Indolent herpetic whitlow of the toe in an elderly patient with diabetic neuropathy
Published Web Location
https://doi.org/10.5070/D31cs0p0twMain Content
Indolent herpetic whitlow of the toe in an elderly patient with diabetic neuropathy.
Maki Ozawa, Tomoyuki Ohtani, and Hachiro Tagami
Dermatology Online Journal 10 (1): 16
Department of Dermatology, Division of Internal Medicine, Tohoku University Graduate School of Medicine. ozawam@gonryo.med.tohoku.ac.jp
Abstract
We report a case of indolent herpetic whitlow of the toe occurring in an elderly male patient with poorly controlled diabetes mellitus. In this case, the mechanism of transmission was not clear, although he was in a habit of taking a hot spring bath. This patient's symptoms were unusual for herpes simplex; he had no pain in the presence of diabetic neuropathy. The standard therapeutic dose of acyclovir was not effective in suppressing the lesions, and a higher dose was required to induce complete healing.
Introduction
Herpetic whitlow is a painful infection caused by the herpes simplex virus (HSV) mostly affecting the hands and fingers. In 1909 Adamson published the first case report of herpetic infection affecting the hand [1]. Since then herpetic whitlow on the fingers has been reported frequently. In contrast, case reports of herpetic infection involving the toe are uncommon.
The following case report describes a unique case of herpetic whitlow of the toe occurring in an elderly diabetic patient acquired by an unknown mechanism of transmission.
Clinical summary
|
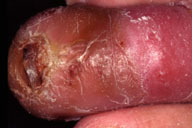
| Figure 1 |
|---|
| Erythematous swelling on his right second toe with formation of a 4-mm ulcer and an irregular shaped pustule. |
On March 4, 2002, a 68-year-old man visited us with a 2-day history of erythematous swelling on his right second toe, which he noticed one day after taking a hot spring bath. He did not complain of any pain. Laboratory examination disclosed that the complete blood cell count, renal and liver functions and urinalysis were all within normal range. His C-reactive protein was high (7.3 mg/dl) and HbA1c was also high (9.3 %). He had been suffering from uncontrolled diabetes mellitus and diabetic neuropathy for the past 10 years. Oral antibiotics were prescribed for presumed bacterial cellulitis. The lesion worsened, however, with formation of a 4-mm ulcer and an irregular-shaped pustule within 48 hours (Fig. 1).
The base of the unroofed pustule of the toe was swabbed for herpes simplex virus (HSV) detection test. It was positive for HSV-1. Even after 5 days of oral acyclovir (1000 mg per day), the response was poor, so that the patient's dosage of acyclovir was increased to 4000 mg per day. Because the toe lesion improved with this treatment after 7 days, the medication was discontinued.
Discussion
The present case is atypical in that herpetic whitlow developed in the toe. Furthermore it lacked the characteristic pain that is usually a clue to the clinician that a lesion not responding to antibacterial treatment may be of herpetic origin. There are 3 reported cases of herpetic whitlow of the toe in the literature. Feder et al. described a 3-year-old girl with HSV-1 infection of the great toe that was thought to be transmitted when her mother with herpes labialis trimmed her daughter's toenail using her teeth [2]. The reported by Egan et al. was a 28-year-old woman with genital herpes who developed HSV-2 infection of her toe [3]. The authors proposed neural transmission from the sacral ganglia to the toe or autoinoculation through toe-genital contact as a possible mode of transmission. The third case was reported by Mohler who found HSV-1 infection of the left fifth toe in a 13-month-old girl [4]. In this case, autoinoculation is thought to be the most likely mode of transmission. In our present case, the transmission mode could not be determined, however he was a frequent visitor at a hot-spring resort, and that might have provided the opportunity for a chance inoculation. No previous cases were found in the literature that had such a form of transmission.
The clinical symptoms of herpetic whitlow characteristically begin with intense itching or pain in the infected finger or toe. In the present case, however, there was no pain in the toe because of his diabetic neuropathy, which made its early diagnosis more difficult.
Cutaneous infections are one of the most important skin disorders in diabetes mellitus. Precise mechanisms for some skin infections to be more common in diabetics is still unclear, however, Cooppan postulated that high frequency of infection in diabetics could be attributed to dehydration, dysfunction of polymorphonuclear leukocytes, microangiopathy, and neuropathy [5]. He also pointed out the low serum level of antibody and complement components in diabetics and considered them as possible underlying factors for these infections. According to these reports, cutaneous infections in diabetic patients should be treated as that in immunocompromised hosts.
The International Herpes Management Forum has presented a guideline for management of herpesvirus infection in the immunocompromised host [6]. According to it, patients should be re-evaluated 3-5 days after onset of treatment and if the response is good, the therapy should be continued until there is evidence of complete healing. In the case of a poor response, the standard therapeutic dosage should be increased and the patient again re-evaluated after several days for the evidence of healing. If there are concerns about patient compliance or the possibility of gastrointestinal disease impairing drug absorption, acyclovir should be administered 1-2 mg/kg/hour as a continuous infusion. The present case did not respond to the first treatment with the standard therapeutic dose, however, it healed with an increase in dosage.
In this case of herpetic whitlow of the toe, the only potential exposure to the virus that we could identify was the communal bath. The clinical symptoms were not typical because, with diabetic neuropathy, the patient had no pain involving the affected area. When standard therapeutic dose of acyclovir is ineffective, increased dosage may provide complete healing.
References
1. Adamson, H. Herpes febrilis attacking the fingers. Br J Dermatology, 21: 323-324, 1909.2. Feder, H. M., Jr. and Geller, R. W. Herpetic whitlow of the great toe. New England Journal of Medicine, 326: 1295-1296, 1992.
3. Egan, L. J., Bylander, J. M., Agerter, D. C., and Edson, R. S. Herpetic whitlow of the toe: an unusual manifestation of infection with herpes simplex virus type 2. Clinical Infectious Diseases, 26: 196-197, 1998.
4. Mohler, A. Herpetic whitlow of the toe. Journal of the American Board of Family Practice, 13: 213-215, 2000.
5. Cooppan, R. Infection and diabetes. In: Joslin's Diabetes Mellitus, 12th edition edition, pp. 737. Philadelphia: Lee & Febiger, 1985.
6. Sivayathorn, A. and Whitley, R. Herpesvirus infections in the immunocompromised host with HIV update. International Herpes Management Forum, pp. 34-35, 1996.
© 2004 Dermatology Online Journal

