Multiple furunculoid myiasis on the scalp of a child
Published Web Location
https://doi.org/10.5070/D317z0g570Main Content
Multiple furunculoid myiasis on the scalp of a child
M Yébenes, C Muñoz, M Sábat, L Palacio, B San Vicente1, FJ Travería2, J Luelmo
Dermatology Online Journal 13 (2): 13
Departments of Dermatology, Pediatrics2 and Pediatric Surgery1, Hospital Parc Taulí, SabadellAbstract
Cutaneous myiasis is easy to diagnose and treat if clinicians are aware of the condition. Because of widespread travel, physicians may encounter this infestation in patients living in geographical regions where the condition is rare. A child is presented with cutaneous myiasis that presented as furuncle-like nodules on the scalp. The larvae were identified as a stage of the bluebottle-like fly, Dermatobia hominis.
Myiasis is the infestation of body tissues of humans and animals by the larvae of Diptera [1]. It is usually classified from an entomological or a clinical point of view. Entomologically, flies may be classified into three myiasis-producing groups: obligatory, facultative, and accidental. Clinically, myiasis can be classified according to the part of the body affected. Cutaneous myiasis includes wound myiasis and furuncular myiasis. Although it is most unusual in our locale, imported cases can be found because of increased traveling and immigration [2]. One study showed that myiasis is the fourth most common travel-associated skin disease [3]. Dermatobia hominis is a bluebottle-like fly that is endemic in tropical regions of Central and South America
Clinical synopsis
A 4-year-old girl, who had just arrived from Bolivia, was referred to our Emergency Department, as a result of furunculous lesions on the scalp. The nodules had appeared 7 days before and the area was itchy and painful.
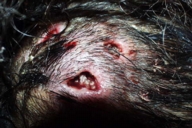
Physical examination revealed a large inflammatory, nodular plaque that occupied the whole vertex of the scalp. There were several pores, each about 1 centimeter in diameter, from which exuded serosanguineous discharge. We also observed a great number of living larvae (Fig. 1). Moreover, the child was febrile and exhibited regional lymphadenopathy. Complete blood count showed eosinophilia.
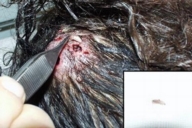
We applied an occlusive dressing with paraffin oil for 24 hours. After we removed the occlusive dressing, cut the hair, and cleaned the wounds, the furunculous nodules were opened and the larvae extracted carefully (Fig. 2A). Partial approximation of the wound was performed by a pediatric surgeon, but the center closed by secondary intention. Microbiology analysis confirmed the diagnosis of myiasis and identified the larvae (Dermatobia hominis), and the subspecies (Cochliomyia hominivorax) (Fig 2B).
During a follow-up of 6 months, the girl has not shown any new lesions.
Discussion
Dermatobia hominia lives predominantly in warm, moist areas such as lowland forests, but can also be found in mountainous regions. The subspecies Cochliomyia hominivorax, an obligatory larval parasite, is one of the most important myiasis-causing flies.
Adult flies capture other insects and deposit 10 to 50 eggs on them. The vector in turn bites the host; the larvae, sensing the increase in temperature, immediately detach themselves and quickly burrow into subcutaneous tissues. There they feed and grow for approximately 6 to 8 weeks. The larvae emerge on maturity, fall to the ground, and pupate into adult flies [5].
As the larvae grow, a subcutaneous mass becomes evident. A pore, called a punctum, is present in the center of the mass and is used for ventilation and excretion of waste. Serosanguineous fluid can be expressed and sudden paroxysmal episodes of severe, sharp pain is usual [6]. For obvious reasons the infestations have a predilection for exposed surfaces.
The diagnosis is mainly clinical. The most important clues to the diagnosis are a history of recent travel to an endemic area, adjacent healing lesions on the skin, pruritus, and a sensation of movement under skin or sudden pains. The diagnosis is confirmed by the extraction of the larvae.
Histopathological examination shows a small cavity in the dermis, containing the developing larva. Surrounding this is a heavy infiltrate of mixed inflammatory cells, which include lymphocytes, histiocytes, occasional giant cells, and plasma cells.
The furuncle-like appearance of the lesion is the reason why Dermatobia infestation is very often mistaken as common pyoderma. Other differential diagnoses include epidermoid cyst, tungiasis, cutaneous larva migrans, and cutaneous leishmaniasis [7].
The most important complications in man are bacterial superinfection (cellulitis, abscess formation, osteomyelitis) and tetanus. Cerebral myiasis as a result of infestation of the skin covering the fontanels of infants is a rare, but life-threatening condition.
Treatment involves removal of all larvae in their entirety; any remnant may provoke an inflammatory response. The successful use of an occlusive dressing in combination with manual extraction has been described in the literature.
The use of topical or oral ivermectin to treat severe cases of myiasis has been published. The use of this molecule paralyzes and then kills the larvae. This allows rapid alleviation of pain and makes the extraction of the larvae easier [8].
In conclusion, our case is interesting because of the large number of nodules and larvae that our patient presented. If this infestation is recognized, confirmation of the diagnosis and therapy are very easy.
References
1. Hawayek LH, Mutasim DF. Myiasis in a giant squamous cell carcinoma. J Am Acad Dermatol. 2006;54:740-12. Langan SM, Dervan P, O'Loughlin S. A moving scalp nodule in a returning traveller. Br J Dermatol. 2004;151:1270.
4. Caumes E, Carriere J, Guermonprez G, Bricaire F, Danis M, Gentilini M. Dermatoses associated with travel to tropical countries: a prospective study of the diagnosis and management of 269 patients presenting to a tropical disease unit. Clin Infect Dis. 1995;20:542-8.
5. Maier H, Honigsmann H. Furuncular myiasis caused by Dermatobia hominis, the human botfly. J Am Acad Dermatol. 2004;50:S26-30.
6. Adisa CA, Mbanaso A. Furuncular myiasis of the breast caused by the larvae of the Tumbu fly (Cordylobia anthropophaga). BMC Surg. 2004;29;4:5.
7. Rodriguez G, Rashid M. Human scrotal myiasis (bot fly): a case of self-diagnosis. J Urol. 2001;166(4):1397-8.
8. Siraj DS, Luczkovich J. Nodular skin lesion in a returning traveler. J Travel Med. 2005;12(4):229-31.
© 2007 Dermatology Online Journal