Intralesional bleomycin as alternative therapy in the treatment of multiple basal cell carcinomas
Published Web Location
https://doi.org/10.5070/D31nw1550fMain Content
Intralesional bleomycin as alternative therapy in the treatment of multiple basal cell carcinomas
Magdalina Stoyanova Gyurova MD, Marieta Zheleva Stancheva MD, Monka Nedelcheva Arnaudova MD, Rumiana Kalopherova Yankova MD
PhD
Dermatology Online Journal 12 (3): 25
Department of Dermatology and Veneorology, Medical University, Plovdiv, Bulgaria. magigiurova@abv.bgAbstract
An 82-year-old female with with multiple basal cell carcinomas is presented. Her history includes treatment for similar lesions for 15 years with surgical and X-ray methods. We injected intralesional bleomycin to eight new histologically proven basal cell cancers. A followup at 2 years demonstrates the effectiveness of this therapy.
Bleomycin is a glucopeptide antitumor antibiotic isolated by Uwezawa et al. from the fungus Streptomyces verticellus in 1962 and clinically tested by Ichikawa et al. in the same year. The drug displayed excellent results in the treatment of malignancies including skin tumors. The first report about intralesional injection of bleomycin was made by Fujita et al. in 1970, presenting successful treatment of warts.
Bleomycin affects G2 and S phases of fast dividing cells and causes breakage of single-stranded DNA. Bleomycin prevents DNA repair by inhibiting DNA ligase. It is deactivated by aminopeptidase and bleomycin hydrolase, which are absent in the skin and this leads to greater concentration of the drug [1]. Intralesionally injected bleomycin leads to direct and indirect cytotoxicity of keratinocytes and eccrine epithelium [2]. Immunocytochemistry demonstrates tissue-fixation of bleomycin in all levels of epidermis except the basal layer and most prominently in the granular layer [3]. By affecting protein synthesis, bleomycin provokes a series of biochemical changes leading to apoptosis and full epidermal necrosis. These effects are dose-dependent and frequent injections of low doses of bleomycin are reported to be most effective. There are reports of successful treatment of warts, keloids, hemangioma, keratoacanthoma, basal cell carcinoma, early-stage squamous cell carcinoma, and single lesions of Kaposi sarcoma.
Clinical synopsis
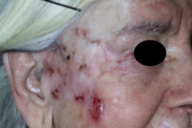
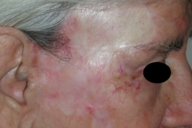
An 82-year-old woman presented with multiple lesions on her right temporal area of d15-years duration. She had been treated with X-ray therapy for some lesions in 1995. She was treated with surgical excision followed by plastic reconstruction in 1997. On examination the skin of the right temporal area had atrophic changes and eight various sized ulcerations with elevated pearly translucent borders. Skin biopsy was done and read as basal cell carcinoma with chronic radiodermatitis of the surrounding skin. Blood count and biochemical results (leukocytes, erythrocytes, thrombocytes, hemoglobin, erythrocyte sedimentation rate, fibrinogen, creatinine, urea, uric acid) before, during and after treatment are normal. Seven intralesional injections of 3IU bleomycin solution every 48 hours were administered (bleomycin was dissolved in normal saline solution to a concentration of 2 IU/ml and further diluted with an equal amount 1 % lidocaine hydrochloride); approximately 0.375 ml of the solution was injected into each lesion with 27-gauge needles. The patient's compliance was very good. The patient was photo-documented before (Fig. 1) and 2 years after treatment (Fig. 2).
 |  |
| Figure 1 | Figure 2 |
|---|---|
| Figure 1. Before treatment Figure 2. After 2 years treatment | |
Discussion
Intralesional therapy with bleomycin was chosen in our case of multiple basal cell carcinomas for several reasons; the patient declined surgical treatment, further X-ray therapy was contraindicated, and she was of advanced age. Bleomycin was repeatedly injected in low doses. Blood counts and biochemistry control allowed us to specify time intervals between applications as well as dosage, and to conduct the treatment effectively and safely. Treatment was continued until there was moderate swelling, perilesional erythema, and necrosis of the tumor tissue. Epithelization of the ulcer lesions started 1 month after treatment and ended 2 months later. The patient was followed for 2 years. No relapse or appearance of new lesions was registered within this period. The result of the intralesional therapy with bleomycin in our case appeared to be very good.
References
1. Dorr RT, Fritz, eds. Cancer chemotherapy handbook. New York: Elsevier science Publiching Co Inc, 1980. p 274- 83.2. Templeton SF, Solomon AR, Swerlick RA. Intradermal bleomycin injections into normal human skin. A histopathologic and immunopathologic study. Arch Dermatol 1994 May;130(5):577-83.
3. James MP, Collier PM, Aherne W, Hardcastle A, Lovegrove S. Histologic, pharmacologic, and immunocytochemical effects of injection of bleomycin into viral warts. J Am Acad Dermatol 1993 Jun;28(6):933-7.
© 2006 Dermatology Online Journal

