdominal skin showed large, epithelioid, round cells with abundant pale-staining cytoplasm, and intraepidermic hypertrophic nuclei containing prominent nucleoli. These cells migrated through the epidermis. A comprehensive immunohistochemical study was carried out (Figure 2). Samples were reactive for cytokeratin 7 (CK-7) and negative for cytokeratin 20 (CK-20), as well as negative for S-100 and reactive for CAM 5.2. These findings were consistent with Paget cells and a diagnosis of primary extramammary Paget disease was made.
He was first treated with fresh MMS. One year later, however, he developed an erythematous plaque on the right side of the surgical scar, confirmed as a relapse of EPD by a skin biopsy. The patient was treated again by slow MMS; cytokeratin-7 (CK-7) immunostain was carried out in order to confirm the complete resection of the tumor. Two years later the patient had shown no recurrence of the disease.
Discussion
Extrammamary Paget disease can be defined as a cutaneous adenocarcinoma of epidermal origin that usually occurs in sites containing apocrine glands and is often associated with internal malignancy. Internal malignancy is found in 24 percent to 33 percent of EMPD cases and adnexal cancers in 12 percent to 18 percent. Typically, the location of an associated internal malignancy is closely related to the anatomic site of EMPD. For example, perianal EMPD is associated with lower gastrointestinal tract malignancies and genital EMPD is associated with genitourinary tract malignancies. Yet, there are several reports of EMPD associated with malignancies that arose in organs distant from the EMPD site [1].
The histogenesis is still controversial. Several authors propose that EMPD is a heterologous entity, with some cases representing an intraepithelial primary adenocarcinoma and others being epidermotropic metastases or a direct extension of an associated internal malignancy. It has been postulated that ectopic EMPD cells derive from pluripotent germinative cells, which may explain how EMPD can appear in areas without apocrine glands [2].
Patients often present with well-defined pink or white plaques accompanied by pruritus [3]. Because it is a nonspecific clinical presentation it has been reported that an average of 1 year will pass before a biopsy is taken and a definitive diagnosis is established [4].
The differential includes psoriasis, contact dermatitis, dermatophytosis, lichen sclerosis, Bowen disease, pagetoid basal cell carcinoma, and mycosis fungoides [5]. An immunohistochemical panel such as low-molecular-weight cytokeratin, high-molecular weight cytokeratin, CEA, EMA, and S-100 protein is useful in differentiating Paget disease from melanoma and pagetoid Bowen disease [3].
Treatment can be topical with 5-Fluoruracil, bleomicin, or imiquimod, for example. Alternative treatments include radiation therapy, cryotherapy, chemotherapy, and photodynamic therapy (10), but the treatment of choice whenever possible is surgical excision with wide margins or Mohs micrographic surgery. Connor et al [6] found that Mohs micrographic surgery compared favorably with wide excision and had a local recurrence rate of 8 percent (at mean follow-up of 24 months) versus 22 percent for patients who underwent wide excision (at mean follow-up of 65 months). Extrammamary Paget disease is a difficult tumor because of the subclinical microscopic extensions that cause marginal tumor persistence or recurrence.
To decrease the rate of persistence or recurrence one can use immunostaining with CK-7 that identifies Paget cells that may otherwise be undetected [7].
We report the use of CK-7 immunostaining in delineating the surgical margins of a pagetoid cutaneous neoplasm during MMS. We believe that the use of CK-7 should be performed routinely in this type of tumor to ensure complete removal.
References
1. Saitou Y, et al. Hepatocellular carcinoma associated with extramammary Paget disease. J Clin Gastroenterol. 2004;38 :89-90. [PubMed].2. Daofeng Ben, Liu Liu, Bing Ma, Yongyan Li, Zhaofan Xia. Extramammary Paget's disease arising from a burn scar of right forearm: An uncommon case report. Burns. 2010;36:145-7. [PubMed].
3. Cohen MA, Hanly A, Poulos E, Goldstein GD. Extramammary Paget's disease presenting on the face. Dermatol Surg. 2004;30:1361-3. [PubMed].
4. Zollo JD, Zeitouni NC. The Roswell Park Cancer Institute experience with extramammary Paget's disease. Br J Dematol 2000;142:59-65. [PubMed].
5. Balducci L, Crawford ED, Smith GF, et al. Extramammary Paget's disease: an annotated review. Cancer Invest 1988;6:293-303. [PubMed].
6. O'Connor WJ, Lim KK, Zalla MJ, Gagnot M, Otley CC, Nguyen TH, Roenigk RK. Comparison of mohs micrographic surgery and wide excision for extramammary Paget's disease. Dermatol Surg. 2003;29:723-7. [PubMed].
7. Hendi A, Perdikis G, Snow JL. Unifocality of extramammary Paget disease. J Am Acad Dermatol. 2008;59:811-3 [PubMed].
© 2011 Dermatology Online Journal

