Eruptive keloids: Spontaneous reactivation after 60 years
Published Web Location
https://doi.org/10.5070/D31rp874txMain Content
Eruptive keloids: Spontaneous reactivation after 60 years
Nuno Menezes1, Ana Moreira1, Antónia Furtado2, Eugenia Bacelar3, Armando Baptista1, Eduarda Osório Ferreira1
Dermatology Online Journal 15 (4): 2
1. Serviço de Dermatologia e Venereologia do CHVNG. nuno.menezes.dermatologia@gmail.com2. Serviço de Anatomia Patológica do CHVNG
3. Clínica de São João da Madeira
Abstract
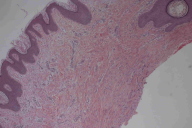
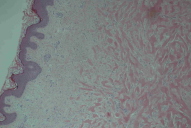
An 84-year-old man with keloids since early adulthood, was referred to our clinic because of the recent appearance of erythematous, tumid plaques upon the old keloids and upon uninvolved skin. The plaques were located mainly on the trunk in a linear distribution. On the back there were round, nodular, erythematous nodules and plaques, with central crusts, that had just appeared on normal skin. A skin biopsy was performed on the plaques that appeared over the older lesions. The histological appearance was consistent with keloid. Similar histology was found in a biopsy taken from a plaque that had erupted on normal skin.
Introduction
Hypertrophic scars and keloids are common problems, especially in individuals of African, Hispanic, and Asian descent. Both keloids and hypertrophic scars are characterized by abundant deposition of collagen and glycoprotein; however, keloids differ from hypertrophic scars both clinically and histologically [1]. The basis for hypertrophic scar and keloid formation is not clear; although, an imbalance of matrix degradation and collagen biosynthesis resulting in excess accumulation of collagen, similar to a wound repair process, has been postulated to be important in the etiology of these skin lesions [2, 3]. Reactivation of old scars is a very specific sign for sarcoidosis, although very unusual. When there is reactivation of a scar one should investigate for the presence of sarcoidosis [4].
Clinical Case
 |  |
| Figure 1 | Figure 2 |
|---|---|
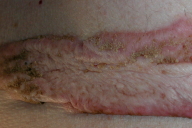
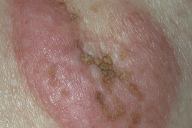
| Figure 1. New lesions growing attached to an old one Figure 2. Lesion arising de novo on normal skin | |
An 84-year-old man with keloids since early adulthood, located mainly on the trunk in a linear distribution, was referred to our clinic because of the appearance of new erythematous, tumid plaques, some of which appeared on old keloids (Fig. 1). Simultaneously, additional round, erythematous nodules and plaques with central crusts appeared on the back (Fig. 2) in areas of previously uninvolved skin. There were no associated symptoms and the plaques progressed gradually over a period of six months without any injury to the skin. The diagnoses of sarcoidosis, cutaneous lymphoma, or scar reactivation were considered. A skin biopsy was performed on the plaques that appeared upon the older keloids. Histological exam showed features of a keloid scar (Fig. 3). Another biopsy was also performed in the plaques appearing on normal skin; this was once again diagnostic for keloid scar (Fig. 4). Laboratory testing showed normal or negative results for serum angiotensin-converting enzyme, HIV1/HIV2 antibodies, and calcium. A chest X-ray was also normal. Possible treatments entertained included pulsed dye laser, intralesional corticosteroids, and silicon dressings. However, the patient refused treatment.
Discussion
Keloidal scarring is one of the most frustrating clinical problems in wound healing. Keloids form following dermal injury and exhibit exuberant, progressive production of collagen [5]. Keloid formation has been ascribed to altered growth factor regulation, aberrant collagen turnover, and immune dysfunction. But no single unifying hypothesis adequately explains keloid formation [5]. Recently TGF-β has been implicated in the pathogenesis of keloid formation. Some studies have demonstrated overproduction of TGF-β, IL-6, IL-13, or IL-15 [6]. However, gene polymorphisms for TGF-β have not been detected in keloid patients [7].
Keloids and hypertrophic scars are separate clinical and histological entities. Clinically, hypertrophic scars remain within the confines of the original scar border, whereas keloids invade adjacent normal dermis. Hypertrophic scars generally arise within 4 weeks, grow persistently for several months, and then regress. In contrast, keloids may appear later, may follow an initial scar, and then progressively grow indefinitely [8, 9].
There are predisposed anatomic regions for the formation of keloids, namely the shoulders, sternum, jaw and arms. Keloids are more common in dark skin races and ethnic groups. The affected regions frequently are difficult to hide, which implies a direct and indirect effect on the quality of life of these patients [10].
Although both keloids and hypertrophic scars show increased fibroblast density, only keloids have increased fibroblast proliferation rates [11]. Collagen fibers in keloids are larger, thicker, and wavier than those found in hypertrophic or normal scars [12]. They assume a random distribution, whereas those in hypertrophic scars have a parallel orientation to the epidermal surface [13].
Despite all research done in this area there is still no understanding of keloids and their pathogenesis. There are theories such as the collagen turnover hypothesis, the tension hypothesis, the genetic immune dysfunction hypothesis, and the sebum reaction hypothesis [5].
Medical advice is sought due to pain, pruritus, restriction of movement, and cosmetic disfigurement [6]. None of the existing treatment protocols seems to work reliably. No single method has produced consistent results [14]. Treatment modalities include compression, intralesional corticosteroids, laser, excision, imiquimod 5 percent cream (alone or after excision), intralesional Interferon-alpha 2b, or silicon dressing, alone or in combination. None is curative, but promote improvement and allow symptomatic relief [6, 14]. Prevention of wounds should be stressed to patients, especially those prone to keloids. When wounds do occur, the challenge remains to limit excessive scarring by reducing the known stimuli for scar overgrowth. The goal should be primary closure of wounds with the lowest tension possible [15].
It is hoped that the development of selective inhibitors of TGF-β, will produce new therapeutic tools with enhanced efficacy and specificity [5].
We intend to stress with this case that spontaneous reactivation of scars can occur. Our patient had quiescent keloids for almost 60 years. Muir, in 1990, stated that some scars may behave in a biphasic fashion, appearing normal initially and later developing into a keloid [9]. Despite the opinion of Sorabjee et al. that reactivation of old scars is inevitably sarcoidosis [4], our patient demonstrates that this is not always the case. Histologically we didn't find any granulomas, epithelioid cells, or eosinophils. Brightly eosinophilic collagen arranged in an haphazard way with some inflammatory infiltrate surrounding the blood vessels, very typical of keloid, were the findings in our patient's biopsies. Blood tests and chest X-ray showed no evidence for sarcoidosis. Recent reports have suggested that eruptive keloid-like plaques could represent a form of nephrogenic systemic fibrosis (NSF) or be a paraneoplastic sign [16, 17]. Although these conditions are not relevant to our case, they should be considered in the differential diagnosis of patients presenting with eruptive keloids. Our patient remains without any symptoms after two years of follow-up and no new lesions have ocurred.
References
1. Navid Bouzari, Stephen C. Davis and Keyvan Nouri. Laser treatment of keloids and hypertrophic scars. International Journal of Dermatology 2007; 46:80-88. [PubMed]2. Urioste SS, Arndt KA, Dover JS. Keloids and hypertrophic scars: review and treatment strategies. Semin Cutan Med Surg 1999; 18: 159-171. [PubMed]
3. Manuskiatti W, Fitzpatrick RE. Treatment response of keloidal and hypertrophic sternotomy scars: comparison among intralesional corticosteroid, 5-fluorouracil, and 585-nm flashlamp-pumped pulsed-dye laser treatments. Arch Dermatol 2002; 138: 1149-1155. [PubMed]
4. J S Sorabjee, R Garje Reactivation of old scars: inevitably sarcoid. Postgrad Med J 2005; 81:60-61. [PubMed]
5. Ali Al-Attar, Sarah Mess et al; Keloid Pathogenesis and Treatment. Plast Reconstr. Surg. 2006; 117: 286-300. [PubMed]
6. Mutalik S. Treatment of keloids and hypertrophic scars. Indian J Dermatol Venereol Leprol. 2005 Jan-Feb; 71(1):3-8. [PubMed]
7. Bayat A, Walter JM, Bock O, Mrowietz U, Ollier WE, Ferguson MW; Genetic susceptibility to keloid disease: mutation screening of the TGFbeta(3) gene. Br J Plast Surg 2005; 58:28-37. [PubMed]
8. Murray, J. C. Keloids and hypertrophic scars. Clin. Dermatol. 1994; 12:27. [PubMed]
9. Muir IF. On the nature of keloid and hypertrophic scars. Br J Plast Surg 1990; 43:61-69. [PubMed]
10. Oliver Bock, Gerhard Schmid-Ott, Peter Malewski, Ulrich Mrowietz; Quality of life of patients with keloid and hypertrophic scarring. Arch Dermatol Res 2006; 297: 433-438. [PubMed]
11. Nakaoka, H., Miyauchi, S., and Miki, Y. Proliferating activity of dermal fibroblasts in keloids and hypertrophic scars. Acta Derm.Venereol. 1995; 75: 102-104. [PubMed]
12. Ehrlich, H. P., Desmouliere, A., Diegelmann, R., et al. Morphological and immunochemical differences between keloid and hypertrophic scar. Am. J. Pathol. 1994; 145: 105. [PubMed]
13. Tina S. Alster and Elizabeth L. Tanzi. Hypertrophic Scars and Keloids. Etiology and Management. Am J Clin Dermatol 2003; 4 (4): 235-243. [PubMed]
14. Lee JH, Kim SE, Lee AY. Effects of interferon-alpha2b on keloid treatment with triamcinalone acetonide intralesional injection. Int J Dermatol. 2008 Feb;47(2):183-6. [PubMed]
15. Alison E. Slemp and Richard E. Kirschner; Keloids and scars: a review of keloids and scars, their pathogenesis, risk factors, and management. Curr Opin Pediatr 2006; 18:396-402. [PubMed]
16. Bremmer M, Deng A, Martin DB. Spontaneous eruptive keloid-like cutaneous lesions in a renal transplant patient: a form of nephrogenic systemic fibrosis? J Dermatolog Treat. 2009;20(1):63-6. [PubMed]
17. Coppa LM, Alam M, Longley FJ, Stiller MJ. Eruptive paraneoplastic keloids. Cútis. 1999 Oct;64(4):243-4. [PubMed]
© 2009 Dermatology Online Journal