Transfascial muscular hernia: An unusual cause for a “hide and seek” subcutaneous nodule
Published Web Location
https://doi.org/10.5070/D31dm023gjMain Content
Transfascial muscular hernia: An unusual cause for a “hide and seek” subcutaneous nodule
Fernando Alfageme1, Victoriano Morales1, Carmen García1, Ana Patricia Miguelez1, Esther Domínguez2, Agustina Segurado1
Dermatology Online Journal 17 (2): 4
1. Department of Dermatology2. Department of Radiology
Hospital del Sureste (Arganda del Rey), Madrid, Spain. fernando.alfageme@salud.madrid.org
Abstract
Subcutaneous masses are usually difficult to diagnose for dermatologists using palpation. We report a case of a disappearing leg nodule that appeared with muscle compression. This is characteristic of a transfascial muscle hernia. Ultrasound is the key to identifying an area of fascial alteration. Treatment alternatives of this unusual condition are discussed.
Clinical case
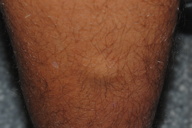 | 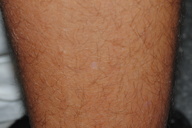 |
| Figure 1 | Figure 2 |
|---|
We report a case of a 14-year-old boy, a football league player, whose father was worried about a lump located on inner side of his son's right leg. The lump appeared when the boy pressed this foot on a rigid surface (Figure 1) and disappeared with pressure release (Figure 2). Neither father nor boy remembered previous trauma at this location.
Physical examination exhibited a soft, compressible, immovable nodule at this location that could not be palpated after pressure release.
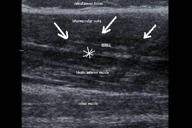 |
| Figure 3 |
|---|
An ultrasound examination (V-F 5-10 MhZ) of this nodule shows irregularity of the fascial layer at the level of the disappearing nodule (Figure 3, asterisk). With pressure, a muscular tibialis anterior hernia is revealed (Figure 3, arrows).
Conservative treatment was recommended and new consultation in case of enlargement or pain was encouraged.
Comment
Muscular hernias are focal protrusions of muscle tissue through fascial defects [1]. Their origin may be either primary or secondary to repetitive blunt trauma as in soccer players [1]. When muscular hernias occur in the lower leg, they are most common in the middle third. However, other muscles such as the peroneal, the extensor digitorum, and the lateral head of the gastrocnemius can be affected [2].
Consultation is often sought to rule out a soft tissue tumor and physical examination shows a lump in the described location. The diagnosis is mainly confirmed by ultrasound, demonstrating muscle protrusion through fascia with increasing compartment pressure. The transducer should be applied with minimum pressure because it can reduce the hernia and provide a false negative [3]. The ultrasound image is of a focal fascial disruption that can go unnoticed and may be recognized by the herniated portion of the muscle that has a mushroom-shaped appearance with a superficial convex contour. The hernia is usually less echogenic than the normal muscle, possibly because of anisotropy or crowding of the fibro-adipose septa. Doppler images may show an increase of vascularization through the hernia caused by this crowding phenomenon [4].
Asymptomatic hernias are treated conservatively. For severe pain or cosmetic reasons surgery may be contemplated. Fasciotomy or patch grafting are treatment options. Simple fascial repair should be avoided because it may result in a compartment syndrome [5].
Conclusion
The diagnosis of muscle hernia in should be considered when a leg lump that is dependant on compartment pressure is observed. Ultrasound is the gold standard test: it allows fast, dynamic, low cost exploration and guidance for treatment if necessary.
References
1. Beggs I. Sonography of muscle hernias. Am J Roentgenol 1993; 180:395–399 [PubMed]2. Mellado JM, Perez del Palomar L Muscle hernias of the lower leg: MRI findings. Skeletal Radiol 1999; 28:465-469. [PubMed]
3. Bates DG. Dynamic ultrasound findings of bilateral anterior tibialis muscle herniation. Pediatr Radiol 2001 31:753–755
4. Bianchi S, Abdelwahab IF, Mazzola CG, Ricci G, Damiani S. Sonographic examination of muscle herniation. J Ultrasound Med. 1995 May; 14(5):357–60. [PubMed]
5. Berglund HT, Stocks GW. Muscle hernia in a recreational athlete. Orthop Rev. 1993; 22(11):1246-8. [PubMed]
© 2011 Dermatology Online Journal

