Clopidogrel-associated vasculopathic cutaneous reaction
Published Web Location
https://doi.org/10.5070/D31886v57wMain Content
Clopidogrel-associated vasculopathic cutaneous reaction
Ramin Fathi1 BA, H Nicholas Shamma2 MD, Ahmad Fathi3 MD
Dermatology Online Journal 19 (1): 7
1. Rush Medical College of Rush University Medical Center, Chicago, Illinois2. Wright State University School of Medicine Department of Dermatology, Dayton, Ohio
3. Skin, Vein & Cosmetic Surgery Clinic, PC, Munster, Indiana
Abstract
We present a case report of a man who experienced vascular thromboses, which subsequently resolved following discontinuation of clopidogrel.
Case report
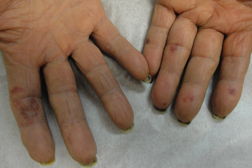
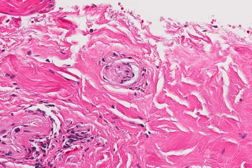
A 76-year-old man with past medical history of peripheral artery disease presented as an inpatient with a 2-week history of multiple gangrenous areas on the fingers of both hands (Figure 1). Review of systems was unremarkable. His medications included clopidogrel, simvastatin, and tamsulosin. Lab tests showed a PT of 12.6 (normal 9.5-13.2), INR of 1.00 (0.83-1.20), aPTT of 34.9 (normal 23-33), platelet count of 254,000 (normal 150-399), activated protein C of 130, activated protein S of 102, and fibrinogen of 368. D-dimer was 3.64 ugFEU/mL (normal <0.5 ugFEU/mL) whereas anti-phospholipid antibodies and cryoglobulins were negative. A cutaneous punch biopsy of the left middle finger was performed (Figure 2).
The biopsy showed small fibrin thrombi present in the lumina of small thin walled superficial blood vessels within the dermis. A sparse perivascular lymphocytic infiltrate was noted in addition to massive full thickness epidermal necrosis. The patient had normal lab values ruling out platelet disorders, cryoglobulinemia, anti-phospholipid antibodies, and protein-C and S deficiencies. Clopidogrel was discontinued and the patient made a full recovery with no sequalae.
Discussion
Vasculopathic cutaneous reactions can occur in a multitude of clinical settings such as altered platelet counts (e.g. idiopathic thrombocytopenic purpura and thrombotic thrombocytopenic purpura), coagulation factor deficiencies (e.g. inherited or acquired protein-C and S deficiencies), coagulopathies associated with connective tissue disease (e.g. lupus anticoagulant and antiphospholipid syndrome), as well as platelet thrombosis and heparin necrosis [1]. Disseminated intravascular coagulation (DIC) and cryoglobulins may show similar histology as well. Whereas the D-dimer assay may be elevated in DIC, there are many conditions unrelated to thrombosis in which D-dimer concentrations are high, making its positive predictive value rather poor. D-dimer is also used to diagnose and manage a vast array of thrombosis-related clinical conditions and is more a marker of sensitivity rather than specificity. In DIC, one would expect a consumptive coagulopathy including abnormally elevated prothrombin time and a decreased platelet count [2]. In the absence of these possible culprits, it appears that clopidogrel may have induced coagulation without thrombocytopenia because discontinuation of clopidogrel resolved the situation.
Clopidogrel, an irreversible inhibitor of adenosine diphosphate (ADP) chemoreceptors on platelet cell membranes, has been associated with thrombotic thrombocytopenic purpura; this has been previously reported as a side effect with an incidence of 1/100,000 [3]. However, in this case thrombosis took place without any clinical and laboratory evidence of thrombocytopenia. Multiple studies have reported thienopyridine-associated TTP as a result of ADAMTS13 deficiency and inhibitors to ADAMTS13 at diagnosis [4]. Other studies describe cases of thienopyridine-associated TTP without severe ADAMTS13 deficiency, usually with the presentation of post-transplantation thrombotic microangiopathy [5]. These patients, however, frequently present with renal insufficiency, moderate thrombocytopenia, and high mortality rates. Others have described TTP-like findings among persons with factor V Leiden mutation [6]. Whether these mechanisms play a role in the presentation of our patient remains to be seen. Recently, Erpolat et al reported a patient with leukocytoclastic vasculitis associated with clopidogrel. This patient presented with painful cutaneous gangrenous areas four days after starting clopidogrel following stent insertion, with a similar recovery as our patient following discontinuation [7].
References
1. Barnhill RL, Mousari CH, Xu X, Barksdale SK. Vascular Diseases. Lever’s Histopathology of the Skin. 10th ed. 2009:228-230.2. Tripodi A. D-Dimer Testing in Laboratory Practice. Clinical Chemistry 2011 Sep;57(9);1256-62. [PubMed]
3. Bennett CL, Kim B, Zakarija A, Bandarenko N, Pandey D, Buffie C, McKoy J, Tevar A, Cursio JF, Yarnold PR. Two Mechanistic Pathways for Thienopyridine-Associated Thrombotic Thrombocytopenic Purpura. A Report From the SERF-TTP Research Group and the RADAR Project. Journal of the American College of Cardiology 2007 Sep;18;50(12):1138-43. [PubMed]
4. Tsai HM, Rice L, Sarode R, Chow TW, Moake JL. Antibody inhibitors to von Willebrand factor metalloproteinase and increased binding of von Willebrand factor to platelets in ticlopidine-associated thrombotic thrombocytopenic purpura. Ann Intern Med 2000 May;132(10):794-9. [PubMed]
5. Qu L, Kiss JE. Thrombotic microangiopathy in transplantation and malignancy. Semin Thromb Hemost 2005 Dec;31(6):691-9. [PubMed]
6. Raife TJ, Lentz SR, Atkinson BS, Vesely SK, Hessner MJ. Factor V Leiden: a genetic risk factor for thrombotic microangiopathy in patients with normal von Willebrand factor-cleaving protease activity. Blood 2002 Jan 15;99(2):437-42. [PubMed]
7. Erpolat S, Nasil Y, Colak N, Yenidunya S. Leucocytoclastic vasculitis associated with clopidogrel. Cutan Ocul Toxicol. 2012 Jun;31(2):171-3. [PubMed]
© 2013 Dermatology Online Journal