Hobnail hemangioma in a nine-year-old boy: A rare case presented with dermoscopy
Published Web Location
https://doi.org/10.5070/D30xn7g257Main Content
Hobnail hemangioma in a nine-year-old boy: A rare case presented with dermoscopy
Marian Ibrahim MD1, Tor Shwayder MD FAAP FAAD2
Dermatology Online Journal 16 (4): 7
1. Wayne State University School of Medicine Detroit, Michigan. mibrahim@med.wayne.edu2. Department of Dermatology, Henry Ford Hospital, Detroit, Michigan
Abstract
Hobnail hemangioma is a benign vascular tumor that typically occurs on the trunk and extremities. Most patients present in the 20s and 30s. We describe a rare case of hobnail hemangioma in a 9-year-old male.
Case report
 |  |
| Figure 1A | Figure 1B |
|---|---|
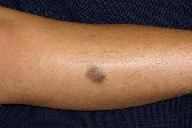
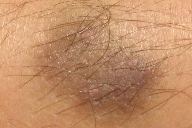
| Figure 1A. Dark macule on right shin of 9-year-old middle eastern male Figure 1B. Close up of lesion showing papular component and yellow tinged edges. | |
 |
| Figure 2 |
|---|
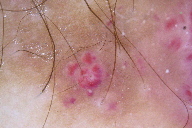
| Figure 2. Dermoscopy showing well defined red circular blebs |
A 9-year-old healthy boy presented for the evaluation of a nonpruritic, nontender hyperpigmented lesion on the right shin. The patient’s mother reports that the lesion first appeared at about 6 to 10 months of age. Initially it appeared to be a bruise and they attributed it to trauma. From the onset, it has been asymptomatic and has not changed or bled. Physical exam revealed a 2 cm x 1.7 cm, ill-defined, indurated plaque, brown to deep blue in color, with slightly yellow tinged edges. Hair was visible within the lesion (Figure 1). There were minute erythematous papules within themacule. No verrucous component was noted. On dermoscopy there were small blebs reminiscent of a lymphangioma (Figure 2).
 | 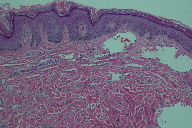 |
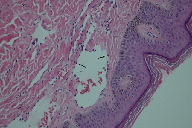
| Figure 3A | Figure 3B |
|---|---|
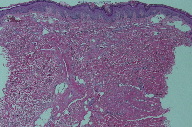
| Figure 3A. Low power showing dilated ectatic blood vessels (H&E) Figure 3B. Higher power showing multiple slit-like blood vessels (H&E) | |
 | 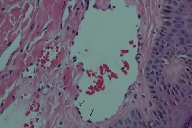 |
| Figure 4 | Figure 5 |
|---|---|
| Figure 4. Note the hobnail appearing endothelial cells Figure 5. Close up of hobnail appearing endothelial cells | |
A 5 mm punch biopsy was taken, which revealed ectatic vascular spaces throughout the dermis (Figure 3). The spaces were lined by slightly prominent endothelial cells (Figures 4 and 5). The dermis was fibrotic and contained numerous siderophages, which extended into the subcutanous tissue. Hemosiderin was noted throughout the dermis down to the fat (Figure 6). No abnormal lymphatic vessels were noted. CD34a immunostaining exhibited patchy positivity (Figure 7). Actin labeling was negative in the pericytes. No plasma cells were seen. No endothelial cell atypia was noted. The lymphatic endothelial cell marker D2-40 was not available.
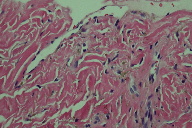 | 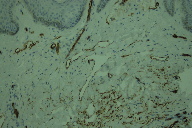 |
| Figure 6 | Figure 7 |
|---|---|
| Figure 6. Note the hemosiderin depositions in the interstitium Figure 7. CD34 stain showing patchy positivity | |
Discussion
Hobnail hemangioma, also known as targetoid hemosiderotic hemangioma was first described as a unique entity in 1988 by Santa Cruz and Aronberg [1]. It is a benign vascular tumor that typically presents on the trunk and extremities, more often the lower extremities [2]. There have also been cases described on the head and neck, in the mouth, on the breast, and on the buttock [2]. Patient age varies from 5 to 72 years old, but most patients present in the 20s or 30s [3]. It is more common in males than females [2]. Trauma, radiation, and trauma to a preexisting hemangioma are proposed etiologies [4]. According to this patient’s mother the growth presented between 6 and 10 months of age, which is an unusually young age for hobnail hemangioma.
In a recent study by Franke et al. the lymphatic origin was proven by immunohistochemistry using the lymphatic endothelial cell marker D2-40 that hobnail hemangioma. Several hobnail hemangiomas stained only with D2-40, indicating lymphatic origin. A lymphatic origin is suggested by the CD34 negativity of the endothelial cells seen in most but not all cases. Lymphatic origin is also supported by the lack of actin-labeled pericytes [5, 6, 7, 8]. There are thought to be mircroshunts connecting these lymphatic vessels and adjacent blood vessels. The capillary pressure can cause the tumor to be filled with erythrocytes, cause aneurismal structures, and causeobstruction of efferent lymphatics. This capillary pressure may also promote extravasation of erythrocytes, resulting in hemosiderin deposition in the interstitium, inflammation, and fibrosis [6, 9, 10].
Typically hobnail hemangioma manifests as a targetoid lesion that is less than 1cm with a central violacious papule and a surrounding halo that can vary in color from tan to black. The color is thought to be partially due to red blood cell extravasation and hemosiderin deposition [2, 3, 4, 11, 12]. Hormones, especially estrogen, have been found to influence the outer halo, resulting in a waxing and waning appearance, especially in females [3, 13]. Clinical presentation is variable; it may be targetoid, nontargetoid, macular, or exophytic. Predominantly, the lesion is asymptomatic, but may be painful. This patient presented with a non-targetoid lesion with no disruption of the normal hair distribution of the lower extremity. To the best of our knowledge hair within the lesion itself has not been described previously.
Upon microscopy, hobnail hemangioma has a biphasic pattern. More superficially, in the papillary dermis there are dilated thin walled vessels lined by hobnail-appearing endothelial cells, which are the reason for the name hobnail hemangioma. In the papillary dermis, intraluminal papillary projections and fibrin thrombi can also be seen. In the deeper dermis there are typically slit-like angulated vascular spaces that dissect through collagen bundles. There is an associated fibrosis, an inflammatory infiltrate, and hemosiderin deposits [2, 3, 6, 9, 12]. Hobnail hemangioma can be mistaken for malignancies such as angiosarcoma, melanoma, and Kaposi sarcoma. It can be differentiated from Kaposi sarcoma in many ways. Hobnail hemangioma has dilated channels along with intraluminal papillary projections, unlike Kaposi sarcoma. It also does not contain plasma cells and does not stain positively with HHV-8, which is typical of Kaposi sarcoma. Angiosarcoma shows endothelial cell atypia, which is not characteristic of hobnail hemangioma [3].
In addition dermoscopy can help in making the correct diagnosis. In melanocytic lesions brown or black streaks, globules and dots are typically seen. Their absence is characteristic of non-melanocytic pigmented skin lesions [14]. In hobnail hemangioma, dermoscopy shows sharply demarcated red round to oval structures that are thought to correspond with the ectatic thin walled vessels in the papillary dermis. Intermixed with these structures are smaller, pale pink, round structures found among a diffuse pink-white pigmentation, which is thought to correspond to the slit-like vascular spaces that dissect collagen bundles in the deeper dermis [5]. In some cases, a few sharply demarcated black macules representing hemorrhagic crust were seen [14].
Treatment options are limited. Nothing specific is published on this. Since it is neither a cancer nor an infection, doing nothing is a viable alternative after diagnosis. Excision of small lesions is possible. Therapeutic sclerosis of the ectatic spaces by the injection of sclerosing solutions is theoretically possible but would probably not affect the lesion beyond the small area treated. This patient chose to do nothing. It is critical to correlate the clinical findings with the dermoscopic and histological findings to make the correct diagnosis.
References
1. Santa Cruz DJ, Aronberg J. Targetoid hemosiderotic hemangioma. J Am Acad Dermatol 1988;19:550-558. [PubMed]2. Mentzel T, Partanen TA, Kutzner H. Hobnail hemangioma (“targetoid hemosiderotic hemangioma”): Clinicopathologic and immunohistochemical analysis of 62 cases. J Cutan Pathol 1999;26:279-286. [PubMed]
3. Bingham LG, Davis DM. Clinicopathologic challenge. Int J Dermatol 2008;47:991-992. [PubMed]
4. Christenson LJ, Stone MS. Trauma-induced simulator of targetoid hemosiderotic hemangioma. Am J Dermatopathol 2001;23:221-223. [PubMed]
5. Morales-Callaghan AM, Martinez-Garcia G, Aragoneses-Fraile H, et al. Targetoid hemosiderotic hemangioma: clinical and dermoscopical findings. J Eur Acad Dermatol Venereol 2007;21:267-269. [PubMed]
6. Franke FE, Steger K, Marks A, et al. Hobnail hemangiomas (targetoid hemosiderotic hemangiomas) are true lymphangiomas. J Cutan Pathology 2004;31:362-367. [PubMed]
7. Kahn HJ, Bailey D, Marks A. Monoclonal antibody D2-40, a new marker of lymphatic endothelium, reacts with Kaposi’s sarcoma and a subset of angiosarcomas. Mod Pathol 2002;15:434. [PubMed]
8. Kahn HJ, Marks A. A new monoclonal antibody, D2-40, for detection of lymphatic invasion in primary tumors. Lab Invest 2002;82:1255. [PubMed]
9. Guillou L, Calonje E, Speight P, et al. Hobnail hemangioma: a pseudomalignant vascular lesion with a reappraisal of targetoid hemosiderotic hemangioma. Am J Surg Pathol 1999;23:97. [PubMed]
10. Calonje E, Fletcher CD, Wilson-Jones E, et al. Retiform hemangioendothelioma: A distinctive form of low-grade angiosarcoma delineated in a series of 15 cases. Am J Surg Pathol 1994;18:115. Abstract
11. Perrin C, Rodot S, Ortonne JP, et al. Targetoid hemosiderotic hemangioma. Ann Dermatol. Venereol 1995;122:111-114. [PubMed]
12. Weed B, Sciallis G, Borrowman T. Targetoid hemosiderotic hemangioma (hobnail hemangioma). J Cutan Pathol 2007;34:115. [PubMed]
13. Ortiz-Rey JA, Gonzalez-Ruiz A, San Miguel P, et al. Hobnail hemangioma associated with the menstrual cycle. J Eur Acad Dermatol Venereol 2005;19:367-369. [PubMed]
14. Sahin MT, Demir MA, Gunduz K, et al. Targetoid hemosiderotic haemangioma: dermoscopic monitoring of three cases and review of the literature. Clin Exp Dermatol 2005;30:672-676. [PubMed]
© 2010 Dermatology Online Journal

